Abstract
Purpose
No “ideal” landmark for tibial component rotation in medial unicompartmental knee arthroplasty (UKA) has been suggested by a biomechanical and clinical study. The aim of this study was to investigate whether the anterior superior iliac spine (ASIS) could provide a consistent rotational landmark of the tibial component during mobile-bearing medial UKA using computed tomography (CT).
Methods
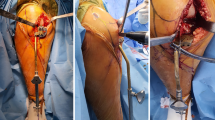
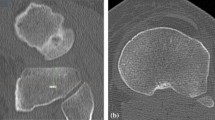
During sagittal tibial resection, we utilized the ASIS as a rotational landmark. In 47 knees that underwent postoperative CT scans after medial UKA, the tibial component position was assessed by drawing a line tangential to the lateral wall of the tibial component. Rotation of the tibial component was measured using two reference lines: a line perpendicular to the posterior cortical rim of the tibia (angle α) and Akagi’s line (angle β). Instant bearing position and posterior cruciate ligament (PCL) fossa involvement were also evaluated. External rotation of the tibial component relative to each reference line was considered positive values.
Results
The mean α and β angles were 8.0° ± 6.1° (range −4.0 to 24.3) and 8.7° ± 4.8° (range 1.9–25.2), respectively. Fourteen knees (29.8 %) showed PCL fossa involvement of the tibial resection margin. One bearing showed complete 180° rotation at 2 weeks postoperatively.
Conclusion
Due to the wide variation and inherent difficulty of identifying the ASIS during the operation, it is not recommended for guidance of sagittal tibial resection during medial UKA. In cases of inappropriate tibia component rotation, risk of PE bearing spinning and iatrogenic PCL injury should be reminded after medial UKA.
Level of evidence
IV.






Similar content being viewed by others
References
Akagi M, Oh M, Nonaka T, Tsujimoto H, Asano T, Hamanishi C (2004) An anteroposterior axis of the tibia for total knee arthroplasty. Clin Orthop Relat Res 420:213–219
Altman DG (1991) Practical statistics for medical research, 1st edn. Chapman and Hall, London, pp 403–405
Anderson CJ, Ziegler CG, Wijdicks CA, Engebretsen L, LaPrade RF (2012) Arthroscopically pertinent anatomy of the anterolateral and posteromedial bundles of the posterior cruciate ligament. J Bone Joint Surg Am 94(21):1936–1945
Barbadoro P, Ensini A, Leardini A, d’Amato M, Feliciangeli A, Timoncini A, Amadei F, Belvedere C, Giannini S (2014) Tibial component alignment and risk of loosening in unicompartmental knee arthroplasty: a radiographic and radiostereometric study. Knee Surg Sports Traumatol Arthrosc 22(12):3157–3162
Campbell DG, Johnson LJ, West SC (2006) Multiparameter quantitative computer-assisted tomography assessment of unicompartmental knee arthroplasties. ANZ J Surg 76(9):782–787
Edwards A, Bull AM, Amis AA (2007) The attachments of the fiber bundles of the posterior cruciate ligament: an anatomic study. Arthroscopy 23(3):284–290
Emerson RH Jr, Higgins LL (2008) Unicompartmental knee arthroplasty with the oxford prosthesis in patients with medial compartment arthritis. J Bone Joint Surg Am 90(1):118–122
Goodfellow J (2006) Unicompartmental arthroplasty with the Oxford knee. Oxford University Press, Oxford
Hatsushika D, Nimura A, Mochizuki T, Yamaguchi K, Muneta T, Akita K (2013) Attachments of separate small bundles of human posterior cruciate ligament: an anatomic study. Knee Surg Sports Traumatol Arthrosc 21(5):998–1004
Iriberri I, Aragon JF (2014) Alignment of the tibial component of the unicompartmental knee arthroplasty, assessed in the axial view by CT scan: does it influence the outcome? Knee 21(6):1269–1274
Kawahara S, Matsuda S, Okazaki K, Tashiro Y, Iwamoto Y (2012) Is the medial wall of the intercondylar notch useful for tibial rotational reference in unicompartmental knee arthroplasty? Clin Orthop Relat Res 470(4):1177–1184
Kawahara S, Okazaki K, Matsuda S, Mitsuyasu H, Nakahara H, Okamoto S, Iwamoto Y (2014) Medial sixth of the patellar tendon at the tibial attachment is useful for the anterior reference in rotational alignment of the tibial component. Knee Surg Sports Traumatol Arthrosc 22(5):1070–1075
Kendrick BJ, Simpson DJ, Kaptein BL, Valstar ER, Gill HS, Murray DW, Price AJ (2011) Polyethylene wear of mobile-bearing unicompartmental knee replacement at 20 years. J Bone Joint Surg Br 93(4):470–475
Khanna G, Levy BA (2007) Oxford unicompartmental knee replacement: literature review. Orthopedics 30(5 Suppl):11–14
Kristensen PW, Holm HA, Varnum C (2013) Up to 10-year follow-up of the Oxford medial partial knee arthroplasty—695 cases from a single institution. J Arthroplasty 28(9 Suppl):195–198
Lewold S, Goodman S, Knutson K, Robertsson O, Lidgren L (1995) Oxford meniscal bearing knee versus the Marmor knee in unicompartmental arthroplasty for arthrosis. A Swedish multicenter survival study. J Arthroplasty 10(6):722–731
Muller PE, Pellengahr C, Witt M, Kircher J, Refior HJ, Jansson V (2004) Influence of minimally invasive surgery on implant positioning and the functional outcome for medial unicompartmental knee arthroplasty. J Arthroplasty 19(3):296–301
Pandit H, Murray DW, Dodd CA, Deo S, Waite J, Goodfellow J, Gibbons CL (2007) Medial tibial plateau fracture and the Oxford unicompartmental knee. Orthopedics 30(5 Suppl):28–31
Paternostre F, Schwab PE, Thienpont E (2014) The combined Whiteside’s and posterior condylar line as a reliable reference to describe axial distal femoral anatomy in patient-specific instrument planning. Knee Surg Sports Traumatol Arthrosc 22(12):3054–3059
Peersman G, Stuyts B, Vandenlangenbergh T, Cartier P, Fennema P (2015) Fixed- versus mobile-bearing UKA: a systematic review and meta-analysis. Knee Surg Sports Traumatol Arthrosc 23(11):3296–3305
Rudol G, Jackson MP, James SE (2007) Medial tibial plateau fracture complicating unicompartmental knee arthroplasty. J Arthroplasty 22(1):148–150
Scott RD (2010) Mobile- versus fixed-bearing unicompartmental knee arthroplasty. Instr Course Lect 59:57–60
Servien E, Fary C, Lustig S, Demey G, Saffarini M, Chomel S, Neyret P (2011) Tibial component rotation assessment using CT scan in medial and lateral unicompartmental knee arthroplasty. Orthop Traumatol Surg Res 97(3):272–275
Shakespeare D, Ledger M, Kinzel V (2005) The influence of the tibial sagittal cut on component position in the Oxford knee. Knee 12(3):169–176
Smith TO, Hing CB, Davies L, Donell ST (2009) Fixed versus mobile bearing unicompartmental knee replacement: a meta-analysis. Orthop Traumatol Surg Res 95(8):599–605
Song MH, Kim BH, Ahn SJ, Yoo SH, Lee MS (2009) Early complications after minimally invasive mobile-bearing medial unicompartmental knee arthroplasty. J Arthroplasty 24(8):1281–1284
Tajima G, Nozaki M, Iriuchishima T, Ingham SJ, Shen W, Smolinski P, Fu FH (2009) Morphology of the tibial insertion of the posterior cruciate ligament. J Bone Joint Surg Am 91(4):859–866
Yoshida K, Tada M, Yoshida H, Takei S, Fukuoka S, Nakamura H (2013) Oxford phase 3 unicompartmental knee arthroplasty in Japan—clinical results in greater than one thousand cases over ten years. J Arthroplasty 28(9 Suppl):168–171
Yoshioka Y, Siu DW, Scudamore RA, Cooke TD (1989) Tibial anatomy and functional axes. J Orthop Res 7(1):132–137
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors of this manuscript have no financial conflicts of interest to report regarding this work.
Rights and permissions
About this article
Cite this article
Lee, SY., Chay, S., Lim, HC. et al. Tibial component rotation during the unicompartmental knee arthroplasty: is the anterior superior iliac spine an appropriate landmark?. Knee Surg Sports Traumatol Arthrosc 25, 3723–3732 (2017). https://doi.org/10.1007/s00167-016-4192-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00167-016-4192-0