Abstract
Purpose
The cause of external hydrocephalus in infants is largely unknown. However, familial macrocephaly and delayed maturation of the arachnoid granulations are thought to play a part in the idiopathic cases. Secondary cases of external hydrocephalus are associated with hemorrhage, meningitis, and elevated venous pressure. Recently, elevated venous pressure has been shown to be a much more common cause of communicating hydrocephalus in children than previously thought. The purpose of this study is to investigate venous pressure as a cause of external hydrocephalus.
Methods
Six children with external hydrocephalus underwent an MRI examination including MR venography and MR flow quantification techniques. A chart review was performed to correlate the clinical findings with the MR findings. Six children with normal head circumferences and growth profile served as controls.
Results
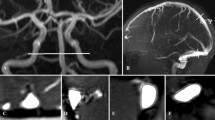
The net aqueduct flow in both normal and hydrocephalic children was into the ventricles. There was a spectrum of blood flow findings in the infants with hydrocephalus. (1) Those with normal arterial inflow showed venous outflow stenoses or anomalies. (2) Those with normal MR venograms tended to have elevated cerebral blood inflow.
Conclusions
The absorption of CSF in infants is into the capillary bed of the deep white matter rather than the arachnoid granulations. Absorption into a capillary bed depends on hydrostatic pressure. Similar to older children with communicating hydrocephalus, the infants in this cohort with external hydrocephalus showed evidence of an elevation in venous pressure. Elevated venous pressure may be a much more common cause of external hydrocephalus than previously recognized.






Similar content being viewed by others
References
Alvarez LA, Maytal J, Shinar S (1986) Idiopathic external hydrocephalus: natural history and relationship to benign familial macrocephaly. Pediatrics 77:901–907
Andersson H, Elfverson J, Svendsen P (1984) External hydrocephalus in infants. Childs Brain 11:398–402
Ayanzen RH, Bird CR, Keller PJ, McCully FJ, Theobald MR, Heiserman JE (2000) Cerebral venography: normal anatomy and potential diagnostic pitfalls. AJNR Am J Neuroradiol 21:74–78
Baledent O, Gondry-Jouet C, Meyer ME, De Marco G, Le Gars D, Henry-Feugeas MC, Idy-Peretti I (2004) Relationship between cerebrospinal fluid and blood dynamics in healthy volunteers and patients with communicating hydrocephalus. Invest Radiol 39:45–55
Barlow CF (1984) CSF dynamics in hydrocephalus—with special attention to external hydrocephalus. Brain Dev 6:119–127
Bateman GA (2002) Vascular hydraulics associated with idiopathic and secondary intracranial hypertension. AJNR Am J Neuroradiol 23:1180–1186
Bateman GA (2006) Association between arterial inflow and venous outflow in idiopathic and secondary intracranial hypertension. J Clin Neurosci 13:550–556
Bateman GA (2008) Arterial inflow and venous outflow in idiopathic intracranial hypertension associated with venous outflow stenoses. J Clin Neurosci 15:402–408
Bateman GA (2010) Hyperemic hydrocephalus: a new form of childhood hydrocephalus analogous to hyperemic intracranial hypertension in adults. J Neurosurg Pediatrics 5:20–26
Bateman GA, Smith RL, Siddique SH (2007) Idiopathic hydrocephalus in children and idiopathic intracranial hypertension in adults: two manifestations of the same pathophysiological process? J Neurosurg 107(6 Suppl):439–444
Blomquist HK, Sundin S, Ekstedt J (1986) Cerebrospinal fluid hydrodynamic studies in children. J Neurol Neurosurg Psychiatry 49:536–548
Bradley WG, Safar FG, Hurtado C, Ord J, Alksne JF (2004) Increased intracranial volume: a clue to the etiology of idiopathic normal-pressure hydrocephalus? AJNR Am J Neuroradiol 25:1479–1484
Carolan PL, McLaurin RL, Towbon RB, Egelhoff JC (1985–1986) Benign extra-axial collections of infancy. Pediatr Neurosci 12:140–144
Chiron C, Raynaud C, Maziere B, Zilbovicius M, Laflamme L, Masure MC, Dulac O, Bouguignon M, Syrota A (1992) Changes in regional cerebral blood flow during brain maturation in children and adolescents. J Nucl Med 33:696–703
Dekaban AS (1978) Changes in brain weights during the span of human life: relation of brain weights to body heights and body weights. Ann Neurol 4:345–356
DiChiro G (1964) Movement of cerebrospinal fluid in human beings. Nature 204:290–291
Hellbush LC (2007) Benign extracerebral fluid collections in infancy: clinical presentation and long-term follow-up. J Neurosurg (2 Suppl Pediatrics) 107:119–125
Hirabuki N, Watanabe Y, Mano T, Fujita N, Tanaka H, Ueguchi T, Nakamura H (2000) Quantitation of flow in the superior sagittal sinus performed with cine phase-contrast MR imaging of healthy and achondroplastic children. AJNR Am J Neuroradiol 21:1497–1501
James AE, De Land RH, Hodgers FJ, Wagner HN (1970) Cerebrospinal fluid (CSF) scanning: cisternography. Am J Roentgenol 110:74–87
Kapila A, Trice J, Spies WG, Seigel BA, Gado MH (1982) Enlarged cerebrospinal fluid spaces in infants with subdural hematomas. Radiology 142:669–672
Karmazyn B, Dagan O, Vidne BA, Horev G, Kornreich L (2002) Neuroimaging findings in neonates and infants from superior vena cava obstruction after cardiac operation. Pediatr Radiol 32:806–810
Kendall B, Holland I (1981) Benign communicating hydrocephalus in children. Neuroradiology 21:93–96
Kim DS, Choi JU, Huh R, Yun PH, Kim DI (1999) Quantitative assessment of cerebrospinal fluid hydrodynamics using a phase-contrast cine MR image in hydrocephalus. Child Nerv Syst 15:461–467
Kimelberg HK (2004) Water homeostasis in the brain: basic concepts. Neuroscience 129:851–860
Kokubo Y, Maki Y (1976) Some characteristic features of RI-cisternography in infancy and childhood. No Shinkei Geka 4:155–162
Leliefeld PH, Gooskens RHJM, Tulleken CAF, Regli L, Uiterwaal CSPM, Han KS, Kappelle LJ (2010) Noninvasive detection of the distinction between progressive and compensated hydrocephalus in infants: is it possible? J Neurosurg Pediatrics 5:562–568
Maki Y, Kokubo Y, Nose T, Yoshii Y (1976) Some characteristic findings of isotope cisternograms in children. J Neurosurg 45:56–59
Maytal J, Alvarez LA, Elkin CM, Shinnar S (1987) External hydrocephalus: radiologic spectrum and differentiation from cerebral atrophy. AJR Am J Roentgenol 148:1223–1230
Ment LR, Duncan CC, Geehr R (1981) Benign enlargement of subarachnoid space in the infant. J Neurosurg 54:504–508
Mori K, Handa H, Itoh M, Okuno T (1980) Benign subdural effusion in infants. J Comput Assist Tomogr 4:466–471
Oi S, Di Rocco C (2006) Proposal of “evolution theory in cerebrospinal fluid dynamics” and minor pathway hydrocephalus in developing immature brain. Childs Nerv Syst 22:662–669
Penn RD, Basati S, Sweetman B, Guo X, Linninger A (2001) Ventricle wall movements and cerebrospinal fluid flow in hydrocephalus. J Neurosurg. doi:10.3171/2010.12.JNS10926
Pettit RE, Kilroy AW, Allen JH (1980) Macrocephaly with head growth parallel to normal growth pattern: neurological, developmental, and computerized tomography findings in full-term infants. Arch Neurol 35:518–521
Portnoy HD, Croissant PD (1978) Megalencephaly in infants and children. The possible role if increased dural sinus pressure. Arch Neurol 35:306–316
Ravid S, Maytal J (2003) External hydrocephalus: a probable cause for subdural hematoma in infancy. Pediatr Neurol 28:139–141
Rollins N, Booth T, Shapiro K (2000) MR venography in children with complex craniostenosis. Pediatr Neurosurg 32:308–315
Rollins N, Ison C, Booth T, Chia J (2005) MR venography in the pediatric patient. AJNR Am J Neuroradiol 26:50–55
Sahar A (1978) Pseudohydrocephalus-megalocephaly, increased intracranial pressure and widened subarachnoid space. Neuropadiatrie 9:131–139
Turner L (1961) The structure of arachnoid granulations with observations on their physiology and pathophysiological significance. Ann R Coll Surg Engl 29:237–264
Conflicts of interest
We declare that we have no conflict of interest.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Bateman, G.A., Napier, B.D. External hydrocephalus in infants: six cases with MR venogram and flow quantification correlation. Childs Nerv Syst 27, 2087–2096 (2011). https://doi.org/10.1007/s00381-011-1549-z
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00381-011-1549-z