Abstract
Doxorubicin (Dox), an effective therapy in different types of cancer, is known to exhibit cardiotoxic effects. Despite previous studies indicating the benefits of dapagliflozin (DAPA) in patients experiencing heart failure, it remains uncertain whether DAPA exerts a protective effect on Dox-induced cardiac dysfunction. Signal transducer and activator of transcription 3 (STAT3) participates in various mechanisms of cardioprotection. Herein, we aimed to investigate the effects of DAPA on Dox-induced cardiotoxicity and the role of STAT3. Sprague–Dawley rats were pretreated with oral DAPA for 6 weeks followed by Dox for 4 weeks. Sequential echocardiography was applied to assess cardiac function. For in vitro analysis, cardiomyocytes were treated with 10 μM DAPA and subsequently exposed to 1 μM Dox. The expression of reactive oxygen species- and apoptosis-related proteins was measured. Using STAT3 siRNA, we further examined the effects of STAT3 effect on DAPA-associated protection against Dox-induced apoptosis. In rats treated with Dox, DAPA significantly reduced cardiac fibrosis and improved cardiac function and hemodynamics. Additionally, DAPA effectively inhibited Dox-induced apoptosis and reactive oxygen species (ROS) in cardiomyocytes. Mechanistically, we showed that DAPA decreased cardiac expression of Bax and cleaved caspase 3 but increased Bcl-2 expression. DAPA also significantly rescued Dox-suppressed STAT3 expression. Conversely, knocking down STAT3 in cardiomyocytes reversed the DAPA-related protective effects on Dox-induced cell apoptosis and ROS. Collectively, our findings indicate that DAPA could be useful for preventing Dox-induced cardiotoxicity by restoring STAT3.








Similar content being viewed by others
Availability of data and materials
The data are available upon the reasonable request to the corresponding author.
Abbreviations
- Dox:
-
Doxorubicin
- Dapa:
-
Dapagliflozin
- STZ:
-
Streptozotocin
- ER:
-
Endoplasmic reticulum
- ROS:
-
Reactive oxygen species
- SGLT2:
-
Sodium glucose cotransporter
- NHI:
-
National Health Insurance
- NHIRD:
-
National Health Insurance Research Database
- MACCEs:
-
Major adverse cardio- and cerebrovascular events
- CKD:
-
Chronic kidney disease
- ESRD:
-
End-stage renal disease
- COPD:
-
Chronic obstructive pulmonary disease
- IVSd:
-
Interventricular septum thickness in diastole
- LVIDd:
-
Left ventricular internal diameter; in diastole
- EF:
-
Ejection fraction
- FS:
-
Fractional shortening
- P-V:
-
Pressure–volume
- HE:
-
Hematoxylin-eosin
- Ves:
-
End-systolic
- Ved:
-
Diastolic volumes
- Pes:
-
End-systolic
- Ped:
-
Diastolic pressures
- +dP/dt and -dP/dt:
-
Maximal velocity of pressure rise and fall
- Ea:
-
Arterial elastance
- tau:
-
Time constant of isovolumic pressure decay
- ESPVR:
-
End-systolic pressure–volume relationship
- EDPVR:
-
End-diastolic pressure–volume relationship
- IVC:
-
Inferior vena cava
- MTT:
-
3-(4,5-Dimethyl-2-thiazolyl)-2,5-dimethyl-2H-tetrazolium bromide
- H2DCF‑DA:
-
Fluorescent 2′,7′‑dichlorofluorescindiacetate
- PI:
-
Propidium iodide
- TUNEL:
-
Terminal deoxynucleotidyl transferase-mediated dUTP nick end labeling
References
Bertero E, Prates Roma L, Ameri P, Maack C (2018) Cardiac effects of SGLT2 inhibitors: the sodium hypothesis. Cardiovasc Res 114(1):12–18. https://doi.org/10.1093/cvr/cvx149
Chang WT, Lin YW, Ho CH, Chen ZC, Liu PY, Shih JY (2021) Dapagliflozin suppresses ER stress and protects doxorubicin-induced cardiotoxicity in breast cancer patients. Arch Toxicol 95(2):659–671. https://doi.org/10.1007/s00204-020-02951-8
Chazaud B, Mouchiroud G (2014) Inflamm-aging: STAT3 signaling pushes muscle stem cells off balance. Cell Stem Cell 15(4):401–402. https://doi.org/10.1016/j.stem.2014.09.010
Chen SH, Murphy DA, Lassoued W, Thurston G, Feldman MD, Lee WM (2008) Activated STAT3 is a mediator and biomarker of VEGF endothelial activation. Cancer Biol Ther 7(12):1994–2003. https://doi.org/10.4161/cbt.7.12.6967
Frias MA, Somers S, Gerber-Wicht C, Opie LH, Lecour S, Lang U (2008) The PGE2-Stat3 interaction in doxorubicin-induced myocardial apoptosis. Cardiovasc Res 80(1):69–77. https://doi.org/10.1093/cvr/cvn171
Fu HY, Sanada S, Matsuzaki T et al (2016) Chemical endoplasmic reticulum chaperone alleviates doxorubicin-induced cardiac dysfunction. Circ Res 118(5):798–809. https://doi.org/10.1161/CIRCRESAHA.115.307604
Harhous Z, Booz GW, Ovize M, Bidaux G, Kurdi M (2019) An update on the multifaceted roles of STAT3 in the heart. Front Cardiovasc Med 6:150. https://doi.org/10.3389/fcvm.2019.00150
Kunisada K, Negoro S, Tone E et al (2000) Signal transducer and activator of transcription 3 in the heart transduces not only a hypertrophic signal but a protective signal against doxorubicin-induced cardiomyopathy. Proc Natl Acad Sci USA 97(1):315–319. https://doi.org/10.1073/pnas.97.1.315
Lahnwong S, Chattipakorn SC, Chattipakorn N (2018) Potential mechanisms responsible for cardioprotective effects of sodium-glucose co-transporter 2 inhibitors. Cardiovasc Diabetol 17(1):101. https://doi.org/10.1186/s12933-018-0745-5
Li C, Zhang J, Xue M et al (2019) SGLT2 inhibition with empagliflozin attenuates myocardial oxidative stress and fibrosis in diabetic mice heart. Cardiovasc Diabetol 18(1):15. https://doi.org/10.1186/s12933-019-0816-2
Lipshultz SE, Scully RE, Lipsitz SR et al (2010) Assessment of dexrazoxane as a cardioprotectant in doxorubicin-treated children with high-risk acute lymphoblastic leukaemia: long-term follow-up of a prospective, randomised, multicentre trial. Lancet Oncol 11(10):950–961. https://doi.org/10.1016/S1470-2045(10)70204-7
Lou Y, Wang Z, Xu Y et al (2015) Resveratrol prevents doxorubicin-induced cardiotoxicity in H9c2 cells through the inhibition of endoplasmic reticulum stress and the activation of the Sirt1 pathway. Int J Mol Med 36(3):873–880. https://doi.org/10.3892/ijmm.2015.2291
McDonagh TA, Metra M, Adamo M et al (2021) 2021 ESC guidelines for the diagnosis and treatment of acute and chronic heart failure. Eur Heart J 42(36):3599–3726. https://doi.org/10.1093/eurheartj/ehab368
McMurray JJV, Solomon SD, Inzucchi SE et al (2019) Dapagliflozin in patients with heart failure and reduced ejection fraction. N Engl J Med 381(21):1995–2008. https://doi.org/10.1056/NEJMoa1911303
Moreira AC, Branco AF, Sampaio SF et al (1842) (2014) Mitochondrial apoptosis-inducing factor is involved in doxorubicin-induced toxicity on H9c2 cardiomyoblasts. Biochim Biophys Acta 12 Pt A:2468–2478. https://doi.org/10.1016/j.bbadis.2014.09.015
Neal B, Perkovic V, Mahaffey KW et al (2017) Canagliflozin and cardiovascular and renal events in type 2 diabetes. N Engl J Med 377(7):644–657. https://doi.org/10.1056/NEJMoa1611925
Nebigil CG, Desaubry L (2018) Updates in anthracycline-mediated cardiotoxicity. Front Pharmacol 9:1262. https://doi.org/10.3389/fphar.2018.01262
Quagliariello V, De Laurentiis M, Rea D et al (2021) The SGLT-2 inhibitor empagliflozin improves myocardial strain, reduces cardiac fibrosis and pro-inflammatory cytokines in non-diabetic mice treated with doxorubicin. Cardiovasc Diabetol 20(1):150. https://doi.org/10.1186/s12933-021-01346-y
Rong J, Li L, Jing L, Fang H, Peng S (2016) JAK2/STAT3 pathway mediates protection of metallothionein against doxorubicin-induced cytotoxicity in mouse cardiomyocytes. Int J Toxicol 35(3):317–326. https://doi.org/10.1177/1091581815614261
Sabatino J, De Rosa S, Tamme L et al (2020) Empagliflozin prevents doxorubicin-induced myocardial dysfunction. Cardiovasc Diabetol 19(1):66. https://doi.org/10.1186/s12933-020-01040-5
Shih JY, Lin YW, Fisch S et al (2021) Dapagliflozin suppresses ER stress and improves subclinical myocardial function in diabetes: from bedside to bench. Diabetes 70(1):262–267. https://doi.org/10.2337/db20-0840
Sreenivasan L, Wang H, Yap SQ, Leclair P, Tam A, Lim CJ (2020) Autocrine IL-6/STAT3 signaling aids development of acquired drug resistance in Group 3 medulloblastoma. Cell Death Dis 11(12):1035. https://doi.org/10.1038/s41419-020-03241-y
Stapel B, Kohlhaas M, Ricke-Hoch M et al (2017) Low STAT3 expression sensitizes to toxic effects of beta-adrenergic receptor stimulation in peripartum cardiomyopathy. Eur Heart J 38(5):349–361. https://doi.org/10.1093/eurheartj/ehw086
Swain SM, Whaley FS, Gerber MC et al (1997) Cardioprotection with dexrazoxane for doxorubicin-containing therapy in advanced breast cancer. J Clin Oncol 15(4):1318–1332. https://doi.org/10.1200/JCO.1997.15.4.1318
Tanaka R, Umemura M, Narikawa M et al (2020) Reactive fibrosis precedes doxorubicin-induced heart failure through sterile inflammation. ESC Heart Fail 7(2):588–603. https://doi.org/10.1002/ehf2.12616
Wallace KB, Sardao VA, Oliveira PJ (2020) Mitochondrial determinants of doxorubicin-induced cardiomyopathy. Circ Res 126(7):926–941. https://doi.org/10.1161/CIRCRESAHA.119.314681
Wang XY, Yang CT, Zheng DD et al (2012) Hydrogen sulfide protects H9c2 cells against doxorubicin-induced cardiotoxicity through inhibition of endoplasmic reticulum stress. Mol Cell Biochem 363(1–2):419–426. https://doi.org/10.1007/s11010-011-1194-6
Yao Y, Lu Q, Hu Z, Yu Y, Chen Q, Wang QK (2017) A non-canonical pathway regulates ER stress signaling and blocks ER stress-induced apoptosis and heart failure. Nat Commun 8(1):133. https://doi.org/10.1038/s41467-017-00171-w
Zhang S, Liu X, Bawa-Khalfe T et al (2012) Identification of the molecular basis of doxorubicin-induced cardiotoxicity. Nat Med 18(11):1639–1642. https://doi.org/10.1038/nm.2919
Zhao L, Zhang B (2017) Doxorubicin induces cardiotoxicity through upregulation of death receptors mediated apoptosis in cardiomyocytes. Sci Rep 7:44735. https://doi.org/10.1038/srep44735
Zinman B, Wanner C, Lachin JM et al (2015) Empagliflozin, cardiovascular outcomes, and mortality in type 2 diabetes. N Engl J Med 373(22):2117–2128. https://doi.org/10.1056/NEJMoa1504720
Acknowledgements
We especially thank the support from Professor Wei-Jan Chen in Linkou Chang Gung Memorial Hospital/Chang Gung University, Taiwan
Funding
This study was supported by Chi-Mei Medical Center, Ministry of Science and Technology (MOST105-2628-B-384-001-MY3; 108-2628-B-384), National Health Research Institute (NHRI-EX106-10618SC).
Author information
Authors and Affiliations
Contributions
All authors were involved in the conception and design of the study and data interpretation. WC and YL drafted the paper and performed data analysis. WC and YL were involved in the data analysis and interpretation. All authors critically revised the paper and approved it for submission.
Corresponding author
Ethics declarations
Conflict of interest
No conflicts of interest.
Ethics approval and consent to participate
This study was approved by the Institutional Review Board of Chi-Mei Medical Center (CV code: 10406-E01). Given that the data is derived from the NHIRD databank, the consent to participate is not applicable.
Consent for publication
Not applicable.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
204_2022_3298_MOESM2_ESM.tif
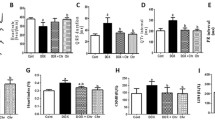
Supplementary file2 Supplement Figure 2. The changes in (A) body weight (BW), (B) blood sugar (BS), and (C) heart rate (HR) in the control, dapagliflozin (DAPA), doxorubicin (Dox) and Dox + DAPA groups (N=6–8) (TIF 740 KB)
204_2022_3298_MOESM3_ESM.tif
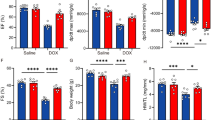
Supplementary file3 Supplement Figure 3. The effects of dapagliflozin (DAPA) on survival, cardiac morphology and lung injury in rats treated with doxorubicin (Dox). (A) The survival curve, (B) harvested hearts, (C) heart-to-body weight ratio, (D) heart-to-tibial bone length ratio, and (E) wet-dry lung ratio in the control, DAPA, Dox, and Dox+DAPA groups. *P < 0.05, **P < 0.01, and ***P < 0.001 compared with the indicated groups (N=6–8) (TIF 2282 KB)
204_2022_3298_MOESM4_ESM.tif
Supplementary file4 Supplement Figure 4. The effects of dapagliflozin (DAPA) on STAT3 in cardiomyocytes of rat after doxorubicin (Dox) treatment. (A) Representative sections of hearts stained with STAT3 (green) and F-actin (blue); scale bars, 20 µm. (B) Quantification of STAT3 expression in the indicated groups of rats. *P < 0.05, and ***P < 0.001 compared with the indicated groups (N=5) (TIF 12685 KB)
204_2022_3298_MOESM5_ESM.tif
Supplementary file5 Supplement Figure 5. The efficiency of transfection in cardiomyocytes treated with STAT3 siRNA compared with cells transfected with control siRNA. Abbreviations: Dox: doxorubicin; Dapa: dapagliflozin; STZ: Streptozotocin; ER: endoplasmic reticulum; ROS: reactive oxygen species; SGLT2: sodium glucose cotransporter; NHI: National Health Insurance; NHIRD: National Health Insurance Research Database; MACCEs: major adverse cardio- and cerebrovascular events; CKD: chronic kidney disease; ESRD: end-stage renal disease; COPD: chronic obstructive pulmonary disease; IVSd: interventricular septum thickness in diastole; LVIDd: left ventricular internal diameter; in diastole; EF: ejection fraction; FS: fractional shortening; P-V: Pressure–volume; HE: hematoxylin–eosin; Ves: end-systolic; Ved: diastolic volumes; Pes: end-systolic; Ped: diastolic pressures; +dP/dt and -dP/dt: maximal velocity of pressure rise and fall; Ea: arterial elastance; tau: time constant of isovolumic pressure decay; ESPVR: end-systolic pressure-volume relationship; EDPVR: end-diastolic pressure–volume relationship; IVC: inferior vena cava; MTT:3-(4,5-dimethyl-2-thiazolyl)-2,5-dimethyl-2H-tetrazolium bromide; H2DCF‑DA: fluorescent 2',7'‑dichlorofluorescindiacetate; PI: propidium iodide; TUNEL: terminal deoxynucleotidyl transferase-mediated dUTP nick-end labeling (TIF 422 KB)
Rights and permissions
About this article
Cite this article
Chang, WT., Shih, JY., Lin, YW. et al. Dapagliflozin protects against doxorubicin-induced cardiotoxicity by restoring STAT3. Arch Toxicol 96, 2021–2032 (2022). https://doi.org/10.1007/s00204-022-03298-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00204-022-03298-y