Abstract
Purpose
Endurance exercise training can ameliorate many cardiovascular and metabolic disorders and attenuate responses to inflammatory stimuli. The purpose of this study was to determine whether the angiogenic and pro-inflammatory cytokine response to acute endurance exercise differs between endurance-trained and sedentary young men.
Methods
Ten endurance-trained and ten sedentary healthy young men performed 30 min of treadmill running at 75 % VO2max with blood sampling before and after exercise. Plasma concentrations of tumor necrosis factor (TNF)-alpha, interleukin (IL)-8, IL-6, vascular endothelial growth factor (VEGF), basic fibroblast growth factor (bFGF), placental growth factor (PlGF), and soluble VEGF receptor-1 (sFlt-1) were measured by multiplex ELISA.
Results
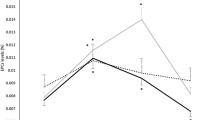
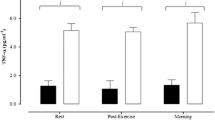
Acute exercise increased IL-6 by 165 % (P < 0.05), IL-8 by 32 % (P < 0.05), PlGF by ~16 % (P < 0.05), sFlt-1 by 36 % (P < 0.001), and tended to increase bFGF by ~25 % (P = 0.06) in main effects analyses. TNF-α and VEGF did not change significantly with exercise in either group. Contrary to our hypothesis, there were no significant differences in TNF-α, IL-6, VEGF, bFGF, PlGF, or sFlt-1 between groups before or after acute exercise; however, there was a tendency for IL-8 concentrations to be higher in endurance-trained subjects compared to sedentary subjects (P = 0.06).
Conclusions
These results indicate that 30 min of treadmill running at 75 % VO2max produces a systemic angiogenic and inflammatory reaction, but endurance exercise training does not appear to significantly alter these responses in healthy young men.


Similar content being viewed by others
Abbreviations
- ACSM:
-
American College of Sports Medicine
- bFGF:
-
Basic fibroblast growth factor
- BMI:
-
Body mass index
- CV:
-
Cardiovascular
- ELISA:
-
Enzyme-linked immunosorbent assay
- IL:
-
Interleukin
- NSAIDs:
-
Non-steroidal anti-inflammatory drugs
- PlGF:
-
Placental growth factor
- sFlt-1:
-
Soluble fms-like tyrosine kinase-1
- TNF-α:
-
Tumor necrosis factor-alpha
- VEGF:
-
Vascular endothelial growth factor
- VO2max :
-
Maximal oxygen uptake
References
Adams V (2004) Increase of circulating endothelial progenitor cells in patients with coronary artery disease after exercise-induced ischemia. Arterioscler Thromb Vasc Biol 24:684–690. doi:10.1161/01.ATV.0000124104.23702.a0
Adams V, Linke A, Breuckmann F et al (2008) Circulating progenitor cells decrease immediately after marathon race in advanced-age marathon runners. Eur J Cardiovasc Prev Rehabil 15:602–607. doi:10.1097/HJR.0b013e328309c756
Ambarish V, Chandrashekara S, Suresh KP (2012) Moderate regular exercises reduce inflammatory response for physical stress. Indian J Physiol Pharmacol 56:7–14
American College of Sports Medicine (2009) ACSM’s guidelines for exercise testing and prescription, 8th edn. Lippincott Williams & Wilkins, Baltimore
American College of Sports Medicine (2012) ACSM’s health/fitness facility standards and guidelines, 4th edn. Human Kinetics, Champaign
Bailey AP, Shparago M, Gu J-W (2006) Exercise increases soluble vascular endothelial growth factor receptor-1 (sFlt-1) in circulation of healthy volunteers. Med Sci Monit 12:CR45–CR50
Blann AD, Belgore FM, McCollum CN et al (2002) Vascular endothelial growth factor and its receptor, Flt-1, in the plasma of patients with coronary or peripheral atherosclerosis, or Type II diabetes. Clin Sci 102:187–194
Croft L, Bartlett JD, MacLaren DPM et al (2009) High-intensity interval training attenuates the exercise-induced increase in plasma IL-6 in response to acute exercise. Appl Physiol Nutr Metab 34:1098–1107. doi:10.1139/H09-117
Dewerchin M, Carmeliet P (2012) PlGF: a multitasking cytokine with disease-restricted Activity. Cold Spring Harb Perspect Med 2:a011056. doi:10.1101/cshperspect.a011056
Dill DB, Costill DL (1974) Calculation of percentage changes in volumes of blood, plasma, and red cells in dehydration. J Appl Physiol 37:247–248
Febbraio MA, Pedersen BK (2002) Muscle-derived interleukin-6: mechanisms for activation and possible biological roles. FASEB J 16:1335–1347. doi:10.1096/fj.01-0876rev
Fischer CP (2004) Endurance training reduces the contraction-induced interleukin-6 mRNA expression in human skeletal muscle. Am J Physiol Endocrinol Metab 287:1189–1194. doi:10.1152/ajpendo.00206.2004
Gigante B, Tarsitano M, Cimini V et al (2004) Placenta growth factor is not required for exercise-induced angiogenesis. Angiogenesis 7:277–284. doi:10.1007/s10456-004-4179-1
Gokhale R, Chandrashekara S, Vasanthakumar KC (2007) Cytokine response to strenuous exercise in athletes and non-athletes—an adaptive response. Cytokine 40:123–127. doi:10.1016/j.cyto.2007.08.006
Gomes EC, Silva AN, de Oliveira MR (2012) Oxidants, antioxidants, and the beneficial roles of exercise-induced production of reactive species. Oxid Med Cell Longev 2012:1–12. doi:10.1152/japplphysiol.01202.2006
Gu JW, Santiago D, Olowe Y, Weinberger J (1997) Basic fibroblast growth factor as a biochemical marker of exercise-induced ischemia. Circulation 95:1165–1168
Heidemann J (2002) Angiogenic effects of interleukin 8 (CXCL8) in human intestinal microvascular endothelial cells are mediated by CXCR2. J Biol Chem 278:8508–8515. doi:10.1074/jbc.M208231200
Hoier B, Passos M, Bangsbo J, Hellsten Y (2013) Intense intermittent exercise provides weak stimulus for vascular endothelial growth factor secretion and capillary growth in skeletal muscle. Exp Physiol 98:585–597. doi:10.1113/expphysiol.2012.067967
Jackson AS, Pollock ML (2004) Generalized equations for predicting body density of men. 1978. Br J Nutr 91:161–168
Jenkins NT, Landers RQ, Prior SJ et al (2011) Effects of acute and chronic endurance exercise on intracellular nitric oxide and superoxide in circulating CD34+ and CD34− cells. J Appl Physiol 111:929–937. doi:10.1152/japplphysiol.00541.2011
Jensen L (2004) Effect of high intensity training on capillarization and presence of angiogenic factors in human skeletal muscle. J Physiol (Lond) 557:571–582. doi:10.1113/jphysiol.2003.057711
Keller C (2005) Effect of exercise, training, and glycogen availability on IL-6 receptor expression in human skeletal muscle. J Appl Physiol 99:2075–2079. doi:10.1152/japplphysiol.00590.2005
Kraus RM (2004) Circulating plasma VEGF response to exercise in sedentary and endurance-trained men. J Appl Physiol 96:1445–1450. doi:10.1152/japplphysiol.01031.2003
Lieb W, Safa R, Benjamin EJ et al (2009) Vascular endothelial growth factor, its soluble receptor, and hepatocyte growth factor: clinical and genetic correlates and association with vascular function. Eur Heart J 30:1121–1127. doi:10.1093/eurheartj/ehp007
Luttun A, Brusselmans K, Fukao H et al (2002) Loss of placental growth factor protects mice against vascular permeability in pathological conditions. Biochem Biophys Res Commun 295:428–434
Mobius-Winkler S, Hilberg T, Menzel K et al (2009) Time-dependent mobilization of circulating progenitor cells during strenuous exercise in healthy individuals. J Appl Physiol 107:1943–1950. doi:10.1152/japplphysiol.00532.2009
Nielsen AR, Pedersen BK (2007) The biological roles of exercise-induced cytokines: IL-6, IL-8, and IL-15. Appl Physiol Nutr Metab 32:833–839. doi:10.1139/H07-054
Nieman DC, Henson DA, Davis JM et al (2006) Blood leukocyte mRNA expression for IL-10, IL-1Ra, and IL-8, but not IL-6, increases after exercise. J Interferon Cytokine Res 26:668–674. doi:10.1089/jir.2006.26.668
Nieman DC, Konrad M, Henson DA et al (2012) Variance in the acute inflammatory response to prolonged cycling is linked to exercise intensity. J Interferon Cytokine Res 32:12–17. doi:10.1089/jir2011.0038
Ostrowski K, Hermann C, Bangash A et al (1998) A trauma-like elevation of plasma cytokines in humans in response to treadmill running. J Physiol (Lond) 513(Pt 3):889–894
Pedersen BK, Fischer CP (2007) Physiological roles of muscle-derived interleukin-6 in response to exercise. Curr Opin Clin Nutr Metab Care 10:265–271. doi:10.1097/MCO.0b013e3280ebb5b3
Popa C, Netea MG, van Riel PLCM et al (2007) The role of TNF- in chronic inflammatory conditions, intermediary metabolism, and cardiovascular risk. J Lipid Res 48:751–762. doi:10.1194/jlr.R600021-JLR200
Ronsen O, Lea T, Bahr R, Pedersen BK (2002) Enhanced plasma IL-6 and IL-1ra responses to repeated vs. single bouts of prolonged cycling in elite athletes. J Appl Physiol 92:2547–2553. doi:10.1152/japplphysiol.01263.2001
Scott JPR, Sale C, Greeves JP et al (2011) Effect of exercise intensity on the cytokine response to an acute bout of running. Med Sci Sports Exerc 43:2297–2306. doi:10.1249/MSS.0b013e31822113a9
Scott JPR, Sale C, Greeves JP et al (2013) Cytokine response to acute running in recreationally-active and endurance-trained men. Eur J Appl Physiol. doi:10.1007/s00421-013-2615-x
Tanaka T, Kanda T, McManus BM et al (2001) Overexpression of interleukin-6 aggravates viral myocarditis: impaired increase in tumor necrosis factor-alpha. J Mol Cell Cardiol 33:1627–1635. doi:10.1006/jmcc2001.1428
Trøseid M (2004) Exercise reduces plasma levels of the chemokines MCP-1 and IL-8 in subjects with the metabolic syndrome. Eur Heart J 25:349–355. doi:10.1016/j.ehj.2003.12.006
Vassilakopoulos T, Karatza M-H, Katsaounou P et al (2002) Antioxidants attenuate the plasma cytokine response to exercise in humans. J Appl Physiol 94:1025–1032. doi:10.1152/japplphysiol.00735.2002
Wahl P, Zinner C, Achtzehn S et al (2010) Effects of acid–base balance and high or low intensity exercise on VEGF and bFGF. Eur J Appl Physiol 111:1405–1413. doi:10.1007/s00421-010-1767-1
Weissgerber TL, Davies GAL, Roberts JM (2010) Modification of angiogenic factors by regular and acute exercise during pregnancy. J Appl Physiol 108:1217–1223. doi:10.1152/japplphysiol.00008.2010
Wellen KE, Hotamisligil GS (2005) Inflammation, stress, and diabetes. J Clin Invest 115:1111–1119. doi:10.1172/JCI25102DS1
Acknowledgments
This study was supported by the University of Maryland’s Kinesiology Graduate Research Initiative Fund (to NTJ), the Baltimore Veterans Affairs Medical Center Geriatric Research, Education and Clinical Center (GRECC), and the University of Maryland Claude D. Pepper Center (P30-AG028747). NTJ and RQL were supported by T32-AG200068 (to JMH), and SJP was supported by a Veterans Affairs Career Development Award and is currently supported by K23-AG040775. The current affiliation for NTJ is the Department of Kinesiology, University of Georgia, Athens, GA.
Conflict of interest
The authors have no conflicts of interest to declare.
Author information
Authors and Affiliations
Corresponding author
Additional information
Communicated by Fabio Fischetti.
Rights and permissions
About this article
Cite this article
Landers-Ramos, R.Q., Jenkins, N.T., Spangenburg, E.E. et al. Circulating angiogenic and inflammatory cytokine responses to acute aerobic exercise in trained and sedentary young men. Eur J Appl Physiol 114, 1377–1384 (2014). https://doi.org/10.1007/s00421-014-2861-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00421-014-2861-6