Abstract
Objectives
Contrast-enhanced cardiac magnetic resonance (CMR) for infarct sizing has been validated in large animals, but studies and follow-up are restricted. We sought to (1) validate CMR for assessment of myocardial area at risk (MAR) and infarct size (IS) in a rabbit model of reperfused myocardial infarction (MI); (2) analyse the relation between ischaemic substrates and subsequent left ventricular (LV) remodelling.
Methods
Experimental reperfused acute MI was induced in 16 rabbits. Ten animals underwent cross-registered cine and contrast-enhanced CMR and histopathology at day 3 for assessment of MAR and IS (group 1). The remaining six rabbits underwent serial CMR for the study of LV remodelling (group 2).
Results
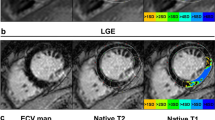
In group 1, mean IS was 12.7 ± 6.4% and 12.7 ± 6.9% of total LV myocardial mass on CMR (late-enhancement technique) and histopathology (P = 0.52; r = 0.93). No significant difference occurred between CMR and histopathology for the calculation of MAR and IS/MAR ratio (P = 0.18 and P = 0.17), whereas correlations were strong (r = 0.92 and r = 0.95). In group 2, mean LV end-diastolic, end-systolic volumes and LV mass were significantly increased at 3 weeks compared with measurements at day 3 (P < 0.01). Significant correlations between initial IS and the increase in LV end-diastolic volume (r = 0.66) and the increase in LV mass (r = 0.48) were observed, as well as correlations between initial MAR and the increase in LV end-diastolic volume (r = 0.70) and the increase in LV mass (r = 0.37).
Conclusions
Comprehensive CMR provides accurate assessment of IS and MAR in reperfused rabbit MI. Infarct size is closely related to LV remodelling. Through the infarct size/MAR ratio, this approach has great potential for assessing interventions aimed at cardioprotection.



Similar content being viewed by others
References
Allman KC, Shaw LJ, Hachamovitch R et al (2002) Myocardial viability testing and impact of revascularisation on prognosis in patients with coronary artery disease and left ventricular dysfunction: a meta-analysis. J Am Coll Cardiol 39:1151–1158
Bax JJ, Poldermans D, Elhendy A et al (1999) Improvement o left ventricular ejection fraction, heart failure symptoms and prognosis after revascularization in patients with chronic coronary artery disease and viable myocardium detected by dobutamine stress echocardiography. J Am Coll Cardiol 34:163–169
Kim RJ, Wu E, Rafael A et al (2000) The use of contrast-enhanced MRI to identify reversible myocardial dysfunction. N Engl J Med 343:1445–1453
Nijveldt R, Hofman MBM, Hirsch A et al (2009) Assessment of microvascular obstruction and prediction of short-term remodeling after acute myocardial infarction: cardiac MR imaging study. Radiology 250:363–370
Gerber BL, Garot J, Bluemke DA et al (2002) Accuracy of contrast-enhanced magnetic resonance imaging in predicting improvement of regional myocardial function in patients after acute myocardial infarction. Circulation 106:1083–1089
Kuhl HP, Beek AM, van der Weerdt AP et al (2003) Myocardial viability in chronic ischemic heart disease: comparison of contrast-enhanced magnetic resonance imaging with (18)F-fluorodeoxyglucose positron emission tomography. J Am Coll Cardiol 41:1341–1348
Wagner A, Mahrholdt H, Holly TA et al (2003) Contrast-enhanced MRI and routine single photon emission computed tomography (SPECT) perfusion imaging for detection of subendocardial myocardial infarcts: an imaging study. Lancet 361:374–379
Cochet AA, Lorgis L, Lalande A, Zeller M, Beer JC, Walker PM, Touzery C, Wolf JE, Brunotte F, Cottin Y (2009) Major prognostic impact of persistent microvascular obstruction as assessed by contrast-enhanced cardiac magnetic resonance in reperfused acute myocardial infarction. Eur Radiol 19:2117–2126
Hunold P, Schlosser T, Barkhausen J (2006) Magnetic resonance cardiac perfusion imaging—a clinical perspective. Eur Radiol 16:1779–1188
Kim RJ, Chen EL, Lima JA et al (1996) Myocardial Gd-DTPA kinetics determine MRI contrast enhancement and reflect the extent and severity of myocardial injury after acute reperfused infarction. Circulation 94:3318–3326
Kim RJ, Fieno DS, Parrish TB et al (1999) Relationship of MRI delayed contrast enhancement to irreversible injury, infarct age, and contractile function. Circulation 100:1992–2002
Fieno DS, Kim RJ, Chen EL et al (2000) Contrast-enhanced magnetic resonance imaging of myocardium at risk: distinction between reversible and irreversible injury throughout infarct healing. J Am Coll Cardio l36:1985–1991
Barkhausen J, Ebert W, Debatin JF et al (2002) Imaging of myocardial infarction: comparison of Magnevist and Gadophrin-3 in rabbits. J Am Coll Cardiol 39:1392–1398
Yellon DM, Baxter GF (2000) Protecting the ischaemic and reperfused myocardium in acute myocardial infarction: distant dream or near reality? Heart 83:381–387
Tissier R, Aouam K, Berdeaux A, Ghaleh B (2003) Evidence for a ceiling of cardioprotection with a nitric oxide donor-induced delayed preconditioning in rabbits. J Pharmacol Exp Ther 306:528–531
Tissier R, Waintraub X, Couvreur N et al (2007) Pharmacological postconditioning with the phytoestrogen genistein. J Mol Cell Cardiol 42:79–87
Saeed M, Bremerich J, Wendland MF et al (1999) Reperfused myocardial infarction as seen with use of necrosis-specific versus standard extracellular contrast agents in rats. Radiology 213:247–257
Carluccio E, Biagioli P, Alunni G et al (2006) Patients with hibernating myocardium show altered left ventricular volumes and shape, which revert after revascularization: evidence that dyssynergy might directly induce cardiac remodeling. J Am Coll Cardiol 47:969–977
Pflugfelder PW, Wisenberg G, Prato FS et al (1986) Serial imaging of canine myocardial infarction by in vivo nuclear magnetic resonance. J Am Coll Cardiol 7:843–849
Caputo GR, Sechtem U, Tscholakoff D et al (1987) Measurements of myocardial infarct size at early and late time intervals using MR imaging: an experimental study in dogs. Am J Roentgenol 149:237–242
Johnston DL, Homma S, Liu P et al (1988) Serial changes in nuclear magnetic resonance relaxation times after myocardial infarction in the rabbit: relationship to water content, severity of ischemia, and histopathology over a six-month period. Magn Reson Med 8:363–379
Ryan T, Tarver RD, Duerk JL et al (1990) Distinguishing viable from infarcted myocardium after experimental ischemia and reperfusion by using nuclear magnetic resonance imaging. J Am Coll Cardiol 15:1355–1364
Bouchard A, Reeves RC, Cranney G et al (1989) Assessment of myocardial infarct size by means of T2-weighted 1H nuclear magnetic resonance imaging. Am Heart J 117:281–289
Acknowledgments
Dr Mansencal was supported by a grant from the Fédération Française de Cardiologie Paris, France. Prof. Garot was supported in part by a “Dotation à la Recherche par équipe” from the Maison du Cœur, Paris, France. None of the authors has any conflict of interest to declare.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Mansencal, N., Tissier, R., Deux, JF. et al. Relation of the ischaemic substrate to left ventricular remodelling by cardiac magnetic resonance at 1.5 T in rabbits. Eur Radiol 20, 1214–1220 (2010). https://doi.org/10.1007/s00330-009-1660-7
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00330-009-1660-7