Abstract
Purpose
When performing knee arthroscopy, joint stressing is essential to increase the operative joint space. Adequate training of joint stressing is important, since high stressing forces can damage knee ligaments, and low stressing might not give sufficient operative space. As forces are difficult to transfer since they cannot be seen, simulators might be suited to train joint stressing as they can visualise the amount of applied stress. This requires the joint stressing thresholds to be validated. The purpose of this study was to measure the variation in the maximum joint stressing forces applied by various surgeons in vivo in a human population and based on that derive thresholds for safe stressing.
Methods
From studies on ligament failure properties, we inferred a theoretical maximum stressing force of 78 N. Twenty-one patients were included, and knee arthroscopies were performed by five experienced surgeons. Forces solely performed in the varus and in valgus direction were measured. A load sensor was mounted on a belt, which was rotated along the hip to measure both varus and valgus stressing. The measurements started as soon as the interior of the knee joint was visualised using joint stressing.
Results
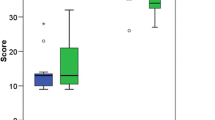
The average maximum stressing force was 60 N (SD = 28 N). The mean first frame force was 47 N (SD = 34 N). No significant differences were found between varus and valgus stressing.
Conclusion
Since variation in stressing forces is high, offering training cases on simulators where the complete range of stressing forces can be experienced is recommended. Abiding to safety levels is essential to increase patient safety.





Similar content being viewed by others
References
Cannon WD, Eckhoff DG, Garrett WE Jr, Hunter RE, Sweeney HJ (2006) Report of a group developing a virtual reality simulator for arthroscopic surgery of the knee joint. Clin Orthop Relat Res 442:21–29
Heng PA, Cheng CY, Wong TT, Wu W, Xu Y, Xie Y et al (2006) Virtual reality techniques. Application to anatomic visualization and orthopaedics training. Clin Orthop Relat Res 442:5–12
Howells NR, Gill HS, Carr AJ, Price AJ, Rees JL (2008) Transferring simulated arthroscopic skills to the operating theatre: a randomised blinded study. J Bone Joint Surg Br 90(4):494–499
Hull ML, Berns GS, Varma H, Patterson HA (1996) Strain in the medial collateral ligament of the human knee under single and combined loads. J Biomech 29(2):199–206
Kennedy JC, Hawkins RJ, Willis RB, Danylchuck KD (1976) Tension studies of human knee ligaments. Yield point, ultimate failure, and disruption of the cruciate and tibial collateral ligaments. J Bone Joint Surg Am 58(3):350–355
Laros GS, Tipton CM, Cooper RR (1971) Influence of physical activity on ligament insertions in the knees of dogs. J Bone Joint Surg Am 53(2):275–286
Mabrey JD, Cannon WD, Gillogly SD, Kasser JR, Sweeney HJ, Zarins B et al (2000) Development of a virtual reality arthroscopic knee simulator. Stud Health Technol Inform 70:192–194
McCarthy AD, Moody L, Waterworth AR, Bickerstaff DR (2006) Passive haptics in a knee arthroscopy simulator: is it valid for core skills training? Clin Orthop Relat Res 442:13–20
Mensch JS, Amstutz HC (1975) Knee morphology as a guide to knee replacement. Clin Orthop Relat Res 112:231–241
Meyer RD, Tamarapalli JR, Lemons JE (1993) Arthroscopy training using a “black box” technique. Arthroscopy 9(3):338–340
Moody L, Waterworth AR, McCarthy AD, Harley P, Smallwood R (2012) The feasibility of a mixed reality surgical training environment. Virtual Real 12:77–86
Nandi S, Parker R (2012) Deep medial collateral ligament tear during knee arthroscopy. J Knee Surg 25(1):79–81
Robinson JR, Bull AM, Amis AA (2005) Structural properties of the medial collateral ligament complex of the human knee. J Biomech 38(5):1067–1074
Safir O, Dubrowski A, Mirsky L, Lin C, Backstein D, Carnahan A (2008) What skills should simulation training in arthroscopy teach residents? Int J Comput Assist Radiol Surg 3:433–437
Schmid RB, Wirz D, Gopfert B, Arnold MP, Friederich NF, Hirschmann MT (2011) Intra-operative femoral condylar stress during arthroscopy: an in vivo biomechanical assessment. Knee Surg Sports Traumatol Arthrosc 19(5):747–752
Smith BW, Green GA (1995) Acute knee injuries: part I. History and physical examination. Am Fam Physician 51(3):615–621
Trent PS, Walker PS, Wolf B (1976) Ligament length patterns, strength, and rotational axes of the knee joint. Clin Orthop Relat Res 117:263–270
Tuijthof GJ, Horeman T, Schafroth MU, Blankevoort L, Kerkhoffs GM (2011) Probing forces of menisci: what levels are safe for arthroscopic surgery. Knee Surg Sports Traumatol Arthrosc 19(2):248–254
Tuijthof GJ, van Sterkenburg MN, Sierevelt IN, Van OJ, Van Dijk CN, Kerkhoffs GM (2010) First validation of the PASSPORT training environment for arthroscopic skills. Knee Surg Sports Traumatol Arthrosc 18(2):218–224
Woo SL, Gomez MA, Sites TJ, Newton PO, Orlando CA, Akeson WH (1987) The biomechanical and morphological changes in the medial collateral ligament of the rabbit after immobilization and remobilization. J Bone Joint Surg Am 69(8):1200–1211
Zivanovic A, Dibble E, Davies B, Moody L, Waterworth A (2003) Engineering requirements for a haptic simulator for knee arthroscopy training. Stud Health Technol Inform 94:413–418
Acknowledgments
This research was funded by the Marti-Keuning Eckhart Foundation, Lunteren, the Netherlands.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Stunt, J.J., Wulms, P.H.L.M., Kerkhoffs, G.M.M.J. et al. Variation in joint stressing magnitudes during knee arthroscopy. Knee Surg Sports Traumatol Arthrosc 22, 1529–1535 (2014). https://doi.org/10.1007/s00167-013-2545-5
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00167-013-2545-5