Abstract
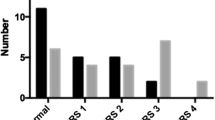
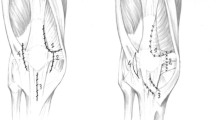
To assess the clinical outcomes of a group of patients who underwent arthroscopic infrapatellar plica (IPP) excision and to determine, whether the IPP was symptomatic or not, to identify the symptoms or signs in the patient’s clinical presentation and to study the correlations between arthroscopic findings and patient’s clinical presentation. A retrospective clinical study. We studied all the patients undergoing arthroscopic resection of symptomatic infrapatellar plica without other intraarticular abnormality at our department from February 1996 to April 2001. Fourteen patients with isolated IPP and with regular follow-up intervals were included in the study. Arthroscopy findings, preoperative magnetic resonance imaging (MRI) findings, and clinical presentation were correlated. The mean duration of follow-up was 36 months with a range of 24–60 months. The IPP was found to be in fenestra pattern in seven patients, separate (cordlike) pattern in five patients and vertical septum pattern in two patients. IPP in all patients was excised with a powered instrument. Two patients were rated as excellent, ten patients as good and two patients as poor results. All the patients were documented with pain, popping or snapping with flexion and extension, giving way and swelling. There was no correlation between IPP type and MRI findings with being symptomatic (P>0.05). It was found that IPP type was not a prognostic factor. Infrapatellar plica should be considered as a potential cause of knee pain with probable MRI imaging and no other evidence of internal derangement. We recommend close correlation with the clinical symptoms and exclusion of other internal derangement before suggesting infrapatellar plica as a sole cause for knee symptoms.


Similar content being viewed by others
References
Cothran RL, McGuire PM, Helms CA, Major NM, Attarian DE (2003) MR imaging of infrapatellar plica injury. Am J Roentgenol 180(5):1443–1447
Hardaker WT, Whipple TL, Bassett FH (1980) Diagnosis and treatment of the plica syndrome of the knee. J Bone Joint Surg Am 62:221–225
Johnson DP, Eastwood DM, Witherow PJ (1993) Symptomatic synovial plicae of the knee. J Bone Joint Surg Am 75:1485–1496
Kim SJ, Choe W (1996) Pathological infrapatellar plica: a report of two cases and literature review. Arthroscopy 12:236–239
Kim SJ, Min BH, Kim HK (1996) Arthroscopic anatomy of the infrapatellar plica. Arthroscopy 12(5):561–564
Kim SJ, Kim JY, Lee JW (2002) Pathologic infrapatellar plica. Arthroscopy 18(5):25–28
Kinnard P, Levesque RY (1984) The plica syndrome: a syndrome of controversy. Clin Orthop 183:141–143
Kohn D, Deiler S, Rudert M (1995) Arterial blood supply of the infrapatellar fat pad; anatomy and clinical consequences. Arch Orthop Trauma Surg 114:72–75
Koserek FJ, Helms CA (1999) The MR appearance of the infrapatellar plica. Am J Roentgenol 172(2):481–484
Magi M, Branca A, Bucca C, Langerame V (1991) Hoffa disease. Ital J Orthop Trauma 17:675–691
Muse GL, Grana WA, Hollingsworth S (1985) Arthroscopic treatment of medial shelf syndrome. Arthroscopy 1(1):63–67
Patel D (1978) Arthroscopy of the plicae-synovial folds and their significance. Am J Sports Med 6:217–225
Patel D (1986) Plica as a cause of anterior knee pain. Orthop Clin North Am 17(2):273–277
Reider B, Marshall JL, Warren RF (1981) Brief note. Persistent vertical septum in the human knee joint. J Bone Joint Surg Am 63:1185–1187
Tindel NL, Nisonson B (1992) The plica syndrome. Orthop Clin North Am 23:613–618
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Demirag, B., Ozturk, C. & Karakayali, M. Symptomatic infrapatellar plica. Knee Surg Sports Traumatol Arthrosc 14, 156–160 (2006). https://doi.org/10.1007/s00167-005-0643-8
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00167-005-0643-8