Abstract
Purpose
Since the 2005 French law on end of life and patients’ rights, it is unclear whether practices have evolved. We investigated whether an intensive communication strategy based on this law would influence practices in terms of withholding and withdrawing treatment (WWT), and outcome of patients hospitalised in intensive care (ICU).
Methods
This was a single-centre, two-period study performed before and after the 2005 law. Between these periods, an intensive strategy for communication was developed and implemented, comprising regular meetings and modalities for WWT. We examined medical records of all patients who died in the ICU or in hospital during both periods.
Results
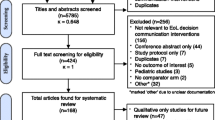
In total, out of 2,478 patients admitted in period 1, 678 (27%) died in the ICU and 823/2,940 (28%) in period 2. In period 1, among patients who died in the ICU, 45% died subsequent to a decision to WWT versus 85% in period 2 (p < 0.01). Among these, median time delay between ICU admission and initiation of decision-making process was significantly different (6–7 days in period 1 vs. 3–5 days in period 2, p < 0.05). Similarly, median time from admission to actual WWT decision was significantly shorter in period 2 (11–13 days in period 1 vs. 4–6 days in period 2, p < 0.05). Finally, median time from admission to death in the ICU subsequent to a decision to WWT was 13–15 days in period 1 versus 7–8 days in period 2, p < 0.05. Reasons for WWT were not significantly different between periods.
Conclusion
Intensive communication brings about quicker end-of-life decision-making in the ICU. The new law has the advantage of providing a legal framework.
Similar content being viewed by others
References
Ferrand E, Robert R, Ingrand P, Lemaire F (2001) Withholding and withdrawal of life support in intensive-care units in France: a prospective survey. French LATAREA Group. Lancet 357:9–14
Prendergast TJ, Luce JM (1997) Increasing incidence of withholding and withdrawal of life support from the critically ill. Am J Respir Crit Care Med 155:15–20
Smedira NG, Evans BH, Grais LS, Cohen NH, Lo B, Cooke M, Schecter WP, Fink C, Epstein-Jaffe E, May C et al (1990) Withholding and withdrawal of life support from the critically ill. N Engl J Med 322:309–315
Rapin M, Le Gall JR (1979) [Palliative comfort therapy in critically ill patients]. Bull Acad Natl Med 163:566–571 (discussion 571)
Knaus WA, Rauss A, Alperovitch A, Le Gall JR, Loirat P, Patois E, Marcus SE (1990) Do objective estimates of chances for survival influence decisions to withhold or withdraw treatment? The French Multicentric Group of ICU Research. Med Decis Making 10:163–171
Lilly CM, De Meo DL, Sonna LA, Haley KJ, Massaro AF, Wallace RF, Cody S (2000) An intensive communication intervention for the critically ill. Am J Med 109:469–475
Deliens L, Mortier F, Bilsen J, Cosyns M, Vander Stichele R, Vanoverloop J, Ingels K (2000) End-of-life decisions in medical practice in Flanders, Belgium: a nationwide survey. Lancet 356:1806–1811
Cook DJ, Guyatt G, Rocker G, Sjokvist P, Weaver B, Dodek P, Marshall J, Leasa D, Levy M, Varon J, Fisher M, Cook R (2001) Cardiopulmonary resuscitation directives on admission to intensive-care unit: an international observational study. Lancet 358:1941–1945
Drazen JM (2003) Decisions at the end of life. N Engl J Med 349:1109–1110
van der Heide A, Deliens L, Faisst K, Nilstun T, Norup M, Paci E, van der Wal G, van der Maas PJ (2003) End-of-life decision-making in six European countries: descriptive study. Lancet 362:345–350
Quill TE (2004) Dying and decision making—evolution of end-of-life options. N Engl J Med 350:2029–2032
Baumann A, Audibert G, Claudot F, Puybasset L (2009) Ethics review: end of life legislation—the French model. Crit Care 13:204
(2005) Loi n° 2005-370 du 22 avril 2005 relative aux droits des malades et à la fin de vie. Code de la Santé Publique. JORF 95:7089
Ferrand E (2002) Active withholding and withdrawal of therapy in adult intensive care units. Reanimation 11:442–449
Pochard F, Azoulay E, Chevret S, Vinsonneau C, Grassin M, Lemaire F, Herve C, Schlemmer B, Zittoun R, Dhainaut JF (2001) French intensivists do not apply American recommendations regarding decisions to forgo life-sustaining therapy. Crit Care Med 29:1887–1892
Antonelli M, Azoulay E, Bonten M, Chastre J, Citerio G, Conti G, De Backer D, Lemaire F, Gerlach H, Hedenstierna G, Joannidis M, Macrae D, Mancebo J, Maggiore SM, Mebazaa A, Preiser JC, Pugin J, Wernerman J, Zhang H (2010) Year in review in Intensive Care Medicine 2009. Part III: mechanical ventilation, acute lung injury and respiratory distress syndrome, pediatrics, ethics, and miscellanea. Intensive Care Med 36:567–584
Azoulay E, Metnitz B, Sprung CL, Timsit JF, Lemaire F, Bauer P, Schlemmer B, Moreno R, Metnitz P (2009) End-of-life practices in 282 intensive care units: data from the SAPS 3 database. Intensive Care Med 35:623–630
Sprung CL, Cohen SL, Sjokvist P, Baras M, Bulow HH, Hovilehto S, Ledoux D, Lippert A, Maia P, Phelan D, Schobersberger W, Wennberg E, Woodcock T (2003) End-of-life practices in European intensive care units: the Ethicus Study. JAMA 290:790–797
Baggs JG, Ryan SA, Phelps CE, Richeson JF, Johnson JE (1992) The association between interdisciplinary collaboration and patient outcomes in a medical intensive care unit. Heart Lung 21:18–24
Fagin CM (1992) Collaboration between nurses and physicians: no longer a choice. Acad Med 67:295–303
Gramelspacher GP, Howell JD, Young MJ (1986) Perceptions of ethical problems by nurses and doctors. Arch Intern Med 146:577–578
Stricker KH, Kimberger O, Schmidlin K, Zwahlen M, Mohr U, Rothen HU (2009) Family satisfaction in the intensive care unit: what makes the difference? Intensive Care Med 35:2051–2059
(1995) A controlled trial to improve care for seriously ill hospitalized patients. The study to understand prognoses and preferences for outcomes and risks of treatments (SUPPORT). The SUPPORT Principal Investigators. JAMA 274:1591–1598
Truog RD, Cist AF, Brackett SE, Burns JP, Curley MA, Danis M, DeVita MA, Rosenbaum SH, Rothenberg DM, Sprung CL, Webb SA, Wlody GS, Hurford WE (2001) Recommendations for end-of-life care in the intensive care unit: The Ethics Committee of the Society of Critical Care Medicine. Crit Care Med 29:2332–2348
Stevens L, Cook D, Guyatt G, Griffith L, Walter S, McMullin J (2002) Education, ethics, and end-of-life decisions in the intensive care unit. Crit Care Med 30:290–296
Cook DJ, Giacomini M, Johnson N, Willms D (1999) Life support in the intensive care unit: a qualitative investigation of technological purposes. Canadian Critical Care Trials Group. CMAJ 161:1109–1113
Asch DA, Hansen-Flaschen J, Lanken PN (1995) Decisions to limit or continue life-sustaining treatment by critical care physicians in the United States: conflicts between physicians’ practices and patients’ wishes. Am J Respir Crit Care Med 151:288–292
Ferrand E, Bachoud-Levi AC, Rodrigues M, Maggiore S, Brun-Buisson C, Lemaire F (2001) Decision-making capacity and surrogate designation in French ICU patients. Intensive Care Med 27:1360–1364
Sprung CL, Eidelman LA (1996) Worldwide similarities and differences in the foregoing of life-sustaining treatments. Intensive Care Med 22:1003–1005
Vincent JL (1990) European attitudes towards ethical problems in intensive care medicine: results of an ethical questionnaire. Intensive Care Med 16:256–264
Stanley JM (1992) The Appleton international conference: developing guidelines for decisions to forgo life-prolonging medical treatment—Preamble, Parts I, II, III, and IV. J Med Ethics 18:S3–S22
(1992) Attitudes of critical care medicine professionals concerning forgoing life-sustaining treatments. The Society of Critical Care Medicine Ethics Committee. Crit Care Med 20:320–326
(1991) Withholding and withdrawing life-sustaining therapy. This Official Statement of the American Thoracic Society was adopted by the ATS Board of Directors, March 1991. Am Rev Respir Dis 144:726–731
Mitchell PH, Armstrong S, Simpson TF, Lentz M (1989) American association of critical-care nurses demonstration project: profile of excellence in critical care nursing. Heart Lung 18:219–237
Ferrand E, Lemaire F, Regnier B, Kuteifan K, Badet M, Asfar P, Jaber S, Chagnon JL, Renault A, Robert R, Pochard F, Herve C, Brun-Buisson C, Duvaldestin P (2003) Discrepancies between perceptions by physicians and nursing staff of intensive care unit end-of-life decisions. Am J Respir Crit Care Med 167:1310–1315
Author information
Authors and Affiliations
Corresponding author
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Quenot, J.P., Rigaud, J.P., Prin, S. et al. Impact of an intensive communication strategy on end-of-life practices in the intensive care unit. Intensive Care Med 38, 145–152 (2012). https://doi.org/10.1007/s00134-011-2405-z
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00134-011-2405-z