Abstract
Purpose
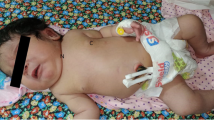
The aim of this study is to present a case series of patients with congenital Zika syndrome (CZS), giving special attention to the more relevant aspects for the paediatric orthopaedic surgeon.
Methods
An analytical cross-sectional study was performed in a group of 47 patients affected by CZS with maternal Zika serology confirmation. Clinical features of the maternal Zika infection, prenatal and perinatal complications, and patient demographic data were recorded. In addition, clinical and radiographic evaluations of the lower limb (hip, knee, and foot) were performed.
Results
Maternal Zika infection occurred at an average of 12.5 (± 6.4) weeks of gestation. The rates of complications during pregnancy and delivery were 37% and 17.4%, respectively. At the time of the clinical evaluation, spasticity was appreciated in 77.3% of the cases, and arthrogryposis was present in 15.2%. Foot deformities were appreciated in 41.2% of the cases, hip alterations in aggregate in 29.8% (adduction contracture in 20.2%; displacement in 7.5%), and knee alterations in 12.8% (displacement in 6.4%). The deformities in arthrogrypotic patients were both more prevalent and severe. All arthrogrypotic patients were simultaneously spastic.
Conclusions
The current study demonstrates a high prevalence of musculoskeletal alterations in patients with CZS. Affected patients were able to be classified as belonging to one of three types at the time of evaluation: Type I patients presented with a low incidence of musculoskeletal complications; Type II demonstrated progressive deformities; Type III presented with simultaneously the most prevalent and severe deformities. This classification system could help guide medical and surgical management of CZS patients based on the frequency and severity of the deformities at the time of initial evaluation.
Similar content being viewed by others
References
Sarno M, Sacramento GA, Khouri R et al (2016) Zika virus infection and stillbirths: a case of hydrops fetalis, hydranencephaly and fetal demise. PLoS Negl Trop Dis 10:e0004517
Driggers RW, Ho CY, Korhonen EM et al (2016) Zika virus infection with prolonged maternal viremia and fetal brain abnormalities. N Engl J Med 374:2142–2151
Ventura CV, Maia M, Bravo-Filho V, Góis AL, Belfort R Jr (2015) Zika virus in Brazil and macular atrophy in a child with microcephaly. Lancet 387:228
Marques FJP, Teixeira MCS, Barra RR et al (2019) Children born with congenital Zika syndrome display atypical gross motor development and a higher risk for cerebral palsy. J Child Neurol 34:81–85
Moore CA, Staples JE, Dobyns WB et al (2017) Characterizing the pattern of anomalies in congenital Zika syndrome for pediatric clinicians. JAMA Pediatr 171:288–295
Kapogiannis BG, Chakhtoura N, Hazra R, Spong CY (2017) Bridging knowledge gaps to understand how Zika virus exposure and infection affect child development. JAMA Pediatr 171:478–485
Del Campo M, Feitosa IM, Ribeiro EM et al (2017) The phenotypic spectrum of congenital Zika syndrome. Am J Med Genet 173:841–857
Linden VD, Filho EL, Lins OG et al (2016) Congenital Zika syndrome with arthrogryposis: retrospective case series study. BMJ 354:i3899
Narayanan U, Mulpuri K, Sankar WN et al (2015) Reliability of a new radiographic classification for developmental dysplasia of the hip. J Pediatr Orthop 35:478–484
Leal MD, Esteves-Pereira AP, Nakamura-Pereira M et al (2016) Prevalence and risk factors related to preterm birth in Brazil. Reprod Health 13(Suppl 3):127
Jain L, Ferre C, Vidyasagar D, Nath S, Sheftel D (1991) Cardiopulmonary resuscitation of apparently stillborn infants: survival and long-term outcome. J Pediatr 118:778–782
Sakkas H, Bozidis P, Giannakopoulos X, Sofikitis N, Papadopoulou C (2018) An update on sexual transmission of Zika virus. Pathogens 7:66
Moreira J, Peixoto TM, Siqueira AM, Lamas SS (2017) Sexually acquired Zika virus: a systematic review. Clin Microbiol Infect 23:296–305
Silva AAM, Ganz JSS, Sousa PS et al (2016) Early growth and neurologic outcomes of infants with probable congenital Zika virus syndrome. Emerg Infect Dis 22:1953–1956
Schuler-Faccini L, Ribeiro EM, Feitosa IML (2015) Brazilian medical genetics society–Zika embryopathy task force. Possible association between Zika virus infection and microcephaly - Brazil. Morb Mortal Wkly Rep 65:59–62
Oliveira Melo AS, Malinger G, Ximenes R, Szejnfeld PO, Alves Sampaio S, Bispo de Filippis AM (2016) Zika virus intrauterine infection causes fetal brain abnormality and microcephaly: tip of the iceberg? Ultrasound Obstet Gynecol 47:6–7
Alvino ACMI, Mello LRM, Oliveira JAMM (2016) Association of arthrogryposis in neonates with microcephaly due to Zika virus - a case serie. Rev Bras Saude Mater Infant 16(suppl.1):S83–S88
Funding
This work was supported by the FUNDAÇÂO DE AMPARO À PESQUISA DO ESTADO DA BAHIA (FAPESB) under grant number PIE00022/2016.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Matos, M.A., Nascimento, M.A.S.T. & Merriman, J.W. Orthopaedic approach to the congenital Zika syndrome. International Orthopaedics (SICOT) 45, 559–564 (2021). https://doi.org/10.1007/s00264-020-04521-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00264-020-04521-0