Abstract
Background
During spring-assisted cranioplasty, the spring transmits forces through adjacent cranium. We have previously demonstrated that the ectocranial–endocranial thickness of cranial sutures increases significantly over time in the presence of continuous spring forces. We wished to investigate if cranial bone showed similar adaptational responses.
Methods
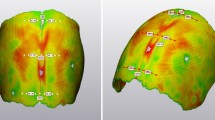
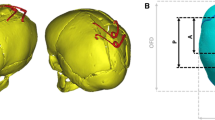
New Zealand white rabbits were randomized into a treatment group [a spring was placed across a posterior frontal suture (PFS) suturectomy and a control group (PFS suturectomy)]. Animals (n = 6) were euthanized from each group at 4, 7, and 10 weeks, respectively. A sham group (n = 6) was euthanized at 10 weeks. Frontal bone thickness was recorded at five reproducible anatomical points on the frontal bone. Histological analysis of the bone architecture was performed.
Results
Frontal bone thickness was significantly greater than controls at all five sites at weeks 7 and 10. There were multiple significant differences between the 4-, 7-, and 10-week groups with each site progressively thickening over time. Histological analysis revealed a uniform increase in thickness of the endocranial and ectocranial cortical bone in the treatment groups.
Conclusions
Cranial bone adapts to the presence of continuous spring cranioplasty forces by progressively thickening over time. This property is beneficial in craniosynostosis cases with very thin and poor quality bone and may partly explain the observed lack of spring erosion through bone.





Similar content being viewed by others
References
Lauritzen C, Davis C, Ivarsson A, Hewitt T (2008) The evolving role of springs in craniofacial surgery: the first 100 clinical cases. Plast Reconstr Surg 121:545–554
Guimaraes-Ferreira J, Gewalli G, David L, Olsson R, Friede H, Lauritzen C (2003) Spring mediated cranioplasty compared with the modified pi-plasty for sagittal synostosis. Scand J Plast Reconstr Surg Hand Surg 37:208–215
Windh P, Davis C, Sanger C, Sahlin P, Lauritzen (2008) Spring-assisted cranioplasty vs pi-plasty for sagittal synostosis—a long-term follow-up study. J Craniofac Surg 19:59–64
Mackenzie K, Davis C, Yang A, MacFarlane M (2009) Evolution of the treatment of sagittal synostosis: the role of new technologies. J Craniofac Surg 20:129–133
Davis C, Wickremesekera A, MacFarlane MR (2009) Correction of nonsynostotic scaphocephaly without cranial osteotomy: spring expansion of the sagittal suture. Childs Nerv Syst 25:225–230
David LR, Proffer P, Hurst WJ, Glazier S, Argenta LC (2004) Spring-mediated cranial reshaping for craniosynostosis. J Craniofac Surg 15:810–816
Davis C, Windh P, Lauritzen C (2009) Spring-assisted cranioplasty alters the growth vectors of adjacent cranial sutures. Plast Reconstr Surg 129:470–474
Coats B, Margulies SS (2006) Material properties of human infant skull and suture at high rates. J Neurotrauma 23:1222–1232
Davis C, Lauritzen C (2009) Frontobasal suture distraction corrects hypotelorism in metopic synostosis. J Craniofac Surg 20:121–124
Davis C, Windh P, Lauritzen C (2009) Cranial bone and suture strains incident to spring-assisted cranioplasty. Plast Reconstr Surg (in press)
Davis C, Windh P, Lauritzen C (2009) Biomechanical characteristics of cranial sutures are altered by spring cranioplasty forces. Plast Reconstr Surg (in press)
Gewalli F, Guimaraes-Ferreira J, Maltese G, Ortengren U, Lauritzen C (2001) Expander elements in craniofacial surgery: an experimental study in rabbits. Scand J Plast Reconstr Hand Surg 35:149–156
David LR, Gewalli F, Guimaraes-Ferreira J et al (2002) Dynamic spring-mediated cranioplasty in a rabbit model. J Craniofac Surg 13:794–801
Davis C, Windh P, Lauritzen C (2009) Do expansile cranial springs erode through the cranium? J Craniofac Surg 20:168–170
Davis C, Lauritzen CG (2008) Spring-assisted remodeling for ventricular shunt-induced cranial deformity. J Craniofac Surg 19:588–592
Mao JJ, Nah HD (2004) Growth and development: hereditary and mechanical modulations. Am J Dentofacial Orthop 125:676–689
Raab-Cullen DM, Theide MA, Petersen DN et al (1994) Mechanical loading stimulates rapid changes in periosteal gene expression. Calcif Tissue Int 55:473–478
Harter LV, Hruska KA, Duncan RL (1995) Human osteoblast-like cells respond to mechanical strain with increased bone matrix production independent of hormonal regulation. Endo 136:528–535
Rubin CT, Lanyon LE (1984) Regulation of bone formation by applied dynamic loads. J Bone Joint Surg 66A:397–402
Frost HM (1996) Perspectives: a proposed general model of the “mechanostat”. Anat Rec 244:139–147
Alexandridis C, Caputo AA, Thanos CE (1985) Distribution of stresses in the human skull. J Oral Rehabil 12:499–507
Witzel U, Preuschoft H (2002) Function-dependent shape characteristics of the human skull. Anthropol Anz 60:113–135
Ross CF (2001) In vivo function of the craniofacial haft: the interorbital pillar. Am J Phys Anthrop 116:108–139
Rafferty KL, Herring SW, Marshall CD (2003) Biomechanics of the rostrum and the role of facial sutures. J Morphol 257:33–44
Herring SW, Teng S (2000) Strain in the braincase and its sutures during function. Am J Phys Anthropol 112:575–593
Popwics TE, Herring SW (2007) Load transmission in the nasofrontal suture of the pig, Sus scrofa. J Biomech 40:837–844
Iwasaki K (1989) Dynamic responses in adult and infant monkey craniums during occlusion and mastication. J Osaka Dent Univ 23:77–97
Liebermann DE (1996) How and why humans grow thin skulls: Experimental evidence for systemic cortical robusticity. Am J Phys Anthropol 101:217–236
Acknowledgments
We are very grateful to Dr. Bronwen Kelly for her expert assistance with the statistical analysis.
Author information
Authors and Affiliations
Corresponding author
Additional information
Financial disclosure and products
Charles Davis, Per Windh, and Claes Lauritzen, the authors of this manuscript, have no financial interest in the spring technology or techniques used in this paper.
Rights and permissions
About this article
Cite this article
Davis, C., Windh, P. & Lauritzen, C.G.K. Adaptation of the cranium to spring cranioplasty forces. Childs Nerv Syst 26, 367–371 (2010). https://doi.org/10.1007/s00381-009-1026-0
Received:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00381-009-1026-0