Abstract
Objective
To evaluate the added value of point shear-wave elastography (pSWE) in the diagnostic performance of conventional US for diagnosis of acute cholecystitis.
Methods
B-mode and colour Doppler US and pSWE were performed prospectively in 216 patients with clinically suspected acute cholecystitis. The morphology and mural vascularity of the gallbladder and median shear wave velocity (SWV) of the right liver were evaluated. Two observers independently reviewed conventional US images and subsequently reviewed combined conventional US and pSWE images.
Results
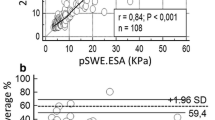
Mean SWVs of the acute cholecystitis group (n = 91) were significantly higher than those of the control group (n = 85) in the right liver within 2 cm lateral to the gallbladder (1.56 versus 1.03 m/s, 1.39 versus 1.04 m/s, P < 0.0001) with a cut-off value of 1.29 or 1.16 m/s. The area under the receiver operating characteristic curve of both observers in the diagnosis of acute cholecystitis improved significantly from 0.790 and 0.777 to 0.963 and 0.962, respectively, after additional review of pSWE images (P < 0.0001). Diagnostic accuracy, sensitivity, specificity, positive and negative predictive values of combined image sets were higher than those of conventional US images alone.
Conclusion
Adding pSWE to conventional US improves the diagnosis of acute cholecystitis when compared with conventional US alone.
Key Points
• In acute cholecystitis, stiffness of the right liver increases adjacent to the gallbladder.
• The cut-off value for diagnosing acute cholecystitis was 1.29 or 1.16 m/s.
• Adding pSWE to conventional US improves the diagnosis of acute cholecystitis.



Similar content being viewed by others
Abbreviations
- US:
-
Ultrasound
- GB:
-
Gallbladder
- pSWE:
-
Point shear-wave elastography
- SWV:
-
Shear wave velocity
- LS:
-
Liver stiffness
- ROC:
-
Receiver operating characteristic
- PPV:
-
Positive predictive value
- NPV:
-
Negative predictive value
References
Strasberg SM (2008) Clinical practice. Acute calculous cholecystitis. N Engl J Med 358:2804–2811
Hirota M, Takada T, Kawarada Y et al (2007) Diagnostic criteria and severity assessment of acute cholecystitis: Tokyo Guidelines. J Hepatobiliary Pancreat Surg 14:78–82
Gurusamy KS, Davidson C, Gluud C, Davidson BR (2013) Early versus delayed laparoscopic cholecystectomy for people with acute cholecystitis. Cochrane Database Syst Rev 6, CD005440
Trowbridge RL, Rutkowski NK, Shojania KG (2003) Does this patient have acute cholecystitis? JAMA 289:80–86
Yokoe M, Takada T, Strasberg SM et al (2012) New diagnostic criteria and severity assessment of acute cholecystitis in revised Tokyo Guidelines. J Hepatobiliary Pancreat Sci 19:578–585
Kiewiet JJ, Leeuwenburgh MM, Bipat S, Bossuyt PM, Stoker J, Boermeester MA (2012) A systematic review and meta-analysis of diagnostic performance of imaging in acute cholecystitis. Radiology 264:708–720
Yarmish GM, Smith MP, Rosen MP et al (2014) ACR appropriateness criteria right upper quadrant pain. J Am Coll Radiol 11:316–322
Hanbidge AE, Buckler PM, O'Malley ME, Wilson SR (2004) From the RSNA refresher courses: imaging evaluation for acute pain in the right upper quadrant. Radiographics 24:1117–1135
Ralls PW, Colletti PM, Lapin SA et al (1985) Real-time sonography in suspected acute cholecystitis. Prospective evaluation of primary and secondary signs. Radiology 155:767–771
Shlaer WJ, Leopold GR, Scheible FW (1981) Sonography of the thickened gallbladder wall: a nonspecific finding. AJR Am J Roentgenol 136:337–339
Cooperberg PL, Gibney RG (1987) Imaging of the gallbladder, 1987. Radiology 163:605–613
Bamber J, Cosgrove D, Dietrich CF et al (2013) EFSUMB guidelines and recommendations on the clinical use of ultrasound elastography. Part 1: Basic principles and technology. Ultraschall Med 34:169–184
Frulio N, Trillaud H (2013) Ultrasound elastography in liver. Diagn Interv Imaging 94:515–534
Goertz RS, Egger C, Neurath MF, Strobel D (2012) Impact of food intake, ultrasound transducer, breathing maneuvers and body position on acoustic radiation force impulse (ARFI) elastometry of the liver. Ultraschall Med 33:380–385
Popescu A, Bota S, Sporea I et al (2013) The influence of food intake on liver stiffness values assessed by acoustic radiation force impulse elastography-preliminary results. Ultrasound Med Biol 39:579–584
Yamashita K, Jin MJ, Hirose Y et al (1995) CT finding of transient focal increased attenuation of the liver adjacent to the gallbladder in acute cholecystitis. AJR Am J Roentgenol 164:343–346
Ito K, Awaya H, Mitchell DG et al (1997) Gallbladder disease: appearance of associated transient increased attenuation in the liver at biphasic, contrast-enhanced dynamic CT. Radiology 204:723–728
Kim YK, Kwak HS, Kim CS et al (2009) CT findings of mild forms or early manifestations of acute cholecystitis. Clin Imaging 33:274–280
Bota S, Sporea I, Peck-Radosavljevic M et al (2013) The influence of aminotransferase levels on liver stiffness assessed by acoustic radiation force impulse elastography: a retrospective multicentre study. Dig Liver Dis 45:762–768
Attia D, Pischke S, Negm AA et al (2014) Changes in liver stiffness using acoustic radiation force impulse imaging in patients with obstructive cholestasis and cholangitis. Dig Liver Dis 46:625–631
Soyer P, Brouland JP, Boudiaf M et al (1998) Color velocity imaging and power Doppler sonography of the gallbladder wall: a new look at sonographic diagnosis of acute cholecystitis. AJR Am J Roentgenol 171:183–188
Uggowitzer M, Kugler C, Schramayer G et al (1997) Sonography of acute cholecystitis: comparison of color and power Doppler sonography in detecting a hypervascularized gallbladder wall. AJR Am J Roentgenol 168:707–712
Toshima T, Shirabe K, Takeishi K et al (2011) New method for assessing liver fibrosis based on acoustic radiation force impulse: a special reference to the difference between right and left liver. J Gastroenterol 46:705–711
Barr RG, Ferraioli G, Palmeri ML et al (2015) Elastography assessment of liver fibrosis: Society of Radiologists in Ultrasound Consensus Conference Statement. Radiology 276:845–861
Ferraioli G, Filice C, Castera L et al (2015) WFUMB guidelines and recommendations for clinical use of ultrasound elastography: Part 3: liver. Ultrasound Med Biol 41:1161–1179
D'Onofrio M, Gallotti A, Mucelli RP (2010) Tissue quantification with acoustic radiation force impulse imaging: measurement repeatability and normal values in the healthy liver. AJR Am J Roentgenol 195:132–136
Karlas T, Pfrepper C, Wiegand J et al (2011) Acoustic radiation force impulse imaging (ARFI) for non-invasive detection of liver fibrosis: examination standards and evaluation of interlobe differences in healthy subjects and chronic liver disease. Scand J Gastroenterol 46:1458–1467
Cohan RH, Mahony BS, Bowie JD, Cooper C, Baker ME, Illescas FF (1987) Striated intramural gallbladder lucencies on US studies: predictors of acute cholecystitis. Radiology 164:31–35
Bota S, Sporea I, Sirli R, Popescu A, Danila M, Sendroiu M (2011) Factors that influence the correlation of acoustic radiation force impulse (ARFI), elastography with liver fibrosis. Med Ultrasound 13:135–140
Ralls PW, Halls J, Lapin SA, Quinn MF, Morris UL, Boswell W (1982) Prospective evaluation of the sonographic Murphy sign in suspected acute cholecystitis. J Clin Ultrasound 10:113–115
Martinez A, Bona X, Velasco M, Martin J (1986) Diagnostic accuracy of ultrasound in acute cholecystitis. Gastrointest Radiol 11:334–338
Bree RL (1995) Further observations on the usefulness of the sonographic Murphy sign in the evaluation of suspected acute cholecystitis. J Clin Ultrasound 23:169–172
Tang A, Cloutier G, Szeverenyi NM, Sirlin CB (2015) Ultrasound elastography and MR elastography for assessing liver fibrosis: Part 1, principles and techniques. AJR Am J Roentgenol 205:22–32
Shiina T, Nightingale KR, Palmeri ML et al (2015) WFUMB guidelines and recommendations for clinical use of ultrasound elastography: Part 1: basic principles and terminology. Ultrasound Med Biol 41:1126–1147
Acknowledgments
The scientific guarantor of this publication is Dae Seob Choi. The authors of this manuscript declare no relationships with any companies, whose products or services may be related to the subject matter of the article. The authors state that this work has not received any funding. No complex statistical methods were necessary for this paper. Institutional Review Board approval was obtained. Written informed consent was obtained from all subjects (patients) in this study. Methodology: prospective, diagnostic study, performed at one institution.
Author information
Authors and Affiliations
Corresponding author
Electronic supplementary material
Below is the link to the electronic supplementary material.
Table 1
Definition of four-point scale used in the first and second reading session (DOC 31 kb)
Appendix
Appendix
In the acute cholecystitis group, 80 patients were referred from the emergency room and 11 were referred from the clinic. In the control group, 50 and 35 patients were referred from the emergency room and clinic, respectively. The median duration between the onset of signs and US was 2 days (range, 1-14 days) and 3 days (range, 1-90 days) in the acute cholecystitis group and control group, respectively. The final clinical outcomes of acute cholecystitis patients (n = 91) were determined by laparoscopic cholecystectomy and histopathology analysis (n = 74) or by percutaneous drainage of pus from the GB (n = 17) according to the surgeon’s decision regarding the underlying conditions or diseases of patients. The median interval between the US and surgery was 1 day (range, 0-3 days). Twenty-four patients had surgery on the same day that the US was performed, 21 patients after 1 day, 20 patients after 2 days, and in 9 cases cholecystectomy was performed 3 days after US. The diagnoses of 91 patients with acute cholecystitis were as follows: acute calculous cholecystitis (n = 68), acute acalculous cholecystitis (n = 23), acute gangrenous cholecystitis (n = 13), and combined xanthogranulomatous cholecystitis (n = 1). Among the control patients (n = 85), 45 patients who underwent laparoscopic cholecystectomy on the same day that the US was performed were diagnosed with chronic cholecystitis. The other control patients were diagnosed by laboratory and CT findings at the admission and clinical follow-up for at least 6 months after admission. The diagnoses of these 40 patients were as follows: acute pancreatitis (n = 24), acute pyelonephritis (n = 5), acute diverticulitis (n = 3), pregnancy (n = 2), hepatobiliary malignancy (n = 4), and undefined diagnosis (n = 2).
Rights and permissions
About this article
Cite this article
Kim, J.E., Choi, D.S., Bae, K. et al. Added value of point shear-wave elastography in the diagnosis of acute cholecystitis. Eur Radiol 27, 1517–1526 (2017). https://doi.org/10.1007/s00330-016-4509-x
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00330-016-4509-x