Abstract
Purpose
To show the different effects of expansion sphincter pharyngoplasty (ESP) and barbed reposition pharyngoplasty (BRP) on muscle tension and muscle fiber tearing using a comparative experimental stress test with a frog thigh muscle model.
Methods
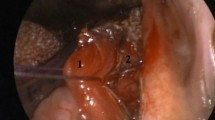
Frog thigh muscle was used for this experimental study. A Barbed suture was used to simulate the BRP pharyngoplasty whereas a Vicryl 3-0 suture was used to simulate the ESP technique. The other extremity of the suture was attached to traction scales. The traction scales were used to measure the weight relative to the amount of force required to obtain muscle breaking. Both surgical techniques were simulated on the frog muscle. Traction was performed until muscle breaking was observed, measuring the value of force needed to obtain muscle rupture.
Results
Specimen muscle breakdown in the ESP simulation occurred with an average value of 0.7 kg of traction force. Contrarily, specimen muscle breakdown in the BRP simulation with Barbed suture occurred with an average value of 1.5 kg of traction force
Conclusion
During simulation of the ESP technique, specimen muscle breakdown occurred with an average value of traction force lower than in the BRP technique. During traction the multiple lateral sustaining suture loops of BRP could ensure greater stability then the single pulling tip suture of ESP with minor risk of muscle fiber damage.






Similar content being viewed by others
References
Park D, Kim JS, Heo SJ (2019) Obstruction patterns during drug-induced sleep endoscopy vs natural sleep endoscopy in patients with obstructive sleep apnea. JAMA Otolaryngol Head Neck Surg. https://doi.org/10.1001/jamaoto.2019.1437
Green KK, Kent DT, D'Agostino MA et al (2019) Drug-induced sleep endoscopy and surgical outcomes: a multicenter cohort study. Laryngoscope 129:761–770
Stuck BA, Ravesloot MJL, Eschenhagen T, de Vet HCW, Sommer JU (2018) Uvulopalatopharyngoplasty with or without tonsillectomy in the treatment of adult obstructive sleep apnea—a systematic review. Sleep Med 50:152–165
Yaremchuk K (2016) Palatal procedures for obstructive sleep apnea. Otolaryngol Clin North Am 49:1383–1397
Fujita S, Conway WA, Zorick FJ et al (1985) Evaluation of the effectiveness of uvulopalatopharyngoplasty. Laryngoscope 95:70–74
Tschopp S, Tschopp K (2019) Tonsil size and outcome of uvulopalatopharyngoplasty with tonsillectomy in obstructive sleep apnea. Laryngoscope 2019:8
Rosvall BR, Chin CJ (2017) Is uvulopalatopharyngoplasty effective in obstructive sleep apnea? Laryngoscope 127:2201–2202
Friberg D, Sundman J, Browaldh N (2019) Long-term evaluation of satisfaction and side effects after modified uvulopalatopharyngoplasty. Laryngoscope 2019:12
Pang KP, Woodson BT (2007) Expansion sphincter pharyngoplasty: a new technique for the treatment of obstructive sleep apnea. Otolaryngol Head Neck Surg 137:110–114
Vicini C, Hendawy E, Campanini A et al (2015) Barbed reposition pharyngoplasty (BRP) for OSAHS: a feasibility, safety, efficacy and teachability pilot study. We are on the giant's shoulders. Eur Arch Otorhinolaryngol 272:3065–3070
Li HY, Lee LA (2009) Relocation pharyngoplasty for obstructive sleep apnea. Laryngoscope 119:2472–2477
Salamanca F, Costantini F, Mantovani M et al (2014) Barbed anterior pharyngoplasty: an evolution of anterior palatoplasty. Acta Otorhinolaryngol Ital 34:434–438
Vicini C, Meccariello G, Cammaroto G, Rashwan M, Montevecchi F (2017) Barbed reposition pharyngoplasty in multilevel robotic surgery for obstructive sleep apnoea. Acta Otorhinolaryngol Ital 37:214–217
Montevecchi F, Meccariello G, Firinu E et al (2018) Prospective multicentre study on barbed reposition pharyngoplasty standing alone or as a part of multilevel surgery for sleep apnoea. Clin Otolaryngol 43:483–488
Rashwan MS, Montevecchi F, Cammaroto G et al (2018) Evolution of soft palate surgery techniques for obstructive sleep apnea patients: a comparative study for single-level palatal surgeries. Clin Otolaryngol 43:584–590
Chi JC, Chiang RP, Chou TY et al (2015) The role of lateral pharyngoplasty in obstructive sleep apnea syndrome. Eur Arch Otorhinolaryngol 272:489–496
Cahali MB (2003) Lateral pharyngoplasty: a new treatment for obstructive sleep apnea hypopnea syndrome. Laryngoscope 113:1961–1968
Vicini C, De Vito A, Iannella G et al (2018) The aging effect on upper airways collapse of patients with obstructive sleep apnea syndrome. Eur Arch Otorhinolaryngol 275:2983–2990
Pang KP, Pang EB, Win MT, Pang KA, Woodson BT (2016) Expansion sphincter pharyngoplasty for the treatment of OSA: a systemic review and meta-analysis. Eur Arch Otorhinolaryngol 273:2329–2333
Sorrenti G, Piccin O (2013) Functional expansion pharyngoplasty in the treatment of obstructive sleep apnea. Laryngoscope 123:2905–2908
Ulualp SO (2014) Modified expansion sphincter pharyngoplasty for treatment of children with obstructive sleep apnea. JAMA Otolaryngol Head Neck Surg 140:817–822
Babademez MA, Gul F, Teleke YC (2019) Barbed palatoplasty vs. expansion sphincter pharyngoplasty with anterior palatoplasty. Laryngoscope [Epub ahead of print]
Funding
None.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Ethical approval
All procedures performed in studies are in accordance with the animal ethical approval.
Ethical standards
All procedures performed in studies are in accordance with the ethical standards of the Morgagni Pierantoni Hospital institutional committee.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
This article is part of the Topical Collection on sleep apnea syndrome Guest Editors: Manuele Casale, Rinaldi Vittorio.
Rights and permissions
About this article
Cite this article
Iannella, G., Magliulo, G., Di Luca, M. et al. Lateral pharyngoplasty techniques for obstructive sleep apnea syndrome: a comparative experimental stress test of two different techniques. Eur Arch Otorhinolaryngol 277, 1793–1800 (2020). https://doi.org/10.1007/s00405-020-05883-2
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00405-020-05883-2