Abstract
Objective
To identify the characteristics of patients with myopic choroidal neovascularization (CNV) who had a favorable visual prognosis without treatment.
Methods
We reviewed the medical records of 52 consecutive patients (57 eyes) with myopic CNV who were followed for at least 5 years after the onset of CNV. Clinical characteristics (patient age, CNV size and location, visual acuity at onset, chorioretinal atrophy development around CNV, and degree of myopia) were compared between patients whose visual acuity 5 years after CNV onset was better than 20/40 and those whose visual acuity was worse than 20/200.
Results
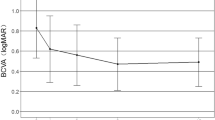
Among 57 eyes, eight eyes (14.0%; 8 patients) had a final visual acuity better than 20/40. On the other hand, 37 eyes (64.9%; 33 patients) had a final visual acuity worse than 20/200. Statistical analysis revealed that the patients with a good prognosis (final visual acuity better than 20/40) were significantly younger, had significantly smaller CNV, and significantly better initial visual acuity (Mann–Whitney U-test, p<0.05). Juxtafoveal CNV was more frequently observed in patients with a good prognosis than in those with a poor prognosis (Fisher’s exact probability test, p<0.05). Only one patient (12.5%) in the good prognosis group developed a very limited area of chorioretinal atrophy around the regressed CNV, while 91.9% of the patients in the poor prognosis group developed chorioretinal atrophy. Refractive status and the axial length measurements did not differ between the two groups.
Conclusions
Some young patients with myopic CNV retain favorable vision over the long term without active treatment. These information might be useful to predict the visual outcome of patients with myopic CNV.


Similar content being viewed by others
References
Avila MP, Weiter JJ, Jalkh AE et al (1984) Natural history of choroidal neovascularization in degenerative myopia. Ophthalmology 91:1573–1581
Cohen SY, Laroche A, Leguen Y, Soubrane G, Coscas GJ (1996) Etiology of choroidal neovascularization in young patients. Ophthalmology 103:1241–1244
Curtin BJ (1985) Basic science and clinical management. In: Curtin BJ (ed) The Myopias. Harper & Row, Philadelphia, pp 237–245
Delori FC, Goger DG, Dorey CK (2001) Age-related accumulation and spatial distribution of lipofuscin in RPE of normal subjects. Invest Ophthalmol Vis Sci 42:1855–1866
Docchio F (1989) Ocular fluorometry: principles, fluorophores, instrumentation, and clinical applications. Lasers Surg Med 9:515–532
Espinosa-Heidmann DG, Suner I, Hernandez EP et al (2002) Age as an independent risk factor for severity of experimental choroidal neovascularization. Invest Ophthalmol Vis Sci 43:1567–1573
Ghafour IM, Allan D, Foulds WS (1983) Common causes of blindness and visual handicap in the West of Scotland. Br J Ophthalmol 67:209–213
Harman AM, Hoskins R, Beazley LD (1999) Experimental eye enlargement in mature animals changes the retinal pigment epithelium. Vis Neurosci 16:619–628
Hayasaka S, Uchida M, Setogawa T (1990) Subretinal hemorrhages with or without choroidal neovascularization in the maculas of patients with pathologic myopia. Graefes Arch Clin Exp Ophthalmol 228:277–280
Hotchkiss ML, Fine SL (1981) Pathologic myopia and choroidal neovascularization. Am J Ophthalmol 91:177–183
Kitaya N, Ishiko S, Abiko T et al (2000) Changes in blood–retinal barrier permeability in form deprivation myopia in tree shrews. Vision Res 40:2369–2377
Miller H, Miller B, Ryan SJ (1986) The role of retinal pigment epithelium in the involution of subretinal neovascularization. Invest Ophthalmol Vis Sci 27:1644–1652
Miller H, Miller B, Ishibashi T, Ryan SJ (1990) Pathogenesis of laser-induced choroidal subretinal neovascularization. Invest Ophthalmol Vis Sci 31:899–908
Pruett RC (1994) Pathologic myopia. In: Albert DM and Jakobiec FA (eds) Principles and practice of ophthalmology. Saunders, Philadelphia, pp 878–882
Sperduto RD, Seigel D, Roberts J, Rowland M (1983) Prevalence of myopia in the United States. Arch Ophthalmol 101:405–407
Tabandeh H, Flynn HW Jr, Scott IU et al (1999) Visual acuity outcomes of patients 50 years of age and older with high myopia and untreated choroidal neovascularization. Ophthalmology 106:2063–2067
Tokoro T (1988) On the definition of pathologic myopia in group studies. Acta Ophthalmol 66:107–108
Tokoro T (1998) Criteria for diagnosis of pathologic myopia. In: Tokoro T (ed) Atlas of posterior fundus changes in pathologic myopia. Springer, Tokyo, pp 1–2
Tokoro T (1998) Myopic choroidal neovascularization (Fuchs’ spot). In: Tokoro T (ed) Atlas of posterior fundus changes in pathologic myopia. Springer, New York, Berlin Heidelberg, pp 161–201
Yoshida A, Ishiko S, Kojima M (1996) Inward and outward permeability of the blood–retinal barrier in experimental myopia. Graefes Arch Clin Exp Ophthalmol 234:S239–S242
Yoshida T, Ohno-Matsui K, Ohtake Y et al (2002) Long-term visual prognosis of choroidal neovascularization in high myopia. A comparison between age groups. Ophthalmology 109:712–719
Yoshida T, Ohno-Matsui K, Yasuzumi K et al (2003) Myopic choroidal neovascularization: a 10-year follow-up. Ophthalmology 110:1297–1305
Acknowledgments
This work was supported in part by research grant 14571659 from the Japan Society for the Promotion of Science, Tokyo, Japan.
Author information
Authors and Affiliations
Corresponding author
Additional information
The authors have no financial interest in any products/drugs discussed in this article.
Rights and permissions
About this article
Cite this article
Hayashi, K., Ohno-Matsui, K., Yoshida, T. et al. Characteristics of patients with a favorable natural course of myopic choroidal neovascularization. Graefe's Arch Clin Exp Ophthalmol 243, 13–19 (2005). https://doi.org/10.1007/s00417-004-0960-5
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00417-004-0960-5