Abstract
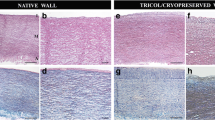
Decellularized porcine aortic valve conduits (AVCs) implanted in a Vietnamese Pig (VP) experimental animal model were matched against decellularized and then cryopreserved AVCs to assess the effect of cryopreservation on graft hemodynamic performance and propensity to in vivo repopulation by host’s cells. VPs (n = 12) underwent right ventricular outflow tract substitution using AVC allografts and were studied for 15-month follow-up. VPs were randomized into two groups, receiving AVCs treated with decellularization alone (D; n = 6) or decellularization/cryopreservation (DC; n = 6), respectively. Serial echocardiography was carried out to follow up hemodynamic function. All explanted AVCs were processed for light and electron microscopy. No signs of dilatation, progressive stenosis, regurgitation, and macroscopic calcification were echocardiographically observed in both D and DC groups. Explanted D grafts exhibited near-normal features, whereas the presence of calcification, inflammatory infiltrates, and disarray of elastic lamellae occurred in some DC grafts. In the unaltered regions of AVCs from both groups, almost complete re-endothelialization was observed for both valve cusps and aorta walls. In addition, side-by-side repopulation by recipient’s fibroblasts, myofibroblasts, and smooth muscle cells was paralleled by ongoing tissue remodeling, as revealed by the ultrastructural identification of typical canals of collagen fibrillogenesis and elastogenesis-related features. Incipient neo-vascularization and re-innervation of medial and adventitial tunicae of grafted aortic walls were also detected for both D and DC groups. Cryopreservation did not affect post-implantation AVC hemodynamic behavior and was topically propensive to cell repopulation and tissue renewal, although graft deterioration including calcification was present in several areas. Thus, these preliminary data provide essential information on feasibility of decellularization and cryopreservation coupling in the perspective of treatment optimization and subsequent clinical trials using similarly treated human allografts as innovative heart valve substitutes.





Similar content being viewed by others
References
Biancari F, Barbanti M, Santarpino G, Deste W, Tamburino C, Gulino S, Immè S, Di Simone E, Todaro D, Pollari F, Fischlein T, Kasama K, Meuris B, Dalén M, Sartipy U, Svenarud P, Lahtinen J, Heikkinen J, Juvonen T, Gatti G, Pappalardo A, Mignosa C, Rubino AS (2016) Immediate outcome after sutureless versus transcatheter aortic valve replacement. Heart Vessels 31:427–433
Jashari R, Goffin Y, Van Hoeck B, Vanderkelen A, du Verger A, Fan Y, Holovska V, Fagu A, Brahy O (2010) Belgian and European experience with the European Homograft Bank (EHB) cryopreserved allograft valves assessment of a 20 year activity. Acta Chir Belg 110(3):280–290
Kobayashi J, Kawashima Y, Matsuda H, Nakano S, Kasugai T, Tokuan Y (1990) Pathological findings of the aortic homograft in a patient with tetralogy of Fallot twenty years after implantation. Heart Vessels 5(2):98–101
Breinholt JP, Hawkins JA, Lambert LM, Fuller TC, Profaizer T, Shaddy R (2000) A prospective analysis of the immunogenicity of cryopreserved non valved allografts used in pediatric heart surgery. Circulation 7 102(19 Suppl 3):III179–III182
Lang SJ, Giordano MS, Cardon-Cardo C, Summers BD, Staiano-Coico L, Hajjar DP (1994) Biochemical and cellular characterization of cardiac valve tissue after cryopreservation or antibiotic preservation. J Thorac Cardiovasc Surg 108:63–67
Gerson CJ, Heacox AE (2009) Retained structural integrity of collagen and elastin within cryopreserved human heart valve tissue as detected by two-photon laser scanning confocal microscopy. Cryobiology 59(2):171–179
Brockbank KG, Lightfoot FG, Song YC, Taylor MJ (2000) Interstitial ice formation in cryopreserved homografts: a possible cause of tissue deterioration and calcification in vivo. J Heart Valve Dis 9:200–206
Schenke-Layland K, Madershahian N, Riemann I, Starcher B, Halbhuber KJ, König K, Stock UA (2006) Impact of cryopreservation on extracellular matrix structures of heart valve leaflets. Ann Thorac Surg 81:918–926
Mitchell RN, Jonas RA, Schoen FJ (1998) Pathology of explanted cryopreserved allograft heart valves: comparison with aortic valves from orthotopic heart transplants. J Thorac Cardiovasc Surg 115:118–127
Ortolani F, Bonetti A, Tubaro F, Petrelli L, Contin M, Nori SL, Spina M, Marchini M (2007) Ultrastructural characterization of calcification onset and progression in subdermally implanted aortic valves. Histochemical and spectrometric data. Histol Histopathol 22(3):261–272
Bonetti A, Della Mora A, Contin M, Tubaro F, Marchini M, Ortolani F (2012) Ultrastructural and spectrophotometric study on the effects of putative triggers on aortic valve interstitial cells in vitro models simulating metastatic calcification. Anat Rec Hoboken 295(7):1117–1127
Affonso da Costa FD, Dohmen PM, Lopes SV, Lacerda G, Pohl F, Vilani R, Affonso Da Costa MB, Vieira ED, Yoschi S, Konertz W, Affonso da Costa I (2004) Comparison of cryopreserved homografts and decellularized porcine heterografts implanted in sheep. Artif Organs 28:366–370
Quinn RW, Hilbert SL, Bert AA, Drake BW, Bustamante JA, Fenton JE, Moriarty SJ, Neighbors SL, Lofland GK, Hopkins RA (2011) Performance and morphology of decellularized pulmonary valves implanted in juvenile sheep. Ann Thorac Surg 92(1):131–137
Verbrugghe P, Meuris B, Flameng W, Herijgers P (2009) Reconstruction of atrioventricular valves with photo-oxidized bovine pericardium. Interact Cardiovasc Thorac Surg 9(5):775–779
Spina M, Ortolani F, ElMesslemani A, Gandaglia A, Bujan J, Garcia-Honduvilla N, Vesely I, Gerosa G, Casarotto D, Petrelli L, Marchini M (2003) Isolation of intact aortic valve scaffolds for heart-valve bioprostheses: extracellular matrix structure, prevention from calcification, and cell repopulation features. J Biomed Mater Res A 67(4):1338–1350
Iop L, Renier V, Naso F, Piccoli M, Bonetti A, Gandaglia A, Pozzobon M, Paolin A, Ortolani F, Marchini M, Spina M, De Coppi P, Sartore S, Gerosa G (2009) The influence of heart valve leaflet matrix characteristics on the interaction between human mesenchymal stem cells and decellularized scaffolds. Biomaterials 30:4104–4116
Bottio T, Tarzia V, Dal Lin C, Buratto E, Rizzoli G, Spina M, Gandaglia A, Naso F, Gerosa G (2010) The changing hydrodynamic performance of the decellularized intact porcine aortic root: considerations on in vitro testing. J Heart Valve Dis 19:485–491
Naso F, Gandaglia A, Iop L, Spina M, Gerosa G (2011) First quantitative assay of alpha-Gal in soft tissues: presence and distribution of the epitope before and after cell removal from xenogeneic heart valves. Acta Biomater 7:1728–1734
Gallo M, Naso F, Poser H, Rossi A, Franci P, Bianco R, Micciolo M, Zanella F, Cucchini U, Aresu L, Buratto E, Busetto R, Spina M, Gandaglia A, Gerosa G (2012) Physiological performance of a detergent decellularized heart valve implanted for 15 months in Vietnamese pigs: surgical procedure, follow-up, and explant inspection. Artif Organs 36(6):E138–E150
Iop L, Bonetti A, Naso F, Rizzo S, Cagnin S, Bianco R, Dal Lin C, Martini P, Poser H, Franci P, Lanfranchi G, Busetto R, Spina M, Basso C, Marchini M, Gandaglia A, Ortolani F, Gerosa G (2014) Decellularized allogeneic heart valves demonstrate self-regeneration potential after a long-term preclinical evaluation. PLoS One 9(6):e99593
Gallo M, Bianco R, Bottio T, Naso F, Franci P, Zanella F, Perona G, Busetto R, Spina M, Gandaglia A, Gerosa G (2013) Tissue-engineered heart valves: intra-operative protocol. J Cardiovasc Transl Res 6(4):660–661
Rossi A, Faggiano P, Amado AE, Cicoira M, Bonapace S, Franceschini L, Dini FL, Ghio S, Agricola E, Temporelli PL, Vassanelli C (2014) Mitral and aortic valve sclerosis/calcification and carotid atherosclerosis: results from 1065 patients. Heart Vessels 29(6):776–783
Brunner E, Langer F (2000) Nonparametric analysis of ordered categorical data in designs with longitudinal observations and small sample sizes. Biom J 42(6):663–675
Theodoridis K, Tudorache I, Calistru A, Cebotari S, Meyer T, Sarikouch S, Bara C, Brehm R, Haverich A, Hilfiker A (2015) Successful matrix guided tissue regeneration of decellularized pulmonary heart valve allografts in elderly sheep. Biomaterials 52:221–228
Baraki H, Tudorache I, Braun M, Hffler K, Grler A, Lichtenberg A, Bara C, Calistru A, Brandes G, Hewicker-Trautwein M, Hilfiker A, Haverich A, Cebotari S (2009) Orthotopic replacement of the aortic valve with decellularized allograft in a sheep model. Biomaterials 30(31):6240–6246
Hopkins RA, Jones AL, Wolfinbarger L, Moore MA, Bert A, Lofland GK (2009) Decellularization reduces calcification while improving both durability and 1-year functional results of pulmonary homograft valves in juvenile sheep. J Thorac Cardiovasc Surg 137(4):907–913
Vincentelli A, Wautot F, Juthier F, Fouquet O, Corseaux D, Marechaux S, Le Tourneau T, Fabre O, Susen S, Van Belle E, Mouquet F, Decoene C, Prat A, Jude B (2007) In vivo autologous recellularization of a tissue-engineered heart valve: are bone marrow mesenchymal stem cells the best candidates? J Thorac Cardiovasc Surg 134(2):424–432
Kasimir M, Weigel G, Sharma J, Rieder E, Seebacher G, Wolner E, Simon P (2005) The decellularized porcine heart valve matrix in tissue engineering: platelet adhesion and activation. Thromb Haemost 94(3):562–567
Rieder E, Seebacher G, Kasimir M, Eva Eichmair, Winter B, Dekan B, Wolner E, Simon P, Weigel G (2005) Tissue engineering of heart valves: decellularized porcine and human valve scaffolds differ importantly in residual potential to attract monocytic cells. Circulation 111(21):2792–2797
Cebotari S, Lichtenberg A, Tudorache I, Hilfiker A, Mertsching H, Leyh R, Breymann T, Kallenbach K, Maniuc L, Batrinac A, Repin O, Maliga O, Ciubotaru A, Haverich A (2006) Clinical application of tissue engineered human heart valves using autologous progenitor cells. Circulation 114(1 Suppl):I132–I137
Huang SD, Liu XH, Bai CG, Lu FL, Yuan Y, Gong DJ, Xu ZY (2007) Synergistic effect of fibronectin and hepatocyte growth factor on stable cell-matrix adhesion, re-endothelialization, and reconstitution in developing tissue-engineered heart valves. Heart Vessels 22(2):116–122
Bechtel JF, Gellissen J, Erasmi AW, Petersen M, Hiob A, Stierle U, Sievers HH (2005) Mid-term findings on echocardiography and computed tomography after RVOT-reconstruction: comparison of decellularized (SynerGraft) and conventional allografts. Eur J Cardiothorac Surg 27(3):410–415
Heng WL, Albrecht H, Chiappini P, Lim YP, Manning L (2013) International heart valve bank survey: a review of processing practices and activity outcomes. J Transplant 2013:163150
Cebotari S, Tudorache I, Ciubotaru A, Boethig D, Sarikouch S, Goerler A, Lichtenberg A, Cheptanaru E, Barnaciuc S, Cazacu A, Maliga O, Repin O, Maniuc L, Breymann T, Haverich A (2011) Use of fresh decellularized allografts for pulmonary valve replacement may reduce the reoperation rate in children and young adults: early report. Circulation 13 124(11 Suppl):S115–S123
Lisy M, Pennecke J, Brockbank KG, Fritze O, Schleicher M, Schenke-Layland K, Kaulitz R, Riemann I, Weber CN, Braun J, Mueller KE, Fend F, ScheunertT Gruber AD, Albes JM, Huber AJ, Stock UA (2010) The performance of ice-free cryopreserved heart valve allografts in an orthotopic pulmonary sheep model. Biomaterials 31(20):5306–5311
Narine K, Ing EC, Cornelissen M, Desomer F, Beele H, Vanlangenhove L, Smet SD, Nooten GV (2006) Readily available porcine aortic valve matrices for use in tissue valve engineering. Is cryopreservation an option? Cryobiology 53(2):169–181
Brockbank KG, Wright GJ, Yao H, Greene ED, Chen ZZ, Schenke-Layland K (2011) Allogeneic heart valve storage above the glass transition at −80°C. Ann Thorac Surg 91(6):1829–1835
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Funding
This study was funded by the RSF 286/08 Regione Veneto Grant and Azione Biotech III.
Conflict of interest
The authors do not have any conflicts to disclose. No competing financial interests exist.
Ethical approval
All applicable international, national, and/or institutional guidelines for the care and use of animals were followed.
Additional information
M. Gallo and A. Bonetti contributed equally to this work.
F. Ortolani, L. Iop and G. Gerosa are equally responsible for the concept and design of the study.
Rights and permissions
About this article
Cite this article
Gallo, M., Bonetti, A., Poser, H. et al. Decellularized aortic conduits: could their cryopreservation affect post-implantation outcomes? A morpho-functional study on porcine homografts. Heart Vessels 31, 1862–1873 (2016). https://doi.org/10.1007/s00380-016-0839-5
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00380-016-0839-5