Abstract
Background
To study the roles of preoperative retinal sensitivity and fixation exams in predicting the long-term prognosis of idiopathic macular hole (IMH) patients after successful vitrectomy.
Methods
A total of 39 IMH patients (39 eyes) were included in this prospective cohort case series study. Twenty-three gauge pars plana vitrectomy was performed on each patient. Results of best-corrected visual acuity (BCVA), macular hole diameter, MP − 1 microperimetry (MP − 1) tests, and continuity of the photoreceptor inner and outer segment (IS/OS) junction were recorded for analysis.
Results
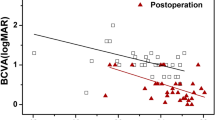
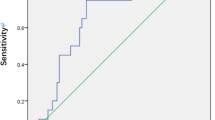
Postoperative BCVA at 12 months was significantly correlated with macular hole diameters (p < 0.05), preoperative BCVA (p = 0.020), mean retinal sensitivity (p < 0.001), and fixation location percentage (p < 0.001). However, merely preoperative mean retinal sensitivity (r = 0.5448, p < 0.001) and fixation location percentage (r = 0.5624, p < 0.001) were suggested to be quantitatively predictive for the visual prognosis by multiple stepwise linear regression analysis. Moreover, patients that had smaller hole sizes (p < 0.01), better mean retinal sensitivity (p = 0.003), higher fixation quality scores, and higher fixation location percentage (p = 0.008) before surgery were prone to get continuous IS/OS junction 12 months after surgery.
Conclusions
MP-1 exams evaluate the dysfunctional hole margin and thus provide more comprehensive information of the preoperative visual function of IMH patients. Both mean retinal sensitivity and fixation behaviors are ideal measurements in predicting the prognosis after successful macular hole surgery.








Similar content being viewed by others
References
McDonnell PJ, Fine SL, Hillis AI (1982) Clinical features of idiopathic macular cysts and holes. Am J Ophthalmol 93:777–786
Gass JD (1988) Idiopathic senile macular hole. Its early stages and pathogenesis. Arch Ophthalmol 106:629–639
Wittich W, Overbury O, Kapusta MA, Faubert J (2005) Visual function assessment and metamorphopsia after macular hole surgery. Ophthalmic Physiol Opt 25:534–542
Grigoropoulos VG, Theodossiadis GP, Theodossiadis PG Association of the preoperative photoreceptor layer defect as assessed by optical coherence tomography with the functional outcome after macular hole closure: a long follow-up study. Ophthalmologica 225:47–54
Kelly NE, Wendel RT (1991) Vitreous surgery for idiopathic macular holes. Results of a pilot study. Arch Ophthalmol 109:654–659
Passemard M, Yakoubi Y, Muselier A, Hubert I, Guillaubey A, Bron AM, Berrod JP, Creuzot-Garcher C Long-term outcome of idiopathic macular hole surgery. Am J Ophthalmol 149:120–126
Haritoglou C, Gass CA, Schaumberger M, Ehrt O, Gandorfer A, Kampik A (2001) Macular changes after peeling of the internal limiting membrane in macular hole surgery. Am J Ophthalmol 132:363–368
Tranos PG, Ghazi-Nouri SM, Rubin GS, Adams ZC, Charteris DG (2004) Visual function and subjective perception of visual ability after macular hole surgery. Am J Ophthalmol 138:995–1002
Ullrich S, Haritoglou C, Gass C, Schaumberger M, Ulbig MW, Kampik A (2002) Macular hole size as a prognostic factor in macular hole surgery. Br J Ophthalmol 86:390–393
Miura G, Mizunoya S, Arai M, Hayashi M, Yamamoto S (2007) Early postoperative macular morphology and functional outcomes after successful macular hole surgery. Retina 27:165–168
Uemoto R, Yamamoto S, Aoki T, Tsukahara I, Yamamoto T, Takeuchi S (2002) Macular configuration determined by optical coherence tomography after idiopathic macular hole surgery with or without internal limiting membrane peeling. Br J Ophthalmol 86:1240–1242
Ryan EH Jr, Gilbert HD (1994) Results of surgical treatment of recent-onset full-thickness idiopathic macular holes. Arch Ophthalmol 112:1545–1553
Tognetto D, Grandin R, Sanguinetti G, Minutola D, Di Nicola M, Di Mascio R, Ravalico G (2006) Internal limiting membrane removal during macular hole surgery: results of a multicenter retrospective study. Ophthalmology 113:1401–1410
Willis AW, Garcia-Cosio JF (1996) Macular hole surgery. Comparison of longstanding versus recent macular holes. Ophthalmology 103:1811–1814
Freeman WR, Azen SP, Kim JW, El-Haig W, Mishell DR 3rd, Bailey I (1997) Vitrectomy for the treatment of full-thickness stage 3 or 4 macular holes. Results of a multicentered randomized clinical trial. The Vitrectomy for Treatment of Macular Hole Study Group. Arch Ophthalmol 115:11–21
Roth DB, Smiddy WE, Feuer W (1997) Vitreous surgery for chronic macular holes. Ophthalmology 104:2047–2052
Bainbridge J, Herbert E, Gregor Z (2008) Macular holes: vitreoretinal relationships and surgical approaches. Eye (Lond) 22:1301–1309
Richter-Mueksch S, Vecsei-Marlovits PV, Sacu SG, Kiss CG, Weingessel B, Schmidt-Erfurth U (2007) Functional macular mapping in patients with vitreomacular pathologic features before and after surgery. Am J Ophthalmol 144:23–31
Vujosevic S, Midena E, Pilotto E, Radin PP, Chiesa L, Cavarzeran F (2006) Diabetic macular edema: correlation between microperimetry and optical coherence tomography findings. Invest Ophthalmol Vis Sci 47:3044–3051
Weingessel B, Sacu S, Vecsei-Marlovits PV, Weingessel A, Richter-Mueksch S, Schmidt-Erfurth U (2009) Interexaminer and intraexaminer reliability of the microperimeter MP-1. Eye (Lond) 23:1052–1058
Zou H, Zhang X, Xu X, Yu S (2006) Quantitative in vivo retinal thickness measurement in Chinese healthy subjects with retinal thickness analyzer. Invest Ophthalmol Vis Sci 47:341–347
Ozdemir H, Karacorlu M, Senturk F, Karacorlu SA, Uysal O (2010) Retinal sensitivity and fixation changes 1 year after triamcinolone acetonide assisted internal limiting membrane peeling for macular hole surgery—a MP-1 microperimetric study. Acta Ophthalmol 88:e222–227
Tarita-Nistor L, Gonzalez EG, Mandelcorn MS, Lillakas L, Steinbach MJ (2009) Fixation stability, fixation location, and visual acuity after successful macular hole surgery. Invest Ophthalmol Vis Sci 50:84–89
Sano M, Shimoda Y, Hashimoto H, Kishi S (2009) Restored photoreceptor outer segment and visual recovery after macular hole closure. Am J Ophthalmol 147(313–318):e311
Fujii GY, de Juan E Jr, Sunness J, Humayun MS, Pieramici DJ, Chang TS (2002) Patient selection for macular translocation surgery using the scanning laser ophthalmoscope. Ophthalmology 109:1737–1744
Gass JD (1995) Reappraisal of biomicroscopic classification of stages of development of a macular hole. Am J Ophthalmol 119:752–759
Gass JD (1999) Müller cell cone, an overlooked part of the anatomy of the fovea centralis: hypotheses concerning its role in the pathogenesis of macular hole and foveomacualr retinoschisis. Arch Ophthalmol 117:821–823
Tanner V, Williamson TH (2000) Watzke-Allen slit beam test in macular holes confirmed by optical coherence tomography. Arch Ophthalmol 118:1059–1063
Nakabayashi M, Fujikado T, Ohji M, Saito Y, Tano Y (2000) Fixation patterns of idiopathic macular holes after vitreous surgery. Retina 20:170–175
White JM, Bedell HE (1990) The oculomotor reference in humans with bilateral macular disease. Invest Ophthalmol Vis Sci 31:1149–1161
Fletcher DC, Schuchard RA (1997) Preferred retinal loci relationship to macular scotomas in a low-vision population. Ophthalmology 104:632–638
Ko TH, Witkin AJ, Fujimoto JG, Chan A, Rogers AH, Baumal CR, Schuman JS, Drexler W, Reichel E, Duker JS (2006) Ultrahigh-resolution optical coherence tomography of surgically closed macular holes. Arch Ophthalmol 124:827–836
Frangieh GT, Green WR, Engel HM (1981) A histopathologic study of macular cysts and holes. Retina 1:311–336
Acknowledgments
Financial disclosure
The author(s) have no proprietary or commercial interests in any materials discussed in this article.
Funding/Support
This study was supported by grant G.Z.X./No. 2007CB512205 from the Ministry of Science and Technology of the People’s Republic of China, by grant G.Z.X./No. 09XD1400900 from the Science and Technology commission of Shanghai Municipality, by grant G.Z.X./No. 30872825 from National Natural Science Foundation of China, and by grant D.G./No. 30801267 from National Natural Science Foundation of China.
Contributions of authors
Involved in conception and design of study (Z.S., D.G., C.J., G.X.); Analysis and interpretation of data (Z.S., D.G., C.J., M.W.); Writing the article (G.X., Z.S.); Critical revision of the article (G.X., A.S., A.C.J.); Final approval of the article (Z.S., D.G., G.X.); Data collection (Z.S.); Patients referring (G.X.); Statistical expertise (Z.S.); Obtaining funding (G.X., D.G.); and Literature search (Z.S., D.G.).
IRB Approval
Approval for data collection and analysis was obtained from the Institutional Review Board of Eye and ENT Hospital of Fudan University (NO. KJ2009-16).
Author information
Authors and Affiliations
Corresponding author
Additional information
Zhongcui Sun and Dekang Gan contributed equally to this work.
The authors have full control of all primary data and agree to allow Graefes Archive for Clinical and Experimental Ophthalmology to review their data upon request.
Rights and permissions
About this article
Cite this article
Sun, Z., Gan, D., Jiang, C. et al. Effect of preoperative retinal sensitivity and fixation on long-term prognosis for idiopathic macular holes. Graefes Arch Clin Exp Ophthalmol 250, 1587–1596 (2012). https://doi.org/10.1007/s00417-012-1997-5
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00417-012-1997-5