Abstract
Purpose
The aim of this study was to evaluate the rationality of the suture locations of distal plantar fascia (DPF) after foot amputation to avoid the risk factors of re-amputation or plantar fasciitis.
Methods
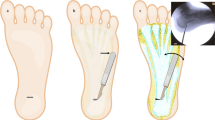
The tensile strain of plantar fascia (PF) in the different regions was measured by uni-axial tensile experiment. A three-dimensional (3D) finite element model was also developed to simulate tensile behaviour of PF in weight bearing conditions. The model includes 12 bones, ligaments, PF, cartilage and soft tissues. Four suture location models for the DPF were considered: the fourth and fifth DPF were sutured on the third metatarsal, the cuboid, and both the third metatarsal and the cuboid, and one un-sutured model.
Results
The peak tensile strain of the first, second and third PF was 0.134, 0.128 and 0.138 based on the mechanical test, respectively. The fourth and fifth DPF sutured at the cuboid and the third metatarsal could offer more favourable outcomes. The peak strain of 4.859 × 10–2, 2.347 × 10–2 and 1.364 × 10–2 in the first, second and third PF showed the least outcomes in stance phase. Also, peak strain and stress of the residual PF reduced to 4.859 × 10–2 and 1.834 MPa, respectively. The stress region was redistributed on the mid-shaft of the first and third PF and the peak stress of medial cuneiform bone evidently decreased.
Conclusions
The fourth and fifth DPF suture at the third metatarsal and cuboid was appropriate for the partial foot. The findings are expected to suggest optimal surgical plan of the DPF suture and guide further therapeutic planning of partial foot patients.








Similar content being viewed by others
References
Fukano M, Fukubayashi T (2009) Motion characteristics of the medial and lateral longitudinal arch during landing. Eur J Appl Physiol 105(3):387–392. doi:10.1007/s00421-008-0915-3
Kirby K (2005) Ten biomechanical functions of the plantar fascia (Abstract). J Sci Med Sport 8(4):146
Hicks JH (1954) The plantar aponeurosis and the arch. J Anat 88:25–30
Ker RF, Bennett MB, Bibby SR, Kester RC, Alexander RM (1987) The spring in the arch of the human foot. Nature 325:147–149
Ponten B (1981) The fasciocutaneous flap: its use in soft tissue defects of the lower leg. Br J Plast Surg 34:215–220
Summers PR, Biswas MK, Herrera EH (1990) Relative strength of a new suture technique for fascial closure. J Gynecol Surg 6:119–121
William W, Shaw MD, David A, Hidalgo MD (1985) Anatomic basic of plantar flap design: clinical applications. Plast Reconstr Surg 78:637–649
Saxena A, Fullem B (2004) Plantar fascia ruptures in athletes. Am J Sports Med 32:662–665. doi:10.1177/03635465032 61727
Louwers MJ, Sabb B, Pangilinan PH (2010) Ultrasound evaluation of a spontaneous plantar fascia rupture. Am J Phys Med Rehabil 89:941–944. doi:10.1097/PHM.0b013e3181f711e2
Lee HS, Choi YR, Kim SW, Lee JY, Seo JH, Jeong JJ (2014) Risk factors affecting chronic rupture of the plantar fascia. Foot Ankle Int 35(3):258–263. doi:10.1177/1071100713514564
Finni T, Komi PV, Lukkariniemi J (1998) Achilles tendon loading during walking: application of a novel optic fiber technique. Eur J Appl Physiol Occup Physiol 77:289–291. doi:10.1007/s004210050335
Carlson RE, Fleming LL, Hutton WC (2000) The biomechanical relationship between the tendoachilles, plantar fascia and metatarsophalangeal joint dorsiflexion angle. Foot Ankle Int 21:18–25. doi:10.1177/107110070002100104
Sakalauskaitė R, Satkunskienė D (2012) The foot arch and viscoelastic properties of plantar fascia and Achilles tendon. J Vibroeng 4(4):1751–1759
Erdemir A, Hamel AJ, Fauth AR, Piazza SJ, Sharkey NA (2004) Dynamic loading of the plantar aponeurosis in walking. J Bone Joint Surg Am 86:546–552
Crary JL, Hollis JM (2003) The effect of plantar fascia release on strain in the spring and long plantar ligaments. Foot Ankle Int 24:245–250. doi:10.1177/107110070302400308
Robert G (2005) Toe and partial foot amputations. Oper Tech Gen Surg 7(2):67–73. doi:10.1053/j.optechgensurg.2005.07.002
Sage RA (2010) Risk and prevention of reulceration after partial foot amputation. Foot Ankle Clin 15(3):495–500. doi:10.1016/j.fcl.2010.04.006
Chittoria R, Mishra SM (2004) Fasciocutaneous flaps in reconstruction of lower extremity: our experience. Kathmandu Univ Med J 2(4):344–348
Ronald A, Sage DPM (2010) Risk and prevention of reulceration after partial foot amputation. Foot Ankle Clin 15:495–500. doi:10.1016/j.fcl.2010.04.006
Liu X, Wang L, Ji J (2014) A mechanical model of the cornea considering the crimping morphology of collagen fibrils. Invest Ophthalmol Vis Sci 55(4):2739–2746. doi:10.1167/iovs.13-12633
Srinivas CT, Ahmet E, Peter RC (2011) Comparison of hexahedral and tetrahedral elements in finite element analysis of the foot and footwear. J Biomech 44:2337–2343. doi:10.1016/j.jbiomech.2011.05.006
Gefen A, Megido-Ravid M, Itzchak Y, Arcan M (2000) Biomechanical analysis of the three-dimensional foot structure during gait: a basic tool for clinical applications. J Biomech Eng 122:630–639. doi:10.1115/1.1318904
Zhang M, Mak AFT (1999) In vivo friction properties of human skin. Prosthetics Orthot Int 23:135–141. doi:10.3109/03093649909071625
Spyrou LA, Aravas N (2012) Muscle-driven finite element simulation of human foot movements. Comput Method Biomech 15(9):925–934. doi:10.1080/10255842.2011.566564
Athanasiou KA, Liu GT, Lavery LA (1998) Biomechanical topography of human articular cartilage in the first metatarsophalangeal joint. Clin Orthop Relat Res 348:269–281
Siegler S, Block J, Schneck CD (1988) The mechanical characteristics of the collateral ligaments of the human ankle joint. Foot Ankle 8:234–242
Erdemir A, Viveiros ML, Ulbrecht JS, Cavanagh PR (2006) An inverse finite-element model of heel-pad indentation. J Biomech 39(7):1279–1286. doi:10.1016/j.jbiomech.2005.03.007
Petre M, Erdemir A, Panoskaltsis VP, Spirka TA, Cavanagh PR (2013) Optimization of nonlinear hyperelastic coefficients for foot tissues using a magnetic resonance imaging deformation experiment. J Biomech Eng 135(6):61001–61012. doi:10.1115/1.4023695
Cheung JT, Zhang M, Leung AK, Fan YB (2005) Three-dimensional finite element analysis of the foot during standing-a material sensitivity study. J Biomech 38:1045–1054. doi:10.1016/j.jbiomech.2004.05.035
Yaodong G, Jianshe L, Xuejun R, Mark J, Yanjun Z (2010) Heel skin stiffness effect on the hind foot biomechanics during heel strike. Skin Res Technol 16(3):291–296. doi:10.1111/j.1600-0846.2010.00425.x
Zhihui Q, Lei R, Luquan R (2010) A coupling analysis of the biomechanical functions of human foot complex during locomotion. J Bionic Eng 1:150–157. doi:10.1016/S1672-6529(09)60229-8
Gratz CM (1931) Tensile strength and elasticity tests on human Fascia Lata. J Bone Joint Surg 13:334–340
Welk AB, Haun DW, Clark TB, Kettner NW (2015) Use of high-resolution ultrasound to measure changes in plantar fascia thickness resulting from tissue creep in runners and walkers. J Manip Physiol Ther 38(1):81–85. doi:10.1016/j.jmpt.2014.10.008
Headlee DL, Leonard JL, Hart JM, Ingersoll CD (2008) Fatigue of the plantar intrinsic foot muscles increases navicular drop. J Electromyogr Kinesiol 18:420–425. doi:10.1016/j.jelekin.2006.11.004
Griffin NL, Richmond BG (2005) Cross-sectional geometry of the human forefoot. Bone 37:253–260. doi:10.1016/j.bone.2005.04.019
Kogler GF, Solomonidis SE, Paul JP (1995) In vitro method for quantifying the effectiveness of the longitudinal arch support mechanism of a foot orthosis. Clin Biomech 10:225–245
Kogler GF, Solomonidis SE, Paul JP (1996) Biomechanics of longitudinal arch support mechanisms in foot orthoses and their effect on plantar aponeurosis strain. Clin Biomech 11:243–252
McMillan AM, Landorf KB, Gilheany MF (2012) Ultrasound guided corticosteroid injection for plantar fasciitis: randomized controlled trial. Br Med J 344:3260
Taunton JE, Ryan MB, Clement DB, McKenzie DC, Lloyd-Smith DR (2002) A retrospective case control analysis of 267 running injuries. Br J Sport Med 36:95–101. doi:10.1136/bmj.e3260
Parada F (2014) Plantar fasciitis. From etiology to treatment. Ann Phys Rehabil Med 57:428. doi:10.1016/j.rehab.2014.03.1562
Smith JW (1954) Elastic properties of the anterior cruciate ligament of the rabbit. J Anat 88:369–380
Kim W, Voloshin AS (1995) Role of plantar fascia in the load bearing capacity of the human foot. J Biomech 28:1025–1033
Halloran JP, Ackermann M, Erdemir A, van den Bogert AJ (2010) Concurrent musculoskeletal dynamics and finite element analysis predicts altered gait patterns to reduce foot tissue loading. J Biomech 43(14):2810–2815. doi:10.1016/j.jbiomech.2010.05.036
Acknowledgments
The project was supported by the National Natural Science Foundation of China (11120101001, 11202017, 11421202), National Science & Technology Pillar Program (2012BAI18B05, 2012BAI18B07), Research Fund for the Doctoral Program of Higher Education of China (20121102120039, 20131102130004) and 111 Project (B13003).
Conflict of interest
There are no conflicts of interest involved in the manuscript.
Author information
Authors and Affiliations
Corresponding authors
Rights and permissions
About this article
Cite this article
Guo, JC., Wang, Lz., Mo, ZJ. et al. Biomechanical analysis of suture locations of the distal plantar fascia in partial foot. International Orthopaedics (SICOT) 39, 2373–2380 (2015). https://doi.org/10.1007/s00264-015-2889-1
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00264-015-2889-1