Abstract
Purpose
This study aimed to investigate the association between macronutrient intake and biological age.
Methods
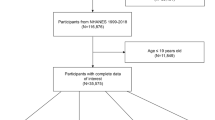
Data were collected from 26,381 adults who participated in the United States National Health and Nutrition Examination Survey (NHANES). Two biological ages were estimated using the Klemera-Doubal method (KDM) and PhenoAge algorithms. Biological age acceleration (AA) was computed as the difference between biological age and chronological age. The associations between macronutrient intakes and AA were investigated.
Results
After fully adjusting for confounding factors, negative associations were observed between AA and fiber intake (KDM-AA: β – 0.53, 95% CI – 0.62, – 0.43, P < 0.05; PhenoAge acceleration: β – 0.30, 95% CI – 0.35, – 0.25, P < 0.05). High-quality carbohydrate intake was associated with decreased AA (KDM-AA: β – 0.57, 95% CI – 0.67, – 0.47, P < 0.05; PhenoAge acceleration: β – 0.32, 95% CI – 0.37, – 0.26, P < 0.05), while low-quality carbohydrate was associated with increased AA (KDM-AA: β 0.30, 95% CI 0.21, 0.38, P < 0.05; PhenoAge acceleration: β 0.16, 95% CI 0.11, 0.21, P < 0.05). Plant protein was associated with decreased AA (KDM-AA: β – 0.39, 95% CI – 0.51, – 0.27, P < 0.05; PhenoAge acceleration: β – 0.21, 95% CI – 0.26, – 0.15, P < 0.05). Long-chain SFA intake increased AA (KDM-AA: β 0.16, 95% CI 0.08, 0.24, P < 0.05; PhenoAge acceleration: β 0.11, 95% CI 0.07, 0.15, P < 0.05). ω-3 PUFA was associated with decreased KDM-AA (β – 0.18, 95% CI – 0.27, – 0.08, P < 0.05) and PhenoAge acceleration (β – 0.09, 95% CI – 0.13, – 0.04, P < 0.05).
Conclusion
Our findings suggest that dietary fiber, high-quality carbohydrate, plant protein, and ω-3 PUFA intake may have a protective effect against AA, while low-quality carbohydrate and long-chain SFA intake may increase AA. Therefore, dietary interventions aimed at modifying macronutrient intakes may be useful in preventing or delaying age-related disease and improving overall health.

Similar content being viewed by others
Data availability
Detailed survey operation manuals, consent documents, and brochures from each period are available on the National Health and Nutrition Examination Survey website (https://www.cdc.gov/nchs/nhanes/about_nhanes).
References
Fontana L, Partridge L, Longo VD (2010) Extending healthy life span–from yeast to humans. Science 328(5976):321–326. https://doi.org/10.1126/science.1172539
Partridge L, Gems D (2002) Mechanisms of ageing: public or private? Nat Rev Genet 3(3):165–175. https://doi.org/10.1038/nrg753
Kirkwood TB, Austad SN (2000) Why do we age? Nature 408(6809):233–238. https://doi.org/10.1038/35041682
Finkel D, Whitfield K, McGue M (1995) Genetic and environmental influences on functional age: a twin study. J Gerontol B Psychol Sci Soc Sci 50(2):P104-113. https://doi.org/10.1093/geronb/50b.2.p104
Levine ME (2013) Modeling the rate of senescence: can estimated biological age predict mortality more accurately than chronological age? J Gerontol A Biol Sci Med Sci 68(6):667–674. https://doi.org/10.1093/gerona/gls233
Earls JC, Rappaport N, Heath L, Wilmanski T, Magis AT, Schork NJ, Omenn GS, Lovejoy J, Hood L, Price ND (2019) Multi-omic biological age estimation and its correlation with wellness and disease phenotypes: a longitudinal study of 3558 individuals. J Gerontol Ser A Biol Sci Med Sci 74(Suppl1):S52-s60. https://doi.org/10.1093/gerona/glz220
Klemera P, Doubal S (2006) A new approach to the concept and computation of biological age. Mech Ageing Dev 127(3):240–248. https://doi.org/10.1016/j.mad.2005.10.004
Levine ME, Lu AT, Quach A, Chen BH, Assimes TL, Bandinelli S, Hou L, Baccarelli AA, Stewart JD, Li Y, Whitsel EA, Wilson JG, Reiner AP, Aviv A, Lohman K, Liu Y, Ferrucci L, Horvath S (2018) An epigenetic biomarker of aging for lifespan and healthspan. Aging 10(4):573–591. https://doi.org/10.18632/aging.101414
Parker DC, Bartlett BN, Cohen HJ, Fillenbaum G, Huebner JL, Kraus VB, Pieper C, Belsky DW (2020) Association of blood chemistry quantifications of biological aging with disability and mortality in older adults. J Gerontol A Biol Sci Med Sci 75(9):1671–1679. https://doi.org/10.1093/gerona/glz219
Hastings WJ, Shalev I, Belsky DW (2019) Comparability of biological aging measures in the national health and nutrition examination study, 1999–2002. Psychoneuroendocrinology 106:171–178. https://doi.org/10.1016/j.psyneuen.2019.03.012
Justice JN, Ferrucci L, Newman AB, Aroda VR, Bahnson JL, Divers J, Espeland MA, Marcovina S, Pollak MN, Kritchevsky SB, Barzilai N, Kuchel GA (2018) A framework for selection of blood-based biomarkers for geroscience-guided clinical trials: report from the TAME biomarkers workgroup. Geroscience 40(5–6):419–436. https://doi.org/10.1007/s11357-018-0042-y
Verburgh K (2015) Nutrigerontology: why we need a new scientific discipline to develop diets and guidelines to reduce the risk of aging-related diseases. Aging Cell 14(1):17–24. https://doi.org/10.1111/acel.12284
Mathers JC (2015) Impact of nutrition on the ageing process. Br J Nutr 113(Suppl):S18-22. https://doi.org/10.1017/s0007114514003237
Stepaniak U, Polak M, Stefler D, Kozela M, Bobak M, Sanchez-Niubo A, Ayuso-Mateos JL, Haro JM, Pająk A (2022) Relationship between dietary macronutrients intake and the ATHLOS healthy ageing scale: results from the polish arm of the HAPIEE study. Nutrients. https://doi.org/10.3390/nu14122454
Kwon D, Belsky DW (2021) A toolkit for quantification of biological age from blood chemistry and organ function test data: BioAge. Geroscience 43(6):2795–2808. https://doi.org/10.1007/s11357-021-00480-5
Shan Z, Rehm CD, Rogers G, Ruan M, Wang DD, Hu FB, Mozaffarian D, Zhang FF, Bhupathiraju SN (2019) Trends in dietary carbohydrate, protein, and fat intake and diet quality among US adults, 1999–2016. JAMA: J Am Med Assoc 322(12):1178–1187. https://doi.org/10.1001/jama.2019.13771
Hou W, Han T, Sun X, Chen Y, Xu J, Wang Y, Yang X, Jiang W, Sun C (2022) Relationship between carbohydrate intake (quantity, quality, and time eaten) and mortality (total, cardiovascular, and diabetes): assessment of 2003–2014 national health and nutrition examination survey participants. Diabetes Care 45(12):3024–3031. https://doi.org/10.2337/dc22-0462
Panth N, Abbott KA, Dias CB, Wynne K, Garg ML (2018) Differential effects of medium- and long-chain saturated fatty acids on blood lipid profile: a systematic review and meta-analysis. Am J Clin Nutr 108(4):675–687. https://doi.org/10.1093/ajcn/nqy167
Chen J, Sun B, Zhang D (2019) Association of dietary n3 and n6 fatty acids intake with hypertension: NHANES 2007–2014. Nutrients. https://doi.org/10.3390/nu11061232
Kwon YJ, Lee HS, Park JY, Lee JW (2020) Associating intake proportion of carbohydrate, fat, and protein with all-cause mortality in Korean adults. Nutrients. https://doi.org/10.3390/nu12103208
World Health O (2010) Global recommendations on physical activity for health. World Health Organization, Geneva
Control CfD, Prevention (1994) Cigarette smoking among adults–United States, 1992, and changes in the definition of current cigarette smoking. MMWR Morb Mortal Wkly Rep 43(19):342–346
Johnson CL, Paulose-Ram R, Ogden CL, Carroll MD, Kruszon-Moran D, Dohrmann SM, Curtin LR (2013) National health and nutrition examination survey: analytic guidelines, 1999–2010. Vital Health Stat 2(161):1–24
Wood SN (2006) Generalized additive models: an introduction with R. chapman and hall/CRC
Quach A, Levine ME, Tanaka T, Lu AT, Chen BH, Ferrucci L, Ritz B, Bandinelli S, Neuhouser ML, Beasley JM, Snetselaar L, Wallace RB, Tsao PS, Absher D, Assimes TL, Stewart JD, Li Y, Hou L, Baccarelli AA, Whitsel EA, Horvath S (2017) Epigenetic clock analysis of diet, exercise, education, and lifestyle factors. Aging 9(2):419–446. https://doi.org/10.18632/aging.101168
You A (2015) Dietary guidelines for Americans. US department of health and human services and US department of agriculture 7
Tucker LA (2018) Dietary fiber and telomere length in 5674 U.S. Adults: an NHANES study of biological aging. Nutrients. https://doi.org/10.3390/nu10040400
Cassidy A, De Vivo I, Liu Y, Han J, Prescott J, Hunter DJ, Rimm EB (2010) Associations between diet, lifestyle factors, and telomere length in women. Am J Clin Nutr 91(5):1273–1280. https://doi.org/10.3945/ajcn.2009.28947
Ding B, Xiao R, Ma W, Zhao L, Bi Y, Zhang Y (2018) The association between macronutrient intake and cognition in individuals aged under 65 in China: a cross-sectional study. BMJ Open 8(1):e018573. https://doi.org/10.1136/bmjopen-2017-018573
Gopinath B, Flood VM, Kifley A, Louie JC, Mitchell P (2016) Association between carbohydrate nutrition and successful aging over 10 years. J Gerontol A Biol Sci Med Sci 71(10):1335–1340. https://doi.org/10.1093/gerona/glw091
Vercambre MN, Boutron-Ruault MC, Ritchie K, Clavel-Chapelon F, Berr C (2009) Long-term association of food and nutrient intakes with cognitive and functional decline: a 13-year follow-up study of elderly French women. Br J Nutr 102(3):419–427. https://doi.org/10.1017/s0007114508201959
Kaye DM, Shihata WA, Jama HA, Tsyganov K, Ziemann M, Kiriazis H, Horlock D, Vijay A, Giam B, Vinh A, Johnson C, Fiedler A, Donner D, Snelson M, Coughlan MT, Phillips S, Du XJ, El-Osta A, Drummond G, Lambert GW, Spector TD, Valdes AM, Mackay CR, Marques FZ (2020) Deficiency of prebiotic fiber and insufficient signaling through gut metabolite-sensing receptors leads to cardiovascular disease. Circulation 141(17):1393–1403. https://doi.org/10.1161/circulationaha.119.043081
Yang Y, Zhao LG, Wu QJ, Ma X, Xiang YB (2015) Association between dietary fiber and lower risk of all-cause mortality: a meta-analysis of cohort studies. Am J Epidemiol 181(2):83–91. https://doi.org/10.1093/aje/kwu257
Mendonça N, Granic A, Hill TR, Siervo M, Mathers JC, Kingston A, Jagger C (2019) Protein intake and disability trajectories in very old adults: the newcastle 85+ study. J Am Geriatr Soc 67(1):50–56. https://doi.org/10.1111/jgs.15592
Beasley JM, LaCroix AZ, Neuhouser ML, Huang Y, Tinker L, Woods N, Michael Y, Curb JD, Prentice RL (2010) Protein intake and incident frailty in the women’s health initiative observational study. J Am Geriatr Soc 58(6):1063–1071. https://doi.org/10.1111/j.1532-5415.2010.02866.x
Houston DK, Tooze JA, Garcia K, Visser M, Rubin S, Harris TB, Newman AB, Kritchevsky SB (2017) Protein intake and mobility limitation in community-dwelling older adults: the health ABC study. J Am Geriatr Soc 65(8):1705–1711. https://doi.org/10.1111/jgs.14856
Krok-Schoen JL, Archdeacon Price A, Luo M, Kelly OJ, Taylor CA (2019) Low dietary protein intakes and associated dietary patterns and functional limitations in an aging population: a NHANES analysis. J Nutr Health Aging 23(4):338–347. https://doi.org/10.1007/s12603-019-1174-1
Zhang Y, Zhou Q, Yang R, Hu C, Huang Z, Zheng C, Liang Q, Gong R, Zhu X, Gong H, Yuan H, Chen C, Li X, Zhang N, Yang Z, Sun L (2020) Serum branched-chain amino acids are associated with leukocyte telomere length and frailty based on residents from Guangxi longevity county. Sci Rep 10(1):10252. https://doi.org/10.1038/s41598-020-67010-9
Shikany JM, Barrett-Connor E, Ensrud KE, Cawthon PM, Lewis CE, Dam TT, Shannon J, Redden DT (2014) Macronutrients, diet quality, and frailty in older men. J Gerontol A Biol Sci Med Sci 69(6):695–701. https://doi.org/10.1093/gerona/glt196
Levine ME, Suarez JA, Brandhorst S, Balasubramanian P, Cheng CW, Madia F, Fontana L, Mirisola MG, Guevara-Aguirre J, Wan J, Passarino G, Kennedy BK, Wei M, Cohen P, Crimmins EM, Longo VD (2014) Low protein intake is associated with a major reduction in IGF-1, cancer, and overall mortality in the 65 and younger but not older population. Cell Metab 19(3):407–417. https://doi.org/10.1016/j.cmet.2014.02.006
Foscolou A, Critselis E, Tyrovolas S, Chrysohoou C, Naumovski N, Sidossis LS, Rallidis L, Matalas AL, Panagiotakos D (2021) The association of animal and plant protein with successful ageing: a combined analysis of MEDIS and ATTICA epidemiological studies. Public Health Nutr 24(8):2215–2224. https://doi.org/10.1017/s1368980020000427
Verspoor E, Voortman T, van Rooij FJA, Rivadeneira F, Franco OH, Kiefte-de Jong JC, Schoufour JD (2020) Macronutrient intake and frailty: the Rotterdam study. Eur J Nutr 59(7):2919–2928. https://doi.org/10.1007/s00394-019-02131-0
Simopoulos AP (1999) Essential fatty acids in health and chronic disease. Am J Clin Nutr 70(3 Suppl):560s–569s. https://doi.org/10.1093/ajcn/70.3.560s
Harris WS, Tintle NL, Imamura F, Qian F, Korat AVA, Marklund M, Djoussé L, Bassett JK, Carmichael PH, Chen YY, Hirakawa Y, Küpers LK, Laguzzi F, Lankinen M, Murphy RA, Samieri C, Senn MK, Shi P, Virtanen JK, Brouwer IA, Chien KL, Eiriksdottir G, Forouhi NG, Geleijnse JM, Giles GG, Gudnason V, Helmer C, Hodge A, Jackson R, Khaw KT, Laakso M, Lai H, Laurin D, Leander K, Lindsay J, Micha R, Mursu J, Ninomiya T, Post W, Psaty BM, Risérus U, Robinson JG, Shadyab AH, Snetselaar L, Sala-Vila A, Sun Y, Steffen LM, Tsai MY, Wareham NJ, Wood AC, Wu JHY, Hu F, Sun Q, Siscovick DS, Lemaitre RN, Mozaffarian D (2021) Blood n-3 fatty acid levels and total and cause-specific mortality from 17 prospective studies. Nat Commun 12(1):2329. https://doi.org/10.1038/s41467-021-22370-2
García-Esquinas E, Ortolá R, Banegas JR, Lopez-García E, Rodríguez-Artalejo F (2019) Dietary n-3 polyunsaturated fatty acids, fish intake and healthy ageing. Int J Epidemiol 48(6):1914–1924. https://doi.org/10.1093/ije/dyz196
Abbatecola AM, Cherubini A, Guralnik JM, Andres Lacueva C, Ruggiero C, Maggio M, Bandinelli S, Paolisso G, Ferrucci L (2009) Plasma polyunsaturated fatty acids and age-related physical performance decline. Rejuvenation Res 12(1):25–32. https://doi.org/10.1089/rej.2008.0799
Sandoval-Insausti H, Pérez-Tasigchana RF, López-García E, García-Esquinas E, Rodríguez-Artalejo F, Guallar-Castillón P (2016) Macronutrients intake and incident frailty in older adults: a prospective cohort study. J Gerontol A Biol Sci Med Sci 71(10):1329–1334. https://doi.org/10.1093/gerona/glw033
Thomas A, Belsky DW, Gu Y (2023) Healthy lifestyle behaviors and biological aging in the U.S. National health and nutrition examination surveys 1999–2018. J Gerontol Ser A Biol Sci Med Sci 78(9):1535–1542. https://doi.org/10.1093/gerona/glad082
Soltani S, Jayedi A, Shab-Bidar S, Becerra-Tomás N, Salas-Salvadó J (2019) Adherence to the mediterranean diet in relation to all-cause mortality: a systematic review and dose-response meta-analysis of prospective cohort studies. Adv Nutr 10(6):1029–1039. https://doi.org/10.1093/advances/nmz041
Grosso G, Marventano S, Yang J, Micek A, Pajak A, Scalfi L, Galvano F, Kales SN (2017) A comprehensive meta-analysis on evidence of Mediterranean diet and cardiovascular disease: are individual components equal? Crit Rev Food Sci Nutr 57(15):3218–3232. https://doi.org/10.1080/10408398.2015.1107021
Wu L, Sun D (2017) Adherence to Mediterranean diet and risk of developing cognitive disorders: an updated systematic review and meta-analysis of prospective cohort studies. Sci Rep 7:41317. https://doi.org/10.1038/srep41317
Morris MC, Evans DA, Bienias JL, Tangney CC, Wilson RS (2004) Dietary fat intake and 6-year cognitive change in an older biracial community population. Neurology 62(9):1573–1579. https://doi.org/10.1212/01.wnl.0000123250.82849.b6
Okereke OI, Rosner BA, Kim DH, Kang JH, Cook NR, Manson JE, Buring JE, Willett WC, Grodstein F (2012) Dietary fat types and 4-year cognitive change in community-dwelling older women. Ann Neurol 72(1):124–134. https://doi.org/10.1002/ana.23593
Laitinen MH, Ngandu T, Rovio S, Helkala EL, Uusitalo U, Viitanen M, Nissinen A, Tuomilehto J, Soininen H, Kivipelto M (2006) Fat intake at midlife and risk of dementia and Alzheimer’s disease: a population-based study. Dement Geriatr Cogn Disord 22(1):99–107. https://doi.org/10.1159/000093478
de Souza RJ, Mente A, Maroleanu A, Cozma AI, Ha V, Kishibe T, Uleryk E, Budylowski P, Schünemann H, Beyene J, Anand SS (2015) Intake of saturated and trans unsaturated fatty acids and risk of all cause mortality, cardiovascular disease, and type 2 diabetes: systematic review and meta-analysis of observational studies. BMJ 351:h3978. https://doi.org/10.1136/bmj.h3978
Fritsche KL (2015) The science of fatty acids and inflammation. Adv Nutr 6(3):293s–301s. https://doi.org/10.3945/an.114.006940
Roderka MN, Puri S, Batsis JA (2020) Addressing obesity to promote healthy aging. Clin Geriatr Med 36(4):631–643. https://doi.org/10.1016/j.cger.2020.06.006
Mooradian AD (2020) The merits and the pitfalls of low carbohydrate diet: a concise review. J Nutr Health Aging 24(7):805–808. https://doi.org/10.1007/s12603-020-1417-1
Si H, Liu D (2014) Dietary antiaging phytochemicals and mechanisms associated with prolonged survival. J Nutr Biochem 25(6):581–591. https://doi.org/10.1016/j.jnutbio.2014.02.001
Belsky DW, Moffitt TE, Cohen AA, Corcoran DL, Levine ME, Prinz JA, Schaefer J, Sugden K, Williams B, Poulton R, Caspi A (2018) Eleven telomere, epigenetic clock, and biomarker-composite quantifications of biological aging: do they measure the same thing? Am J Epidemiol 187(6):1220–1230. https://doi.org/10.1093/aje/kwx346
Acknowledgements
The authors thank the investigators and participants of the National Health and Nutrition Examination Survey, the parent study, who made this report possible.
Funding
The study was supported by funding from the following: Scientific Research Project of Hunan Provincial Health Commission (No. 202103050756), Changsha Municipal Natural Science Foundation (No. kq2014276), Provincial Natural Science Foundation of Hunan (No. 2021JJ40972), National Youth Science Foundation of China (No. 81600536).
Author information
Authors and Affiliations
Contributions
Study concept: WHC; Acquisition of data: XZ, RM; Analysis and interpretation of data: XZ, WJD; Drafting of the manuscript: WHC, JX, XZ; Study supervision: HX, QLZ, QZ; Critical revision of the manuscript for important intellectual content: all declared authors; All authors have read and approved the final manuscript.
Corresponding authors
Ethics declarations
Conflict of interest
The authors declare that they have no competing interests.
Ethical approval
The study was conducted according to the guidelines of the Declaration of Helsinki. All study participants gave informed consent in accordance with the Institutional Review Board and study ethic guidelines at the Centers for Disease Control and Prevention.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Zhu, X., Xue, J., Maimaitituerxun, R. et al. Relationship between dietary macronutrients intake and biological aging: a cross-sectional analysis of NHANES data. Eur J Nutr 63, 243–251 (2024). https://doi.org/10.1007/s00394-023-03261-2
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00394-023-03261-2