Abstract
Purpose
Bacterial vaginosis is a recalcitrant polymicrobial biofilm infection that often resists standard antibiotic treatment. We therefore considered repeated treatment with octenidine, a local antiseptic that has previously been shown to be highly effective in several biofilm-associated infections.
Methods
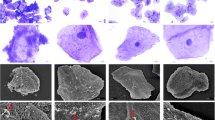
Twenty-four patients with recurrent BV were treated with a 7-day course of octenidine (octenidine dihydrochloride spray application with the commercial product Octenisept®). In case of treatment failure or relapse within 6 months, patients were re-treated with a 28-day course of octenidine. In case of recurrence within 6 months after the second treatment course, patients were treated again with a 28-day course followed by weekly applications for 2 months. Treatment effect was evaluated by assessment of the presence of the biofilm on voided vaginal epithelial cells through fluorescence in situ hybridisation.
Results
The initial cure rate following a 7-day course of octenidine was as high as 87.5 %. The 6-month relapse rate was, however, as high as 66.6 %. Repeated treatment for 28 days led to an overall cure rate of 75.0 %; however, it was also associated with emergence of complete resistance to octenidine in a subset of women. The overall cure rate after three treatment courses with 1-year follow-up was 62.5 %, with 37.5 % of the patients showing complete resistance to octenidine.
Conclusion
Our preliminary results showed that octenidine dihydrochloride was initially highly effective, but the efficacy of repeated and prolonged treatment dropped quickly as challenge with the antiseptic rapidly led to bacterial resistance in a considerable subset of women.



Similar content being viewed by others
References
Verstraelen H, Verhelst R (2009) Bacterial vaginosis: an update on diagnosis and treatment. Expert Rev Anti Infect Ther 7:1109–1124
Oakeshott P, Hay P, Hay S, Steinke F, Rink E, Kerry S (2002) Association between bacterial vaginosis or chlamydial infection and miscarriage before 16 weeks’ gestation: prospective community based cohort study. BMJ 325:1334
Leitich H, Kiss H (2007) Asymptomatic bacterial vaginosis and intermediate flora as risk factors for adverse pregnancy outcome. Best Pract Res Clin Obstet Gynaecol 21:375–390
Kirakoya-Samadoulougou F, Nagot N, Defer MC, Yaro S, Fao P, Ilboudo F, Langani Y, Meda N, Robert A (2011) Epidemiology of herpes simplex virus type 2 infection in rural and urban Burkina Faso. Sex Transm Dis 38:117–123
Gillet E, Meys JF, Verstraelen H, Bosire C, De Sutter P, Temmerman M, Broeck DV (2011) Bacterial vaginosis is associated with uterine cervical human papillomavirus infection: a meta-analysis. BMC Infect Dis 11:10
Atashili J, Poole C, Ndumbe PM, Adimora AA, Smith JS (2008) Bacterial vaginosis and HIV acquisition: a meta-analysis of published studies. AIDS 22:1493–1501
Swidsinski A, Mendling W, Loening-Baucke V, Ladhoff A, Swidsinski S, Hale LP, Lochs H (2005) Adherent biofilms in bacterial vaginosis. Obstet Gynecol 106:1013–1023
Swidsinski A, Mendling W, Loening-Baucke V, Swidsinski S, Dörffel Y, Scholze J, Lochs H, Verstraelen H (2008) An adherent Gardnerella vaginalis biofilm persists on the vaginal epithelium after standard therapy with oral metronidazole. Am J Obstet Gynecol 198:97.e1-6.1
Swidsinski A, Dörffel Y, Loening-Baucke V, Schilling J, Mendling W (2011) Response of Gardnerella vaginalis biofilm to 5 days of moxifloxacin treatment. FEMS Immunol Med Microbiol 61:41–46
Cos P, Toté K, Horemans T, Maes L (2010) Biofilms: an extra hurdle for effective antimicrobial therapy. Curr Pharm Des 16:2279–2295
Høiby N, Bjarnsholt T, Givskov M, Molin S, Ciofu O (2010) Antibiotic resistance of bacterial biofilms. Int J Antimicrob Agents 35:322–332
Rupf S, Balkenhol M, Sahrhage TO, Baum A, Chromik JN, Ruppert K, Wissenbach DK, Maurer HH, Hannig M (2012) Biofilm inhibition by an experimental dental resin composite containing octenidine dihydrochloride. Dent Mater 28:974–984
Bartoszewicz M, Rygiel A, Krzemiński M, Przondo-Mordarska A (2007) Penetration of a selected antibiotic and antiseptic into a biofilm formed on orthopedic steel implants. Ortop Traumatol Rehabil 9:310–318
Sennhenn-Kirchner S, Wolff N, Klaue S, Mergeryan H, Borg-von Zepelin M (2009) Decontamination efficacy of antiseptic agents on in vivo grown biofilms on rough titanium surfaces. Quintessence Int 40:e80–e88
Hübner NO, Siebert J, Kramer A (2010) Octenidine dihydrochloride, a modern antiseptic for skin, mucous membranes and wounds. Skin Pharmacol Physiol 23:244–258
Swidsinski A, Doerffel Y, Loening-Baucke V, Swidsinski S, Verstraelen H, Vaneechoutte M, Lemm V, Schilling J, Mendling W (2010) Gardnerella biofilm involves females and males and is transmitted sexually. Gynecol Obstet Invest 70:256–263
Novakov Mikic A, Budakov D (2010) Comparison of local metronidazole and a local antiseptic in the treatment of bacterial vaginosis. Arch Gynecol Obstet 282:43–47
Verstraelen H, Verhelst R, Roelens K, Temmerman M (2012) Antiseptics and disinfectants for the treatment of bacterial vaginosis: a systematic review. BMC Infect Dis 12:148
Cantón R, Morosini MI (2011) Emergence and spread of antibiotic resistance following exposure to antibiotics. FEMS Microbiol Rev 35:977–991
Conflict of interest
None.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Swidsinski, A., Loening-Baucke, V., Swidsinski, S. et al. Polymicrobial Gardnerella biofilm resists repeated intravaginal antiseptic treatment in a subset of women with bacterial vaginosis: a preliminary report. Arch Gynecol Obstet 291, 605–609 (2015). https://doi.org/10.1007/s00404-014-3484-1
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00404-014-3484-1