Abstract
Objective
The objective of our study is to estimate the prevalence of endometrial cavity fluid (ECF) in Assisted Reproductive Techniques (ART) cycles and analyze its effects on pregnancy outcome in such cycles.
Data sources
PubMed, Cochrane Central, Scopus, and clinicaltrials.gov were searched for articles. The reference lists of relevant publications were explored for other studies.
Study eligibility criteria
Studies that had assessed the pregnancy outcome in ART cycles and had commented on ECF accumulation were included. Pregnancy outcomes were assessed in all ART cycles where ECF was observed and were compared to the non-ECF cycles.
Results
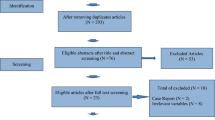
A total of nine studies were included in the meta-analysis for a total of 28,210 cycles. Pooled analysis of the prevalence of ECF cycles out of total cycles in females undergoing ART using a fixed effect model showed that it was 14% (95% CI is 13% to 14%; I2 = 99%, p = < 0.01). The random effect model prevalence of ECF cycles was around 7% (95% CI: 4% to 10%). There was a statistically significant (25%) decrease in pregnancy rates per cycle transfer in the ECF cycle versus the non-ECF cycle group during ART [OR = 0.75, 95% CI = 0.67–0.84), p < 0.001; moderate quality evidence]. When ECF size was compared, there was a statistically significant increase in pregnancy rates if ECF size was less than 3.5 mm versus greater than or equal to 3.5 mm [OR = 13.67, 95% CI = 1.43–130.40), p = 0.02; high quality evidence].
Sub-group analysis revealed that the ECF present at the time of embryo transfer significantly decreased the pregnancy rates by 26% as compared to the group where the ECF was not present at the time of embryo transfer [OR = 0.74, 95% CI = 0.65–0.85), p < 0.001].
Conclusions
This meta-analysis proposes that the presence of ECF significantly decreases the implantation and pregnancy rates of ART cycles, and even more so if its size is greater than 3.5 mm. Interventions to decrease ECF formation or treat it have enhanced the pregnancy outcome in ART cycles.
Prospero registration
Date: 17th September 2020; Number: CRD42020182262.





Similar content being viewed by others
Availability of supporting data
The datasets used and/or analyzed during the current study are available from the corresponding author on request.
Code availability
Not applicable.
Abbreviations
- ECF:
-
Endometrial cavity fluid
- ART:
-
Assisted reproductive technology
References
Cavagna M, Petersen CG, Mauri AL, Oliveira JBA, Baruffi RRL, Franco JG Jr (2014) Administration of progesterone on the day of oocyte retrieval to reverse accumulation of fluid in the endometrial cavity during assisted reproductive techniques. JBRA Assist Reprod 18(4):136–138
Na ED, Cha DH, Cho JH, Kim MK (2012) Comparison of IVF-ET outcomes in patients with hydrosalpinx pretreated with either sclerotherapy or laparoscopic salpingectomy. Clin Exp Reprod Med 39(4):182–186
He RH, Gao HJ, Li YQ, Zhu XM (2010) The associated factors to endometrial cavity fluid and the relevant impact on the IVF-ET outcome. Reprod Biol Endocrinol 8:46
Chien LW, Au HK, Xiao J, Tzeng CR (2002) Fluid accumulation within the uterine cavity reduces pregnancy rates in women undergoing IVF. Hum Reprod 17(2):351–356
Al-Hussaini TK, Shaaban OM (2018) Aspiration of endometrial cavity fluid at the time of egg collection. Middle East Fertility Soc J 23(4):354–356
Moher D, Liberati A, Tetzlaff J, Altman DG, Group P (2009) Preferred reporting items for systematic reviews and meta-analyses: the PRISMA statement. BMJ 339:b2535
Sterne JA, Hernan MA, Reeves BC, Savovic J, Berkman ND, Viswanathan M et al (2016) ROBINS-I: a tool for assessing risk of bias in non-randomised studies of interventions. BMJ 355:i4919
McGuinness LA, Higgins JPT. (2020) Risk-of-bias VISualization (robvis): An r package and Shiny web app for visualizing risk-of-bias assessments. Res Synth Methods
R Core Team (2013). R: a language and environment for statistical computing. R Foundation for Statistical Computing, Vienna, Austria. URL http://www.R-project.org/.
Higgins J, Green S, (Editors). Cochrane handbook for systematic reviews of interventions: The cochrane collaboration, 2011; 2011 [cited 2020 28 May]. Available from: www.handbook.cochrane.org.
Kjaergard LL, Villumsen J, Gluud C (2001) Reported methodologic quality and discrepancies between large and small randomized trials in meta-analyses. Ann Intern Med 135(11):982–989
Copenhagen: The nordic cochrane centre. The cochrane collaboration. Review manager (RevMan) [Computer program]. Version 5.3.
Schünemann H, Brożek J, Guyatt G, Oxman A, (Editors). GRADE handbook for grading quality of evidence and strength of recommendations. Updated October 2013. The GRADE Working Group, 2013. 2013. Available from: guidelinedevelopment.org/handbook.
GRADEpro GDT: GRADEpro guideline development tool [Software]. McMaster University, 2015 (developed by Evidence Prime, Inc.). [Internet]. Available from: gradepro.org.
Akman MA, Erden HF, Bahceci M (2005) Endometrial fluid visualized through ultrasonography during ovarian stimulation in IVF cycles impairs the outcome in tubal factor, but not PCOS, patients. Hum Reprod 20(4):906–909
Chen QL, Hong YE, Zeng PH, Liu DY, Pei L, Huang GN (2009) Clinical analysis on 106 cases of endometrial cavity fluid visualized through ultrasound during IVF-ET [In Chinese]. J Pract Obstet Gynecol 25(3):178–180
Lee RK, Yu SL, Chih YF, Tsai YC, Lin MH, Hwu YM et al (2006) Effect of endometrial cavity fluid on clinical pregnancy rate in tubal embryo transfer (TET). J Assist Reprod Genet 23(5):229–234
Levi AJ, Segars JH, Miller BT, Leondires MP (2001) Endometrial cavity fluid is associated with poor ovarian response and increased cancellation rates in ART cycles. Hum Reprod 16(12):2610–2615
Liu DE, Li YP, Lv QF, Ma YL, Zhou QE, Deng L (2004) Endometrial cavity fluid in ART cycles: analysis of 25 cases [in Chinese]. Chin J Pract Gynecol Obstet 20(4):213–214
Zhang WX, Cao LB, Zhao Y, Li J, Li BF, Lv JN et al (2021) Endometrial cavity fluid is associated with deleterious pregnancy outcomes in patients undergoing in vitro fertilization/intracytoplasmic sperm injection: a retrospective cohort study. Ann Transl Med 9(1):9
Mansour RT, Aboulghar MA, Serour GI, Riad R (1991) Fluid accumulation of the uterine cavity before embryo transfer: a possible hindrance for implantation. J In Vitro Fert Embryo Transf 8(3):157–159
Griffiths AN, Watermeyer SR, Klentzeris LD (2002) Fluid within the endometrial cavity in an IVF cycle–a novel approach to its management. J Assist Reprod Genet 19(6):298–301
Liu S, Shi L, Shi J (2016) Impact of endometrial cavity fluid on assisted reproductive technology outcomes. Int J Gynaecol Obstet 132(3):278–283
Lu S, Peng H, Zhang H, Zhang L, Cao Q, Li R et al (2013) Excessive intrauterine fluid cause aberrant implantation and pregnancy outcome in mice. PLoS ONE 8(10):e78446
Camus E, Poncelet C, Goffinet F, Wainer B, Merlet F, Nisand I et al (1999) Pregnancy rates after in-vitro fertilization in cases of tubal infertility with and without hydrosalpinx: a meta-analysis of published comparative studies. Hum Reprod 14(5):1243–1249
Acknowledgements
We acknowledge the GRADE Pro team [McMaster University and Evidence Prime Inc., available from: https://gradepro.org/] for letting us use the software for the synthesis, overall assessment, and grading of systematic review.
Funding
None.
Author information
Authors and Affiliations
Contributions
All authors contributed to the study’s conception and design. Material preparation, data collection, and analysis were performed by SS, PK, The first draft of the manuscript was written by SS and PK and all authors commented on previous versions of the manuscript. All authors read and approved the final manuscript. Study design and planning of systematic review—All of the authors. PK: Literature search, Roles/Writing, Data collection and analysis, review & editing. SS: Literature search, Figures, ROB, GRADE, Data collection and analysis, review & editing. NKG: Literature search, Data collection and analysis, review & editing. GY: Project administration, Tables. PS: Final approval of Manuscript, Project administration. VS: Tables, Data collection and analysis. NG: Resources, Approval of final manuscript. Corrections and Final approval of Manuscript—All of the authors.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Ethical approval
Not applicable.
Consent to participate
Not applicable.
Consent for publication
Not applicable.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Kathuria, P., Ghuman, N.K., Yadav, G. et al. Systematic review analyzing significance of endometrial cavity fluid during assisted reproductive techniques. Arch Gynecol Obstet 309, 413–425 (2024). https://doi.org/10.1007/s00404-023-07072-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00404-023-07072-y