Abstract
Background
Traumatic atlanto-occipital dislocation is an uncommon, severely unstable pathology, which can lead to detrimental or even fatal neurological impairment. Specifically, children have consistently been reported to be more susceptible to this type of injury because of their disproportionately larger head, ligament laxity, and injury mechanisms. However, to date, rates of missed injury and outcomes including neurologic recovery of pediatric and adult populations following this insult have not been comparatively evaluated.
Methods
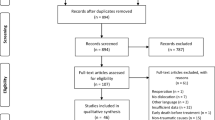
Standard search engines were used to investigate outcomes of traumatic atlanto-occipital dislocation in children and adolescents compared to adults.
Conclusions
Based on case reports and small series from the literature, it seems that children and adolescents tend to have a better likelihood of survival with the possibility of long-term neurological complications. Comparatively, adults who suffer traumatic atlanto-occipital dislocation either succumb to their injuries or survive with very little if any neurological complications.
Similar content being viewed by others
References
Blackwood NJ (1908) Atlanto-occipital dislocation. A case of fracture of the atlas and axis and forward dislocation of the occiput on the spinal column, life being maintained for thirty-four hours and forty minutes by artificial respiration during which a laminectomy was performed upon the third cervical vertebra. Ann Surg 47:654–658
Hall G, Kinsman M, Nazar R, Hruska T, et al. (2015) Atlanto-occipital dislocation. World J Orthod 6:236–243
Martinez-Lage J, Alarcón F, Alfaro R, et al. (2013) Severe spinal cord injury in craniocervical dislocation: case based update. Childs Nerv Syst 29:187–194
Jeszenszky D, Fekete T, Lattig F, Bognár L (2010) Intraarticular atlantooccipital fusion for the treatment of traumatic occipitocervical dislocation in a child. Spine 35:E421–E426
Horn E, Feiz-Erfan I, Lekovic G, et al. (2007) Survivors of occipitoatlantal dislocation injuries: imaging and clinical correlates. J Neurosurg Spine 6:113–120
McElwee K, Wargo C (2006) Traumatic atlanto-occipital dislocation: a pediatric case report. J Transcult Nurs 13:186–189
Hosalkar H, Cain E, Horn D, et al. (2005) Traumatic atlanto-occipital dislocation in children. J Bone Joint Surg 87:2480–2488
Houle P, McDonnell D, Vender J (2001) Traumatic atlanto-occipital dislocation in children. Pediatr Neurosurg 34:193–197
Astur N, Klimo P Jr, Sawyer J, et al. (2013) Traumatic atlanto-occipital dislocation in children: evaluation, treatment and outcomes. J Bone Joint Surg 95(e194):1–8
Astur N, Sawyer J, Klimo P Jr, et al. (2014) Traumatic atlanto-occipital dislocation in children. J Am Acad Orthop Surg 22:274–282
Steinmetz M, Lechner R, Anderson J (2003) Atlantooccipital dislocation in children: presentation, diagnosis, and management. Neurosurg Focus 14:1–7
Kriss V (1999) Down syndrome: imaging of multiorgan involvement. Clin Pediatr 38:441–449
Dimaio D, DiMaio V (2001) Forensic pathology. CRC Press, Boca Raton, pp. 179–181
Avellino AM, Mann FA, Grady MS, Chapman JR, Ellenbogen RG, Alden TD, Mirza SK (2005) The misdiagnosis of acute cervical spine injuries and fractures in infants and children: the 12-year experience of a level I pediatric and adult trauma center. Childs Nerv Syst 21(2):122–127
Ghatan S, Newell DW, Grady MS, Mirza SK, Chapman JR, Mann FA, Ellenbogen RG (2004) Severe posttraumatic craniocervical instability in the very young patient. Report of three cases. J Neurosurg 101(1 Suppl):102–107
Bellabarba C, Mirza SK, West GA, Mann FA, Dailey AT, Newell DW, Chapman JR (2006) Diagnosis and treatment of craniocervical dislocation in a series of 17 consecutive survivors during an 8-year period. J Neurosurg Spine 4(6):429–440
Vaccaro A, Fehlings M, Dvorak M (2011) Essentials of spinal cord injury: basic research to clinical practice. Thieme Medeical Publishers, Inc, New York
Eck J, DiPaola C (2014) Essentials of spinal disorders. JP Medical LTD, London, pp. 70–71
Reed C, Campbell S, Beall D, Bui J, Stefko R (2005) Atlanto-occipital dislocation with traumatic pseudomeningocele formation and post-traumatic syringomyelia. Spine 30:E128–E133
Carvalho M, Swash M (2014) Neurologic complications of craniovertebral dislocation. Handb Clin Neurol 119:435–448
Aoyama M, Yasuda M, Joko M, Takeuchi M, Niwa A, Takayasu M (2015) Pitfalls in the management of atlanto-occipital dislocation. Asian Spine J 9:465–470
Bransford R, Alton T, Patel A, Bellabarba C (2014) Upper cervical spine trauma. J Am Acad Orthop Surg 22:718–729
Sun P, Poffenbarger G, Durham S, Zimmerman R (2000) Spectrum of occipitoatlantoaxial injury in young children. J Neurosurg Spine 93:28–39
Donahue D, Muhlbauer M, Kaufman R, Warner W, Sanford R (1994) Childhood survival of atlantooccipital dislocation: underdiagnosis, recognition, treatment and review of the literature. Pediatr Neurosurg 21:105–111
Pang D (2012) Treating atlantooccipital dislocation in very young children and infants: solving the Archimedean spiral. World Neurosurg 78:614–616
Joaquim A, Ghizoni E, Tedeschi H, Lawrence B, et al. (2014) Upper cervical injuries—a rational approach to guide surgical management. J Spinal Cord Med 37:139–151
Singh B, Cree A (2015) Laminar screw fixation of the axis in the pediatric population: a series of eight patients. Spine J 15:E17–E25
Gire J, Roberto R, Bobinski M, Klineberg E, Durbin-Johnson B (2013) The utility and accuracy of computed tomography in the diagnosis of occipitocervical dissocation. The Spine J 13:510–519
Ben-Galim P, Sibai T, Hipp J, Heggeness M, Reitman C (2008) Internal decapitation: survival after head to neck dissociation injuries. Spine 33:1774–1749
Ehlinger M, Charles Y, Adam P, et al. (2011) Survivor of a traumatic atlanto-occipital dislocation. J Orthop Trauma 97:335–340
Grabb B, Frye T, Hedlund G, et al. (1999) MRI diagnosis of suspected atlanto-occipital dissociation in childhood. Pediatr Radiol 29:275–281
Kaufman R, Dunbar J, Botsford J, McLaurin R (1982) Traumatic longitudinal atlanto-occipital distraction injuries in children. AJNR Am J Neuroradiol 3:415–419
Kalani M, Ratliff J (2013) Considering the diagnosis of occipitocervical dissociation. Spine J 13:520–522
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors have no conflict of interest.
Rights and permissions
About this article
Cite this article
Tubbs, R.S., Patel, C., Loukas, M. et al. Traumatic atlanto-occipital dislocation: do children and adolescents have better or worse outcomes than adults? A narrative review. Childs Nerv Syst 32, 1387–1392 (2016). https://doi.org/10.1007/s00381-016-3118-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00381-016-3118-y