Abstract
Objectives
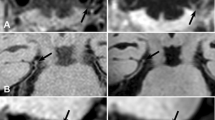
Previous studies using intracranial vessel wall MRI techniques showed that over 50 % of patients with ischemic stroke or TIA had one or more intracranial vessel wall lesions. In the current study, we assessed the preferential location of these lesions within the intracranial arterial tree and their potential changes over time in these patient groups.
Methods
Forty-nine patients with ischemic stroke (n = 25) or TIA (n = 24) of the anterior cerebral circulation underwent 7.0 T MRI, including a T1-weighted magnetization-preparation inversion recovery turbo-spin-echo (MPIR-TSE) sequence within one week and approximately one month after symptom onset. Intracranial vessel wall lesions were scored for multiple locations within the arterial tree and differences between one-week and one-month images.
Results
At baseline, 132 intracranial vessel wall lesions were found in 41 patients (84 %), located primarily in the anterior cerebral circulation (74 %), with a preferential location in the distal internal carotid artery and M1 and M2 segments of the middle cerebral artery. During follow-up, presence or enhancement patterns changed in 14 lesions (17 %).
Conclusions
A large burden of intracranial vessel wall lesions was found in both the anterior and posterior cerebral circulation. Most lesions were found to be relatively stable, possibly indicating a more generalized atherosclerotic process.
Key points
• Intracranial vessel wall lesions are present in patients with varying cerebrovascular diseases.
• Intracranial vessel wall 7.0 T MRI provides information on preferential location and natural course.
• Distal ICA and M1 and M2 segments of MCA are predilection sites.
• 83 % of lesions found remained stable, possibly indicating more generalized atherosclerosis.




Similar content being viewed by others
Abbreviations
- A1:
-
A1 segment of anterior cerebral artery
- ACA:
-
Anterior cerebral artery
- FFE:
-
Fast field echo
- FOV:
-
Field of view
- ICA:
-
Internal carotid artery
- IVI:
-
Intracranial vessel wall imaging
- TIA:
-
Transient ischemic attack
- M1:
-
M1 segment of middle cerebral artery
- M2:
-
M2 segment of middle cerebral artery
- M3:
-
M3 segment of middle cerebral artery
- MCA:
-
Middle cerebral artery
- MPIR-TSE:
-
Magnetization-preparation inversion recovery turbo-spin-echo
- MRI:
-
Magnetic resonance imaging
- NSA:
-
Number of signal averages
- P1:
-
P1 segment of posterior cerebral artery
- P2:
-
P2 segment of posterior cerebral artery
- PCA:
-
Posterior cerebral artery
- SSS-TOAST:
-
Stop Stroke Study Trial of Org 10172 in Acute Stroke Treatment
- T:
-
Tesla
- TE:
-
Echo time
- TI:
-
Inversion time
- TOF-MRA:
-
Time-of-flight magnetic resonance angiography
- TR:
-
Repetition time
- TSE:
-
Turbo-spin-echo
References
Gorelick PB, Wong KS, Bae HJ, Pandey DK (2008) Large artery intracranial occlusive disease: a large worldwide burden but a relatively neglected frontier. Stroke 39:2396–2399
Qureshi AI, Caplan LR (2014) Intracranial atherosclerosis. Lancet 383:984–998
Park JK, Kim SH, Kim BS, Choi G, Jeong SY, Choi JC (2011) Imaging of intracranial plaques with black-blood double inversion recovery MR imaging and CT. J Neuroimaging 21:e64–e68
van der Kolk AG, Zwanenburg JJ, Brundel M et al (2011) Intracranial vessel wall imaging at 7.0-T MRI. Stroke 42:2478–2484
Turan TN, Bonilha L, Morgan PS, Adams RJ, Chimowitz MI (2011) Intraplaque hemorrhage in symptomatic intracranial atherosclerotic disease. J Neuroimaging 21:e159–e161
Xu WH, Li ML, Gao S et al (2011) Plaque distribution of stenotic middle cerebral artery and its clinical relevance. Stroke 42:2957–2959
Chung GH, Kwak HS, Hwang SB, Jin GY (2012) High resolution MR imaging in patients with symptomatic middle cerebral artery stenosis. Eur J Radiol 81:4069–4074
Kim YS, Lim SH, Oh KW et al (2012) The advantage of high-resolution MRI in evaluating basilar plaques: a comparison study with MRA. Atherosclerosis 224:411–416
Lou X, Ma N, Ma L, Jiang WJ (2013) Contrast-enhanced 3 T high-resolution MR imaging in symptomatic atherosclerotic basilar artery stenosis. AJNR Am J Neuroradiol 34:513–517
Skarpathiotakis M, Mandell DM, Swartz RH, Tomlinson G, Mikulis DJ (2013) Intracranial atherosclerotic plaque enhancement in patients with ischemic stroke. AJNR Am J Neuroradiol 34:299–304
van der Kolk AG, Hendrikse J, Brundel M et al (2013) Multi-sequence whole-brain intracranial vessel wall imaging at 7.0 tesla. Eur Radiol 23:2996–3004
Glagov S, Weisenberg E, Zarins CK, Stankunavicius R, Kolettis GJ (1987) Compensatory enlargement of human atherosclerotic coronary arteries. N Engl J Med 316:1371–1375
Kiechl S, Willeit J (1999) The natural course of atherosclerosis. Part II: vascular remodeling. Bruneck Study Group. Arterioscler Thromb Vasc Biol 19:1491–1498
Mazighi M, Labreuche J, Gongora-Rivera F, Duyckaerts C, Hauw JJ, Amarenco P (2008) Autopsy prevalence of intracranial atherosclerosis in patients with fatal stroke. Stroke 39:1142–1147
Vink A, Schoneveld AH, Poppen M, de Kleijn DP, Borst C, Pasterkamp G (2002) Morphometric and immunohistochemical characterization of the intimal layer throughout the arterial system of elderly humans. J Anat 200:97–103
Maes F, Collignon A, Vandermeulen D, Marchal G, Suetens P (1997) Multimodality image registration by maximization of mutual information. IEEE Trans Med Imaging 16:187–198
Chimowitz MI, Kokkinos J, Strong J et al (1995) The warfarin-aspirin symptomatic intracranial disease study. Neurology 45:1488–1493
Mazighi M, Tanasescu R, Ducrocq X et al (2006) Prospective study of symptomatic atherothrombotic intracranial stenoses: the GESICA study. Neurology 66:1187–1191
Turan TN, Makki AA, Tsappidi S et al (2010) Risk factors associated with severity and location of intracranial arterial stenosis. Stroke 41:1636–1640
Pu Y, Liu L, Wang Y et al (2013) Geographic and sex difference in the distribution of intracranial atherosclerosis in china. Stroke 44:2109–2114
Cecchi E, Giglioli C, Valente S et al (2011) Role of hemodynamic shear stress in cardiovascular disease. Atherosclerosis 214:249–256
Tao WD, Liu M, Fisher M et al (2012) Posterior versus anterior circulation infarction: how different are the neurological deficits? Stroke 43:2060–2065
Adams HP Jr, Bendixen BH, Kappelle LJ et al (1993) Classification of subtype of acute ischemic stroke. Definitions for use in a multicenter clinical trial. TOAST. Trial of Org 10172 in Acute Stroke Treatment. Stroke 24:35–41
Acknowledgments
The scientific guarantor of this publication is Jeroen Hendrikse. The authors of this manuscript declare relationships with the following companies: Fredy Visser is employed by of Philips Healthcare, Best, the Netherlands. This study was performed within the framework of the Center for Translational Molecular Medicine (CTMM, www.ctmm.nl) project PARISk (grant 01C-202), and supported by the Dutch Heart Foundation. No complex statistical methods were necessary for this paper. Institutional Review Board approval was obtained. Written informed consent was obtained from all subjects (patients) in this study. Some study subjects or cohorts have been previously reported in Stroke 2011;42(9):2478–2484 (in this technical study evaluating the small-coverage MPIR-TSE sequence, partial baseline data of 21 patients was published). Methodology: prospective, observational study, performed at one institution.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
van der Kolk, A.G., Zwanenburg, J.J.M., Brundel, M. et al. Distribution and natural course of intracranial vessel wall lesions in patients with ischemic stroke or TIA at 7.0 tesla MRI. Eur Radiol 25, 1692–1700 (2015). https://doi.org/10.1007/s00330-014-3564-4
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00330-014-3564-4