Abstract
Purpose
This study describes the epidemiological patterns of hydrocephalus in toddlers in our setting in order to determine the proportion of those who could benefit from endoscopic third ventriculostomy (ETV).
Methods
This prospective and descriptive study included all toddlers operated on for hydrocephalus from 1 March 2008 to 31 March 2010 at the Yaounde Central Hospital.
Results
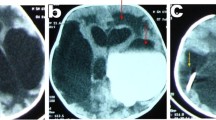
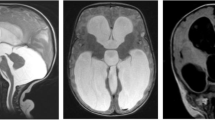
Forty-six toddlers were included representing 72% of all hydrocephalus cases managed at the Neurosurgery Unit during the study period. The mean age was 6.9 ± 1.6 months. The delay before treatment varied from 5 days to 15.8 months (mean = 3.7 ± 0.5 months). The commonest clinical presentation was macrocrania (78.3%). Of the toddlers, 58.7% presented with a probable blindness (loss of ocular pursuit); dilated and non-reactive pupils were found in nine patients (19.6%). The diagnosis was based on transfontanellar echography (TFE), CT scan or combined TFE and CT scan. Identified aetiologies were aqueduct stenosis (28.7%), haemorrhage (18%), Dandy–Walker’s syndrome (14.3%), meningitis (10.8%), myelomeningocele (10.8%), agenesis of Monro’s foramen (3.6%), brain abscess (3.2%) and posterior fossa tumour (3.6%). No specific cause was found in 7% of cases. The treatment was ventriculoperitoneal shunting in 42 cases (91.3%) and ETV in two cases (4.3%). Infections (11.1%) and shunts’ obstruction (5.4%) were the main complications.
Conclusion
Cases of hydrocephalus in toddlers are frequent in our setting. Regardless of the patient’s age, the most prevailing aetiologies (infections, haemorrhage, myelomeningocele) and technological conditions (neuroendoscope) are less favourable for ETV. The use of ETV in the treatment of hydrocephalus in sub-Saharan Africa is still marginal and needs to be encouraged in selected cases. The prevention of non-tumoral hydrocephalus is of critical importance.

Similar content being viewed by others
References
Abena OMT, Dongmo L, Kagmeni G, Gaggini J, Camara M, Mbede J (1994) L’hydrocéphalie en milieu pédiatrique a Yaoundé, Cameroun: étude de 69 cas. Ann Pediatr 41(7):249–252
Adeloye A (2001) Management of infantile hydrocephalus in Central Africa. Trop Doctor 31:67–70
Barlow P, Ching HS (1997) An economic argument in favour of endoscopic third ventriculostomy as a treatment for obstructive hydrocephalus. Minim Invasive Neurosurg 40:37–39
Beems T, Grotenhuis JA (2002) Is the success rate of endoscopic third ventriculostomy age-dependent? An analysis of the results of endoscopic third ventriculostomy in young children. Childs Nerv Syst 18:605–608
Buxton N, Macarthur D, Mallucci C, Punt J, Vloeberghs M (1998) Neuroendoscopic third ventriculostomy in patients less than 1 year old. Pediatr Neurosurg 29:73–76
Cinalli G, Sainte-Rose C, Chumas P, Zerah M, Brunelle F, Lot G et al (1999) Failure of third ventriculostomy in the treatment of aqueductal stenosis in children. J Neurosurg 90:448–454
Djientcheu VP, Njamnshi AK, Wonkam A, Njiki J, Guemse M, Mbu R et al (2008) Neural tube defects in a Sub-Saharan country: the situation in Yaounde, Cameroun. J Neurol Sci 275:29–32
Djientcheu VP, Wonkam A, Njamnshi AK, Ongolo-Zogo P, Kobela M, Rillet B, Morris M (2006) Discordant encephalocele in monozygotic twins. Am J Med Genet 140:526–527
Djientcheu VP, Zona G, Rilliet B (2000) Neurocysticercosis: migration and proliferation of cysticercus in a CSF valve. Br J Neurosurg 14(2):135–137
Djientcheu VP, Zoung-Kanyi BAC, Njamnshi AK (2009) Neural tube defects in the African child: a commentary. J Neurol Sci 280(1–2):131–132
Fukuhara T, Vorster SJ, Luciano MG (2000) Risk factors for failure of endoscopic third ventriculostomy for obstructive hydrocephalus. Neurosurg 46:1100–1111
Garton HJ, Kestle JR, Cochrane DD, Steinbok P (2002) A cost-effective analysis of endoscopic third ventriculostomy. Neurosurg 51:69–78
Gonsu FJ, Kago I, Dzogang MT, Kamga HG, Camara M (1990) Cerebral complications of purulent meningitis in children assessed by transfontanellar ultrasonography in Yaounde (Cameroon). Ann Radiol 33(3):195–199
Goumnerova LC, Frim DM (1997) Treatment of hydrocephalus with third ventriculocisternostomy: outcome and CSF flow patterns. Pediatr Neurosurg 27:149–152
Hopf NJ, Grunert P, Fries G, Resch KDM, Perneczky A (1999) Endoscopic third ventriculostomy: outcome analysis of 100 consecutive procedures. Neurosurg 44:795–806
Javadpour M, Mallucci C, Brodbelt A, Golash A, May P (2001) The impact of endoscopic third ventriculostomy on the management of newly diagnosed hydrocephalus in infants. Pediatr Neurosurg 35:131–135
Kéïta AD, Sidibé M, Kéïta T, Kéïta MM, Sidibé T, Traoré I (1996) Apport de l’échographie dans le diagnostic de l’hydrocéphalie chez le nourrisson: à propos de 55 cas. Mali Médical 11:10–13
Mohanty A, Vasudev MK, Sampath S, Radhesh S, Sastry Kolluri VR (2002) Failed endoscopic third ventriculostomy in children: management options. Pediatr Neurosurg 37:304–309
Njamnshi AK, Djientcheu VP, Lekoubou A, Guemse M, Obama MT, Mbu R et al (2008) Neural tube defects are rare among black Americans but not in Sub-Saharan black Africans: the case of Yaounde-Cameroon. J Neurol Sci 270:13–17
Nko’o AS, Koki NP, Beyeme OM, Abena OMT (1990) Incidence of cerebral hemorrhage in newborn infants diagnosed by echography in Yaoundé, Cameroon. Pediatr 45(10):721–724
Prusseit J, Simon M, von der Brelie C, Heep A, Molitor E, Volz S, Simon A (2009) Epidemiology, prevention and management of ventriculoperitoneal shunt infections in children. Pediatr Neurosurg 45(5):325–336
Rajshekhar V (2009) Management of hydrocephalus in patients with tuberculous meningitis. Neurol India 57(4):368–374
Sanoussi S (2001) Les malformations du tube neural au Niger. A propos de 387 cas en 10 ans. Plaidoyer pour un traitement par l’acide folique en période péri-conceptionnelle. Med Afr Noire 48:509–515
Shako D et al (1978) Troubles hydrodynamiques du liquide céphalo-rachidien aux C.U de Kinshasa. Afr Med 17:711–716
Teo C, Jones R (1996) Management of hydrocephalus by endoscopic third ventriculostomy in patients with myelomeningocele. Pediatr Neurosurg 25:57–63
Veyrac C, Couture A, Saguintaah M, Baud C (2001) L’échographie cérébrale en l’an 2001. Le point sur l’exploration d’une macrocrânie du nourrisson. J Radiol 82(6):717–725
Warf BC (2005) Hydrocephalus in Uganda: the predominance of infectious origin and primary management with endoscopic third ventriculostomy. J Neurosurg Paediatr 102:1–15
Warf BC, Mugamba J, Kulkarni AV (2010) Endoscopic third ventriculostomy in the treatment of childhood hydrocephalus in Uganda: report of a scoring system that predicts success. J Neurosurg Paediatr 5(2):143–148
Wellons JC, Shannon CN, Kulkarni AV, Simon TD, Riva-Cambrin J, Whitehead WE, Oakes WJ, Drake JM, Luerssen TG, Walker ML, Kestle JR (2009) A multicenter retrospective comparison of conversion from temporary to permanent cerebrospinal fluid diversion in very low birth weight infants with posthemorrhagic hydrocephalus. J Neurosurg Pediatr 4(1):50–55
Acknowledgement
We are grateful to all the staff that contributed to the realization of the present study. We also thank all parents who gave their consent for their children to take part in this study. This study was approved by the Cameroon National Ethical Committee.
Declaration of interest
This study received no specific grant from any funding agency in the public, commercial or not-for-profit sectors. No conflict of interest was reported by the authors.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Djientcheu, V., Nguefack, S., Mouafo, T.O. et al. Hydrocephalus in toddlers: the place of shunts in sub-Sahara African countries. Childs Nerv Syst 27, 2097–2100 (2011). https://doi.org/10.1007/s00381-011-1548-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00381-011-1548-0