Abstract
Introduction
Hospital readmission rates are used as a metric of the quality of patient care in adults. Readmission data is lacking for pediatric surgical patients. The objective of this study is to evaluate our institution’s 30-day unexpected pediatric surgical readmission data to identify potentially preventable readmissions.
Methods
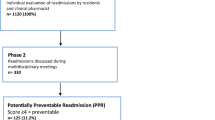
An internal database of all pediatric surgical 30-day readmissions to two tertiary-referral children’s hospitals in a single health system was reviewed. All pediatric general surgery admissions between January 2008 and May 2013 with hospital readmission within 30 days were included in the study. Patient demographics, diagnoses, cause of readmission, procedure performed, and length of stay were recorded. Charts were individually reviewed to evaluate causality of readmission.
Results
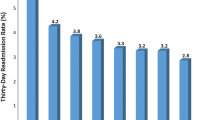
There were 2217 pediatric general surgery admissions during the study period. Of these, 145 (6.5 %) experienced unexpected readmission within 30 days. One-third of all readmissions occurred in infants between 0 and 364 days of age, 50 % occurred in those under 2 years and wholly 80 % of all readmissions occurred in those under 9 years of age. A majority of readmissions were associated with chronic comorbid conditions.
Conclusion
Analysis of pediatric surgical readmission data may assist hospitals in focusing quality of care and cost effectiveness strategies. Development of coordination of care strategies and discharge planning involving both pediatric surgical teams and pediatric hospitalists/specialists may reduce pediatric surgical readmission rates.


Similar content being viewed by others
References
Srivastava R, Keren R (2013) Pediatric readmissions as a hospital quality measure. JAMA 309(4):396–398. doi:10.1001/jama.2012.217006
Berry JG, Toomey SL, Zaslavsky AM et al (2013) Pediatric readmission prevalence and variability across hospitals. JAMA 309(4):372–380. doi:10.1001/jama.2012.188351
Averill RF, McCullough EC, Hughes JS, Goldfield NI, Vertrees JC, Fuller RL (2009) Redesigning the medicare inpatient PPS to reduce payments to hospitals with high readmission rates. Health Care Financ Rev 30(4):1–15
Goldfield NIN, McCullough ECE, Hughes JSJ et al (2008) Identifying potentially preventable readmissions. Health Care Financ Rev 30(1):75–91
Dougherty D, Schiff J, Mangione-Smith R (2011) The Children’s Health Insurance Program Reauthorization Act quality measures initiatives: moving forward to improve measurement, care, and child and adolescent outcomes. Acad Pediatr 11(3):S1–S10. doi:10.1016/j.acap.2011.02.009
Feudtner C, Levin JE, Srivastava R et al (2009) How well can hospital readmission be predicted in a cohort of hospitalized children? A retrospective, multicenter study. Pediatrics 123(1):286–293
Hain PD, Gay JC, Berutti TW, Whitney GM, Wang W, Saville BR (2013) Preventability of early readmissions at a children’s hospital. Pediatrics 131(1):e171–e181. doi:10.1542/peds.2012-0820
Berry JG, Hall DE, Kuo DZ et al (2011) Hospital utilization and characteristics of patients experiencing recurrent readmissions within children’s hospitals. JAMA 305(7):682–690. doi:10.1001/jama.2011.122
Rice-Townsend S, Hall M, Barnes JN, Baxter JK, Rangel SJ (2012) Hospital readmission after management of appendicitis at freestanding children’s hospitals: contemporary trends and financial implications. J Pediatr Surg 47(6):1170–1176. doi:10.1016/j.jpedsurg.2012.03.025
Berry JG, Hall MA, Sharma V, Goumnerova L, Slonim AD, Shah SS (2008) A multi-institutional, 5-year analysis of initial and multiple ventricular shunt revisions in children. Neurosurgery 62(2):445–453. doi:10.1227/01.neu.0000316012.20797.04 discussion 453-4
Lautz TB, Reynolds M (2011) Context and significance of emergency department visits and readmissions after pediatric appendectomy. J Pediatr Surg 46(10):1918–1922
Feudtner C, Hays RM, Haynes G, Geyer JR, Neff JM, Koepsell TD (2001) Deaths attributed to pediatric complex chronic conditions: national trends and implications for supportive care services. Pediatrics 107(6):E99
Gay JC, Hain PD, Grantham JA, Saville BR (2011) Epidemiology of 15-day readmissions to a children’s hospital. Pediatrics 127(6):e1505–e1512. doi:10.1542/peds.2010-1737
Feudtner C, Pati S, Goodman DM et al (2010) State-level child health system performance and the likelihood of readmission to children’s hospitals. J Pediatr. doi:10.1016/j.jpeds.2010.01.049
Simon TD, Berry J, Feudtner C et al (2010) Children with complex chronic conditions in inpatient hospital settings in the United States. Pediatrics 126(4):647–655. doi:10.1542/peds.2009-3266
Lawson EH, Hall BL, Louie R et al (2013) Association between occurrence of a postoperative complication and readmission: implications for quality improvement and cost savings. Ann Surg. doi:10.1097/SLA.0b013e31828e3ac3
Tsai TC, Joynt KE, Orav EJ, Gawande AA, Jha AK (2013) Variation in surgical-readmission rates and quality of hospital care. N Engl J Med 369(12):1134–1142. doi:10.1056/NEJMsa1303118
Bardach NS, Vittinghoff E, Asteria-Peñaloza R et al (2013) Measuring hospital quality using pediatric readmission and revisit rates. Pediatrics 132(3):429–436. doi:10.1542/peds.2012-3527
Rice-Townsend S, Hall M, Barnes JN, Lipsitz S, Rangel SJ (2013) Variation in risk-adjusted hospital readmission after treatment of appendicitis at 38 children’s hospitals: an opportunity for collaborative quality improvement. Ann Surg 257(4):758–765
Marshall AP, Gay JC, Hain PD, Snyder R, Tice JS, Rauth TP, Blakely ML (2012) Which diagnoses are responsible for most 30-day pediatric surgery readmissions? J Am Coll Surg 215(3):S98–S99
Gonzalez AA, Shih T, Dimick JB, Ghaferi AA (2014) Using same hospital readmission rates to estimate all-hospital readmission rates. J Am Coll Surg 219(4):656–663
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Burjonrappa, S., Theodorus, A., Shah, A. et al. Pediatric surgery readmissions: a root cause analysis. Pediatr Surg Int 31, 551–555 (2015). https://doi.org/10.1007/s00383-015-3701-4
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00383-015-3701-4