Abstract
Objectives
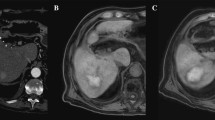
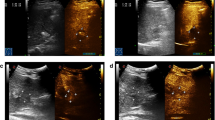
To assess the incidence and degree of MRI contrast enhancement in liver tumours following successful percutaneous cryoablation.
Methods
Thirty-eight patients with liver metastases (n = 29) or hepatocellular carcinoma (n = 9) underwent percutaneous cryoablation of 45 tumours between March 2004 and June 2009, with complete ablation zone coverage of the tumour and no local recurrence on follow-up imaging to date (range 3–60 months, mean 16). Contrast-enhanced MRI was used to assess 45 tumours at 24 h, 32 tumours at 2–4 months, and 21 tumours at 5–7 months. Percentage of tumours with contrast enhancement was assessed using dynamic spoiled gradient echo T1-weighted images.
Results
Twenty-four hours post-cryoablation, 23 out of 45 tumours (51%) enhanced compared with 42 out of 43 (98%) pre-ablation (p < 0.001). Mean percentage tumour enhancement decreased from 157% (range 26–745%) pre-ablation, to 107% (27–260%) at 24 h (p = 0.003), and 43% (24–103%) at 2–4 months (p < 0.001). The incidence and degree of tumour enhancement decreased through 5–7 months.
Conclusions
Unlike previously reported studies of radiofrequency ablation, successful cryoablation of liver tumours is often associated with persistent tumour contrast enhancement on MRI performed at 24 h and decreasing over 2–7 months.
Key Points
• Liver neoplasms often demonstrate MRI contrast enhancement following successful percutaneous cryoablation.
• This differs from radiofrequency ablation techniques where contrast enhancement suggests residual tumour
• This difference could potentially lead to important errors in follow up strategies.


Similar content being viewed by others
References
McGahan JP, van Raalte VA (2005) History of ablation. In: van Sonnenberg E, McMullen W, Solbiati L (eds) Tumor ablation: principles and practice. Springer, New York, pp 3–12
Hinshaw JL, Lee FT (2007) Cryoablation for liver cancer. Tech Vasc Interv Radiol 10:47–57
Silverman SG, Tuncali KT, Adams DF, van Sonnenberg E, Zou KH, Kacher DF, Morrison PR, Jolesz FA (2000) MR imaging-guided percutaneous cryotherapy of liver tumors: initial experience. Radiology 217:657–664
Vossen JA, Buijs M, Kamel IR (2006) Assessment of tumor response on MR imaging after locoregional therapy. Tech Vasc Interv Radiol 9:125–132
Rossi S, Buscarini E, Garbagnati F, Di Stasi M, Quaretti P, Rago M, Zangrandi A, Andreola S, Silverman D, Buscarini L (1998) Percutaneous treatment of small hepatic tumors by an expandable RF needle electrode. AJR Am J Roentgenol 170:1015–1022
Kierans AS, Elazzazi M, Braga L, Leonardou P, Gerber D, Burke C, Qureshi W, Kanematsu M, Semelka R (2010) Thermoablative treatments for malignant liver lesions: 10-year experience of MRI appearances of treatment response. AJR Am J Roentgenol 194:523–529
Porter CA, Woodrum DA, Callstrom MR, Schmit GD, Misra S, Charboneau JW, Atwell TD (2010) MRI after technically successful renal cryoablation: early contrast enhancement as a common finding. AJR Am J Roentgenol 194:790–793
Ho VB, Allen SF, Hood MN, Choyke PL (2002) Renal masses: quantitative assessment of enhancement with dynamic MR imaging. Radiology 224:695–700
Hoffmann NE, Bischof JC (2002) The cryobiology of cryosurgical injury. Urology 60S:40–49
Mazur P (1984) Freezing of living cells: mechanisms and implications. Am J Physiol 247:C125–C142
Pollock GA, Pegg DE, Hardie IR (1986) An isolated perfused rat mesentery model for direct observation of the vasculature during cryopreservation. Cryobiology 23:500–511
Zook N, Hussmann J, Brown R (1998) Microcirculatory studies of frostbite injury. Ann Plast Surg 40:246–253
Goldberg SN, Grassi CJ, Cardella JF et al (2005) Image-guided tumor ablation: standardization of terminology and reporting criteria. Radiology 235:728–739
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Shyn, P.B., Oliva, M.R., Shah, S.H. et al. MRI contrast enhancement of malignant liver tumours following successful cryoablation. Eur Radiol 22, 398–403 (2012). https://doi.org/10.1007/s00330-011-2254-8
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00330-011-2254-8