Abstract
Introduction
Isolated spinal cord angiitis (ISCA) is very rare disease. But, it is frequently encountered in the differential diagnosis of atypical spinal cord syndromes.
Case presentation and review of the literature
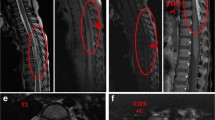
We present a 31-year-old male who presented with progressive paraparesis, and diagnosed with pathologically confirmed ISCA. Longitudinal cystic transverse myelitis was documented in spinal MRI. He responded well to cyclophosphamide and steroid combination, and no relapse was noted during the 4-year follow-up.
A standard systematic analysis of the germane literature disclosed 15 more ISCA cases. In total 16 cases (mean age: 46.5, 10 males), ISCA was diagnosed with pathological evaluation in all (Biopsy in 11, Autopsy in 5). MRI lesion is characterized by usually multisegmental longitudinal and sometimes cystic expansile lesions. In seven cases, it was described as “(pseudo)tumoral” by the authors. Albeit absence of elevation of CSF protein/WBC or “compatible” spinal MRI lesion may aid to exclude ISCA to some extent, pathological confirmation is currently necessary for the diagnosis. In 11 cases, ISCA was treated similar to primary supratentorial vasculitis. Mortality rate is 31%.
Discussion
ISCA diagnosis, a typical example of which we have presented here, can only be established by tissue examination. However, noninvasive diagnostic criteria are critically needed. Our data suggest that this can only be possible with multinational multicenter prospective registry.


Similar content being viewed by others
References
Baumer D, Flossmann E, Cudlip S, Quaghebeur G, Jeans A, Talbot K (2008) Primary angiitis of the CNS mimicking a spinal cord tumour. J Neurol 255:1970–1972
Bhibhatbhan A, Katz NR, Hudon M, Clark AW, Hurlbert RJ, Zochodne DW (2006) Primary angiitis of the spinal cord presenting as a conus mass: long-term remission. Surg Neurol 66:622–625
Caccamo DV, Garcia JH, Ho KL (1992) Isolated granulomatous angiitis of the spinal cord. Ann Neurol 32:580–582
Calabrese LH, Mallek JA (1988) Primary angiitis of the central nervous system. Report of 8 new cases, review of the literature, and proposal for diagnostic criteria. Medicine (Baltimore) 67:20–39
Chen SH, Sur S, Sedighim S, Kassi A, Yavagal D, Peterson EC, Starke RM (2019) Utility of diagnostic cerebral angiography in the management of suspected central nervous system vasculitis. J Clin Neurosci 64:98
Cupps TR, Moore PM, Fauci AS (1983) Isolated angiitis of the central nervous system. Prospective diagnostic and therapeutic experience. Am J Med 74:97–105
Feasby TE, Ferguson GG, Kaufmann JC (1975) Isolated spinal cord arteritis. Can J Neurol Sci Le Journal canadien des sciences neurologiques 2:143–146
Fisher A, Rahman H, Farrell M, Hennessy M (2017) Progressive fatal myelopathy secondary to isolated spinal cord vasculitis. Front Neurol 8:705
Goertz C, Wegner C, Brück W, Berlit P (2010) Primary angiitis of the CNS with pure spinal cord involvement: a case report. J Neurol 257:1762–1764
Judice DJ, LeBlanch HJ, McGarry PA (1978) Spinal cord vasculitis presenting as a spinal cord tumor in a heroin addict. Case report J Neurosurg 48:131–134
Lie JT (1991) Angiitis of the central nervous system. Curr Opin Rheumatol 3:36–45
Lie JT (1992) Primary (granulomatous) angiitis of the central nervous system: a clinicopathologic analysis of 15 new cases and a review of the literature. Hum Pathol 23:164–171
Mair WG, Folkerts JF (1953) Necrosis of the spinal cord due to thrombophlebitis (subacute necrotic myelitis). Brain J Neurol 76:563–575
Pagni F, Isimbaldi G, Vergani F, Casiraghi P, Marzorati L, Migliorino G, Cattoretti G (2012) Primary angiitis of the central nervous system: 2 atypical cases. Folia Neuropathol 3:293–299
Ropper AH, Ayata C, Adelman L (2003) Vasculitis of the spinal cord. Arch Neurol 60:1791–1794
Rourke T, Hamidian JA, Pretorius P, Morris J, Samandouras G, Cudlip S (2009) Intraoperative, imaging and pathological features in spinal cord vasculitis. J Clin Neurosci 16:1093–1095
Salvarani C, Brown RD Jr, Calamia KT, Christianson TJ, Huston J 3rd, Meschia JF, Giannini C, Miller DV, Hunder GG (2008) Primary CNS vasculitis with spinal cord involvement. Neurology 70:2394–2400
Salvarani C, Brown RD Jr, Calamia KT, Christianson TJ, Weigand SD, Miller DV, Giannini C, Meschia JF, Huston J 3rd, Hunder GG (2007) Primary central nervous system vasculitis: analysis of 101 patients. Ann Neurol 62:442–451
Strunk D, Schulte-Mecklenbeck A, Golombeck KS, Meyer ZuHorste G, Melzer N, Beuker C, Schmidt A, Wiendl H, Meuth SG, Gross CC, Minnerup J (2018) Immune cell profiling in the cerebrospinal fluid of patients with primary angiitis of the central nervous system reflects the heterogeneity of the disease. J Neuroimmunol 321:109–116
Wang CR, Peng SL, Huang HW (2018) Isolated cervical cord involvement in primary central nervous system vasculitis. J Rheumatol 45:962–963
Wang LJ, Kong DZ, Guo ZN, Zhang FL, Zhou HW, Yang Y (2019) Study on the clinical, imaging, and pathological characteristics of 18 cases with primary central nervous system vasculitis. J Stroke Cerebrovasc Dis 28:920–928
Acknowledgements
Not applicable.
Funding
None.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflicts of interest
On behalf of all authors, Mehmet Akif Topcuoglu, the corresponding author, states that there is no conflict of interest.
Ethical approval
This study does not contain any studies with human participants performed by the authors. Therefore, ethical committee aproval was waived. The patient signed informed consent for publication.
Informed consent
We have obtained the patient´s permission and written informed consent for publishing of his information/case.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Ayvacıoğlu Cagan, C., Temucin, C.M., Arslan, D. et al. Isolated spinal cord granulomatous angiitis: a case report and review of the literature. J Neurol 269, 3175–3179 (2022). https://doi.org/10.1007/s00415-021-10912-z
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00415-021-10912-z