Abstract
Purpose
Many biliary atresia (BA) patients will eventually develop liver failure even after a successful Kasai portoenterostomy. A common complication of long-term BA survivors with their native liver is problematic portal hypertension. The aim of this study was to defend the view that portosystemic shunts can delay or negate the need for transplantation in these children.
Methods
A retrospective single center review of the efficacy of portosystemic shunts in BA patients after a successful Kasai portoenterostomy was conducted.
Results
From 1991 to 2017, 11 patients received portosystemic shunts. Median age of Kasai operation was 48 (36–61) days. Shunts were performed at the median age of 6.2 (4.1–6.8) years. Three of these eleven patients required subsequent liver transplantation. OS at 5 and 10 years were 90.9% and 81.8%, respectively. TFS at 5 and 10 years were 90.9% and 72.7%, respectively. Long-term complications included mild encephalopathy in 2 patients, hypersplenism in 3, and cholestasis in 1.
Conclusion
Portosystemic shunt for the treatment of portal hypertension in carefully selected BA patients is an effective option in delaying or negating the need for liver transplantation.

Similar content being viewed by others
References
Australia & New Zealand Liver and Intestinal Transplant Registry_30thReport.pdf.
Kim WR, Lake JR, Smith JM, Schladt DP, Skeans MA, Noreen SM, Robinson AM, Miller E, Snyder JJ, Israni AK, Kasiske BL (2019) OPTN/SRTR 2017 annual data report: liver. Am J Transpl 19(Suppl 2):184–283. https://doi.org/10.1111/ajt.15276
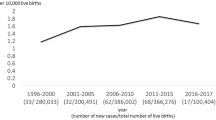
Hopkins PC, Yazigi N, Nylund CM (2017) Incidence of biliary atresia and timing of hepatoportoenterostomy in the United States. J Pediatr 187:253–257. https://doi.org/10.1016/j.jpeds.2017.05.006
Shun A, Delaney DP, Martin HC, Henry GM, Stephen M (1997) Portosystemic shunting for paediatric portal hypertension. J Pediatr Surg 32(3):489–493. https://doi.org/10.1016/s0022-3468(97)90613-8
Shneider BL, de ville de Goyet J, Leung DH, Srivastava A, Ling SC, Duche M, McKiernan P, Superina R, Squires RH, Bosch J, Groszmann R, Sarin SK, de Franchis R, Mazariegos GV (2016) Primary prophylaxis of variceal bleeding in children and the role of MesoRex bypass: summary of the Baveno VI pediatric satellite symposium. Hepatology 63(4):1368–1380. https://doi.org/10.1002/hep.28153
Karrer FM, Wallace BJ, Estrada AE (2017) Late complications of biliary atresia: hepatopulmonary syndrome and portopulmonary hypertension. Pediatr Surg Int 33(12):1335–1340. https://doi.org/10.1007/s00383-017-4176-2
Superina RA, Alonso EM (2006) Medical and surgical management of portal hypertension in children. Curr Treat Options Gastroenterol 9(5):432–443. https://doi.org/10.1007/bf02738533
Villanueva C, Balanzó J, Novella MT, Soriano G, Sáinz S, Torras X, Cussó X, Guarner C, Vilardell F (1996) Nadolol plus isosorbide mononitrate compared with sclerotherapy for the prevention of variceal rebleeding. N Engl J Med 334(25):1624–1629. https://doi.org/10.1056/nejm199606203342502
Villanueva C, Lopez-Balaguer JM, Aracil C, Kolle L, Gonzalez B, Minana J, Soriano G, Guarner C, Balanzo J (2004) Maintenance of hemodynamic response to treatment for portal hypertension and influence on complications of cirrhosis. J Hepatol 40(5):757–765. https://doi.org/10.1016/j.jhep.2004.01.017
Poddar U, Shava U, Yachha SK, Agarwal J, Kumar S, Baijal SS, Srivastava A (2015) beta-Blocker therapy ameliorates hypersplenism due to portal hypertension in children. Hepatol Int 9(3):447–453. https://doi.org/10.1007/s12072-014-9575-z
Villanueva C, Albillos A, Genescà J, Garcia-Pagan JC, Calleja JL, Aracil C, Bañares R, Morillas RM, Poca M, Peñas B, Augustin S, Abraldes JG, Alvarado E, Torres F, Bosch J (2019) β blockers to prevent decompensation of cirrhosis in patients with clinically significant portal hypertension (PREDESCI): a randomised, double-blind, placebo-controlled, multicentre trial. Lancet 393(10181):1597–1608. https://doi.org/10.1016/s0140-6736(18)31875-0
Garcia-Tsao G, Abraldes JG, Berzigotti A, Bosch J (2017) Portal hypertensive bleeding in cirrhosis: risk stratification, diagnosis, and management: 2016 practice guidance by the American Association for the study of liver diseases. Hepatology 65(1):310–335. https://doi.org/10.1002/hep.28906
Huppert PE, Goffette P, Astfalk W, Sokal EM, Brambs HJ, Schott U, Duda SH, Schweizer P, Claussen CD (2002) Transjugular intrahepatic portosystemic shunts in children with biliary atresia. Cardiovasc Intervent Radiol 25(6):484–493. https://doi.org/10.1007/s00270-002-1913-1
Heyman MB, LaBerge JM, Somberg KA, Rosenthal P, Mudge C, Ring EJ, Snyder JD (1997) Transjugular intrahepatic portosystemic shunts (TIPS) in children. J Pediatr 131(6):914–919. https://doi.org/10.1016/s0022-3476(97)70043-x
Hackworth CA, Leef JA, Rosenblum JD, Whitington PF, Millis JM, Alonso EM (1998) Transjugular intrahepatic portosystemic shunt creation in children: initial clinical experience. Radiology 206(1):109–114. https://doi.org/10.1148/radiology.206.1.9423659
Di Giorgio A, Nicastro E, Agazzi R, Colusso M, D’Antiga L (2020) Long-term outcome of transjugular intrahepatic portosystemic shunt in children with portal hypertension. J Pediatr Gastroenterol Nutr 70(5):615–622. https://doi.org/10.1097/MPG.0000000000002597
Esquivel CO, Klintmalm G, Iwatsuki S, Makowka L, Gordon RD, Tzakis A, Starzl TE (1987) Liver transplantation in patients with patent splenorenal shunts. Surgery 101(4):430–432
Lautz TB, Keys LA, Melvin JC, Ito J, Superina RA (2013) Advantages of the meso-Rex bypass compared with portosystemic shunts in the management of extra-hepatic portal vein obstruction in children. J Am Coll Surg 216(1):83–89. https://doi.org/10.1016/j.jamcollsurg.2012.09.013
Guerin F, Charre L, Jasienski S, Duche M, Franchiabella S, Bernard O, Jacquemin E, Agostini H, Gauthier F, Branchereau S (2019) The efficacy of surgical shunts to treat severe portal hypertension after a Kasai procedure for biliary atresia. J Pediatr Surg 54(3):531–536. https://doi.org/10.1016/j.jpedsurg.2018.06.023
Sheil AG, Stephen MS, Chui AK, Ling J, Bookallil MJ (1997) A liver transplantation technique in a patient with a thrombosed portal vein and a functioning renal-lieno shunt. Clin Transpl 11(1):71–73
Kanazawa H, Takada Y, Ogura Y, Oike F, Egawa H, Uemoto S (2009) Mesorenal shunt using inferior mesenteric vein and left renal vein in a case of LDLT. Transpl Int 22(12):1189–1192. https://doi.org/10.1111/j.1432-2277.2009.00928.x
Kinaci E, Kayaalp C (2016) Portosystemic shunts for “too small-for-size syndrome” After Liver Transplantation: a systematic review. World J Surg 40(8):1932–1940. https://doi.org/10.1007/s00268-016-3518-x
Kokai H, Sato Y, Yamamoto S, Oya H, Nakatsuka H, Watanabe T, Takizawa K, Hatakeyama K (2008) Successful super-small-for-size graft liver transplantation by decompression of portal hypertension via splenectomy and construction of a mesocaval shunt: a case report. Transplant Proc 40(8):2825–2827. https://doi.org/10.1016/j.transproceed.2008.08.080
D’Antiga L (2012) Medical management of esophageal varices and portal hypertension in children. Semin Pediatr Surg 21(3):211–218. https://doi.org/10.1053/j.sempedsurg.2012.05.004
Yadav SK, Srivastava A, Srivastava A, Thomas MA, Agarwal J, Pandey CM, Lal R, Yachha SK, Saraswat VA, Gupta RK (2010) Encephalopathy assessment in children with extra-hepatic portal vein obstruction with MR, psychometry and critical flicker frequency. J Hepatol 52(3):348–354. https://doi.org/10.1016/j.jhep.2009.12.012
Masson S, Mardini HA, Rose JD, Record CO (2008) Hepatic encephalopathy after transjugular intrahepatic portosystemic shunt insertion: a decade of experience. QJM 101(6):493–501. https://doi.org/10.1093/qjmed/hcn037
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflicts of interest
The authors declare that they have no conflicts of interest.
Human and animal rights
This article does not contain any studies with animals performed by any of the authors.
Ethical approval
This study was approved by the hospital’s ethical board (HREC reference number: LNR/15/SCHN/307, SSA reference number: LNRSSA/16/SCHN/270).
Informed consent
The individual written informed consent was waived because of the retrospective design.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Shimizu, T., Shun, A. & Thomas, G. Portosystemic shunt for portal hypertension after Kasai operation in patients with biliary atresia. Pediatr Surg Int 37, 101–107 (2021). https://doi.org/10.1007/s00383-020-04773-2
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00383-020-04773-2