Abstract
Purpose
So far, few data is available on Methicillin-resistant Staphylococcus aureus (MRSA) infections in urology. To obtain a better insight into MRSA infections, we studied prevalence, colonization and infection site and clinical implications of MRSA in a urological department over a 10-year period.
Methods
A retrospective study of all patients diagnosed with MRSA for the first time over a 10-year period was set-up.
Results
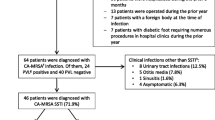
Between 2000 and 2009, a total of 95.161 in- and outpatients were seen at our department. The prevalence of patients with newly diagnosed MRSA was low, that is, <0.1 % per year (mean 0.07%, 0.02–0.1 %). In total, 62 MRSA cases were identified over a 10-year period. MRSA incidence was 10 times higher in inpatients (0.2 %) than in outpatients (0.02 %). Asymptomatic MRSA colonization was present in 25/62 patients (40.3 %), the remaining 59.7 % (37/62) showed clinical symptoms: MRSA positive swabs from open wounds were seen in 10/62 patients (16.1 %). Urinary tract infections were seen in 26/10 patients (41.9 %), while life-threatening MRSA sepsis occurred in one patient only over a decade.
Conclusions
In summary, we observed very low rates of MRSA colonization and infection. Still, complications like delayed wound healing, development of abscess and even sepsis may occur.
Similar content being viewed by others
References
Garibaldi RA, Cushing D, Lerer T (1991) Predictors of intraoperative-acquired surgical wound infections. J Hosp Infect 18:289–298
Antimicrobial resistance surveillance in Europe (2009) Annual report of the European antimicrobial resistance surveillance network (EARS-Net). http://ecdc.europa.eu/en/publications/Publications/1011_SUR_annual_EARS_Net_2009.pdf. Accessed 2009
Magistrat der Stadt Wien (2011) Bezirksporträts - Bezirke 16 bis 23. Statistisches Jahrbuch der Stadt Wien, Austria, pp 312–315
Merkblatt des Bundesministeriums für Gesundheit und Konsumentenschutz (1994) Patient mit MRSA - was tun? http://www.angewandtehygiene.com/gesetze/download/MRSA.pdf. Accessed 1994
Naber KG, Bergman B, Bishop MC et al (2001) Urinary tract infection (UTI) working group of the health care office (HCO) of the European association of urology (EAU). EAU guidelines for the management of urinary and male genital tract infections. Urinary tract infection (UTI) working group of the health care office (HCO) of the European association of urology (EAU). Eur Urol 40:576–588
Dindo D, Demartines N, Clavien PA (2004) Classification of surgical complications: a new proposal with evaluation in a cohort of 6,336 patients and results of a survey. Ann Surg 240:205–213
Coia JE, Duckworth GJ, Edwards DJ et al (2006) Guidelines for the control and prevention of meticillin-resistant Staphylococcus aureus (MRSA) in healthcare facilities. J Hosp Infect 1:1–44
Klein E, Smith DL, Laxminarayan R (2007) Hospitalizations and deaths caused by methicillin-resistant Staphylococcus aureus, United States, 1999–2005. Emerg Infect Dis 13:1840–1846
Cosgrove SE, Qi Y, Kaye KS, Harbarth S, Karchmer AW, Carmeli Y (2005) The impact of methicillin resistance in Staphylococcus aureus bacteremia on patient outcomes: mortality, length of stay, and hospital charges. Infect Control Hosp Epidemiol 26:166–174
Duerden BL (2012) MRSA: why have we got it and can we do anything about it? Eye 26:218–221
Koski ME, DeMarco RT, Brock JW, Pope JC, Adams MC, Thomas JC (2008) Community associated methicillin resistant staphylococcal infections in a pediatric urology practice. J Urol 179:1098–1101
Routh JC, Alt AL, Ashley RA, Kramer SA, Boyce TG (2009) Increasing prevalence and associated risk factors for methicillin resistant Staphylococcus aureus bacteriuria. J Urol 181:1694–1698
Shigemura K, Tanaka K, Okada H, Nakan Y, Kinoshita S, Gotoh A, Arakawa S, Fujisawa M (2005) Pathogen occurrence and antimicrobial susceptibility of urinary tract infection cases during a 20-year period (1983–2002) at a single institution in Japan. Jpn J Infect Dis 58:303–308
Kallen AJ, Mu Y, Bulens S et al (2010) Active bacterial core surveillance (ABCs) MRSA Investigators of the emerging infections program. Health care-associated invasive MRSA infections, 2005–2008. Jama 304:641–648
Thiruchelvam N, Yeoh SL, Keoghane SR (2006) MRSA in urology: a UK hospital experience. Eur Urol 49:896–899
Sista RR, Oda G, Barr J (2004) Methicillin-resistant Staphylococcus aureus infections in ICU patients. Anesthisiol Clin N Am 22:405–435
Ishikawa K, Miyakawa S, Hayakawa S, Hoshinaga K (2004) Epidemical study of methicillin-resistant Staphylococcus aureus isolated from the urology ward in 2003—nosocomial infection and community acquired infection. Kansenshogaku Zasshi 78:853–864
Girou E, Loyeau S, Legrand P, Oppein F, Brun-Buisson C (2002) Efficacy of handrubbing with alcohol based solution versus standard handwashing with antiseptic soap: randomised clinical trial. BMJ 325:325–362
Bhalla A, Pultz NJ, Gries DM et al (2004) Acquisition of nosocomial pathogens on hands after contact with environmental surfaces near hospitalized patients. Infect Control Hosp Epidemiol 25:164–167
Cooper BS, Stone SP, Kibbler CC et al (2004) Isolation measures in the hospital management of methicillin resistant Staphylococcus aureus (MRSA): systematic review of the literature. BMJ 329:329–533
Jones JW, Carter A, Ewings P, O’Boyle PJ (1999) An MRSA outbreak in a urology ward and its association with Nd:YAG coagulation laser treatment of the prostate. J Hosp Infect 41:39–44
Kyoda Y, Takahashi S, Takeyama K, Masumori N, Tsukamoto T (2010) Decrease in incidence of surgical site infections in contemporary series of patients with radical cystectomy. J Infect Chemother 16:118–122
Conflict of interest
There is no conflict of interest.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Heidler, S., Asboth, F., Mert, C. et al. Methicillin-resistant Staphylococcus aureus (MRSA) in an Austrian urological department: 10 years experience covering 95.161 patients. World J Urol 31, 559–563 (2013). https://doi.org/10.1007/s00345-012-0920-3
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00345-012-0920-3