Abstract
Objectives
To evaluate the effects of computer-aided diagnosis (CAD) on inter-reader agreement in Lung Imaging Reporting and Data System (Lung-RADS) categorization.
Methods
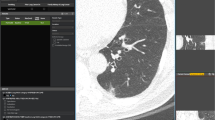
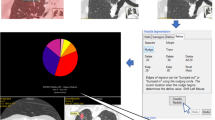
Two hundred baseline CT scans covering all Lung-RADS categories were randomly selected from the National Lung Cancer Screening Trial. Five radiologists independently reviewed the CT scans and assigned Lung-RADS categories without CAD and with CAD. The CAD system presented up to five of the most risk-dominant nodules with measurements and predicted Lung-RADS category. Inter-reader agreement was analyzed using multirater Fleiss κ statistics.
Results
The five readers reported 139–151 negative screening results without CAD and 126–142 with CAD. With CAD, readers tended to upstage (average, 12.3%) rather than downstage Lung-RADS category (average, 4.4%). Inter-reader agreement of five readers for Lung-RADS categorization was moderate (Fleiss kappa, 0.60 [95% confidence interval, 0.57, 0.63]) without CAD, and slightly improved to substantial (Fleiss kappa, 0.65 [95% CI, 0.63, 0.68]) with CAD. The major cause for disagreement was assignment of different risk-dominant nodules in the reading sessions without and with CAD (54.2% [201/371] vs. 63.6% [232/365]). The proportion of disagreement in nodule size measurement was reduced from 5.1% (102/2000) to 3.1% (62/2000) with the use of CAD (p < 0.001). In 31 cancer-positive cases, substantial management discrepancies (category 1/2 vs. 4A/B) between reader pairs decreased with application of CAD (pooled sensitivity, 85.2% vs. 91.6%; p = 0.004).
Conclusions
Application of CAD demonstrated a minor improvement in inter-reader agreement of Lung-RADS category, while showing the potential to reduce measurement variability and substantial management change in cancer-positive cases.
Key Points
• Inter-reader agreement of five readers for Lung-RADS categorization was minimally improved by application of CAD, with a Fleiss kappa value of 0.60 to 0.65.
• The major cause for disagreement was assignment of different risk-dominant nodules in the reading sessions without and with CAD (54.2% vs. 63.6%).
• In 31 cancer-positive cases, substantial management discrepancies between reader pairs, referring to a difference in follow-up interval of at least 9 months (category 1/2 vs. 4A/B), were reduced in half by application of CAD (32/310 to 16/310) (pooled sensitivity, 85.2% vs. 91.6%; p = 0.004).






Similar content being viewed by others
Abbreviations
- ACR:
-
American College of Radiology
- CAD:
-
Computer-aided diagnosis
- CI:
-
Confidence interval
- Lung-RADS:
-
Lung Imaging Reporting and Data System
- NLST:
-
National Lung Screening Trial
References
National Lung Screening Trial Research Team, Aberle DR, Adams AM et al (2011) Reduced lung-cancer mortality with low-dose computed tomographic screening. N Engl J Med 365:395–409
de Koning HJ, van der Aalst CM, de Jong PA et al (2020) Reduced lung-cancer mortality with volume CT screening in a randomized trial. N Engl J Med 382:503–513
Pastorino U, Silva M, Sestini S et al (2019) Prolonged lung cancer screening reduced 10-year mortality in the MILD trial: new confirmation of lung cancer screening efficacy. Ann Oncol 30:1162–1169
American College of Radiology (2014) Lung CT screening reporting and data system (Lung-RADS). Available via https://www.acr.org/Clinical-Resources/Reporting-and-Data-Systems/Lung-Rads
Henschke CI, Yip R, Yankelevitz DF, Smith JP, International Early Lung Cancer Action Program Investigators (2013) Definition of a positive test result in computed tomography screening for lung cancer: a cohort study. Ann Intern Med 158:246–252
McKee BJ, Regis SM, McKee AB, Flacke S, Wald C (2015) Performance of ACR Lung-RADS in a clinical CT lung screening program. J Am Coll Radiol 12:273–276
van Riel SJ, Sánchez CI, Bankier AA et al (2015) Observer variability for classification of pulmonary nodules on low-dose CT images and its effect on nodule management. Radiology 277:863–871
Revel MP, Bissery A, Bienvenu M, Aycard L, Lefort C, Frija G (2004) Are two-dimensional CT Measurements of small noncalcified pulmonary nodules reliable? Radiology 231:453–458
Kim H, Park CM, Woo S et al (2013) Pure and part-solid pulmonary ground-glass nodules: measurement variability of volume and mass in nodules with a solid portion less than or equal to 5 mm. Radiology 269:585–593
Ridge CA, Yildirim A, Boiselle PM et al (2015) Differentiating between subsolid and solid pulmonary nodules at CT: inter- and intraobserver agreement between experienced thoracic radiologists. Radiology 278:888–896
van Riel SJ, Jacobs C, Scholten ET et al (2019) Observer variability for Lung-RADS categorisation of lung cancer screening CTs: impact on patient management. Eur Radiol 29:924–931
Zhao Y, de Bock GH, Vliegenthart R et al (2012) Performance of computer-aided detection of pulmonary nodules in low-dose CT: comparison with double reading by nodule volume. Eur Radiol 22:2076–2084
Liang M, Tang W, Xu DM et al (2016) Low-dose CT screening for lung cancer: computer-aided detection of missed lung cancers. Radiology 281:279–288
Rubin GD, Lyo JK, Paik DS et al (2005) Pulmonary nodules on multi-detector row CT scans: performance comparison of radiologists and computer-aided detection. Radiology 234:274–283
Christe A, Leidolt L, Huber A et al (2013) Lung cancer screening with CT: evaluation of radiologists and different computer assisted detection software (CAD) as first and second readers for lung nodule detection at different dose levels. Eur J Radiol 82:e873–e878
Wang S, Zhou M, Liu Z et al (2017) Central focused convolutional neural networks: developing a data-driven model for lung nodule segmentation. Med Image Anal 40:172–183
Ciompi F, Chung K, van Riel SJ et al (2017) Towards automatic pulmonary nodule management in lung cancer screening with deep learning. Sci Rep 7:46479
Ardila D, Kiraly AP, Bharadwaj S et al (2019) End-to-end lung cancer screening with three-dimensional deep learning on low-dose chest computed tomography. Nat Med 25:954–961
National Lung Screening Trial Research Team, Aberle DR, Berg CD et al (2011) The National Lung Screening Trial: overview and study design. Radiology 258:243–253
Lung-RADS Assessment Categories, Version 1.1. American College of Radiology. Lung CT Screening Reporting and Data System (Lung-RADS™). Available via http://www.acr.org/Quality-Safety/Resources/LungRADS. Accessed September 2019
Landis JR, Koch GG (1977) The measurement of observer agreement for categorical data. Biometrics 33:159–174
Liang M, Tang W, Xu DM et al (2016) Low-dose CT screening for lung cancer: computer-aided detection of missed lung cancers. Radiology 281:279–288
Brown M, Browning P, Wahi-Anwar MW et al (2019) Integration of chest CT CAD into the clinical workflow and impact on radiologist efficiency. Acad Radiol 26:626–631
Armato SG 3rd, McLennan G, Bidaut L et al (2011) The Lung Image Database Consortium (LIDC) and Image Database Resource Initiative (IDRI): a completed reference database of lung nodules on CT scans. Med Phys 38:915–931
Clark TJ, Flood TF, Maximin ST, Sachs PB (2015) Lung CT screening reporting and data system speed and accuracy are increased with the use of a semiautomated computer application. J Am Coll Radiol 12:1301–1306
Li L, Liu Z, Huang H, Lin M, Luo D (2019) Evaluating the performance of a deep learning-based computer-aided diagnosis (DL-CAD) system for detecting and characterizing lung nodules: comparison with the performance of double reading by radiologists. Thorac Cancer 10:183–192
Pinsky PF, Gierada DS, Black W et al (2015) Performance of Lung-RADS in the National Lung Screening Trial: a retrospective assessment. Ann Intern Med 162:485–491
Funding
This study received funding from the Industrial Strategic Technology Development program (10072064, Development of Novel Artificial Intelligence Technologies to Assist Imaging Diagnosis of Pulmonary, Hepatic, and Cardiac Diseases and Their Integration into Commercial Clinical PACS Platforms) funded by the Ministry of Trade Industry and Energy (MI, Korea) and from the Korea Health Technology R&D Project through the Korea Health Industry Development Institute (KHIDI), funded by the Ministry of Health & Welfare, Republic of Korea (grant number: HI18C0673).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Guarantor
The scientific guarantor of this publication is Sang Min Lee.
Conflict of interest
Two of the authors of this manuscript (Hyunho Park and Kyuhwan Jung) belong to VUNO Inc., Seoul, South Korea, but they were not involved in the data analysis, and they did not control the data. Otherwise, none of the authors have conflicts of interest and all authors have read and approved this manuscript.
Statistics and biometry
Seo Young Park, who is a statistician in Asan medical center, provided statistical advice for this manuscript.
Informed consent
All study cases were derived from the National Lung Cancer Screening Trial (NLST) and all participants provided informed consent.
Ethical approval
The NLST was approved by the institutional review board of all participating centers.
Study subjects or cohorts overlap
All of our study patients (200 out of 200) were reported in a previous retrospective study, which built a deep learning-based computer-aided diagnosis system performing lung cancer risk categorization tasks and evaluated its performance for lung cancer screening (reference 14, End-to-end lung cancer screening with three-dimensional deep learning on low-dose chest computed tomography. Nat Med 25:954-961).
Methodology
• retrospective
• observational
• performed at one institution
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
ESM 1
(DOCX 23 kb)
Rights and permissions
About this article
Cite this article
Park, S., Park, H., Lee, S.M. et al. Application of computer-aided diagnosis for Lung-RADS categorization in CT screening for lung cancer: effect on inter-reader agreement. Eur Radiol 32, 1054–1064 (2022). https://doi.org/10.1007/s00330-021-08202-3
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00330-021-08202-3