Abstract
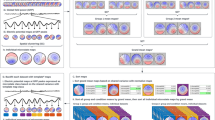
Patients suffering from disorders of consciousness still present a diagnostic challenge due to the fact that their assessment is mainly based on behavioral scales with their motor responses often being strongly impaired. We therefore focused on resting electroencephalography (EEG) in order to reveal potential alternative measures of the patient’s current state independent of rather complex abilities (e.g., language comprehension). Resting EEG was recorded in nine minimally conscious state (MCS) and eight vegetative state/unresponsive wakefulness syndrome (VS/UWS) patients. Behavioral assessments were conducted using the Coma-Recovery Scale—Revised (CRS-R). The signal was analyzed in the frequency domain and association between resting EEG and CRS-R score as well as clinical diagnosis were calculated using Pearson correlation and repeated-measures ANOVAs. The analyses revealed robust positive correlations between CRS-R score and ratios between frequencies above 8 Hz and frequencies below 8 Hz. Furthermore, the frequency of the spectral peak was also highly indicative of the patient’s CRS-R score. Concerning differences between clinical diagnosis and healthy controls, it could be revealed that while VS/UWS patients showed higher delta and theta activity than controls, MCS did not differ from controls in this frequency range. Alpha activity, on the other hand, was strongly decreased in both patient groups as compared to controls. The strong relationship between various resting EEG parameters and CRS-R score provides significant clinical relevance. Not only is resting activity easily acquired at bedside, but furthermore, it does not depend on explicit cooperation of the patient. Especially in cases where behavioral assessment is difficult or ambiguous, spectral analysis of resting EEG can therefore complement clinical diagnosis.



Similar content being viewed by others
References
Schnakers C, Perrin F, Schabus M, Majerus S, Ledoux D, Damas P, Boly M, Vanhaudenhuyse A, Bruno MA, Moonen G, Laureys S (2008) Voluntary brain processing in disorders of consciousness. Neurology 71(20):1614–1620. doi:10.1212/01.wnl.0000334754.15330.69
Perrin F, Schnakers C, Schabus M, Degueldre C, Goldman S, Bredart S, Faymonville ME, Lamy M, Moonen G, Luxen A, Maquet P, Laureys S (2006) Brain response to one’s own name in vegetative state, minimally conscious state, and locked-in syndrome. Arch Neurol 63(4):562–569
Fellinger R, Klimesch W, Schnakers C, Perrin F, Freunberger R, Gruber W, Laureys S, Schabus M (2011) Cognitive processes in disorders of consciousness as revealed by EEG time-frequency analyses. Clin Neurophysiol doi:10.1016/j.clinph.2011.03.004
Owen AM, Coleman MR, Boly M, Davis MH, Laureys S, Pickard JD (2006) Detecting awareness in the vegetative state. Science 313(5792):1402
Monti MM, Vanhaudenhuyse A, Coleman MR, Boly M, Pickard JD, Tshibanda L, Owen AM, Laureys S (2010) Willful modulation of brain activity in disorders of consciousness. N Engl J Med 362(7):579–589. doi:10.1056/NEJMoa0905370
Cruse D, Chennu S, Chatelle C, Bekinschtein TA, Fernández-Espejo D, Pickard JD, Laureys S, Owen AM (2011) Bedside detection of awareness in the vegetative state: a cohort study. Lancet
Goldfine AM, Bardin JC, Noirhomme Q, Fins JJ, Schiff ND, Victor JD (2013) Reanalysis of “bedside detection of awareness in the vegetative state: a cohort study”. Lancet 381:289–291
Goldfine AM, Victor JD, Conte MM, Bardin JC, Schiff ND (2011) Determination of awareness in patients with severe brain injury using EEG power spectral analysis. Clin Neurophysiol 122:2157–2168
Bekinschtein TA, Dehaene S, Rohaut B, Tadel F, Cohen L, Naccache L (2009) Neural signature of the conscious processing of auditory regularities. Proc Natl Acad Sci 106(5):1672
Boly M (2011) Measuring the fading consciousness in the human brain. Curr Opin Neurol 24(4):394–400. doi:10.1097/WCO.0b013e328347da94
Vanhaudenhuyse A, Noirhomme Q, Tshibanda LJF, Bruno MA, Boveroux P, Schnakers C, Soddu A, Perlbarg V, Ledoux D, Brichant JF (2010) Default network connectivity reflects the level of consciousness in non-communicative brain-damaged patients. Brain 133(1):161–171
Soddu A, Vanhaudenhuyse A, Bahri MA, Bruno MA, Boly M, Demertzi A, Tshibanda JF, Phillips C, Stanziano M, Ovadia-Caro S, Nir Y, Maquet P, Papa M, Malach R, Laureys S, Noirhomme Q (2011) Identifying the default-mode component in spatial IC analyses of patients with disorders of consciousness. Hum Brain Mapp. doi:10.1002/hbm.21249
Fernandez-Espejo D, Bekinschtein T, Monti MM, Pickard JD, Junque C, Coleman MR, Owen AM (2011) Diffusion-weighted imaging distinguishes the vegetative state from the minimally conscious state. Neuroimage 54:103–112
Bagnato S, Boccagni C, Prestandrea C, Sant’Angelo A, Castiglione A, Galardi G (2010) Prognostic value of standard EEG in traumatic and non-traumatic disorders of consciousness following coma. Clin Neurophysiol 121:274–280
Fingelkurts AA, Fingelkurts AA, Bagnato S, Boccagni C, Galardi G (2011) Life or death: prognostic value of a resting EEG with regards to survival in patients in vegetative and minimally conscious states. PLoS One 6:e25967
Rosanova M, Gosseries O, Casarotto S, Boly M, Casali AG, Bruno M-A, Mariotti M, Boveroux P, Tononi G, Laureys S (2012) Recovery of cortical effective connectivity and recovery of consciousness in vegetative patients. Brain 135:1308–1320
Giacino JT, Kalmar K, Whyte J (2004) The JFK coma recovery scale-revised: measurement characteristics and diagnostic utility. Arch Phys Med Rehabil 85(12):2020–2029
Kulkarni VP, Lin K, Benbadis SR (2007) EEG findings in the persistent vegetative state. J Clin Neurophysiol 24(6):433–437
Kotchoubey B, Lang S, Bostanov V, Birbaumer N (2002) Is there a mind? Electrophysiology of unconscious patients. Physiology 17(1):38–42
Kobylarz EJ, Schiff ND (2005) Neurophysiological correlates of persistent vegetative and minimally conscious states. Neuropsychol Rehabil 15(3–4):323–332
Laureys S, Berré J, Goldman S (2001) Cerebral function in coma, vegetative state, minimally conscious state, locked-in syndrome, and brain death. Yearbook of Intensive Care and Emergency Medicine, pp 386–396
Klimesch W (1999) EEG alpha and theta oscillations reflect cognitive and memory performance: a review and analysis. Brain Res Brain Res Rev 29(2–3):169–195
Klimesch W (1997) EEG-alpha rhythms and memory processes. Int J Psychophysiol 26(1–3):319–340
Steriade M, Jones EG, Llinas RR (1990) Thalamic oscillations and signalling. Wiley, New York
Herrmann CS, Arnold T, Visbeck A, Hundemer HP, Hopf H (2001) Adaptive frequency decomposition of EEG with subsequent expert system analysis. Comput Biol Med 31(6):407–427
Chen ACN, Feng W, Zhao H, Yin Y, Wang P (2008) EEG default mode network in the human brain: spectral regional field powers. Neuroimage 41(2):561–574
Ishii R, Shinosaki K, Ukai S, Inouye T, Ishihara T, Yoshimine T, Hirabuki N, Asada H, Kihara T, Robinson SE (1999) Medial prefrontal cortex generates frontal midline theta rhythm. Neuroreport 10(4):675–679
Asada H, Fukuda Y, Tsunoda S, Yamaguchi M, Tonoike M (1999) Frontal midline theta rhythms reflect alternative activation of prefrontal cortex and anterior cingulate cortex in humans. Neurosci Lett 274(1):29–32
Iber C, Ancoli-Israel S, Chesson A, Quan SF (2007) The AASM manual for the scoring of sleep and associated events: rules terminology and technical specifications, 1st edn. American Academy of Sleep Medicine, Westchester
Jensen O, Mazaheri A (2010) Shaping functional architecture by oscillatory alpha activity: gating by inhibition. Frontiers Human Neurosci 4
Klimesch W, Sauseng P, Hanslmayr S (2007) EEG alpha oscillations: the inhibition-timing hypothesis. Brain Res Rev 53(1):63–88
Sarà M, Pistoia F (2010) Complexity loss in physiological time series of patients in a vegetative state. Nonlinear Dynam Psychol Life Sci 14(1):1
Gosseries O, Schnakers C, Ledoux D, Vanhaudenhuyse A, Bruno M-A, Demertzi A, Noirhomme Q, Lehembre R, Damas P, Goldman S (2011) Automated EEG entropy measurements in coma, vegetative state/unresponsive wakefulness syndrome and minimally conscious state. Funct Neurol
Zhang X-S, Roy RJ, Jensen EW (2001) EEG complexity as a measure of depth of anesthesia for patients. IEEE Trans Biomed Eng 48(12):1424–1433
Bruhn J, Röpcke H, Hoeft A (2000) Approximate entropy as an electroencephalographic measure of anesthetic drug effect during desflurane anesthesia. Anesthesiology 92(3):715–726
Ferenets R, Lipping T, Anier A, Jantti V, Melto S, Hovilehto S (2006) Comparison of entropy and complexity measures for the assessment of depth of sedation. IEEE Trans Biomed Eng 53(6):1067–1077
Acknowledgments
We thank Nicole Chwala-Schlegel, Theresa Stemeseder, Katharina Weilhart, and Christoph Pelikan for conducting a considerable amount of EEG recordings and clinical assessments. We would also like to thank the staff of the Apallic Care Units at the “Geriatriezentrum am Wienerwald” in Vienna and at the “Albert-Schweitzer-Klink” in Graz, Austria, for their extensive support.
Conflicts of interest
The authors declare that they have no conflicts of interest.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Lechinger, J., Bothe, K., Pichler, G. et al. CRS-R score in disorders of consciousness is strongly related to spectral EEG at rest. J Neurol 260, 2348–2356 (2013). https://doi.org/10.1007/s00415-013-6982-3
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00415-013-6982-3