Abstract
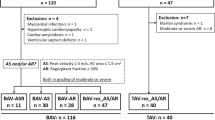
Bicuspid aortic valve (BAV) disease demonstrates a range of clinical presentations and complications. We aim to use cardiac MRI (CMR) to evaluate left ventricular (LV) parameters, myocardial strain and aortic hemodynamics in pediatric BAV patients with and without aortic stenosis (AS) or regurgitation (AR) compared to tricuspid aortic valve (TAV) controls. We identified 58 pediatric BAV patients without additional cardiovascular pathology and 25 healthy TAV controls (15.3 ± 2.2 years) who underwent CMR with 4D flow. BAV cohort included subgroups with no valvulopathy (n = 13, 14.3 ± 4.7 years), isolated AS (n = 19, 14.5 ± 4.0 years), mixed valve disease (AS + AR) (n = 13, 17.1 ± 3.2 years), and prior valvotomy/valvuloplasty (n = 13, 13.9 ± 3.2 years). CMR data included LV volumetric and mass indices, myocardial strain and aortic hemodynamics. BAV patients with no valvulopathy or isolated AS had similar LV parameters to controls excepting cardiac output (p < 0.05). AS + AR and post-surgical patients had abnormal LV volumetric and mass indices (p < 0.01). Post-surgical patients had decreased global longitudinal strain (p = 0.02); other subgroups had comparable strain to controls. Patients with valvulopathy demonstrated elevated velocity and wall shear stress (WSS) in the ascending aorta (AAo) and arch (p < 0.01), while those without valve dysfunction had only elevated AAo velocity (p = 0.03). Across the cohort, elevated AAo velocity and WSS correlated to higher LV mass (p < 0.01), and abnormal hemodynamics correlated to decreased strain rates (p < 0.045). Pediatric BAV patients demonstrate abnormalities in LV parameters as a function of valvular dysfunction, most significantly in children with AS + AR or prior valvotomy/valvuloplasty. Correlations between aortic hemodynamics, LV mass and strain suggest valvular dysfunction could drive LV remodeling. Multiparametric CMR assessment in pediatric BAV may help stratify risk for cardiac remodeling and dysfunction.




Similar content being viewed by others
References
Braverman AC, Guven H, Beardslee MA, Makan M, Kates AM, Moon MR (2005) The bicuspid aortic valve. Curr Probl Cardiol 30(9):470–522. https://doi.org/10.1016/j.cpcardiol.2005.06.002
Masri A, Svensson LG, Griffin BP, Desai MY (2017) Contemporary natural history of bicuspid aortic valve disease: a systematic review. Heart 103(17):1323–1330. https://doi.org/10.1136/heartjnl-2016-309916
Rose MJ, Rigsby CK, Berhane H, Bollache E, Jarvis K, Barker AJ, Schnell S, Allen BD, Robinson JD, Markl M (2019) 4-D flow MRI aortic 3-D hemodynamics and wall shear stress remain stable over short-term follow-up in pediatric and young adult patients with bicuspid aortic valve. Pediatr Radiol 49(1):57–67. https://doi.org/10.1007/s00247-018-4257-y
Schnell S, Smith DA, Barker AJ, Entezari P, Honarmand AR, Carr ML, Malaisrie SC, McCarthy PM, Collins J, Carr JC, Markl M (2016) Altered aortic shape in bicuspid aortic valve relatives influences blood flow patterns. Eur Heart J Cardiovasc Imaging 17(11):1239–1247. https://doi.org/10.1093/ehjci/jew149
van Ooij P, Potters WV, Collins J, Carr M, Carr J, Malaisrie SC, Fedak PW, McCarthy PM, Markl M, Barker AJ (2015) Characterization of abnormal wall shear stress using 4D flow MRI in human bicuspid aortopathy. Ann Biomed Eng 43(6):1385–1397. https://doi.org/10.1007/s10439-014-1092-7
Geiger J, Rahsepar AA, Suwa K, Powell A, Ghasemiesfe A, Barker AJ, Collins JD, Carr JC, Markl M (2018) 4D flow MRI, cardiac function, and T1-mapping: association of valve-mediated changes in aortic hemodynamics with left ventricular remodeling. J Magn Reson Imaging 48(1):121–131. https://doi.org/10.1002/jmri.25916
von Knobelsdorff-Brenkenhoff F, Karunaharamoorthy A, Trauzeddel RF, Barker AJ, Blaszczyk E, Markl M, Schulz-Menger J (2016) Evaluation of aortic blood flow and wall shear stress in aortic stenosis and its association with left ventricular remodeling. Circ Cardiovasc Imaging 9(3):e004038. https://doi.org/10.1161/circimaging.115.004038
Friedman KG, McElhinney DB, Rhodes J, Powell AJ, Colan SD, Lock JE, Brown DW (2013) Left ventricular diastolic function in children and young adults with congenital aortic valve disease. Am J Cardiol 111(2):243–249. https://doi.org/10.1016/j.amjcard.2012.09.026
Miyazaki S, Daimon M, Miyazaki T, Onishi Y, Koiso Y, Nishizaki Y, Ichikawa R, Chiang SJ, Makinae H, Suzuki H, Daida H (2011) Global longitudinal strain in relation to the severity of aortic stenosis: a two-dimensional speckle-tracking study. Echocardiography 28(7):703–708. https://doi.org/10.1111/j.1540-8175.2011.01419.x
Robinson JD, Del Nido PJ, Geggel RL, Perez-Atayde AR, Lock JE, Powell AJ (2010) Left ventricular diastolic heart failure in teenagers who underwent balloon aortic valvuloplasty in early infancy. Am J Cardiol 106(3):426–429. https://doi.org/10.1016/j.amjcard.2010.03.045
Robinson JD, Marx GR, Del Nido PJ, Lock JE, McElhinney DB (2009) Effectiveness of balloon valvuloplasty for palliation of mitral stenosis after repair of atrioventricular canal defects. Am J Cardiol 103(12):1770–1773. https://doi.org/10.1016/j.amjcard.2009.02.062
Tuluce K, Yakar Tuluce S, Cagri Simsek E, Bayata S, Nazli C (2017) Assessment of contributors of aortopathy and subclinical left ventricular dysfunction in normally functioning bicuspid aortic valves. J Heart Valve Dis 26(1):37–44
Tripathi A, Wang Y, Jerrell JM (2018) Population-based treated prevalence, risk factors, and outcomes of bicuspid aortic valve in a pediatric Medicaid cohort. Ann Pediatr Cardiol 11(2):119–124. https://doi.org/10.4103/apc.APC_137_17
Leonardi B, Margossian R, Sanders SP, Chinali M, Colan SD (2014) Ventricular mechanics in patients with aortic valve disease: longitudinal, radial, and circumferential components. Cardiol Young 24(1):105–112. https://doi.org/10.1017/s1047951112002326
Zhang X, Zhu M, He T, Yuan J, Zhu H, Morrisroe DE, Ashraf M, Sahn DJ (2015) Cardiac mechanics in isolated bicuspid aortic valve disease with normal ejection fraction: a study of various valvular lesion types. Medicine 94(47):e2085. https://doi.org/10.1097/md.0000000000002085
Buckert D, Cieslik M, Tibi R, Radermacher M, Rasche V, Bernhardt P, Hombach V, Rottbauer W, Wohrle J (2018) Longitudinal strain assessed by cardiac magnetic resonance correlates to hemodynamic findings in patients with severe aortic stenosis and predicts positive remodeling after transcatheter aortic valve replacement. Clin Res Cardiol 107(1):20–29. https://doi.org/10.1007/s00392-017-1153-7
Burris NS, Lima APS, Hope MD, Ordovas KG (2018) Feature tracking cardiac MRI reveals abnormalities in ventricular function in patients with bicuspid aortic valve and preserved ejection fraction. Tomography 4(1):26–32. https://doi.org/10.18383/j.tom.2018.00005
Kutty S, Rangamani S, Venkataraman J, Li L, Schuster A, Fletcher SE, Danford DA, Beerbaum P (2013) Reduced global longitudinal and radial strain with normal left ventricular ejection fraction late after effective repair of aortic coarctation: a CMR feature tracking study. Int J Cardiovasc Imaging 29(1):141–150. https://doi.org/10.1007/s10554-012-0061-1
Allen BD, van Ooij P, Barker AJ, Carr M, Gabbour M, Schnell S, Jarvis KB, Carr JC, Markl M, Rigsby C, Robinson JD (2015) Thoracic aorta 3D hemodynamics in pediatric and young adult patients with bicuspid aortic valve. J Magn Reson Imaging 42(4):954–963. https://doi.org/10.1002/jmri.24847
Markl M, Schnell S, Wu C, Bollache E, Jarvis K, Barker AJ, Robinson JD, Rigsby CK (2016) Advanced flow MRI: emerging techniques and applications. Clin Radiol 71(8):779–795. https://doi.org/10.1016/j.crad.2016.01.011
Rose MJ, Jarvis K, Chowdhary V, Barker AJ, Allen BD, Robinson JD, Markl M, Rigsby CK, Schnell S (2016) Efficient method for volumetric assessment of peak blood flow velocity using 4D flow MRI. J Magn Reson Imaging 44(6):1673–1682. https://doi.org/10.1002/jmri.25305
Sievers HH, Schmidtke C (2007) A classification system for the bicuspid aortic valve from 304 surgical specimens. J Thoracic Cardiovasc Surg 133(5):1226–1233. https://doi.org/10.1016/j.jtcvs.2007.01.039
Chubb H, Simpson JM (2012) The use of Z-scores in paediatric cardiology. Ann Pediatr Cardiol 5(2):179–184. https://doi.org/10.4103/0974-2069.99622
Cerqueira MD, Weissman NJ, Dilsizian V, Jacobs AK, Kaul S, Laskey WK, Pennell DJ, Rumberger JA, Ryan T, Verani MS (2002) Standardized myocardial segmentation and nomenclature for tomographic imaging of the heart. A statement for healthcare professionals from the Cardiac Imaging Committee of the Council on Clinical Cardiology of the American Heart Association. Circulation 105(4):539–542
Gabriel RS, Renapurkar R, Bolen MA, Verhaert D, Leiber M, Flamm SD, Griffin BP, Desai MY (2011) Comparison of severity of aortic regurgitation by cardiovascular magnetic resonance versus transthoracic echocardiography. Am J Cardiol 108(7):1014–1020. https://doi.org/10.1016/j.amjcard.2011.05.034
Nishimura RA, Otto CM, Bonow RO, Carabello BA, Erwin JP 3rd, Guyton RA, O'Gara PT, Ruiz CE, Skubas NJ, Sorajja P, Sundt TM 3rd, Thomas JD (2014) 2014 AHA/ACC guideline for the management of patients with valvular heart disease: executive summary: a report of the American College of Cardiology/American Heart Association Task Force on Practice Guidelines. Circulation 129(23):2440–2492. https://doi.org/10.1161/cir.0000000000000029
Rose MJ, Rigsby CK, Berhane H, Bollache E, Jarvis K, Barker AJ, Schnell S, Allen BD, Robinson JD, Markl M (2018) 4-D flow MRI aortic 3-D hemodynamics and wall shear stress remain stable over short-term follow-up in pediatric and young adult patients with bicuspid aortic valve. Pediatr Radiol. https://doi.org/10.1007/s00247-018-4257-y
Potters WV, van Ooij P, Marquering H, vanBavel E, Nederveen AJ (2015) Volumetric arterial wall shear stress calculation based on cine phase contrast MRI. J Magn Reson Imaging 41(2):505–516. https://doi.org/10.1002/jmri.24560
van Ooij P, Powell AL, Potters WV, Carr JC, Markl M, Barker AJ (2016) Reproducibility and interobserver variability of systolic blood flow velocity and 3D wall shear stress derived from 4D flow MRI in the healthy aorta. J Magn Reson Imaging 43(1):236–248. https://doi.org/10.1002/jmri.24959
Barker AJ, Markl M, Burk J, Lorenz R, Bock J, Bauer S, Schulz-Menger J, von Knobelsdorff-Brenkenhoff F (2012) Bicuspid aortic valve is associated with altered wall shear stress in the ascending aorta. Circ Cardiovasc Imaging 5(4):457–466. https://doi.org/10.1161/circimaging.112.973370
Al Musa T, Uddin A, Swoboda PP, Garg P, Fairbairn TA, Dobson LE, Steadman CD, Singh A, Erhayiem B, Plein S, McCann GP, Greenwood JP (2017) Myocardial strain and symptom severity in severe aortic stenosis: insights from cardiovascular magnetic resonance. Quant Imaging Med Surg 7(1):38–47. https://doi.org/10.21037/qims.2017.02.05
Nucifora G, Miller J, Gillebert C, Shah R, Perry R, Raven C, Joseph MX, Selvanayagam JB (2018) Ascending aorta and myocardial mechanics in patients with "clinically normal" bicuspid aortic valve. Int Heart J 59(4):741–749. https://doi.org/10.1536/ihj.17-230
Dogan V, Ocal B, Orun UA, Ozgur S, Yilmaz O, Keskin M, Ceylan O, Karademir S, Senocak F (2013) Strain and strain rate echocardiography findings in children with asymptomatic congenital aortic stenosis. Pediatr Cardiol 34(5):1152–1158. https://doi.org/10.1007/s00246-012-0619-7
Dusenbery SM, Lunze FI, Jerosch-Herold M, Geva T, Newburger JW, Colan SD, Powell AJ (2015) Left ventricular strain and myocardial fibrosis in congenital aortic stenosis. Am J Cardiol 116(8):1257–1262. https://doi.org/10.1016/j.amjcard.2015.07.042
Stefani L, De Luca A, Maffulli N, Mercuri R, Innocenti G, Suliman I, Toncelli L, Vono MC, Cappelli B, Pedri S, Pedrizzetti G, Galanti G (2009) Speckle tracking for left ventricle performance in young athletes with bicuspid aortic valve and mild aortic regurgitation. Eur J Echocardiogr 10(4):527–531. https://doi.org/10.1093/ejechocard/jen332
Ng AC, Delgado V, Bertini M, Antoni ML, van Bommel RJ, van Rijnsoever EP, van der Kley F, Ewe SH, Witkowski T, Auger D, Nucifora G, Schuijf JD, Poldermans D, Leung DY, Schalij MJ, Bax JJ (2011) Alterations in multidirectional myocardial functions in patients with aortic stenosis and preserved ejection fraction: a two-dimensional speckle tracking analysis. Eur Heart J 32(12):1542–1550. https://doi.org/10.1093/eurheartj/ehr084
Yamauchi MSW, Puchalski MD, Weng HT, Pinto NM, Etheridge SP, Presson AP, Tani LY, Minich LL, Williams RV (2018) Disease progression and variation in clinical practice for isolated bicuspid aortic valve in children. Congenit Heart Dis 13(3):432–439. https://doi.org/10.1111/chd.12591
Hochstrasser L, Ruchat P, Sekarski N, Hurni M, von Segesser LK (2015) Long-term outcome of congenital aortic valve stenosis: predictors of reintervention. Cardiol Young 25(5):893–902. https://doi.org/10.1017/s1047951114001085
Egbe AC, Luis SA, Padang R, Warnes CA (2016) Outcomes in moderate mixed aortic valve disease: is it time for a paradigm shift? J Am Coll Cardiol 67(20):2321–2329. https://doi.org/10.1016/j.jacc.2016.03.509
Hill AC, Brown DW, Colan SD, Gauvreau K, del Nido PJ, Lock JE, Rathod RH (2014) Mixed aortic valve disease in the young: initial observations. Pediatr Cardiol 35(6):934–942. https://doi.org/10.1007/s00246-014-0878-6
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflicts of interest
The authors of this manuscript have no relevant conflicts of interest.
Ethical Approval
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki Declaration and its later amendments or comparable ethical standards.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Stefek, H.A., Berhane, H., Robinson, J.D. et al. Comprehensive MR Analysis of Cardiac Function, Aortic Hemodynamics and Left Ventricular Strain in Pediatric Cohort with Isolated Bicuspid Aortic Valve. Pediatr Cardiol 40, 1450–1459 (2019). https://doi.org/10.1007/s00246-019-02157-5
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00246-019-02157-5