Abstract
Introduction
The biomechanical stability of a newly developed humerus nail (Sirus™) for the treatment of fractures of the proximal humerus was analyzed in comparison to established systems. In total, three randomized groups were formed (n = 4 pairs) from 12 matched pairs of human cadaver humeri.
Materials and methods
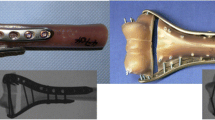
All intact bones were mechanically characterized by five subsequent load cycles under bending and torsional loading. The bending moment at the osteotomy was 7.5 N m the torsional moment was 8.3 N m over the hole specimen length. Loading was consistently initiated at the distal epiphysis and the deformation at the distal epiphysis was continuously recorded. Prior to implant reinforcement, a defect of 5 mm was created to simulate an unstable subcapital humerus fracture. For paired comparison, one humerus of each pair was stabilized with the Sirus proximal humerus nail while the counterpart was stabilized by a reference implant. In detail, the following groups were created: Sirus versus Proximal humerus nail (PHN) with spiral blade (group I); Sirus versus PHILOS plate (group II); Sirus versus 4.5 mm AO T-plate (group III).
Results
The Sirus nail demonstrated significantly higher stiffness values compared to the reference implants for both bending and torsional loading. The following distal epiphyseal displacements were recorded for a bending moment of 7.5 N m at the osteotomy: Sirus I: 8.8 mm, II: 8.4 mm, III: 7.7 mm (range 6.9–10.9), PHN 21.1 mm (range 15.7–25.2) (P = 0.005), PHILOS plate 27.5 mm (range 21.6–35.8) (P < 0.001), 4.5 AO T-plate 26.3 mm (range 24.3–33.9) (P = 0.01). The rotations corresponding to 8.3 N m torsional moment were: Sirus I: 9.1°, II: 9.3°, III: 10.6° (range 7.5–12.2), PHN 13.5° (range 10.3–15.6) (P = 0.158), PHILOS plate 15.6° (range 13.7–20.8) (P = 0.007), 4.5 AO T-Platte 14.1° (range 11.5–19.7) (P = 0.158).
Conclusion
The intramedullary load carriers were biomechanically superior when compared to the plating systems in the fracture model presented here. Supplementary, the Sirus Nail showed higher stiffness values than the PHN. However, the latter are gaining in importance due to the possibility of minimal invasive implantation. Whether this will be associated with functional advantages requires further clinical investigation.






Similar content being viewed by others
References
Blum J, Machemer H, Baumgart F, Schlegel U, Wahl D, Rommens PM (1999) Biomechanical comparison of bending and torsional properties in retrograde intramedullary nailing of humeral shaft fractures. J Orthop Trauma 13(5):344–50
Fierlbeck J, Füchtmeier B, Hammer J, Nerlich M (2003) Finite element modelling of proximal humeral fractures reinforced by intramedullary titanium nailing. In: Lütjering G, Albrecht J (eds) Ti—science and technology, Wiley-VCH, New York, pp 3253–60
Füchtmeier B, Hammer, Nerlich M (2002) Biomechanical behaviour of implant reinforced proximal humeral fractures. Z Metallkd 93(8):819–24
Gerber C, Schneeberger AG, Vinh TS (1990) The arterial vascularization of the humeral head. an anatomical study. J Bone Joint Surg Am 72(10):1486–94
Hepp P, Lill H, Bail H, Korner J, Niederhagen M, Haas NP, Josten C, Duda GN (2003) Where should implants be anchored in the humeral head? Clin Orthop 415:139–47
Hente R, Kampshoff J, Kinner B, Fuchtmeier B, Nerlich M (2004) Treatment of displaced 3- and 4-part fractures of the proximal humerus with fixator plate comprising angular stability. Unfallchirurg 107(9):769–82
Hessmann MH, Rommens PM (2001) Osteosynthesis techniques in proximal humeral fractures. Chirurg 72(11):1235–45
Hessmann MH, Sternstein W, Krummenauer F, Hofmann A, Rommens PM (2005) Internal fixation of proximal humerus fractures. Chirurg 76(2):167–74
Itoi E, Hsu HC, An KN (1996) Biomechanical investigation of the glenohumeral joint. J Shoulder Elbow Surg 5(5):407–24
Koval KJ, Blair B, Takei R, Kummer FJ, Zuckerman JD (1996) Surgical neck fractures of the proximal humerus: a laboratory evaluation of ten fixation techniques. J Trauma 40(5):778–83
Lill H, Hepp P, Korner J, Kassi JP, Verheyden AP, Josten C, Duda GN (2003) Proximal humeral fractures: how stiff should an implant be? A comparative mechanical study with new implants in human specimens. Arch Orthop Trauma Surg 123(2–3):74–81
Lill H, Hepp P, Rose T, Konig K, Josten C (2004) The angle stable locking-proximal-humerus-plate (LPHP) for proximal humeral fractures using a small anterior-lateral-deltoid-splitting-approach technique and first results. Zentralbl Chir 129(1):43–8
Marti A, Fankhauser C, Frenk A, Cordey J, Gasser B (2001) Biomechanical evaluation of the less invasive stabilization system for the internal fixation of distal femur fractures. J Orthop Trauma 15(7):482–7
Müller ME, Nazarian S, Koch P (1987) AO classification of fractures. Springer, Heidelberg, Tokyo
Dempster WT (1955) Space requirements of the seated operator (WADC-TR-55–159) Wright-Patterson Air Force Base, Ohio http://www.sport.uni-frankfurt.de/Personen/Preiss/Anthropometrie
Ruch DS, Glisson RR, Marr AW, Russell GB, Nunley JA (2000) Fixation of three-part proximal humeral fractures: a biomechanical evaluation. J Orthop Trauma 14(1):36–40
Ruchholtz S, Nast-Kolb D (2003) Die oberarmkopffraktur. Unfallchirurg 106(6):498–513
Rommens PM, Blum J, Runkel M (1998) Retrograde nailing of humeral shaft fractures. Clin Orthop 350:26–39
Stedtfeld HW, Attmanspacher W, Thaler K, Frosch B (2003) Fixation of humeral head fractures with antegrade intramedullary nailing. Zentralbl Chir 128(1):6–11
Wheeler DL, Colville MR (1997) Biomechanical comparison of intramedullary and percutaneous pin fixation for proximal humeral fracture fixation. J Orthop Trauma 11(5):363–7
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Füchtmeier, B., May, R., Hente, R. et al. Proximal humerus fractures: a comparative biomechanical analysis of intra and extramedullary implants. Arch Orthop Trauma Surg 127, 441–447 (2007). https://doi.org/10.1007/s00402-007-0319-6
Received:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00402-007-0319-6