Abstract
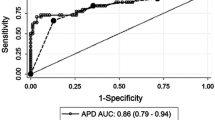
Background: There is a necessity to standardize postnatal ultrasonographic markers predictive of significant uropathies. The purpose of this study was to assess the accuracy of anteroposterior renal pelvic diameter (APD) on postnatal ultrasound to discriminate between significant uropathy and idiopathic renal pelvic dilatation. Materials and methods: Neonates (n=110) who were found to have isolated fetal renal pelvic dilatation underwent systematic investigation and were prospectively followed up. A US scan was performed after the 1st week of life, and all infants underwent voiding cystourethrography. Neonates with an APD larger than 10 mm were examined with renal scintigraphy. Receiver-operating characteristic (ROC) plots were constructed to determine the best cutoffs for APD to identify renal units with significant uropathy as well as those requiring surgical intervention. Results: The area under the curve (AUC) estimated by the ROC curve was 0.921 (95% CI=0.869–0.957), indicating excellent discriminant power between nonsignificant pelvis dilatation and significant uropathy. A cutoff of 10 mm for APD showed the best accuracy for identifying infants with a significant uropathy (sensitivity, 90.4%; specificity, 91%). To identify infants who required surgical intervention, the calculated AUC was 0.976 (95% CI=0.940–0.993). A cutoff of 15 mm showed the best diagnostic performance for identifying the renal units requiring pyeloplasty (sensitivity, 100%; specificity, 92.5%). Conclusion: Our results suggest that postnatal APD is an excellent test for identifying fetuses with significant uropathy, as well as those requiring postnatal intervention.




Similar content being viewed by others
References
Riccabona M, Fotter R (2004) Reorientation and future trends in paediatric uroradiology. Pediatr Radiol 34:295–301
Oliveira EA, Diniz JS, Cabral AC, et al (1999) Prognostic factors in fetal hydronephrosis: a multivariate analysis. Pediatr Nephrol 13:859–864
Cooper CS, Andrews JI, Hansen WF, et al (2002) Antenatal hydronephrosis: evaluation and outcome. Curr Urol Rep 3:131–138
Sairam S, Al-Habib A, Sasson S, et al (2001) Natural history of fetal hydronephrosis diagnosed on mid-trimester ultrasound. Ultrasound Obstet Gynecol 17:191–196
Elder JS (1997) Antenatal hydronephrosis. fetal and neonatal management. Pediatr Clin North Am 44:1299–1321
Woodward M, Frank D (2002) Postnatal management of antenatal hydronephrosis. BJU Int 89:149–156
de Bruyn R, Gordon I (2001) Postnatal investigation of fetal renal disease. Prenat Diagn 21:984–991
Fernbach SK, Maizels M, Conway JJ (1993) Ultrasound grading of hydronephrosis: introduction to the system used by the Society for Fetal Urology. Pediatr Radiol 23:478–480
Corteville JE, Gray DL, Crane JP (1991) Congenital hydronephrosis: correlation of fetal ultrasonographic findings with infant outcome. Am J Obstet Gynecol 165:384–348
Adra AM, Mejides AA, Dennaoui MS, et al (1995) Fetal pyelectasis: is it always “physiologic”? Am J Obstet Gynecol 173:1263–1266
Bouzada MCF, Oliveira EA, Pereira AK, et al (2004) Diagnostic accuracy of fetal renal pelvis anteroposterior diameter as a predictor of uropathy: a prospective study. Ultrasound Obstet Gynecol (in press)
Konda R, Sakai K, Ota S, et al (2002) Ultrasound grade of hydronephrosis and severity of renal cortical damage on 99 m technetium dimercaptosuccinic acid renal scan in infants with unilateral hydronephrosis during follow-up and after pyeloplasty. J Urol 167:2159–2163
Bossuyt PM, Reitsma JB, Bruns DE, et al (2003) The STARD statement for reporting studies of diagnostic accuracy: explanation and elaboration. Ann Intern Med 138:40–44
Ismaili K, Hall M, Donner C, et al (2003) Results of systematic screening for minor degrees of fetal renal pelvis dilatation in an unselected population. Am J Obstet Gynecol 188:242–246
Harding LJ, Malone PS, Wellesley DG (1999) Antenatal minimal hydronephrosis: is its follow-up an unnecessary cause of concern? Prenat Diagn 19:701–705
Thomas DF, Madden NP, Irving HC, et al (1994) Mild dilatation of the fetal kidney: a follow-up study. Br J Urol 74:236–239
Langer B (2000) Fetal pyelectasis. Ultrasound Obstet Gynecol 16:1–5
Marra G, Barbieri G, Moioli C, et al (1994) Mild fetal hydronephrosis indicating vesicoureteric reflux. Arch Dis Child Fetal Neonatal Ed 70:147–149
Johnson CE, Elder JS, Judge NE, et al (1992) The accuracy of antenatal ultrasonography in identifying renal abnormalities. Am J Dis Child 146:1181–1184
Anderson N, Clautice-Engle T, Allan R, et al (1995) Detection of obstructive uropathy in the fetus: predictive value of sonographic measurements of renal pelvic diameter at various gestational ages. AJR 164:719–723
Ouzounian JG, Castro MA, Fresquez M, et al (1996) Prognostic significance of antenatally detected fetal pyelectasis. Ultrasound Obstet Gynecol 7:424–428
Zweig MH, Campbell G (1993) Receiver-operating characteristic (ROC) plots: a fundamental evaluation tool in clinical medicine. Clin Chem 39:561–577
Grignon A, Filion R, Filiatrault D, et al (1986) Urinary tract dilatation in utero: classification and clinical applications. Radiology 160:645–647
Avni FE, Hall M, Schulman CC (1998) Congenital uro-nephropathies: is routine voiding cystourethrography always warranted? Clin Radiol 53:247–250
Blane CE, DiPietro MA, Zerin JM, et al (1993) Renal sonography is not a reliable screening examination for vesicoureteral reflux. J Urol 150:752–725
Tibballs JM, De Bruyn R (1996) Primary vesicoureteric reflux—how useful is postnatal ultrasound? Arch Dis Child 75:444–447
Walsh G, Dubbins PA (1996) Antenatal renal pelvis dilatation: a predictor of vesicoureteral reflux? AJR 167:897–900
Anderson NG, Abbott GD, Mogridge N, et al (1997) Vesicoureteric reflux in the newborn: relationship to fetal renal pelvic diameter. Pediatr Nephrol 11:610–616
Phan V, Traubici J, Hershenfield B, et al (2003) Vesicoureteral reflux in infants with isolated antenatal hydronephrosis. Pediatr Nephrol 18:1224–1228
Avni EF, Ayadi K, Rypens F, et al (1997) Can careful ultrasound examination of the urinary tract exclude vesicoureteric reflux in the neonate? Br J Radiol 70:977–982
Ismaili K, Avni FE, Hall M (2002) Results of systematic voiding cystourethrography in infants with antenatally diagnosed renal pelvis dilation. J Pediatr 141:21–24
Ransley PG, Dhillon HK, Gordon I, et al (1990) The postnatal management of hydronephrosis diagnosed by prenatal ultrasound. J Urol 144:584–587
Acknowledgments
This study was partly supported by Conselho de Desenvolvimento Científico e Tecnológico (CNPq), FAPEMIG, and Pró-Reitoria de Pesquisa-UFMG.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Bouzada, M.C.F., Oliveira, E.A., Pereira, A.K. et al. Diagnostic accuracy of postnatal renal pelvic diameter as a predictor of uropathy: a prospective study. Pediatr Radiol 34, 798–804 (2004). https://doi.org/10.1007/s00247-004-1283-8
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00247-004-1283-8