Abstract
Purpose
The standard treatment of rectal adenocarcinoma is total mesorectal excision (TME), in many cases requires a temporary or permanent stoma. TME is associated with high morbidity and genitourinary alterations. Transanal endoscopic microsurgery (TEM) allows access to tumors up to 20 cm from the anal verge, achieves minimal postoperative morbidity and mortality rates, and does not require an ostomy. The treatment of T2, N0, and M0 cancers remains controversial. Preoperative chemoradiotherapy (CRT) in association with TEM reduces local recurrence and increases survival. The TAU-TEM study aims to demonstrate the non-inferiority of the oncological outcomes and the improvement in morbidity and quality of life achieved with TEM compared with TME.
Methods
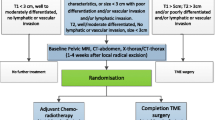
Prospective, multicenter, randomized controlled non-inferiority trial includes patients with rectal adenocarcinoma less than 10 cm from the anal verge and up to 4 cm in size, staged as T2 or T3-superficial N0-M0. Patients will be randomized to two areas: CRT plus TEM or radical surgery (TME). Postoperative morbidity and mortality will be recorded and patients will complete the quality of life questionnaires before the start of treatment, after CRT in the CRT/TEM arm, and 6 months after surgery in both arms. The estimated sample size for the study is 173 patients. Patients will attend follow-up controls for local and systemic relapse.
Conclusions
This study aims to demonstrate the preservation of the rectum after preoperative CRT and TEM in rectal cancer stages T2–3s, N0, M0 and to determine the ability of this strategy to avoid the need for radical surgery (TME).
Trial registration
ClinicalTrials.gov identifier: NCT01308190. Número de registro del Comité de Etica e Investigación Clínica (CEIC) del Hospital universitario Parc Taulí: TAU-TEM-2009-01.

Similar content being viewed by others
References
Sun G, Tang Y, X L, Meng J, Liang G (2014) Analysis of 116 cases of rectal cancer treated by transanal local excision. World J Surg Oncol 12:202
Borstlap WAA, Coeymans TJ, Tanis PJ, Marijnen CAM, Cunningham C, Bemelman WA, Tuynman JB (2016) Meta-analysis of oncological outcomes after local excision of pT1–2 rectal cancer requiring adjuvant (chemo)radiotherapy or completion surgery. Br J Surg 103:1105–1116
Law WL, Chu KW (2004) Anterior resection for rectal cancer with mesorectal excision: a prospective evaluation of 622 patients. Ann Surg 240:260–268
Kneist W, Junginger T (2004) Residual urine volume after total mesorectal excision: an indicator of pelvic autonomic nerve preservation? Results of a case-control study. Color Dis 6:432–437
Shah EF, Huddy SPJ (2001) A prospective study of genito-urinary dysfunction after surgery for colorectal cancer. Color Dis 3(122):5
Buess G, Hutterer F, Theiss J et al (1984) A system for a transanal endoscopic rectum operation. Chirurg 55:677–680
Lee W, Lee D, Choi S, Chun H (2003) Transanal endoscopio microsurgery and radical surgery for T1 and T2 rectal cancer. Surg Endosc 17:1283–1287
Serra Aracil X, Bombardó Junca J, Mora López L, Alcántara Moral M, Ayguavives Garnica I, Navarro Soto S (2006) La microcirugía endoscopica transanal (TEM). situacion actual y expectativas de futuro. Cir Esp 80:123–132
Serra Aracil X, Bombardó Juncá J, Mora López L et al (2009) Lugar de la cirugía local en el adenocarcinoma de recto T2N0M0. Cir Esp 85:103–109
Habr-Gama A, Perez RO, Nadalin W et al (2004) Operative versus nonoperative treatment for stage 0 distal rectal cancer following chemoradiation therapy: long-term results. Ann Surg 240:711–717
Maas M, Nelemans PJ, Valentini V et al (2010) Long-term outcome in patients with a pathological complete response after chemoradiation for rectal cancer: a pooled analysis of individual patient data. Lancet Oncol 11:835–844
Coco C, Rizzo G, Mattana C et al (2013) Transanal endoscopic microsurgery after neoadjuvant radiochemotherapy for locally advanced extraperitoneal rectal cancer: Short-term morbidity and functional outcome. Surg Endosc 27:2860–2867
Serra-Aracil X, Pericay C, Mora-Lopez L, Garcia Pacheco JC, Latorraca JI, Ocaña-Rojas J, Casalots A, Ballesteros E, Navarro-Soto S (2017) Neoadjuvant therapy and transanal endoscopic surgery in T2-T3 superficial, N0, M0 rectal tumors. Local recurrence, complete clinical and pathological response. Cir Esp 95:199–207
Dindo D, Demartines N, Clavien PA (2004) Classification of surgical complications: a new proposal with evaluation in a cohort of 6336 patients and results of a survey. Ann Surg 240:205–213
Slankamenac K, Graf R, Barkun J et al (2013) The comprehensive complication index: a novel continuous scale to measure surgical morbidity. Ann Surg 258:1–7
Hildebrandt U, Feifel G (1985) Preoperative staging of rectal cancer by intrarectal ultrasound. Dis Colon rectum 28:42–46
Brown G, Richards CJ, Newcombe RG, Dallimore NS, Radcliffe AG, Carey DP, Bourne MW, Williams GT (1999) Rectal carcinoma: thin-section MR imaging for staging in 28 patients. Radiology 211:215–222
Brown G, Richards CJ, Bourne MW, Newcombe RG, Radcliffe AG, Dallimore NS, Williams GT (2003) Morphologic predictors of lymph node status in rectal cancer with use of high-spatial-resolution MR imaging with histopathologic comparison. Radiology 227:371–377
Mercury study grup (2007) Extramural depth of tumor invasion at thin-section MR in patients with rectal cancer: results of the MERCURY study. Radiology 243:132–139
Therasse P, Arbuck SG, Eisenhauer EA, Wanders J, Kaplan RS, Rubinstein L, Verweij J, Van Glabbeke M, van OosteromAT CMC, Gwyther SG (2000) New guidelines to evaluate the response to treatment in solid tumors. J Natl Cancer Inst 92:205–216
Arraras JI, Arias de la Vega F, Vera R, Manterota A, Martinez M, Villafranca E, Salgado E (2006) Quality of life assessment through the EORTC questionnaires of locally advanced rectal cancer patients treated with preoperative chemo-radiotherapy. Clin Transl Oncol 8:423–429
Aaronson NK, Ahmedzai S, Bergman B et al (1993) The European Organization for Research and Treatment of Cancer QLQ-C30: a quality-of-life instrument for use in international clinical trials in oncology. J Natl Cancer Inst 85:365–376
Sprangers MA, te Velde A, Aaronson NK (1999) The construction and testing of the EORTC colorectal cancer-specific quality of life questionnaire module (QLQ-CR38). European Organization for Research and Treatment of Cancer Study Group on Quality of Life. Eur J Cancer 35:238–247
Karnofsky DA, Abelmann WH, Craver LF, Burchenal JH (1948) The use of nitrogen mustards in the palliative treatment of carcinoma. Cancer 1:634–656
Emanuel EJ (2013) Reconsidering the Declaration of Helsinki. Lancet (London, England) 381:1532–1533
Chan A-W, Tetzlaff JM, Altman DG et al (2013) SPIRIT 2013 statement: defining standard protocol items for clinical trials. Ann Intern Med 158:200–207
Mohiuddin M, Regine WF, John WJ et al (2000) Preoperative chemoradiation in fixed distal rectal cancer: dose time factors for pathological complete response. Int J Radiat Oncol Biol Phys 46:883–888
Ahmad NR, Marks G, Mohiuddin M et al (1993) High dose preoperative radiation for cancer of the rectum: impact of radiation dose on patterns of failure and survival. Int J Radiat Oncol Biol Phys 27:773–778
Rocha JJ, Feres O (2008) Transanal endoscopic operation: a new proposal. Acta Cir Bras 23:93–104 discussion 104
Atallah S, Albert M, Larach S (2010) Transanal minimally invasive surgery: a giant leap forward. Surg Endosc 24:2200–2205
Heald RJ, Ryall RDH (1986) Recurrence and survival after total mesorectal excision for rectal cancer. Lancet 1:1479–1482
Bouzourene H, Bosman FT, Seelentag W, Matter M, Coucke P (2002) Importance of tumor regression assessment in predicting the outcome in patients with locally advanced rectal carcinoma who are treated with preoperative radiotherapy. Cancer 94:1121–1130
Dworak O, Keilholz L, Hoffmann A (1997) Pathological features of rectal cancer after preoperative radiochemotherapy. Int J Color Dis 12:19–23
Kaul S, Diamond GA (2006) Good enough: a primer on the analysis and interpretation of noninferiority trials. Ann Intern Med 145:62–69
Piaggio G, Elbourne DR, Altman DG, Pocock SJ, Evans SJ, CONSORT Group (2006) Reporting of noninferiority and equivalence randomized trials: an extension of the CONSORT statement. JAMA 295:1152–1160
Sauer R, Becker H, Hohenberger W et al (2004) Preoperative versus postopreative chemoradiotherapy for rectal cancer. N Engl J Med 351:1731–1740
(1990) NHI consensus conference: adjuvant therapy for patients with colon and rectal cancer. JAMA 264:1444–1450
Merkel S, Mansmann U, Siassi M, Papadopoulos T, Hohenberger W, Hermanek P (2001) The prognostic inhomogeneity in pT3 rectal carcinomas. Int J Color Dis 16:298–304
Arezzo A, Arolfo S, Allaix ME et al (2015) Results of neoadjuvant short-course radiation therapy followed by transanal endoscopic microsurgery for T1-T2 N0 extraperitoneal rectal cancer. Int J Radiat Oncol Biol Phys 92:299–306
Garcia-Aguilar J, Shi Q, Thomas CR Jr et al (2012) A phase II trial of neoadjuvant chemoradiation and local excision for T2N0 rectal cancer: preliminary results of the ACOSOG Z6041 trial. Ann Surg Oncol 19:384–391
Garcia-Aguilar J, Renfro LA, Chow OS et al (2015) Organ preservation for clinical T2N0 distal rectal cancer using neoadjuvant chemoradiotherapy and local excision (ACOSOG Z6041): results of an open-label, single-arm, multi-institutional, phase 2 trial. Lancet Oncol 16:1537–1546
Perez RO, Habr-Gama A, GP S˜o J˜o, Proscurshim I, Scanavini Neto A, Gama-Rodrigues J (2011) Transanal endoscopic microsurgery for residual rectal cancer after neoadjuvant chemoradiation therapy is associated with significant immediate pain and hospital readmission rates. Dis Colon rectum 54:545–551
Arraras JI, Arias de la vega F, Vera R, Manterota A, Martinez M, Villafranca E, Salgado E (2006) Quality of life assessment through the EORTC questionnaires of locally advanced rectal cancer patients treated with preoperative chemo-radiotherapy. Clin Transl Oncol 8:423–429
Smith JJ, Chow OS, Gollub MJ, Nash GM, Temple LK, Weiser MR, Guillem JG, Paty PB, Avila K, Garcia-Aguilar J, Rectal Cancer Consortium (2015) Organ preservation in rectal adenocarcinoma: a phase II randomized controlled trial evaluating 3-year disease-free survival in patients with locally advanced rectal cancer treated with chemoradiation plus induction or consolidation chemotherapy, and total mesorectal excision or nonoperative management. BMC Cancer 15:767
Rullier E, Rouanet P, Tuech JJ, Valverde A, Lelong B, Rivoire M, Faucheron JL, Jafari M, Portier G, Meunier B, Sileznieff I, Prudhomme M, Marchal F, Pocard M, Pezet D, Rullier A, Vendrely V, Denost Q, Asselineau J, Doussau A (2017) Organ preservation for rectal cancer (GRECCAR 2): a prospective, randomised, open-label, multicentre, phase 3 trial. Lancet 390:469–479
Acknowledgements
We thank all the members of the multidisciplinary committee for colorectal tumors at our hospital for their support. We are also grateful to Cristina Gomez Vigo for correcting the manuscript and Michael Maudsley for help with the English.
TAU-TEM study group
Hospital Parc Taulí: Xavier Serra-Aracil, Carles Pericay, Laura Mora, Sheila Serra, Eugeni Saigi, Emma Dotor, Aleidis Pisa, Ismael Macias, Anna Pallisera, Salvador Navarro. Hospital Clinic I Provincial: Antonio Lacy, Anna Otero. Hospital de Bellvitge: Sebastiano Biondo, Thomas Golda. Hospital de la Santa Creu i Sant Pau: Eduardo Tarragona, Pilar Hernández; Mª Carmen Martínez, Juan Carlos Pernas, Marta Martín, Dolores González, David Paez, Xavier Cussó, C. Balagué. Hospital General Universitari de Valencia: Mª José García Coret, Francisco Villalba Ferrer. Hospital Universitario La Paz: Beatriz Díaz San Andrés, Álvarez Gallego, Higuera, Prieto. Hospital Universitario de Getafe: Jose Luis Ramos, Javier Jiménez Miramó, Javier García Septiem, Francisco Angulo. Hospital Marqués de Valdecilla: Julio Castillo, Joaquín Alonso Martín, Isabel Seco, Carlos Manuel Palazuelo. Hospital Torrecárdenas de Almeria: Ángel Reina, Francisco A. Rubio Gil, Carmen Caro, Rubén Varela, Fco. Manuel Ramos, Ana Fernández, Ricardo Belda, Ramon Solbes, Begoña Medina, Piedad Reche. Hospital Universitari Vall d’Hebrón: Eloy Espín, Francesc Vallribera, Stefania Landolfini, Jaume Capdevila. Hospital del Mar: Marta Pascual, Silvia Salvans, Miguel Pera. Hospital Reina Sofía. Córdoba: César Díaz, Jose Gomez Barbadillo, Amalia Palacios, Carlos Villar Pastor, María Pleguezuelo, Francisco Triviño, José L. Martínez de Dueñas, Auxiliadora Gómez España y Elena Navarro Rodriguez. Hospital de Sagunto: Roberto Lozoya Trujillo, Andrés Frangi, Mª Dolores Ruiz Carmona, Rodolfo Rodríguez Carrillo, Mireia Gil, Vicente Miranda. Hospital de Cabueñes. Gijón: Carlos Álvarez Laso, Paola Lora. Hospital de Donosti: José Mª Enriquez Navascues, Carlos Placer, Dra. Nerea Borda, Adelaida La Casta, JL Elosegui, Yolanda Saralegui, Elena Guimón, JA Múgica. Hospital General Universitario de Elche: Javier Gallego Plazas, Antonio Arroyo. Hospital Universitari Juan XXIII: Aleidis Caro, Monica Millan.
Funding
Funding obtained by the principal investigator (PI): Xavier Serra-Aracil, Olga Torres Grant, Grant from the Ministry of Health and Social Policy, Independent Clinical Research grants Ayudas de Investigación Clínica Independiente, Parc Taulí Foundation grant, and Spanish Coloproctology Foundation grant.
Author information
Authors and Affiliations
Consortia
Contributions
XSA, CP, and LM wrote and edited the paper. TG, AR, SD, and ET will contribute patients to the study and are active in the management of the protocol. All authors have reviewed the research protocol, revising it critically for intellectual content. Each author has participated sufficiently in the work of reviewing and approving the protocol as written. In addition, FV, JMEN, AA, MP, JC, CD, AC, and RL will contribute patients and have reviewed and approved the protocol. JCGP and SS are the clinical research managers of the trial.
Corresponding author
Ethics declarations
Competing interests
The authors have no competing interests to declare.
Consent for publication
Not applicable.
Ethics approval and consent to participate
The study has been approved by the local ethics committees of the participating centers.
Availability of data and materials
Not applicable.
Rights and permissions
About this article
Cite this article
Serra-Aracil, X., Pericay, C., Golda, T. et al. Non-inferiority multicenter prospective randomized controlled study of rectal cancer T2–T3s (superficial) N0, M0 undergoing neoadjuvant treatment and local excision (TEM) vs total mesorectal excision (TME). Int J Colorectal Dis 33, 241–249 (2018). https://doi.org/10.1007/s00384-017-2942-1
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00384-017-2942-1