Abstract
Objective
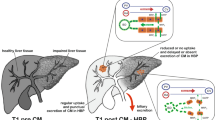
To determine if transit time for excretion of gadoxetate into major bile ducts and duodenum correlates with clinical models of hepatocellular function.
Methods
This retrospective research was approved by the Institutional Review Board with waiver of informed consent. Search of the radiology database from January 1, 2013 to March 4, 2014 revealed 84 patients with chronic liver disease (65 males, mean age 47 years). Eighteen control subjects with no known liver disease or risk factors were also enrolled for analysis (9 males, mean age 43 years). MRI was performed with hepatobiliary phases at 10, 15, 20, and 25 min after injection of 0.025 mmol/kg of gadoxetate (Primovist, Bayer HealthCare, Shanghai, China). The time of excreted contrast appearing in the biliary tree and in the duodenum was recorded. Linear trend analysis was performed to determine the relationship between excretion time and hepatic function.
Results
The patient cohort was stratified by Child-Pugh classification (A, B, and C with n = 53, 27, and 4, respectively). Arrival of gadoxetate in the gall bladder at 10-min hepatobiliary phase was seen in 87% of control group and 45% of Child-Pugh A group (p = 0.02). There was no difference between these groups for later hepatobiliary phases. The arrival of biliary contrast in the right hepatic duct, common bile duct, and gall bladder were significantly earlier in the Child-Pugh A group compared to the Child-Pugh B/C group at all hepatobiliary phases after 10 min (p < 0.05). Linear trend analysis showed that biliary transit times were significantly delayed with worsening liver function (p = 0.01). There was no difference in entry time of gadoxetate into the duodenum between the normal, Child-Pugh A, and Child-Pugh B/C groups.
Conclusions
The transit time for gadoxetate to appear in extrahepatic duct is a reasonable indicator of liver function, and may be included in radiology reports. The appearance in the duodenum, however, may depend on factors other than liver function, such as the physiology of the gallbladder and sphincter of Oddi.



Similar content being viewed by others
References
Hamm B, Staks T, Muhler A, et al. (1995) Phase I clinical evaluation of Gd-EOB-DTPA as a hepatobiliary MR contrast agent: safety, pharmacokinetics, and MR imaging. Radiology 195(3):785–792
Kim H, Kim MJ (2013) Hepatic uptake of gadoxetic acid. Radiology 267(1):314–315
van Montfoort JE, Stieger B, Meijer DK, et al. (1999) Hepatic uptake of the magnetic resonance imaging contrast agent gadoxetate by the organic anion transporting polypeptide Oatp1. J Pharmacol Exp Ther 290(1):153–157
Jang YJ, Cho SH, Bae JH, et al. (2013) Noninvasive assessment of hepatic fibrosis using gadoxetate-disodium-enhanced 3T MRI. Ann Hepatol 12(6):926–934
Schuhmann-Giampieri G, Schmitt-Willich H, Press WR, et al. (1992) Preclinical evaluation of Gd-EOB-DTPA as a contrast agent in MR imaging of the hepatobiliary system. Radiology 183(1):59–64
Hoekstra LT, de Graaf W, Nibourg GA, et al. (2013) Physiological and biochemical basis of clinical liver function tests: a review. Ann Surg 257(1):27–36
Carson ER, Jones EA (1979) Use of kinetic analysis and mathematical modeling in the study of metabolic pathways in vivo: applications to hepatic organic anion metabolism (second of two parts). N Engl J Med 300(19):1078–1086
Feier D, Balassy C, Bastati N, et al. (2013) Liver fibrosis: histopathologic and biochemical influences on diagnostic efficacy of hepatobiliary contrast-enhanced MR imaging in staging. Radiology 269(2):460–468
Verloh N, Haimerl M, Rennert J, et al. (2013) Impact of liver cirrhosis on liver enhancement at Gd-EOB-DTPA enhanced MRI at 3 Tesla. Eur J Radiol 82(10):1710–1715
Chernyak V, Kim J, Rozenblit AM, Mazzoriol F, Ricci Z (2011) Hepatic enhancement during the hepatobiliary phase after gadoxetate disodium administration in patients with chronic liver disease: the role of laboratory factors. J Magn Reson Imaging 34(2):301–309
Okada M, Ishii K, Numata K, et al. (2012) Can the biliary enhancement of Gd-EOB-DTPA predict the degree of liver function? Hepatobiliary Pancreat Dis Int 11(3):307–313
Yamada A, Hara T, Li F, et al. (2011) Quantitative evaluation of liver function with use of gadoxetate disodium-enhanced MR imaging. Radiology 260(3):727–733
Wibmer A, Aliya Q, Steininger R, et al. (2012) Liver transplantation: impaired biliary excretion of gadoxate is associated with an inferior 1-year retransplantation-free survival. Invest Radiol 47(6):353–358
Wibmer A, Prusa AM, Nolz R, et al. (2013) Liver failure after major liver resection: risk assessment by using preoperative Gadoxetic acid-enhanced 3-T MR imaging. Radiology 269(3):777–786
Cho SH, Kang UR, Kim JD, Han YS, Choi DL (2011) The value of gadoxetate disodium-enhanced MR imaging for predicting posthepatectomy liver failure after major hepatic resection: a preliminary study. Eur J Radiol 80(2):e195–e200
Motosugi U, Ichikawa T, Sou H, et al. (2009) Liver parenchymal enhancement of hepatocyte-phase images in Gd-EOB-DTPA-enhanced MR imaging: which biological markers of the liver function affect the enhancement? J Magn Reson Imaging 30(5):1042–1046
Onishi H, Theisen D, Dietrich O, Reiser MF, Zech CJ (2014) Hepatic steatosis: effect on hepatocyte enhancement with gadoxetate disodium-enhanced liver MR imaging. J Magn Reson Imaging 39(1):42–50
Tamada T, Ito K, Yamamoto A, et al. (2013) Simple method for evaluating the degree of liver parenchymal enhancement in the hepatobiliary phase of gadoxetic acid-enhanced magnetic resonance imaging. J Magn Reson Imaging 37(5):1115–1121
Ringe KI, Husarik DB, Gupta RT, Boll DT, Merkle EM (2011) Hepatobiliary transit times of gadoxetate disodium (Primovist(R)) for protocol optimization of comprehensive MR imaging of the biliary system–what is normal? Eur J Radiol 79(2):201–205
Brancatelli G, Federle MP, Ambrosini R, et al. (2007) Cirrhosis: CT and MR imaging evaluation. Eur J Radiol 61(1):57–69
Faria SC, Ganesan K, Mwangi I, et al. (2009) MR imaging of liver fibrosis: current state of the art. Radiographics 29(6):1615–1635
Bentler PM, Yuan KH (1996) Test of linear trend in eigenvalues of a covariance matrix with application to data analysis. Br J Math Stat Psychol 49(Pt 2):299–312
Nassif A, Jia J, Keiser M, et al. (2012) Visualization of hepatic uptake transporter function in healthy subjects by using gadoxetic acid-enhanced MR imaging. Radiology 264(3):741–750
Planchamp C, Hadengue A, Stieger B, et al. (2007) Function of both sinusoidal and canalicular transporters controls the concentration of organic anions within hepatocytes. Mol Pharmacol 71(4):1089–1097
Erlinger S (1996) Mechanisms of hepatic transport and bile secretion. Acta Gastroenterol Belg 59(2):159–162
Harvey E, Loberg M, Ryan J, et al. (1979) Hepatic clearance mechanism of Tc-99m-HIDA and its effect on quantitation of hepatobiliary function: concise communication. J Nucl Med 20(4):310–313
Burra P, Masier A (2004) Dynamic tests to study liver function. Eur Rev Med Pharmacol Sci 8(1):19–21
Tschirch FT, Struwe A, Petrowsky H, et al. (2008) Contrast-enhanced MR cholangiography with Gd-EOB-DTPA in patients with liver cirrhosis: visualization of the biliary ducts in comparison with patients with normal liver parenchyma. Eur Radiol 18(8):1577–1586
Takao H, Akai H, Tajima T, et al. (2011) MR imaging of the biliary tract with Gd-EOB-DTPA: effect of liver function on signal intensity. Eur J Radiol 77(2):325–329
Rosenthall L, Shaffer EA, Lisbona R, Pare P (1978) Diagnosis of hepatobiliary disease by 99mTc-HIDA cholescintigraphy. Radiology 126(2):467–474
Author information
Authors and Affiliations
Corresponding author
Additional information
Hui Li and Yuning Lin are co-first authors.
Rights and permissions
About this article
Cite this article
Wu, J., Li, H., Lin, Y. et al. Value of gadoxetate biliary transit time in determining hepatocyte function. Abdom Imaging 40, 95–101 (2015). https://doi.org/10.1007/s00261-014-0200-3
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00261-014-0200-3