Abstract
Summary
Fibula response to disuse is unknown; we assessed fibula bone in spinal cord injury (SCI) patients and able-bodied counterparts. Group differences were smaller than in the neighbouring tibia which could not be explained by bone geometry. Differential adaptation of the shank bones may indicate previously unknown mechanoadaptive behaviours of bone.
Introduction
The fibula supports only a small and highly variable proportion of shank compressive load (−8 to +19 %), and little is known about other kinds of stresses. Hence, whilst effects of habitual loading on tibia are well-known, fibula response to disuse is difficult to predict.
Methods
Therefore, we assessed fibular bone strength using peripheral quantitative computed tomography (pQCT) at 5 % increments from 5 to 90 % distal-proximal tibia length in nine participants with long-term spinal cord injury (SCI; age 39.2 ± 6.2 years, time since injury 17.8 ± 7.4 years), representing a cross-sectional model of long-term disuse and in nine able-bodied counterparts of similar age (39.6 ± 7.8 years), height and mass.
Results
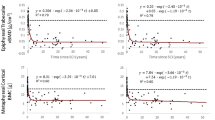
There was no group difference in diaphyseal fibula total bone mineral content (BMC) (P = 0.22, 95 % CIs -7.4 % to -13.4 % and +10.9 % to +19.2 %). Site by group interactions (P < 0.001) revealed 27 and 22 % lower BMC in SCI at 5 and 90 % (epiphyseal) sites only. Cortical bone geometry differed at mid and distal diaphysis, with lower endocortical circumference and greater cortical thickness in SCI than able-bodied participants in this region only (interactions both P < 0.01). Tibia bone strength was also assessed; bone by group interactions showed smaller group differences in fibula than tibia for all bone parameters, with opposing effects on distal diaphysis geometry in the two bones (all Ps < 0.001).
Conclusions
These results suggest that the structure of the fibula diaphysis is not heavily influenced by compressive loading, and only mid and distal diaphysis are influenced by bending and/or torsional loads. The fibula is less influenced by disuse than the tibia, which cannot satisfactorily be explained by differences in bone geometry or relative changes in habitual loading in disuse. Biomechanical study of the shank loading environment may give new information pertaining to factors influencing bone mechanoadaptation.




Similar content being viewed by others
References
Funk JR, Rudd RW, Kerrigan JR, Crandall JR (2007) The line of action in the tibia during axial compression of the leg. J Biomech 40:2277–2282
Wang Q, Whittle M, Cunningham J, Kenwright J (1996) Fibula and its ligaments in load transmission and ankle joint stability. Clin Orthop Relat Res:261–270
Thambyah A, Pereira BP (2006) Mechanical contribution of the fibula to torsion stiffness in the lower extremity. Clin Anat 19:615–620
Cointry GR, Nocciolino L, Ireland A, Hall NM, Kriechbaumer A, Ferretti JL, Rittweger J, Capozza RF (2015) Structural differences in cortical shell properties between upper and lower human fibula as described by pQCT serial scans. A biomechanical interpretation. Bone 90:185–194
Alho A, Høiseth A (1991) Bone mass distribution in the lower leg. A quantitative computed tomographic study of 36 individuals. Acta Orthop Scand 62:468–470
Taddei F, Balestri M, Rimondi E, Viceconti M, Manfrini M (2009) Tibia adaptation after fibula harvesting: an in vivo quantitative study. Clin Orthop Relat Res 467:2149–2158
Marchi D, Shaw CN (2011) Variation in fibular robusticity reflects variation in mobility patterns. J Hum Evol 61:609–616
Pećina M, Ruszkowsky I, Muftić O, Antičević D (1982) The fibula in clinical and experimental evaluation of the theory on functional adaptation of bone. Collegium Antropologicum 6:197–206
Coupaud S, McLean AN, Purcell M, Fraser MH, Allan DB (2015) Decreases in bone mineral density at cortical and trabecular sites in the tibia and femur during the first year of spinal cord injury. Bone 74:69–75
Eser P, Frotzler A, Zehnder Y, Wick L, Knecht H, Denoth J, Schiessl H (2004) Relationship between the duration of paralysis and bone structure: a pQCT study of spinal cord injured individuals. Bone 34:869–880
Rittweger J, Goosey-Tolfrey VL, Cointry G, Ferretti JL (2010) Structural analysis of the human tibia in men with spinal cord injury by tomographic (pQCT) serial scans. Bone 47:511–518
Dudley-Javoroski S, Shields RK (2012) Regional cortical and trabecular bone loss after spinal cord injury. J Rehabil Res Dev 49:1365–1376
Rittweger J, Frost HM, Schiessl H, Ohshima H, Alkner B, Tesch P, Felsenberg D (2005) Muscle atrophy and bone loss after 90 days’ bed rest and the effects of flywheel resistive exercise and pamidronate: results from the LTBR study. Bone 36:1019–1029
Kern DS, Semmler JG, Enoka RM (2001) Long-term activity in upper- and lower-limb muscles of humans. J Appl Physiol 91:2224–2232
Rittweger J, Michaelis I, Giehl M, Wüsecke P, Felsenberg D (2004) Adjusting for the partial volume effect in cortical bone analyses of pQCT images. J Musculoskelet Neuronal Interact 4:436–441
Ward KA, Adams JE, Hangartner TN (2005) Recommendations for thresholds for cortical bone geometry and density measurement by peripheral quantitative computed tomography. Calcif Tissue Int 77:275–280
Hangartner TN, Gilsanz V (1996) Evaluation of cortical bone by computed tomography. J Bone Miner Res 11:1518–1525
Rittweger J, Beller G, Ehrig J et al (2000) Bone-muscle strength indices for the human lower leg. Bone 27:319–326
Rittweger J, Simunic B, Bilancio G, De Santo NG, Cirillo M, Biolo G, Pisot R, Eiken O, Mekjavic IB, Narici M (2009) Bone loss in the lower leg during 35 days of bed rest is predominantly from the cortical compartment. Bone 44:612–618
Rantalainen T, Duckham RL, Suominen H, Heinonen A, Alén M, Korhonen MT (2014) Tibial and fibular mid-shaft bone traits in young and older sprinters and non-athletic men. Calcif Tissue Int 95:132–140
Rantalainen T, Nikander R, Heinonen A, Suominen H, Sievänen H (2010) Direction-specific diaphyseal geometry and mineral mass distribution of tibia and fibula: a pQCT study of female athletes representing different exercise loading types. Calcif Tissue Int 86:447–454
Parfitt AM (2002) Misconceptions (2): turnover is always higher in cancellous than in cortical bone. Bone 30:807–809
Frost HM (1987) Bone “mass” and the “mechanostat”: a proposal. Anat Rec 219:1–9
Noble BS, Peet N, Stevens HY, Brabbs A, Mosley JR, Reilly GC, Reeve J, Skerry TM, Lanyon LE (2003) Mechanical loading: biphasic osteocyte survival and targeting of osteoclasts for bone destruction in rat cortical bone. Am J Physiol Cell Physiol 284:C934–C943
Rodríguez JI, Palacios J, García-Alix A, Pastor I, Paniagua R (1988) Effects of immobilization on fetal bone development. A morphometric study in newborns with congenital neuromuscular diseases with intrauterine onset. Calcif Tissue Int 43:335–339
Biggin A, Briody JN, Ramjan KA, Middleton A, Waugh MC, Munns CF (2013) Evaluation of bone mineral density and morphology using pQCT in children after spinal cord injury. Dev Neurorehabil 16:391–397
Cullen DM, Smith RT, Akhter MP (2001) Bone-loading response varies with strain magnitude and cycle number. J Appl Physiol 91:1971–1976
Turner CH, Owan I, Takano Y (1995) Mechanotransduction in bone: role of strain rate. Am J Phys 269:E438–E442
Warden SJ, Mantila Roosa SM, Kersh ME, Hurd AL, Fleisig GS, Pandy MG, Fuchs RK (2014) Physical activity when young provides lifelong benefits to cortical bone size and strength in men. Proc Natl Acad Sci U S A 111(14):5337–5342
Ireland A, Maden-Wilkinson T, Ganse B, Degens H, Rittweger J (2014) Effects of age and starting age upon side asymmetry in the arms of veteran tennis players: a cross-sectional study. Osteoporos Int 25:1389–1400
Vatsa A, Breuls RG, Semeins CM, Salmon PL, Smit TH, Klein-Nulend J (2008) Osteocyte morphology in fibula and calvaria—is there a role for mechanosensing? Bone 43:452–458
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
The study was approved by the ethics committee of Manchester Metropolitan University, and all participants gave written informed consent prior to participation.
Conflict of interest
None.
Rights and permissions
About this article
Cite this article
Ireland, A., Capozza, R.F., Cointry, G.R. et al. Meagre effects of disuse on the human fibula are not explained by bone size or geometry. Osteoporos Int 28, 633–641 (2017). https://doi.org/10.1007/s00198-016-3779-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00198-016-3779-0