Abstract
Objectives
To evaluate the value of MRI in differentiating benign (b-MCN) and malignant (m-MCN) MCN. European guidelines suggest that certain mucinous cystic neoplasms (MCN) of the pancreas can be conservatively managed.
Methods
A retrospective single-center study of consecutive patients with resected MCN. MRIs were independently reviewed by two readers blinded to the pathological results. The authors compared b-MCN (i.e., mucinous-cystadenoma comprising high-grade dysplasia (HGD)) and m-MCN (i.e., cystadenocarcinoma).
Results
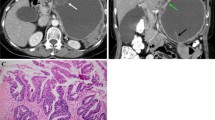
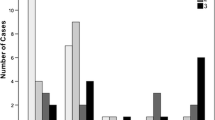
Sixty-three patients (62 women [98%]) with 63 MCN (6 m-MCN, 2 HGD) were included. m-MCN tumors had a tendency to be larger than b-MCN (median 86 [25–103] vs. 45 [17–130] mm, p = .055). The combination of signal heterogeneity on T2-weighted imaging, wall thickness ≥ 5 mm, the presence of mural nodules ≥ 9 mm, and enhancing septa had an area under the ROC curve of 0.97 (95% CI 0.91–1.00) for the diagnosis of m-MCN. A total of 24 (37%), 20 (32%), 10 (16%), 5 (8%), and 4 (6%) out of 63 MCNs showed 0, 1, 2, 3, and 4 of these features, respectively. The corresponding rate of m-MCN was 0%, 0%, 10%, 20%, and 100%, respectively, with a good-to-excellent inter-reader agreement. Patterns with a high NPV for m-MCN included an absence of enhancing septa or walls (NPV 97% and 100%, respectively), wall thickness < 3 mm (NPV 100%), and no mural nodules (NPV 100%).
Conclusions
A combination of 4 imaging features suggests malignant MCN on MRI. On the other hand, visualization of a thin non-enhancing wall with no mural nodules suggests benign MCN.
Key Points
• A heterogenous signal on T2-weighted MRI, a ≥ 5-mm-thick wall, mural nodules ≥ 9 mm, and/or enhancing septa suggest malignant MCNs.
• A thin non-enhancing wall with no mural nodules suggests benign MCNs.
• MRI should be performed in the pre-therapeutic evaluation of MCN to help determine the therapeutic strategy in these patients.





Similar content being viewed by others
Abbreviations
- b-MCN:
-
Benign mucinous cystic neoplasm
- HGD:
-
High-grade dysplasia
- MCN:
-
Mucinous cystic neoplasms
- m-MCN:
-
Malignant mucinous cystic neoplasm
References
Nagtegaal ID, Odze RD, Klimstra D et al (2020) The 2019 WHO classification of tumours of the digestive system. Histopathology 76:182–188
Zamboni G, Scarpa A, Bogina G et al (1999) Mucinous cystic tumors of the pancreas: clinicopathological features, prognosis, and relationship to other mucinous cystic tumors. Am J Surg Pathol 23:410–422
Nilsson LN, Keane MG, Shamali A et al (2016) Nature and management of pancreatic mucinous cystic neoplasm (MCN): a systematic review of the literature. Pancreatology 16:1028–1036
Hui L, Rashid A, Foo WC et al (2018) Significance of T1a and T1b carcinoma arising in mucinous cystic neoplasm of pancreas. Am J Surg Pathol 42:578
O'Toole D, Palazzo L, Hammel P et al (2004) Macrocystic pancreatic cystadenoma: the role of EUS and cyst fluid analysis in distinguishing mucinous and serous lesions. Gastrointest Endosc 59:823–829
Cizginer S, Turner B, Bilge AR, Karaca C, Pitman MB, Brugge WR (2011) Cyst fluid carcinoembryonic antigen is an accurate diagnostic marker of pancreatic mucinous cysts. Pancreas 40:1024–1028
Zhong N, Zhang L, Takahashi N et al (2012) Histologic and imaging features of mural nodules in mucinous pancreatic cysts. Clin Gastroenterol Hepatol 10:192–198. e192
Genevay M, Mino-Kenudson M, Yaeger K et al (2011) Cytology adds value to imaging studies for risk assessment of malignancy in pancreatic mucinous cysts. Ann Surg 254
The European Study Group on Cystic Tumours of the Pancreas (2018) European evidence-based guidelines on pancreatic cystic neoplasms. Gut 67:789–804
Park JW, Jang J-Y, Kang MJ, Kwon W, Chang YR, Kim S-W (2014) Mucinous cystic neoplasm of the pancreas: is surgical resection recommended for all surgically fit patients? Pancreatology 14:131–136
Crippa S, Salvia R, Warshaw AL et al (2008) Mucinous cystic neoplasm of the pancreas is not an aggressive entity: lessons from 163 resected patients. Ann Surg 247:571
Yamao K, Yanagisawa A, Takahashi K et al (2011) Clinicopathological features and prognosis of mucinous cystic neoplasm with ovarian-type stroma: a multi-institutional study of the Japan Pancreas Society. Pancreas 40:67–71
Kosmahl M, Egawa N, Schröder S, Carneiro F, Lüttges J, Klöppel G (2002) Mucinous nonneoplastic cyst of the pancreas: a novel nonneoplastic cystic change? Mod Pathol 15:154–158
Jais B, Rebours V, Malleo G et al (2016) Serous cystic neoplasm of the pancreas: a multinational study of 2622 patients under the auspices of the International Association of Pancreatology and European Pancreatic Club (European Study Group on Cystic Tumors of the Pancreas). Gut 65(2):305–312
Le Baleur Y, Couvelard A, Vullierme MP et al (2011) Mucinous cystic neoplasms of the pancreas: definition of preoperative imaging criteria for high-risk lesions. Pancreatology 11:495–499
Di Paola V, Manfredi R, Mehrabi S et al (2016) Pancreatic mucinous cystoadenomas and cystoadenocarcinomas: differential diagnosis by means of MRI. Br J Radiol 89:20150536
Falconi M, Mantovani W, Crippa S, Mascetta G, Salvia R, Pederzoli P (2008) Pancreatic insufficiency after different resections for benign tumours. Br J Surg 95:85–91
Regi P, Salvia R, Cena C, Girelli R, Frigerio I, Bassi C (2013) Cystic “feminine” pancreatic neoplasms in men. Do any clinical alterations correlate with these uncommon entities? Int J Surg 11:157–160
Procacci C, Carbognin G, Accordini S et al (2001) CT features of malignant mucinous cystic tumors of the pancreas. Eur Radiol 11:1626–1630
Garces-Descovich A, Beker K, Castillo-Angeles M et al (2018) Mucinous cystic neoplasms of the pancreas: high-resolution cross-sectional imaging features with clinico-pathologic correlation. Abdom Radiol (NY) 43:1413–1422
Postlewait LM, Ethun CG, McInnis MR et al (2017) Association of preoperative risk factors with malignancy in pancreatic mucinous cystic neoplasms: a multicenter study. JAMA Surg 152:19–25
Keane MG, Shamali A, Nilsson LN et al (2018) Risk of malignancy in resected pancreatic mucinous cystic neoplasms. Br J Surg 105:439–446
Goh BK, Tan Y-M, Chung Y-FA et al (2006) A review of mucinous cystic neoplasms of the pancreas defined by ovarian-type stroma: clinicopathological features of 344 patients. World J Surg 30:2236–2245
Manfredi R, Ventriglia A, Mantovani W et al (2015) Mucinous cystic neoplasms and serous cystadenomas arising in the body-tail of the pancreas: MR imaging characterization. Eur Radiol 25:940–949
Mamone G, Barresi L, Tropea A, Di Piazza A, Miraglia R (2020) MRI of mucinous pancreatic cystic lesions: a new updated morphological approach for the differential diagnosis. Updates Surg 72:617–637
Funding
The authors state that this work has not received any funding.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Guarantor
The scientific guarantor of this publication is Dr. Marie-Pierre Vullierme, MD.
Conflict of interest
The authors of this manuscript declare no relationships with any companies whose products or services may be related to the subject matter of the article.
Statistics and biometry
Dr. Maxime Ronot and Dr. Jules Gregory kindly provided statistical advice for this manuscript. Both authors have significant statistical expertise. No complex statistical methods were necessary for this paper.
Informed consent
Written informed consent was not required for this study because the study was retrospective upon preoperative MRI.
Ethical approval
Institutional Review Board approval was obtained, Board -IRB 00006477- of HUPNVS, Paris 7 University, AP-HP.
Methodology
• retrospective
• case-control study
• performed at one institution
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
ESM 1
(DOCX 16 kb)
Rights and permissions
About this article
Cite this article
Vullierme, MP., Gregory, J., Rebours, V. et al. MRI is useful to suggest and exclude malignancy in mucinous cystic neoplasms of the pancreas. Eur Radiol 32, 1297–1307 (2022). https://doi.org/10.1007/s00330-021-08091-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00330-021-08091-6