Abstract
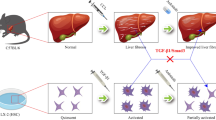
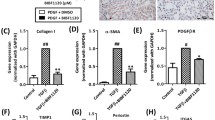
Tyrosine kinase inhibitors have been emerged recently as an effective therapy against liver fibrosis. The current study was designed to test a potential anti-fibrotic effect of the multi-targeted receptor tyrosine kinase inhibitor pazopanib. Carbon tetrachloride (CCl4; 1 mL/kg) was injected intraperitoneally (i.p.) twice/week for 8 weeks. Pazopanib (10 and 30 mg/kg, i.p.) was administered three times/week at the beginning of week 5. Levels of liver function biomarkers (alanine aminotransferase (ALT), aspartate aminotransferase (AST), albumin, and total bilirubin), malondialdehyde, transforming growth factor-β1 (TGF-β1), caspase-3, factor-related apoptosis (FAS), vascular endothelial growth factor (VEGF) receptor-1, and pigment endothelial derived factor (PEDF) were measured. The tissue level of the inflammatory cytokines IL-6 and tumor necrosis factor-α (TNF-α) were assigned. Fibrotic area was measured by morphometry and expression of alpha-smooth muscle actin (α-SMA), caspase-3, platelet-derived growth factor (PDGF) receptor-β, and matrix metalloproteinase-2 (MMP-2) was scored immunohistochemically. Hepatic expression of collagen-1-alpha-1 (Col1A1) and tissue inhibitor metalloproteinase-1 (TIMP-1) mRNA were assigned by RT-qPCR. Injection of CCl4 resulted in marked collagen deposition, necroinflammation, and fibrosis (2.67 %). Pazopanib in a dose of 30 mg/kg improved liver function, reduced fibrosis (1.48 %), and decreased significantly (P < 0.01) liver expression of malondialdehyde, TGF-β1, IL-6, TNF-α, Col1A1, TIMP-1, α-SMA, MMP-2, PDGF receptor-β, and VEGF receptor-1. Additionally, the apoptotic markers (caspase-3, FAS) and the anti-angiogenic factor PEDF were upregulated significantly (P < 0.05). Pazopanib at a certain dose level can halt liver fibrosis progression through modulating inflammatory cytokines, suppressing stellate cell activity, inducing apoptosis, and potentially regulating angiogenesis.






Similar content being viewed by others
References
Ankoma-Sey V, Wang Y, Dai Z (2000) Hypoxic stimulation of vascular endothelial growth factor expression in activated rat hepatic stellate cells. Hepatology 31:141–148. doi:10.1002/hep.510310122
Bataller R, Brenner DA (2005) Liver fibrosis. J Clin Invest 115:209–218. doi:10.1172/JCI200524282
Benyon RC, Arthur MJ (2001) Extracellular matrix degradation and the role of hepatic stellate cells. Semin Liver Dis 21:373–384. doi:10.1055/s-2001-17552
Beyer C, Distler HW (2013) Tyrosine kinase signaling in fibrotic disorders: translation of basic research to human disease. Biochim Biophys Acta 1832:897–904. doi:10.1016/j.bbadis.2012.06.008
Brenner DA, Kisseleva T, Scholten D, Paik YH, Iwaisako K, Inokuchi S, et al. (2012) Origin of myofibroblasts in liver fibrosis. Fibrogenesis Tissue Repair 5(Suppl. 1):S17. doi:10.1186/1755-1536-5-S1-S17
Cai J, Jiang WG, Grant MB, Boulton M (2006) Pigment epithelium-derived factor inhibits angiogenesis via regulated intracellular proteolysis of vascular endothelial growth factor receptor 1. J Biol Chem 281:3604–3613
Chakraborty JB, Oakley F, Walsh MJ (2012) Mechanisms and biomarkers of apoptosis in liver disease and fibrosis. Int J Hepatol 2012:648915. doi:10.1155/2012/648915
Consolo M, Amoroso A, Spandidos DA, Mazzarino MC (2009) Matrix metalloproteinases and their inhibitors as markers of inflammation and fibrosis in chronic liver disease (review). Int J Mol Med 24:143–152. doi:10.3892/ijmm_00000217
Corpechot C, Barbu V, Wendum D, Kinnman N, Rey C, Poupon R, et al. (2002) Hypoxia-induced VEGF and collagen I expressions are associated with angiogenesis and fibrogenesis in experimental cirrhosis. Hepatology 35:1010–1021. doi:10.1053/jhep.2002.32524
Coward WR, Saini G, Jenkins G (2010) The pathogenesis of idiopathic pulmonary fibrosis. Ther Adv Respir Dis 4:367–388. doi:10.1177/1753465810379801
Dawson DW, Volpert OV, Gillis P, Crawford SE, Xu HJ, Benedict W, et al. (1999) Pigment epithelium-derived factor: a potent inhibitor of angiogenesis. Science 285:245–248
Desmet VJ, Roskams T (2004) Cirrhosis reversal: a duel between dogma and myth. J Hepatol 40:860–867
Elsharkawy AM, Oakley F, Mann DA (2005) The role and regulation of hepatic stellate cell apoptosis in reversal of liver fibrosis. Apoptosis 10:927–939. doi:10.1007/s10495-005-1055-4
Fausther M, Lavoie EG, Dranoff JA (2013) Contribution of myofibroblasts of different origins to liver fibrosis. Curr Pathobiol Rep 1:225–230. doi:10.1007/s40139-013-0020-0
Ferrara N (2001) Role of vascular endothelial growth factor in regulation of physiological angiogenesis. Am J Physiol-Cell Physiol 280:C1358–C1366
Friedman SL (2008) Mechanisms of hepatic fibrogenesis. Gastroenterology 134:1655–1669. doi:10.1053/j.gastro.2008.03.003
Gaça MD, Zhou X, Issa R, Kiriella K, Iredale JP, Benyon RC (2003) Basement membrane-like matrix inhibits proliferation and collagen synthesis by activated rat hepatic stellate cells: evidence for matrix-dependent deactivation of stellate cells. Matrix Biol 22:229–239. doi:10.1016/S0945-053X(03)00017-9
Gao G, Li Y, Gee S, Dudley A, Fant J, Crosson C, et al. (2002) Down-regulation of vascular endothelial growth factor and up-regulation of pigment epithelium-derived factor: a possible mechanism for the anti-angiogenic activity of plasminogen kringle 5. J Biol Chem 277:9492–9497
Gérard-Monnier D, Erdelmeier I, Régnard K, Moze-Henry N, Yadan JC, Chaudière J (1998) Reactions of 1-methyl-2-phenylindole with malondialdehyde and 4-hydroxyalkenals. Analytical applications to a colorimetric assay of lipid peroxidation. Chem Res Toxicol 11:1176-1183. doi: 10.1021/tx9701790
Gieling RG, Burt AD, Mann DA (2008) Fibrosis and cirrhosis reversibility—molecular mechanisms. Clin Liver Dis 12:915–937. doi:10.1016/j.cld.2008.07.001
Hamberg P, Verweij J, Sleijfer S (2010) (Pre-) clinical pharmacology and activity of pazopanib, a novel multikinase angiogenesis inhibitor. The oncologist 15:539–547. doi:10.1634/theoncologist.2009-0274
Harris PA, Boloor A, Cheung M, Kumar R, Crosby RM, Davis-Ward RG, et al. (2008) Discovery of 5-[[4-[(2,3-dimethyl-2H-indazol-6-yl) methylamino]-2-pyrimidinyl]amino]-2-methyl-benzenesulfonamide (pazopanib), a novel and potent vascular endothelial growth factor receptor inhibitor. J Med Chem 51:4632–4640. doi:10.1021/jm800566m
Hemmann S, Graf J, Roderfeld M, Roeb E (2007) Expression of MMPs and TIMPs in liver fibrosis—a systematic review with special emphasis on anti-fibrotic strategies. J Hepatol 46:955–975. doi:10.1016/j.jhep.2007.02.003
Iredale JP (2001) Hepatic stellate cell behavior during resolution of liver injury. Semin. Liver Dis. 21:427–436. doi:10.1055/s-2001-17557
Ishak K, Baptista A, Bianchi L, Callea F, De Groote J, Gudat F, et al. (1995) Histological grading and staging of chronic hepatitis. J Hepatol 22:696–699. doi:10.1016/0168-8278(95)80226-6
James J, Bosch KS, Aronson DC, Houtkooper JM (1990) Sirius red histophotometry and spectrophotometry of sections in the assessment of the collagen content of liver tissue and its application in growing rat liver. Liver 10:1–5. doi:10.1111/j.1600-0676.1990.tb00428.x
Juliachs M, Vidal A, del Muro XG, Piulats JM, Condom E, Casanovas O, et al. (2013) Effectivity of pazopanib treatment in orthotopic models of human testicular germ cell tumors. BMC Cancer. 13:382. doi:10.1186/1471-2407-13-382
Kawada N (2006) Human hepatic stellate cells are resistant to apoptosis: implications for human fibrogenic liver disease. Gut 55:1073–1074. doi:10.1136/gut.2005.090449
Levitzki A (2004) PDGF receptor kinase inhibitors for the treatment of PDGF driven diseases. Cytokine Growth Factor Rev 15:229–235. doi:10.1016/j.cytogfr.2004.03.010
Liu Y, Wang Z, Kwong SQ, Lui ELH, Friedman SL, Li FR, et al. (2011) Inhibition of PDGF, TGF-β, and Abl signaling and reduction of liver fibrosis by the small molecule Bcr-Abl tyrosine kinase antagonist nilotinib. J. Hepatol. 55:612–625. doi:10.1016/j.jhep.2010.11.035
Majumder S, Piguet AC, Dufour JF, Chatterjee S (2013) Study of the cellular mechanism of sunitinib mediated inactivation of activated hepatic stellate cells and its implications in angiogenesis. Eur J Parmacol 705:86–95
Matsumoto T, Claesson-Welsh L (2001) VEGF receptor signal transduction. Sci STKE 2001:re21. doi:10.1126/stke.2001.112.re21
Matsumoto K. Ishikawa H, Nishimura D, Hamasaki K, Nakao K, Eguchi K (2004) Antiangiogenic property of pigment epithelium-derived factor in hepatocellular carcinoma. Hepatology 40: 252-259. doi:10.1002/hep.20259
McPartland JL, Guzail MA, Kendall CH, Pringle JH (2005) Apoptosis in chronic viral hepatitis parallels histological activity: an immunohistochemical investigation using anti-activated caspase-3 and M30 cytodeath antibody. Int J Exp Pathl 86:19–24
Novo E, Marra F, Zamara E, Di Bonzo LV, Monitillo L, Cannito S, et al. (2006) Overexpression of Bcl-2 by activated human hepatic stellate cells: resistance to apoptosis as a mechanism of progressive hepatic fibrogenesis in humans. Gut 55:1174–1182. doi:10.1136/gut.2005.082701
Nyberg P, Xie L, Kalluri R (2005) Endogenous inhibitors of angiogenesis. Cancer Res 65:3967–3979
Paternostro C, David E, Novo E, Parola M (2010) Hypoxia, angiogenesis and liver fibrogenesis in the progression of chronic liver diseases. World J Gastroenterol 16:281–288. doi:10.3748/wjg.v16.i3.281
Pellicoro A, Ramachandran P, Iredale JP, Fallowfield JA (2014) Liver fibrosis and repair: immune regulation of wound healing in a solid organ. Nat Rev Immunol 14:181–194. doi:10.1038/nri3623
Pfaffl MW (2001) A new mathematical model for relative quantification in real-time RT–PCR. Nucleic Acids Res 29:e45. doi:10.1093/nar/29.9.e45
Podar K, Tonon G, Sattler M, Tai YT, LeGouill S, Yasui H, et al. (2006) The small-molecule VEGF receptor inhibitor pazopanib (GW786034B) targets both tumor and endothelial cells in multiple myeloma. Proc Natl Acad Sci USA 103:19478–19483. doi:10.1073/pnas.0609329103
Préaux AM, Mallat A, Van Nhieu JT, d’Ortho MP, Hembry RM, Mavier P (1999) Matrix metalloproteinase-2 activation in human hepatic fibrosis regulation by cell-matrix interactions. Hepatology 30:944–950. doi:10.1002/hep.510300432
Rosmorduc O, Housset C (2010) Hypoxia: a link between fibrogenesis, angiogenesis, and carcinogenesis in liver disease. Semin Liver Dis 30:258–270. doi:10.1055/s-0030-1255355
Shiha GE, Abu-Elsaad NM, Zalata KR, Ibrahim TM (2014) Tracking anti-fibrotic pathways of nilotinib and imatinib in experimentally induced liver fibrosis: an insight. Clin Exp Pharm Physiol 41:788–797. doi:10.1111/1440-1681.12286
Tang X, Yang J, Li J (2009) Accelerative effect of leflunomide on recovery from hepatic fibrosis involves TRAIL-mediated hepatic stellate cell apoptosis. Life Sci 84:552–557. doi:10.1016/j.lfs.2009.01.017
Taura K, De Minicis S, Seki E, Hatano E, Iwaisako K, Osterreicher CH, et al. (2008) Hepatic stellate cells secrete angiopoietin 1 that induces angiogenesis in liver fibrosis. Gastroenterology 135:1729–1738. doi:10.1053/j.gastro.2008.07.065
Thabut D, Routray C, Lomberk G, Shergill U, Glaser K, Huebert R, et al. (2011) Complementary vascular and matrix regulatory pathways underlie the beneficial mechanism of action of sorafenib in liver fibrosis. Hepatology 54:573–585
Theodorakis NG, Wang YN, Wu J, Maluccio MA, Sitzmann JV, Skill NJ (2009) Role of endothelial nitric oxide synthase in the development of portal hypertension in the carbon tetrachloride induced liver fibrosis model. Am J Physiol Gastrointest Liver Physiol 297:G792–G799. doi:10.1152/ajpgi.00229.2009
Tsukada BS, Parsons CJ, Rippe RA (2006) Mechanisms of liver fibrosis. Clin. Chim. Acta. 364:33–60. doi:10.1016/j.cca.2005.06.014
Tsukamoto H (2002) Redox regulation of cytokine expression in Kupffer cells. Antioxid Redox Signal 4:741–748. doi:10.1089/152308602760598882
Ushio-Fukai M (2007) VEGF signaling through NADPH oxidase-derived ROS. Antioxid Redox Signal 9:731–739. doi:10.1089/ars.2007.1556
Ushio-Fukai M, Tang Y, Fukai T, Dikalov SI, Ma Y, Fujimoto M, et al. (2002) Novel role of gp91phox-containing NAD(P)H oxidase in vascular endothelial growth factor–induced signaling and angiogenesis. Circ Res 91:1160–1167. doi:10.1161/01.RES.0000046227.65158.F8
Xu J, Liu X, Koyama Y, Wang P, Lan T, Kim IG, et al. (2014) The types of hepatic myofibroblasts contributing to liver fibrosis of different etiologies. Front Pharmacol 5:167. doi:10.3389/fphar.2014.00167
Zhang F, Zhang Z, Chen L, Kong D, Zhang X, Lu C, et al. (2014) Curcumin attenuates angiogenesis in liver fibrosis and inhibits angiogenic properties of hepatic stellate cells. J. Cell. Mol Med 18:1392–1406. doi:10.1111/jcmm.12286
Zhu XD, Zhang JB, Fan PL, Xiong YQ, Zhuang PY, Zhang W, et al. (2011) Antiangiogenic effects of pazopanib in xenograft hepatocellular carcinoma models: evaluation by quantitative contrast-enhanced ultrasonography. BMC Cancer 11:28. doi:10.1186/1471-2407-11-28
Conflict of interest
The authors declare that they have no competing interests.
Ethical approval
Animal care and experimental procedures carried out in the study were in accordance with the ethical guidelines adopted by the Scientific Research Ethics Committee, Faculty of Pharmacy, Mansoura University.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Elshal, M., Abu-Elsaad, N., El-Karef, A. et al. The multi-kinase inhibitor pazopanib targets hepatic stellate cell activation and apoptosis alleviating progression of liver fibrosis. Naunyn-Schmiedeberg's Arch Pharmacol 388, 1293–1304 (2015). https://doi.org/10.1007/s00210-015-1157-7
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00210-015-1157-7