Abstract
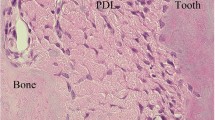
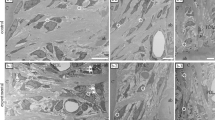
Reference data are lacking on the periodontal ligament and the gingival tissue of the rat model, which would be useful for studies of new medical or biomaterial periodontal treatments. The objective of the current study was to propose cellular and collagen reference values of gingival and periodontal ligament tissues in rat, using a simple and reliable quantitative method after decalcification. Mandibular samples of ten adult Sprague–Dawley rats were used. Mild decalcification was carried out using ethylenediaminetetraacetic acid (EDTA) to preserve the morphology of tissues. Half of the samples were decalcified and the other half were not. The gingiva and the periodontal ligament were analyzed. Descriptive histology and computer-assisted image analysis were performed. The data showed that qualitatively, cellular and extracellular matrix morphologies were well preserved compared to non-decalcified periodontal soft tissue biopsies. Histomorphometrically, constitutive cellularity and the total amount of native collagen, collagen directionality and collagen anisotropy in both experimental conditions did not significantly differ. Taken together, these results suggested that EDTA decalcification did not negatively affect the studied endpoints. Moreover, this mild decalcification method allowed in situ maintenance of the periodontal soft and hard tissue integrity. The structural and compositional computerized assessment performed in the healthy periodontal soft tissue could provide reference values that will be required for future assessment on the effects of pathological, reparative and regenerative processes in rat periodontal soft tissues.


Similar content being viewed by others
References
Almeida T, Valverde T, Martins-Júnior P et al (2015) Morphological and quantitative study of collagen fibers in healthy and diseased human gingival tissues. Romanian J Morphol Embryol Rev Roum Morphol Embryol 56:33–40
Alves A, Gritsch K, Sirieix C et al (2015) Computerized histomorphometric study of the splenic collagen polymorphism: a control-tissue for polarization microscopy: Histomorphometric study of the splenic collagen. Microsc Res Tech 78:900–907. https://doi.org/10.1002/jemt.22553
Alves A, Attik N, Bayon Y et al (2018) Devising tissue ingrowth metrics: a contribution to the computational characterization of engineered soft tissue healing. Biomed Mater 13(3):035010. https://doi.org/10.1088/1748-605X/aaa9d4
Basiouny HS, Salama NM, Maadawi ZME, Farag EA (2013) Effect of bone marrow derived mesenchymal stem cells on healing of induced full-thickness skin wounds in albino rat. Int J Stem Cells 6:12–25
Bourgeois D, Bouchard P, Mattout C (2007) Epidemiology of periodontal status in dentate adults in France, 2002–2003. J Periodontal Res 42:219–227. https://doi.org/10.1111/j.1600-0765.2006.00936.x
Bourque WT, Gross M, Hall BK (1993) A histological processing technique that preserves the integrity of calcified tissues (bone, enamel), yolky amphibian embryos, and growth factor antigens in skeletal tissue. J Histochem Cytochem 41:1429–1434
Campos AC, Groth AK, Branco AB (2008) Assessment and nutritional aspects of wound healing. Curr Opin Clin Nutr Metab Care 11:281–288. https://doi.org/10.1097/MCO.0b013e3282fbd35a
Castania VA, de Souza da Silveira JW, Issy AC et al (2015) Advantages of a combined method of decalcification compared to EDTA: advantages of a combined method. Microsc Res Tech 78:111–118. https://doi.org/10.1002/jemt.22451
Choi S-E, Hong SW, Yoon SO (2015) Proposal of an appropriate decalcification method of bone marrow biopsy specimens in the era of expanding genetic molecular study. J Pathol Transl Med 49:236–242. https://doi.org/10.4132/jptm.2015.03.16
dos Santos Neves J, Omar NF, Narvaes EAO et al (2011) Influence of different decalcifying agents on EGF and EGFR immunostaining. Acta Histochem 113:484–488. https://doi.org/10.1016/j.acthis.2010.04.006
El Sadik AO, El Ghamrawy TA, Abd El-Galil TI (2015) The effect of mesenchymal stem cells and chitosan gel on full thickness skin wound healing in albino rats: histological, immunohistochemical and fluorescent study. PloS One 10:e0137544. https://doi.org/10.1371/journal.pone.0137544
Elburki MS, Moore DD, Terezakis NG et al (2016) A novel chemically modified curcumin reduces inflammation-mediated connective tissue breakdown in a rat model of diabetes: periodontal and systemic effects. J Periodontal Res. https://doi.org/10.1111/jre.12381
Farina R, Simonelli A, Rizzi A et al (2013) Early postoperative healing following buccal single flap approach to access intraosseous periodontal defects. Clin Oral Investig 17:1573–1583. https://doi.org/10.1007/s00784-012-0838-6
Frank JD, Balena R, Masarachia P et al (1993) The effects of three different demineralization agents on osteopontin localization in adult rat bone using immunohistochemistry. Histochemistry 99:295–301
Gajendrareddy PK, Junges R, Cygan G et al (2016) Increased oxygen exposure alters collagen expression and tissue architecture during ligature-induced periodontitis. J Periodontal Res. https://doi.org/10.1111/jre.12408
Gazoti Debessa CR, Mesiano Maifrino LB, Rodrigues de Souza R (2001) Age related changes of the collagen network of the human heart. Mech Ageing Dev 122:1049–1058
Genna F (2006) A micromechanically-based, three-dimensional interface finite element for the modelling of the periodontal ligament. Comput Methods Biomech Biomed Engin 9:243–256. https://doi.org/10.1080/10255840600733364
Guibas GV, Lakis S, Gkimpas C et al (2014) Efficiency of different decalcification protocols for nasal osseous structures in a rat experimental model of allergic rhinitis, and their effects on epithelial histology: an attempt at standardization. Exp Toxicol Pathol 66:469–475. https://doi.org/10.1016/j.etp.2014.09.001
Gupta S (2014) Qualitative histological evaluation of hard and soft tissue components of human permanent teeth using various decalcifying agents—a comparative study. J Clin Diagn Res. https://doi.org/10.7860/jcdr/2014/10195.4874
Hammouda O, Seif M, Brinkley B et al (1980) Gingival matrix collagen in chronic periodontitis. J Dent Res 59:17–22
Jacob SP, Nath S (2013) Rat gingival model for testing drugs influencing inflammation. IeJSME 7:8–16
Karsdal MA, Genovese F, Madsen EA et al (2016) Collagen and tissue turnover as a function of age: implications for fibrosis. J Hepatol 64:103–109. https://doi.org/10.1016/j.jhep.2015.08.014
Kim YS, Kang SJ, Kim JW et al (2012) Effects of polycan, a β-glucan, on experimental periodontitis and alveolar bone loss in Sprague–Dawley rats: protective effects of β-glucan. J Periodontal Res 47:800–810. https://doi.org/10.1111/j.1600-0765.2012.01502.x
Kraft-Neumärker M, Lorenz K, Koch R et al (2012) Full-mouth profile of active MMP-8 in periodontitis patients. J Periodontal Res 47:121–128. https://doi.org/10.1111/j.1600-0765.2011.01416.x
Kudalkar M, Nayak A, Bhat K, Nayak R (2014) Effect of Azadirachta indica (Neem) and Aloe vera as compared to subantimicrobial dose doxycycline on matrix metalloproteinases (MMP)-2 and MMP-9: an in vitro study. AYU Int Q J Res Ayurveda 35:85. https://doi.org/10.4103/0974-8520.141947
Lima GMG, Corazza BJM, Moraes RM et al (2016) The effect of an inhibitor of gut serotonin (LP533401) during the induction of periodontal disease. J Periodontal Res 51:661–668. https://doi.org/10.1111/jre.12346
Lin JD, Lee J, Özcoban H et al (2014) Biomechanical adaptation of the bone-periodontal ligament (PDL)-tooth fibrous joint as a consequence of disease. J Biomech 47:2102–2114. https://doi.org/10.1016/j.jbiomech.2013.10.059
Mello ML, Vidal BC, Valdrighi L (1974) Anisotropy and isoelectrical point determinations on collagen bundles of the rat periodontal fibers. Histochemistry 42:163–174
Mukai K, Yoshimura S, Anzai M (1986) Effects of decalcification on immunoperoxidase staining. Am J Surg Pathol 10:413–419
Nagasupriya A, Rao DB, Ravikanth M et al (2014) Immunohistochemical expression of matrix metalloproteinase 13 in chronic periodontitis. Int J Periodontics Restor Dent 34:e79–e84
Natali AN, Pavan PG, Carniel EL, Dorow C (2004) Viscoelastic response of the periodontal ligament: an experimental-numerical analysis. Connect Tissue Res 45:222–230. https://doi.org/10.1080/03008200490885742
Pamuk F, Cetinkaya BO, Ayas B et al (2015) Evaluation of gingival alterations in rats medicated with cyclosporine A, tacrolimus and sirolimus: a stereological study. J Periodontal Res 50:629–636. https://doi.org/10.1111/jre.12243
Pettinicchio M, Traini T, Murmura G et al (2012) Histologic and histomorphometric results of three bone graft substitutes after sinus augmentation in humans. Clin Oral Investig 16:45–53. https://doi.org/10.1007/s00784-010-0484-9
Pickering JG, Boughner DR (1991) Quantitative assessment of the age of fibrotic lesions using polarized light microscopy and digital image analysis. Am J Pathol 138:1225–1231
Pihlstrom BL, Michalowicz BS, Johnson NW (2005) Periodontal diseases. Lancet 366:1809–1820. https://doi.org/10.1016/S0140-6736(05)67728-8
Polyakova V, Loeffler I, Hein S et al (2011) Fibrosis in endstage human heart failure: severe changes in collagen metabolism and MMP/TIMP profiles. Int J Cardiol 151:18–33. https://doi.org/10.1016/j.ijcard.2010.04.053
Ricard-Blum S (2011) The collagen family. Cold Spring Harb Perspect Biol 3:a004978. https://doi.org/10.1101/cshperspect.a004978
Romanos GE, Schröter-Kermani C, Hinz N et al (1991) Immunohistochemical localization of collagenous components in healthy periodontal tissues of the rat and marmoset (Callithrix jacchus). II. Distribution of collagen types IV, V and VI. J Periodontal Res 26:323–332
Romanos GE, Schröter-Kermani C, Hinz N et al (1992) Immunohistochemical localization of collagenous components in healthy periodontal tissues of the rat and marmoset (Callithrix jacchus). I. Distribution of collagen types I and III. J Periodontal Res 27:101–110
Sanjai K, Patil A, Jayaram S et al (2012) Evaluation and comparison of decalcification agents on the human teeth. J Oral Maxillofac Pathol 16:222. https://doi.org/10.4103/0973-029X.99070
Takamori Y, Atsuta I, Nakamura H et al (2016) Histopathological comparison of the onset of peri-implantitis and periodontitis in rats. Clin Oral Implants Res. https://doi.org/10.1111/clr.12777
Villa MM, Wang L, Huang J et al (2013) Visualizing osteogenesis in vivo within a cell-scaffold construct for bone tissue engineering using two-photon microscopy. Tissue Eng Part C Methods 19:839–849. https://doi.org/10.1089/ten.TEC.2012.0490
Vogel HG (1980) Influence of maturation and aging on mechanical and biochemical properties of connective tissue in rats. Mech Ageing Dev 14:283–292
Yang D, Liu R, Liu L et al (2017) Involvement of CD147 in alveolar bone remodeling and soft tissue degradation in experimental periodontitis. J Periodontal Res. https://doi.org/10.1111/jre.12435
Yates CC, Hebda P, Wells A (2012) Skin wound healing and scarring: fetal wounds and regenerative restitution. Birth Defects Res Part C Embryo Today Rev 96:325–333. https://doi.org/10.1002/bdrc.21024
Acknowledgements
This work was partly financially supported by the Fonds unique interministériel (FUI No AAP:15-Project No F1312025 V) within the REVAMED (Régénération et Evaluation des Dispositifs Médicaux) project. The experimental rats have been obtained from a collaborative study performed with the partnership of Institut Bourgelat (Marcy l’Etoile, France). The authors gratefully acknowledge Dr. Elodie Devron Gaillot, Pathologist, for reviewing the slides as independent reader and Mr. Paul Bonijol, Engineer, for his contribution in the adaptation of part of the algorithms of this project.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that there is no conflict of interest, financial or otherwise regarding the publication of this paper.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Alves, A., Attik, N., Wirth, C. et al. Cellular and collagen reference values of gingival and periodontal ligament tissues in rats: a pilot study. Histochem Cell Biol 152, 145–153 (2019). https://doi.org/10.1007/s00418-019-01789-1
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00418-019-01789-1