Abstract
Objective
To prospectively assess the diagnostic performance of contrast-enhanced ultrasound (CEUS) and MR imaging in incidental solid focal liver lesions not characterised on ultrasound.
Materials and methods
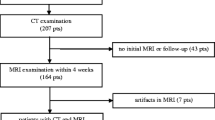
Forty-seven patients with 50 lesions underwent MR imaging and CEUS: 24 focal nodular hyperplasias (FNH), 11 adenomas, 10 haemangiomas, 1 focal fatty change and 4 malignant lesions were identified. Two experienced radiologists randomly reviewed contrast-enhanced MR imaging and CEUS data, and provided the most likely diagnosis. Sensitivity (Se), specificity (Sp), likelihood ratios (LR) and kappa value were calculated.
Results
A histotype diagnosis was obtained in 66–52% with MR imaging and 52–53% with CEUS, respectively, for both readers. Se, Sp and LR for haemangioma were 100–100, 100–100 and 78–78 with MR imaging and 89–89, 100–100 and 68–70 with CEUS; for FNH with MR imaging they were 88–63, 96–100 and 23–34 and 74–67, 88–96 and 6–17 with CEUS. If the diagnosis of haemangioma was uncertain with CEUS, MR imaging always confirmed the diagnosis. If the diagnosis of FNH was uncertain with either CEUS or MR imaging, the other imaging technique confirmed the diagnosis in approximately half the cases.
Conclusion
Both CEUS and MR imaging have a high diagnostic performance in incidental focal liver lesions and are complementary when diagnosis is uncertain.



Similar content being viewed by others
References
Little JM, Richardson A, Tait N (1991) Hepatic dystychoma: a five year experience. HPB Surg 4:291–297
Semelka RC, Sofka CM (1997) Hepatic hemangiomas. Magn Reson Imaging Clin N Am 5:241–253
Vilgrain V (2006) Focal nodular hyperplasia. Eur J Radiol 58:236–245
Quaia E, Stacul F, Gaiani S, Ricci P, Passariello R, Curzio D et al (2004) Comparison of diagnostic performance of unenhanced vs SonoVue - enhanced ultrasonography in focal liver lesions characterization. The experience of three Italian centers. Radiol Med (Torino) 108:71–81
Nicolau C, Vilana R, Catala V, Bianchi L, Gilabert R, Garcia A et al (2006) Importance of evaluating all vascular phases on contrast-enhanced sonography in the differentiation of benign from malignant focal liver lesions. AJR Am J Roentgenol 186:158–167
Albrecht T, Blomley M, Bolondi L, Claudon M, Correas JM, Cosgrove D et al (2004) Guidelines for the use of contrast agents in ultrasound. January 2004. Ultraschall Med 25:249–256
Claudon M, Cosgrove D, Albrecht T, Bolondi L, Bosio M, Calliada F et al (2008) Guidelines and good clinical practice recommendations for contrast enhanced ultrasound (CEUS) - update 2008. Ultraschall Med 29:28–44
Elsayes KM, Leyendecker JR, Menias CO et al (2007) MRI characterization of 124 CT-indeterminate focal hepatic lesions: evaluation of clinical utility. HPB (Oxford) 9:208–215
Phongkitkarun S, Srianujata T, Jatchavala J (2009) Supplement value of magnetic resonance imaging in small hepatic lesion (< or = 20 mm) detected on routine computed tomography. J Med Assoc Thai 92:677–686
Vilgrain V, Flejou JF, Arrive L, Belghiti J, Najmark D, Menu Y et al (1992) Focal nodular hyperplasia of the liver: MR imaging and pathologic correlation in 37 patients. Radiology 184:699–703
Soyer P, Gueye C, Somveille E, Laissy JP, Scherrer A (1995) MR diagnosis of hepatic metastases from neuroendocrine tumors versus hemangiomas: relative merits of dynamic gadolinium chelate-enhanced gradient-recalled echo and unenhanced spin-echo images. AJR Am J Roentgenol 165:1407–1413
Buetow PC, Pantongrag-Brown L, Buck JL, Ros PR, Goodman ZD (1996) Focal nodular hyperplasia of the liver: radiologic-pathologic correlation. Radiographics 16:369–388
Horton KM, Bluemke DA, Hruban RH, Soyer P, Fishman EK (1999) CT and MR imaging of benign hepatic and biliary tumors. Radiographics 19:431–451
Arrive L, Flejou JF, Vilgrain V, Belghiti J, Najmark D, Zins M et al (1994) Hepatic adenoma: MR findings in 51 pathologically proved lesions. Radiology 193:507–512
Quaia E, Calliada F, Bertolotto M, Rossi S, Garioni L, Rosa L et al (2004) Characterization of focal liver lesions with contrast-specific US modes and a sulfur hexafluoride-filled microbubble contrast agent: diagnostic performance and confidence. Radiology 232:420–430
Kim TK, Jang HJ, Burns PN, Murphy-Lavallee J, Wilson SR (2008) Focal nodular hyperplasia and hepatic adenoma: differentiation with low-mechanical-index contrast-enhanced sonography. AJR Am J Roentgenol 190:58–66
Wilson SR, Burns PN (2006) An algorithm for the diagnosis of focal liver masses using microbubble contrast-enhanced pulse-inversion sonography. AJR Am J Roentgenol 86:1401–1412
Harvey CJ, Albrecht T (2001) Ultrasound of focal liver lesions. Eur Radiol 11:1578–1593
Trillaud H, Bruel JM, Valette PJ et al (2009) Characterization of focal liver lesions with SonoVue-enhanced sonography: international multicenter-study in comparison to CT and MRI. World J Gastroenterol 15:3748–3756
Fagan TJ (1975) Letter: Nomogram for Bayes theorem. N Engl J Med 293:257
Agresti A (2002) Categorical data analysis, 2nd edn. Wiley, New York
Ihaka R, Gentleman R (1996) R: a language for data analysis and graphics. J Comp GraphStat 5:299–314
Begg CB, Greenes RA, Iglewicz B (1986) The influence of uninterpretability on the assessment of diagnostic tests. J Chronic Dis 39:575–584
Youk JH, Kim CS, Lee JM (2003) Contrast-enhanced agent detection imaging: value in the characterization of focal hepatic lesions. J Ultrasound Med 22:897–910
Leen E, Ceccotti P, Kalogeropoulou C, Angerson WJ, Moug SJ, Horgan PG (2006) Prospective multicenter trial evaluating a novel method of characterizing focal liver lesions using contrast-enhanced sonography. AJR Am J Roentgenol 186:1551–1559
Burns PN, Wilson SR (2007) Focal liver masses: enhancement patterns on contrast-enhanced images–concordance of US scans with CT scans and MR images. Radiology 242:162–174
Jaeschke R, Guyatt GH, Sackett DL (1994) Users' guides to the medical literature. III. How to use an article about a diagnostic test. B. What are the results and will they help me in caring for my patients? The Evidence-Based Medicine Working Group. JAMA 271:703–707
Nguyen BN, Flejou JF, Terris B, Belghiti J, Degott C (1999) Focal nodular hyperplasia of the liver: a comprehensive pathologic study of 305 lesions and recognition of new histologic forms. Am J Surg Pathol 3(12):1441–1454
Attal P, Vilgrain V, Brancatelli G, Paradis V, Terris B, Belghiti J et al (2003) Telangiectatic focal nodular hyperplasia: US, CT, and MR imaging findings with histopathologic correlation in 13 cases. Radiology 228:465–472
Paradis V, Champault A, Ronot M, Deschamps L, Valla DC, Vidaud D et al (2007) Telangiectatic adenoma: an entity associated with increased body mass index and inflammation. Hepatology 46:140–146
Romanini L, Passamonti M, Aiani L, Cabassa P, Raieli G, Montermini I et al (2007) Economic assessment of contrast-enhanced ultrasonography for evaluation of focal liver lesions: a multicentre Italian experience. Eur Radiol 17(Suppl 6):F99–F106
Cherqui D, Rahmouni A, Charlotte F, Boulahdour H, Metreau JM, Meignan M et al (1995) Management of focal nodular hyperplasia and hepatocellular adenoma in young women: a series of 41 patients with clinical, radiological, and pathological correlations. Hepatology 22:1674–1681
Semelka RC, Brown ED, Ascher SM, Patt RH, Bagley AS, Li W et al (1994) Hepatic hemangiomas: a multi-institutional study of appearance on T2-weighted and serial gadolinium-enhanced gradient-echo MR images. Radiology 192:401–406
Herman P, Pugliese V, Machado MA et al (2000) Hepatic adenoma and focal nodular hyperplasia: differential diagnosis and treatment. World J Surg 24:372–376
Choi BY, Nguyen MH (2005) The diagnosis and management of benign hepatic tumors. J Clin Gastroenterol 39:401–412
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Soussan, M., Aubé, C., Bahrami, S. et al. Incidental focal solid liver lesions: diagnostic performance of contrast-enhanced ultrasound and MR imaging. Eur Radiol 20, 1715–1725 (2010). https://doi.org/10.1007/s00330-009-1700-3
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00330-009-1700-3