Abstract
Background
Considering the increasing acknowledgment of the human sense of smell as a significant component of the quality of life, olfactory drug effects gain potential clinical importance. A recent observation in a human experimental context indicated that Δ9-tetrahydrocannabinol (THC) impaired the subject’s performance in olfactory tests. To further analyze the role of THC in human olfaction, the present report addresses its effects on the central processing of olfactory stimuli.
Methods
Employing a placebo-controlled randomized crossover design, an oral dose of 20 mg THC was administered in 15 healthy volunteers. The central processing of olfactory input, consisting of short pulses of gaseous vanillin or hydrogen sulfide, and for comparison, of non-odorous but painful carbon dioxide, were investigated before and after administration of THC or placebo in a pharmacological functional magnet resonance imaging study.
Results
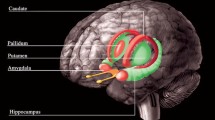
Following THC administration, the vanillin stimuli lost their pleasantness and became hedonically inert. This observation had its functional correlate in reduced stimulus-associated brain activations located in the left amygdala, the hippocampus and superior temporal pole (peak MNI coordinates x = − 27, y = − 1, z = − 26 mm p = 0.039). Differences in amygdala activations were significantly correlated with the corresponding differences in vanillin pleasantness (p = 0.025). By contrast, no effects were observed on the perception of processing of H2S stimuli.
Conclusions
The results support that THC induced a modulation of the central processing of olfactory input. The THC-induced reduction in the pleasantness of a pleasurable odor was accompanied by reduced activations in the limbic system. Results agree with previous observation of negative effects of cannabinoids on the human sense of smell and strengthen the evidence that THC-based medications will be among drugs with olfactory side effects.


Similar content being viewed by others
References
Damm M, Temmel A, Welge-Lüssen A, Eckel HE, Kreft MP, Klussmann JP et al (2004) Epidemiologie und Therapie von Riechstörungen in Deutschland, Österreich und der Schweiz. HNO 52:112–120
Hummel T, Nordin S (2005) Olfactory disorders and their consequences for quality of life. Acta Otolaryngol 125(2):116–121
Rinaldi A (2007) The scent of life. The exquisite complexity of the sense of smell in animals and humans. EMBO Rep 8(7):629–633
Croy I, Nordin S, Hummel T (2014) Olfactory disorders and quality of life--an updated review. Chem Senses 39(3):185–194
Birkett D, Brosen K, Cascorbi I, Gustafsson LL, Maxwell S, Rago L et al (2010) Clinical pharmacology in research, teaching and health care: considerations by IUPHAR, the International Union of Basic and Clinical Pharmacology. Basic Clin Pharmacol Toxicol 107(1):531–559
Lötsch J, Geisslinger G, Hummel T (2012) Sniffing out pharmacology: interactions of drugs with human olfaction. Trends Pharmacol Sci 33(4):193–199
Walter C, Oertel BG, Ludyga D, Ultsch A, Hummel T, Lotsch J (2014) Effects of 20 mg oral Delta(9) -tetrahydrocannabinol on the olfactory function of healthy volunteers. Br J Clin Pharmacol 78(5):961–969
Green B, Kavanagh D, Young R (2003) Being stoned: a review of self-reported cannabis effects. Drug Alcohol Rev 22(4):453–460
Guindon J, Hohmann AG (2009) The endocannabinoid system and pain. CNS Neurol Disorders Drug. Targets 8(6):403–421
Breunig E, Manzini I, Piscitelli F, Gutermann B, Di Marzo V, Schild D et al (2010) The endocannabinoid 2-arachidonoyl-glycerol controls odor sensitivity in larvae of Xenopus laevis. J Neurosci 30(26):8965–8973
Katona I, Rancz EA, Acsady L, Ledent C, Mackie K, Hajos N et al (2001) Distribution of CB1 cannabinoid receptors in the amygdala and their role in the control of GABAergic transmission. J Neurosci 21(23):9506–9518
Walter C, Oertel BG, Felden L, Kell CA, Noth U, Vermehren J et al (2016) Brain mapping-based model of Delta(9)-tetrahydrocannabinol effects on connectivity in the pain matrix. Neuropsychopharmacology 41(6):1659–1669
Farrell M, Ritson B (2001) Cannabis and health. Br J Psychiatry 178:98
Ware MA, Wang T, Shapiro S, Collet JP (2015) Cannabis for the management of pain: assessment of safety study (COMPASS). J Pain 16(12):1233–1242
Zajicek JP, Hobart JC, Slade A, Barnes D, Mattison PG (2012) Multiple sclerosis and extract of cannabis: results of the MUSEC trial. J Neurol Neurosurg Psychiatry 83(11):1125–1132
Miwa T, Furukawa M, Tsukatani T, Costanzo RM, DiNardo LJ, Reiter ER (2001) Impact of olfactory impairment on quality of life and disability. Arch Otolaryngol Head Neck Surg. 127:497–503
Roberts JD, Gennings C, Shih M (2006) Synergistic affective analgesic interaction between delta-9-tetrahydrocannabinol and morphine. Eur J Pharmacol 530(1–2):54–58
Naef M, Curatolo M, Petersen-Felix S, Arendt-Nielsen L, Zbinden A, Brenneisen R (2003) The analgesic effect of oral delta-9-tetrahydrocannabinol (THC), morphine, and a THC-morphine combination in healthy subjects under experimental pain conditions. Pain 105(1–2):79–88
Lee MC, Ploner M, Wiech K, Bingel U, Wanigasekera V, Brooks J et al (2013) Amygdala activity contributes to the dissociative effect of cannabis on pain perception. Pain 154(1):124–134
Desmond JE, Glover GH (2002) Estimating sample size in functional MRI (fMRI) neuroimaging studies: statistical power analyses. J Neurosci Methods 118(2):115–128
Kobal G, Hummel T, Sekinger B, Barz S, Roscher S, Wolf SR (1996) “Sniffin’ sticks”: screening of olfactory performance. Rhinology 34:222–226
Hummel T, Kobal G, Gudziol H, Mackay-Sim A (2007) Normative data for the “Sniffin’ sticks” including tests of odor identification, odor discrimination, and olfactory thresholds: an upgrade based on a group of more than 3,000 subjects. Eur Arch Otorhinolaryngol 264(3):237–243
Hollister LE, Gillespie HK, Ohlsson A, Lindgren JE, Wahlen A, Agurell S (1981) Do plasma concentrations of delta 9-tetrahydrocannabinol reflect the degree of intoxication? J Clin Pharmacol 21(8–9 Suppl):171S–177S
Walter C, Ferreiros N, Bishay P, Geisslinger G, Tegeder I, Lötsch J (2013) Exogenous delta(9)-tetrahydrocannabinol influences circulating endogenous cannabinoids in humans. J Clin Psychopharmacol 33(5):699–705
Walter C, Oertel BG, Felden L, Noth U, Deichmann R, Lötsch J (2011) The effects of delta-9-tetrahydrocannabinol on nasal chemosensitivity: a pharmacological fMRI study in healthy volunteers. Naunyn Schmiedeberg's Arch Pharmacol 383(Suppl 1):75
Lötsch J, Walter C, Nöth U, Deichmann R, Oertel BG. (2013) Delta-9-tetrahydrocannabinol impedes pain memory: a pharmacological fMRI study in humans. Naunyn-Schmiedebergs Arch Pharmacol;386, Abstract 194(Suppl 1):48
Kobal G, Hummel T (1998) Olfactory and intranasal trigeminal event-related potentials in anosmic patients. Laryngoscope 108(7):1033–1035
Doty RL, Brugger WPE, Jurs PC, Orndorff MA, Snyder PJ, Lowry LD (1978) Intranasal trigeminal stimulation from odorous volatiles: psychometric responses from anosmic and normal humans. Physiol Behav 20:175–185
Kobal G (1981) Elektrophysiologische Untersuchungen des menschlichen Geruchsinnes. Thieme-Verlag, Stuttgart
Walter C, Oertel BG, Lötsch J (2015) THC may reproducibly induce electrical hyperalgesia in healthy volunteers. Eur J Pain 19(4):516–518
Kobal G (1985) Pain-related electrical potentials of the human nasal mucosa elicited by chemical stimulation. Pain 22(2):151–163
Kobal G, Hummel C, Nuernberg B, Brune K (1990) Effects of pentazocine and acetylsalicylic acid on pain-rating, pain-related evoked potentials and vigilance in relationship to pharmacokinetic parameters. Agents Actions 29:342–359
Kobal G, Hummel T (1990) Brain responses to chemical stimulation of the trigeminal nerve in man. In: Green BGMJ, Kare MR (eds) Irritation. Chemical senses, vol 2. Marcel Dekker, New York, pp 123–136
Hummel T, Livermore A, Hummel C, Kobal G (1992) Chemosensory event-related potentials: relation to olfactory and painful sensations elicited by nicotine. Electroencephalogr Clin Neurophysiol 84:192–195
Hummel T, Rothbauer C, Pauli E, Kobal G (1998) Effects of the nasal decongestant oxymetazoline on human olfactory and intranasal trigeminal function in acute rhinitis. Eur J Clin Pharmacol 54(7):521–528
Grosser K, Oelkers R, Hummel T, Geisslinger G, Brune K, Kobal G et al (2000) Olfactory and trigeminal event-related potentials in migraine. Cephalalgia 20(7):621–631
Hummel T, Gruber M, Pauli E, Kobal G (1994) Chemo-somatosensory event-related potentials in response to repetitive painful chemical stimulation of the nasal mucosa. Electroencephalogr Clin Neurophysiol 92:426–432
Bonferroni CE (1936) Teoria statistica delle classi e calcolo delle probabilita. Pubblicazioni del R Istituto Superiore di Scienze Economiche e Commerciali di Firenze;8:3–62
Andersson JL, Hutton C, Ashburner J, Turner R, Friston K (2001) Modeling geometric deformations in EPI time series. NeuroImage 13(5):903–919
Hutton C, Bork A, Josephs O, Deichmann R, Ashburner J, Turner R (2002) Image distortion correction in fMRI: a quantitative evaluation. NeuroImage 16(1):217–240
Mugler JP 3rd, Brookeman JR (1991) Rapid three-dimensional T1-weighted MR imaging with the MP-RAGE sequence. J Magn Reson Imaging 1(5):561–567
Griswold MA, Jakob PM, Heidemann RM, Nittka M, Jellus V, Wang J et al (2002) Generalized autocalibrating partially parallel acquisitions (GRAPPA). Magn Reson Med 47(6):1202–1210
Friston KJ, Holmes AP, Poline JB, Grasby PJ, Williams SC, Frackowiak RS et al (1995) Analysis of fMRI time-series revisited. NeuroImage 2(1):45–53
Worsley KJ, Friston KJ (1995) Analysis of fMRI time-series revisited—again. NeuroImage 2(3):173–181
Maldjian JA, Laurienti PJ, Kraft RA, Burdette JH (2003) An automated method for neuroanatomic and cytoarchitectonic atlas-based interrogation of fMRI data sets. NeuroImage 19(3):1233–1239
Lotsch J, Hahner A, Gossrau G, Hummel C, Walter C, Ultsch A et al (2016) Smell of pain: intersection of nociception and olfaction. Pain 157(10):2152–2157
Gläscher J (2009) Visualization of group inference data in functional neuroimaging. Neuroinformatics 7(1):73–82
Kendall MG (1938) A new measure of rank correlation. Biometrika 30(1–2):81–93
Eickhoff SB, Stephan KE, Mohlberg H, Grefkes C, Fink GR, Amunts K et al (2005) A new SPM toolbox for combining probabilistic cytoarchitectonic maps and functional imaging data. NeuroImage 25(4):1325–1335
R Development Core Team (2008) R: A language and environment for statistical computing. Vienna, Austria
Czesnik D, Schild D, Kuduz J, Manzini I (2007) Cannabinoid action in the olfactory epithelium. Proc Natl Acad Sci U S A 104(8):2967–2972
McPartland JM, Glass M, Pertwee RG (2007) Meta-analysis of cannabinoid ligand binding affinity and receptor distribution: interspecies differences. Br J Pharmacol 152(5):583–593
Sridharan D, Levitin DJ, Menon V (2008) A critical role for the right fronto-insular cortex in switching between central-executive and default-mode networks. Proc Natl Acad Sci U S A 105(34):12569–12574
Eckert MA, Menon V, Walczak A, Ahlstrom J, Denslow S, Horwitz A et al (2009) At the heart of the ventral attention system: the right anterior insula. Hum Brain Mapp 30(8):2530–2541
Seeley WW, Menon V, Schatzberg AF, Keller J, Glover GH, Kenna H et al (2007) Dissociable intrinsic connectivity networks for salience processing and executive control. J Neurosci 27(9):2349–2356
Noyes R Jr, Brunk SF, Avery DA, Canter AC (1975) The analgesic properties of delta-9-tetrahydrocannabinol and codeine. Clin Pharmacol Ther 18(1):84–89
Ohlsson A, Lindgren JE, Wahlen A, Agurell S, Hollister LE, Gillespie HK (1980) Plasma delta-9 tetrahydrocannabinol concentrations and clinical effects after oral and intravenous administration and smoking. Clin Pharmacol Ther 28(3):409–416
Walter C, Ferreiros N, Bishay P, Geisslinger G, Tegeder I, Lotsch J (2013) Exogenous Delta9-tetrahydrocannabinol influences circulating endogenous cannabinoids in humans. J Clin Psychopharmacol 33(5):699–705. https://10.1097/JCP.0b013e3182984015
Solvay Pharmaceuticals. Summary of Product Characteristics Marinol (2004) Available https://www.fda.gov/ohrms/dockets/dockets/05n0479/05N-0479-emc0004-04.pdf. Accessed Aug 2017
Nail RL, Gunderson EK, Kolb D (1974) Motives for drug use among light and heavy users. J Nerv Ment Dis 159(2):131–136
Haines L, Green W (1970) Marijuana use patterns. The British journal of addiction to alcohol and other drugs 65(4):347–362
Mattes RD, Shaw LM, Engelman K (1994) Effects of cannabinoids (marijuana) on taste intensity and hedonic ratings and salivary flow of adults. Chem Senses 19(2):125–140
Cowan J, Neidert G, Miller L (1982) Marijuana and memory for feelings. Prog Neuro-Psychopharmacol Biol Psychiatry 6(1):63–73
Schlicker E, Kathmann M (2001) Modulation of transmitter release via presynaptic cannabinoid receptors. Trends Pharmacol Sci 22(11):565–572
Rubino T, Parolaro D (2011) Sexually dimorphic effects of cannabinoid compounds on emotion and cognition. Front Behav Neurosci 5:64
Viveros MP, Marco EM, Lopez-Gallardo M, Garcia-Segura LM, Wagner EJ (2011) Framework for sex differences in adolescent neurobiology: a focus on cannabinoids. Neurosci Biobehav Rev 35(8):1740–1751
Gonzalez S, Bisogno T, Wenger T, Manzanares J, Milone A, Berrendero F et al (2000) Sex steroid influence on cannabinoid CB(1) receptor mRNA and endocannabinoid levels in the anterior pituitary gland. Biochem Biophys Res Commun 270(1):260–266
Ben-Zvi Z, Mechoulam R, Edery H, Porath G (1971) 6-hydroxy-1-tetrahydrocannabinol synthesis and biological activity. Science 174(12):951–952
Kearn CS, Greenberg MJ, DiCamelli R, Kurzawa K, Hillard CJ (1999) Relationships between ligand affinities for the cerebellar cannabinoid receptor CB1 and the induction of GDP/GTP exchange. J Neurochem 72(6):2379–2387
Tseng AH, Harding JW, Craft RM (2004) Pharmacokinetic factors in sex differences in Delta 9-tetrahydrocannabinol-induced behavioral effects in rats. Behav Brain Res 154(1):77–83
Narimatsu S, Watanabe K, Yamamoto I, Yoshimura H (1991) Sex difference in the oxidative metabolism of delta 9-tetrahydrocannabinol in the rat. Biochem Pharmacol 41(8):1187–1194
Doty RL, Cameron EL (2009) Sex differences and reproductive hormone influences on human odor perception. Physiol Behav 25;97(2):213–28. https://10.1016/j.physbeh.2009.02.032
Hummel T, Lötsch J (2010) Prognostic factors of olfactory dysfunction. Arch Otolaryngol Head Neck Surg 136(4):347–351
Lötsch J, Knothe C, Lippmann C, Ultsch A, Hummel T, Walter C (2015) Olfactory drug effects approached from human-derived data. Drug Discov Today 20(11):1398–1406
Doty RL, Bromley SM (2004) Effects of drugs on olfaction and taste. Otolaryngol Clin N Am 37(6):1229–1254
Hill MN, Patel S, Campolongo P, Tasker JG, Wotjak CT, Bains JS (2010) Functional interactions between stress and the endocannabinoid system: from synaptic signaling to behavioral output. J Neurosci 30(45):14980–14986
Kraft B (2012) Is there any clinically relevant cannabinoid-induced analgesia? Pharmacology 89(5–6):237–246
Acknowledgements
Parts of this complex project have been reported separately with other focus and in a non-redundant manner in J Clin Psychopharmacol 33(5): 699-705, Neuropsychopharmacology 41(6): 1659-1669, Eur J Pain 19(4): 516-518, and Br J Clin Pharmacol 78(5): 961-969.
Funding
This work has been funded by the Deutsche Forschungsgemeinschaft, DFG Lo 612/10-1 (JL), European Graduate School GRK757 (JL), and the Bundesministerium für Bildung und Forschung (Brain Imaging Center Frankfurt, DLR 01GO0203, RD). The funders had no role in study design, data collection and analysis, decision to publish, or preparation of the manuscript.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflicts of interest.
Rights and permissions
About this article
Cite this article
Walter, C., Oertel, B.G., Felden, L. et al. Effects of oral Δ9-tetrahydrocannabinol on the cerebral processing of olfactory input in healthy non-addicted subjects. Eur J Clin Pharmacol 73, 1579–1587 (2017). https://doi.org/10.1007/s00228-017-2331-2
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00228-017-2331-2