Abstract
Purpose
Separation of midline abdominal wall components or other procedures involving the papilla umbilicalis within the context of abdominal wall reconstruction can significantly affect vasculature of the umbilicus. Adjusting dissection to the vascular anatomy of that region may evade such complications. For this purpose, an anatomic microdissection study was performed, focusing on the vascular architecture of the papilla umbilicalis in the midst of the stratigraphical anatomy of the midline abdominal wall.
Methods
Ramifications of the epigastric vessels were filled with dye on 27 abdominal walls originating from 15 female and 12 male corpses. Vascular architecture of the midline abdominal wall was examined by X-ray imaging and microdissection focusing region of the papilla umbilicalis.
Results
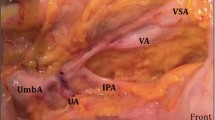
Vasculature of the papilla umbilicalis is provided by both myocutaneous and septocutaneous perforator vessels originating from the medial branch of the arteria epigastrica inferior and accompanying veins. On their way to the inferiolateral basis of the papilla umbilicalis, these perforators prove an intimate and regular association with the rectus abdominis muscle, and different components of the rectus sheath.
Conclusions
Vasculature of the papilla umbilicalis is susceptible to damage resulting from separation of midline abdominal wall components or periumbilical dissections. To secure vasculature of the papilla umbilicalis, the integrity of the loose areolar fascia covering the posterior surface of the rectus abdominis muscle must be kept from being harmed by dissection. In addition, the musculo-fibrous-aponeurotic anatomy on either the left or the right side of the papilla umbilicalis must be left in structural continuity.





Similar content being viewed by others
References
O’Dey DM, von Heimburg D, Prescher A, Pallua N (2004) The arterial vascularisation of the abdominal wall with special regard to the umbilicus. Br J Plast Surg 57:392–397
O’Dey D, Prescher A, Pallua N (2007) Vascular reliability of nipple–areola complex-bearing pedicles: an anatomical microdissection study. Plast Reconstr Surg 119:1167–1177
O’Dey DM, Prescher A, Pallua N (2006) Anatomic considerations to improve vasculature of the nipple–areola complex in vertical mammaplasty. Handchir Mikrochir Plast Chir 38:370–377, German
Paar O, mon O’Dey D, Magin MN, Prescher A (2000) Disruption of the arteria nutricia tibiae by reamed and unreamed intramedullary nailing. Study of the vascular architecture of the human tibial intramedullary cavity. Z Orthop Ihre Grenzgeb 138:79–84, German
Taylor GI, Corlett RJ, Boyd JB (1984) The versatile deep epigastric (inferior rectus abdominis) flap. Br J Plast Surg 37:330–350
Itoh Y, Arai K (1993) The deep inferior epigastric artery free skin flap. Anatomic study and clinical application. Plast Reconstr Surg 91:853–863
El-Mrakby HH, Milner RH (2001) The vascular anatomy of the lower anterior abdominal wall: a microdissection study on the deep inferior epigastric vessels and the perforator branches. Plast Reconstr Surg 109:539–554, discussion 544-547
Munhoz AM, Ishida LH, Duarte GG, Cunha MS, Montag E, Sturtz G, Gemperli R, Ferreira MC (2003) Aesthetic refinements in breast augmentation with deep inferior epigastric perforator flap: a case report. Aesthet Plast Surg 27:107–111
Stokes RB, Whetzel TP, Sommerhaug E, Saunders CJ (1998) Arterial vascular anatomy of the umbilicus. Plast Rekonstr Surg 102:761–764
Boyd JB, Taylor GI, Corlett R (1984) The vascular territories of the superior epigastric and the deep inferior epigastric systems. Plast Reconstr Surg 73:1–13
Onishi K, Maruyama Y (1986) Cutaneous and fascial vasculature around the rectus abdominis muscle: anatomic basis of abdominal fasciocutaneous flaps. J Reconstr Microsurg 4:247–253
Blondeel PN, Van Landuyt KH, Monstrey SJ, Hamdi M, Matton GE, Allen RJ, Dupin C, Feller AM, Koshima I, Kostakoglu N, Wei FC (2003) The “Gent” consensus on perforator flap terminology: preliminary definitions. Plast Reconstr Surg 112:1378–1382
Axer H, Keyserlingk DG, Prescher A (2001) Collagen fibers in linea alba and rectus sheaths. I. General sheme and morphological aspects. J Surg Res 96:127–134
Competing interest statement
The authors declare that they have no competing financial interests.
Authors’ contributions
Study conception and design: Dan mon O’Dey.
Acquisition of data: Dan mon O’Dey, Chukwubikem Akabogu Okafor.
Analysis and/or interpretation of data: Dan mon O’Dey, Chukwubikem Akabogu Okafor, Ahmet Bozkurt, Andreas Prescher, and Norbert Pallua.
Drafting of manuscript: Dan mon O’Dey.
Critical revision of manuscript: Dan mon O’Dey, Chukwubikem Akabogu Okafor, Ahmet Bozkurt, Andreas Prescher, and Norbert Pallua.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
O’Dey, D.m., Okafor, C.A., Bozkurt, A. et al. Perforator vessel anatomy of the papilla umbilicalis: topography and importance for reconstructive abdominal wall surgery. Langenbecks Arch Surg 395, 1121–1127 (2010). https://doi.org/10.1007/s00423-010-0657-7
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00423-010-0657-7