Abstract
Introduction
Blood flow restriction (BFR) exercise has emerged as a method of increasing muscle size and strength with low intensity resistance training. While the cuff pressures used during BFR are typically a percentage of resting arterial occlusion pressure (AOP), the impact these cuff pressures have on blood flow during lower body exercise is unknown.
Purpose
To determine how various cuff pressures impact blood flow and tissue perfusion during exercise.
Methods
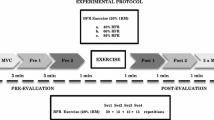
Eleven healthy male participants completed four sets of knee extension (30 reps per set at 30% max torque) with 0%, 60%, 80%, and 100% of arterial occlusion pressure (AOP) was applied to the proximal portion of the thigh. Femoral artery blood flow, tissue oxygenation, and central hemodynamics were continuously recorded before, during, and after exercise. Electromyography (EMG) amplitude was recorded from the vastus lateralis during exercise.
Results
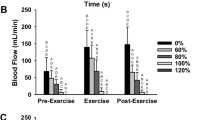
Blood flow increased during exercise compared to rest across all cuff pressures (p < 0.001), however compared to 0%, the absolute blood flow was reduced by 34 ± 17%, 45 ± 22%, and 72 ± 19% for 60, 80, and 100% AOP, respectively. Furthermore, each cuff pressure resulted in similar relative changes in blood flow before, during, and after exercise. During exercise, tissue saturation index (TSI) decreased as cuff pressure increased (p ≤ 0.005) with the exception of 80 to 100% AOP. Deoxyhemoglobin increased (p ≤ 0.001) with cuff pressure.
Conclusion
Our data indicate that while BFR knee extension elicits an absolute hyperemic response at cuff pressures up to 100% resting AOP, the relative reductions in blood flow are consistent across rest, exercise and recovery.






Similar content being viewed by others
References
Braith RW, Stewart KJ (2006) Resistance exercise training. Circulation 113:2642–2650
Cook CJ, Kilduff LP, Beaven CM (2014) Improving strength and power in trained athletes with 3 weeks of occlusion training. Int J Sports Physiol Perform 9:166–172. https://doi.org/10.1123/ijspp.2013-0018
Counts BR, Dankel SJ, Barnett BE et al (2016) Influence of relative blood flow restriction pressure on muscle activation and muscle adaptation. Muscle Nerve 53:438–445. https://doi.org/10.1002/mus.24756
Downs M, Hackney K, Martin D et al (2014) Acute vascular and cardiovascular responses to blood flow-restricted exercise. Med Sci Sports Exerc 46:1489–1497. https://doi.org/10.1249/MSS.0000000000000253
Fujita T, Brechue WF, Kurita K et al (2008) Increased muscle volume and strength following six days of low-intensity resistance training with restricted muscle blood flow. Int J KAATSU Train Res 4:1–8. https://doi.org/10.3806/ijktr.4.1
Ganesan G, Cotter JA, Reuland W et al (2015) Effect of blood flow restriction on tissue oxygenation during knee extension. Med Sci Sports Exerc 47:185–193. https://doi.org/10.1249/MSS.0000000000000393
Habazettl H, Athanasopoulos D, Kuebler WM et al (2010) Near-infrared spectroscopy and indocyanine green derived blood flow index for noninvasive measurement of muscle perfusion during exercise. J Appl Physiol 108:962–967
Hass CJ, Feigenbaum MS, Franklin BA (2001) Prescription of resistance training for healthy populations. Sports Med 31:953–964
Inagaki Y, Madarame H, Neya M, Ishii N (2011) Increase in serum growth hormone induced by electrical stimulation of muscle combined with blood flow restriction. Eur J Appl Physiol 111:2715–2721
Jones G, Burnham V, Francis P, Johnson MI (2018) An investigation into the effect of blood flow restriction on pain and muscular endurance in healthy human participants. J Phys Med 1(1):1–9
Kacin A, Strazar K (2011) Frequent low-load ischemic resistance exercise to failure enhances muscle oxygen delivery and endurance capacity. Scand J Med Sci Sports 21(6):231–241
Kilgas MA, McDaniel J, Stavres J et al (2019) Limb blood flow and tissue perfusion during exercise with blood flow restriction. Eur J Appl Physiol 119:377–387. https://doi.org/10.1007/s00421-018-4029-2
Kraemer WJ, Deschenes MR, Fleck SJ (1988) Physiological adaptations to resistance exercise. Sports Med 6:246–256
Laurentino GC, Ugrinowitsch C, Roschel H et al (2012) Strength training with blood flow restriction diminishes myostatin gene expression. Med Sci Sports Exerc 44:406–412
Lixandrão ME, Ugrinowitsch C, Laurentino G et al (2015) Effects of exercise intensity and occlusion pressure after 12 weeks of resistance training with blood-flow restriction. Eur J Appl Physiol 115:2471–2480. https://doi.org/10.1007/s00421-015-3253-2
Loenneke JP, Pujol TJ (2009) The use of occlusion training to produce muscle hypertrophy. Strength Cond J 31:77. https://doi.org/10.1519/SSC.0b013e3181a5a352
Loenneke JP, Fahs CA, Wilson JM, Bemben MG (2011) Blood flow restriction: the metabolite/volume threshold theory. Med Hypotheses 77:748–752. https://doi.org/10.1016/j.mehy.2011.07.029
MacDougall JD, Tuxen D, Sale DG et al (1985) Arterial blood pressure response to heavy resistance exercise. J Appl Physiol Bethesda Md 58:785–790. https://doi.org/10.1152/jappl.1985.58.3.785
Manini TM, Clark BC (2009) Blood flow restricted exercise and skeletal muscle health. Exerc Sport Sci Rev 37:78–85
Mouser JG, Dankel SJ, Jessee MB et al (2017a) A tale of three cuffs: the hemodynamics of blood flow restriction. Eur J Appl Physiol 117:1493–1499. https://doi.org/10.1007/s00421-017-3644-7
Mouser JG, Laurentino GC, Dankel SJ et al (2017b) Blood flow in humans following low-load exercise with and without blood flow restriction. Appl Physiol Nutr Metab Physiol Appl Nutr Metab 42:1165–1171. https://doi.org/10.1139/apnm-2017-0102
Mouser JG, Ade CJ, Black CD et al (2018) Brachial blood flow under relative levels of blood flow restriction is decreased in a nonlinear fashion. Clin Physiol Funct Imaging 38:425–430. https://doi.org/10.1111/cpf.12432
Mouser JG, Mattocks KT, Buckner SL et al (2019a) High-pressure blood flow restriction with very low load resistance training results in peripheral vascular adaptations similar to heavy resistance training. Physiol Meas 40:035003. https://doi.org/10.1088/1361-6579/ab0d2a
Mouser JG, Mattocks KT, Dankel SJ et al (2019b) Very-low-load resistance exercise in the upper body with and without blood flow restriction: cardiovascular outcomes. Appl Physiol Nutr Metab Physiol Appl Nutr Metab 44:288–292. https://doi.org/10.1139/apnm-2018-0325
Patterson SD, Ferguson RA (2010) Increase in calf post-occlusive blood flow and strength following short-term resistance exercise training with blood flow restriction in young women. Eur J Appl Physiol 108:1025–1033
Pearson SJ, Hussain SR (2015) A review on the mechanisms of blood-flow restriction resistance training-induced muscle hypertrophy. Sports Med 45:187–200. https://doi.org/10.1007/s40279-014-0264-9
Poton R, Polito MD (2016) Hemodynamic response to resistance exercise with and without blood flow restriction in healthy subjects. Clin Physiol Funct Imaging 36:231–236. https://doi.org/10.1111/cpf.12218
Renzi CP, Tanaka H, Sugawara J (2010) Effects of leg blood flow restriction during walking on cardiovascular function. Med Sci Sports Exerc 42:726–732. https://doi.org/10.1249/MSS.0b013e3181bdb454
Sallinen J, Fogelholm M, Volek JS et al (2007) Effects of strength training and reduced training on functional performance and metabolic health indicators in middle-aged men. Int J Sports Med 28:815–822. https://doi.org/10.1055/s-2007-964901
Scott BR, Loenneke JP, Slattery KM, Dascombe BJ (2016) Blood flow restricted exercise for athletes: a review of available evidence. J Sci Med Sport 19:360–367. https://doi.org/10.1016/j.jsams.2015.04.014
Spranger MD, Krishnan AC, Levy PD et al (2015) Blood flow restriction training and the exercise pressor reflex: a call for concern. Am J Physiol-Heart Circ Physiol 309:H1440–H1452. https://doi.org/10.1152/ajpheart.00208.2015
Stavres J, Singer TJ, Brochetti A et al (2018) The feasibility of blood flow restriction exercise in patients with incomplete spinal cord injury. PM&R 10:1368–1379. https://doi.org/10.1016/j.pmrj.2018.05.013
Takarada Y, Nakamura Y, Aruga S et al (2000a) Rapid increase in plasma growth hormone after low-intensity resistance exercise with vascular occlusion. J Appl Physiol 88:61–65. https://doi.org/10.1152/jappl.2000.88.1.61
Takarada Y, Takazawa H, Ishii N (2000b) Applications of vascular occlusion diminish disuse atrophy of knee extensor muscles. Med Sci Sports Exerc 32:2035–2039. https://doi.org/10.1097/00005768-200012000-00011
Trappe S, Williamson D, Godard M (2002) Maintenance of whole muscle strength and size following resistance training in older men. J Gerontol Ser A 57:B138–B143. https://doi.org/10.1093/gerona/57.4.B138
Yasuda T, Abe T, Brechue WF et al (2010a) Venous blood gas and metabolite response to low-intensity muscle contractions with external limb compression. Metabolism 59:1510–1519. https://doi.org/10.1016/j.metabol.2010.01.016
Yasuda T, Abe T, Brechue WF et al (2010b) Venous blood gas and metabolite response to low-intensity muscle contractions with external limb compression. Metabolism 59:1510–1519. https://doi.org/10.1016/j.metabol.2010.01.016
Yasuda T, Loenneke JP, Thiebaud RS, Abe T (2012) Effects of blood flow restricted low-intensity concentric or eccentric training on muscle size and strength. PLoS One 7:e52843. https://doi.org/10.1371/journal.pone.0052843
Zou K, Meador BM, Johnson B et al (2011) The α7β1-integrin increases muscle hypertrophy following multiple bouts of eccentric exercise. J Appl Physiol 111:1134–1141. https://doi.org/10.1152/japplphysiol.00081.2011
Acknowledgements
The authors would like to thank everyone who participated in this study.
Funding
No external funding was received for this work.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The author declares that they have no competing interests.
Additional information
Communicated by I. Mark Olfert.
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Singer, T.J., Stavres, J., Elmer, S.J. et al. Knee extension with blood flow restriction: Impact of cuff pressure on hemodynamics. Eur J Appl Physiol 120, 79–90 (2020). https://doi.org/10.1007/s00421-019-04250-2
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00421-019-04250-2