Abstract
Aims/hypothesis
Islets or beta cells from Sur1 −/− mice were used to determine whether changes in plasma membrane potential (V m) remain coupled to changes in cytosolic Ca2+ ([Ca2+]i) in the absence of KATP channels and thus provide a triggering signal for insulin secretion. The study also sought to elucidate whether [Ca2+]i influences oscillations in V m in sur1−/− beta cells.
Methods
Plasma membrane potential and ion currents were measured with microelectrodes and the patch–clamp technique. [Ca2+]i was monitored with the fluorescent dye fura-2. Insulin secretion from isolated islets was determined by static incubations.
Results
Membrane depolarisation of Sur1−/− islets by arginine or increased extracellular K+, elevated [Ca2+]i and augmented insulin secretion. Oligomycin completely abolished glucose-stimulated insulin release from Sur1−/− islets. Oscillations in V m were influenced by [Ca2+]i as follows: (1) elevation of extracellular Ca2+ lengthened phases of membrane hyperpolarisation; (2) simulating a burst of action potentials induced a Ca2+-dependent outward current that was augmented by increased Ca2+ influx through L-type Ca2+ channels; (3) Ca2+ depletion of intracellular stores by cyclopiazonic acid increased the burst frequency in Sur1−/− islets, elevating [Ca2+]i and insulin secretion; (4) store depletion activated a Ca2+ influx that was not inhibitable by the L-type Ca2+ channel blocker D600.
Conclusions/interpretation
Although V m is largely uncoupled from glucose metabolism in the absence of KATP channels, increased electrical activity leads to elevations of [Ca2+]i that are sufficient to stimulate insulin secretion. In Sur1−/− beta cells, [Ca2+]i exerts feedback mechanisms on V m by activating a hyperpolarising outward current and by depolarising V m via store-operated ion channels.
Similar content being viewed by others
Introduction
In wild-type mice, glucose-stimulated insulin secretion involves two different mechanisms referred to as triggering and amplifying pathways (reviewed in [1]). The triggering pathway, which is well characterised and comprises closure of ATP-dependent K+ channels (KATP channels), membrane depolarisation and Ca2+ influx through L-type Ca2+ channels, initiates coordinated oscillations of membrane potential (V m), cytosolic free Ca2+ concentration ([Ca2+]i) and insulin secretion [2–6]. Loss of beta cell KATP channels results in persistent Ca2+-dependent electrical activity and elevated [Ca2+]i [7, 8], including oscillation of V m [9]. In humans, impairment of the triggering pathway by loss-of-function mutations in either the Kir6.2 or the SUR1 genes encoding the KATP channel subunits [10] results in a severe disregulation of glucose homeostasis known as congenital hyperinsulinism [11–13], while gain-of-function mutations in Kir6.2 can produce neonatal diabetes [14]. The knock-out mouse models are only mildly glucose-intolerant [7, 8, 15] pointing to activation of compensatory mechanisms. Recent studies suggest that excessive secretion of insulin may be prevented by a reduced sensitivity of Sur1−/− beta cells to incretins [8, 16, 17]. In addition, inhibitory signals via the sympathetic nervous system or neuropeptides are still operative. It has been shown that epinephrine and galanin could hyperpolarise V m in sur1−/− beta cells [9, 18]. Thus these mechanisms may counterbalance the loss of KATP channel-mediated regulation. Several groups have reported that glucose stimulation of insulin release is reduced in Sur1−/− mice [8, 15] and in their isolated islets [8, 15, 17]. Some have argued for a compensatory increase in sensitivity to cholinergic stimulation [8, 19] and/or amino acid stimulation [20, 21] contributing to the euglycaemia observed in fed animals. A recent report [21] described persistent, elevated insulin secretion in low glucose (1 mmol/l) that was stimulated by high glucose secondary to a transient increase in [Ca2+]i, consistent with an intact amplifying pathway.
Beta cell KATP channels are considered essential for the generation of effective triggering signals, i.e. membrane depolarisation and Ca2+ influx, and have been suggested to underlie V m oscillations [22, 23]. Early studies on isolated Sur1−/− [8, 15, 24] and Kir6.2−/− [7] beta cells described Ca2+-dependent action potentials and elevated, oscillating [Ca2+]i, in the absence of V m oscillations. Subsequent recording from sur1−/− beta cells in intact islets demonstrated V m oscillations [9], but the extent to which changes in membrane potential or [Ca2+]i participate in regulating insulin secretion in the absence of these channels is unclear. Our recent study showing that the neuropeptide galanin terminates not only oscillations of V m, but also decreases [Ca2+]i in sur1−/− beta cells [9] indicates that [Ca2+]i is determined by V m. The aim of the present study was to evaluate the coupling between V m and [Ca2+]i in KATP channel-deficient mice and its influence on insulin secretion.
Wild-type beta cells exhibit a strong glucose dependence on V m that is close to the K+ equilibrium potential at low glucose concentrations, oscillates between 7 and 18 mmol/l and shows continuous electrical activity at higher concentrations [25]. During glucose stimulation transient openings of KATP channels [23, 26, 27] and activation of a small Ca2+-dependent K+ current [28–30] produce hyperpolarised intervals of V m that transiently reduce [Ca2+]i. Interestingly, Sur1−/− beta cells also show oscillations in V m and [Ca2+]i [8, 9]. These oscillations are not driven by glucose metabolism [9]. We therefore investigated whether there is a direct feedback of [Ca2+]i on V m in Sur1−/− beta cells by testing the effect of increased Ca2+ influx through voltage-dependent L-type Ca2+ channels and the influence of store-operated ion channels on V m, [Ca2+]i and insulin secretion.
Material and methods
Cell and islet preparation
Experiments were performed using islets, clusters or single pancreatic beta cells isolated from fed C57BL/6 (Charles River, Sulzfeld, Germany) or Sur1−/− (breeding facility of the Dept of Pharmacology, University of Tübingen, Germany) mice that had been killed by cervical dislocation or CO2. For measurements of cell membrane potential with microelectrodes, a piece of pancreas was fixed in a perifusion chamber and islets were microdissected by hand. Other experiments were performed with islets isolated by collagenase digestion. For generation of clusters or single cells islets were dispersed in Ca2+-free medium and cultured for up to 4 days in RPMI 1640 medium (11.1 mmol/l glucose) supplemented with 10% fetal calf serum, 100 U/ml penicillin and 100 μg/ml streptomycin [31]. The principles of laboratory animal care (NIH publication nos. 85–23, revised 1985) and German laws were followed.
Solutions and chemicals
Cell membrane potential and current patch–clamp recordings were done with amphotericin B (250 μg/ml) in the pipette solution which contained: 10 mmol/l KCl, 10 mmol/l NaCl, 70 mmol/l K2SO4, 4 mmol/l MgCl2, 2 mmol/l CaCl2, 10 mmol/l EGTA, 5 mmol/l HEPES, pH 7.15 adjusted with KOH. The bath solution contained: 140 mmol/l NaCl, 3.6 mmol/l KCl, 2 mmol/l NaHCO3, 0.5 mmol/l NaH2PO4, 0.5 mmol/l MgSO4, 1 mmol/l CaCl2, 15 mmol/l glucose, 5 mmol/l HEPES, pH 7.4 adjusted with NaOH. [Ca2+]i was determined in a bath solution containing: 140 mmol/l NaCl, 5 mmol/l KCl, 1.2 mmol/l MgCl2, 2.5 mmol/l CaCl2, 15 mmol/l glucose, 10 mmol/l HEPES, pH 7.4 adjusted with NaOH. Cell membrane potential measurements with intracellular microelectrodes were done in a bath solution containing: 120 mmol/l NaCl, 5 mmol/l KCl, 2.5 mmol/l CaCl2, 1.2 mmol/l MgCl2, 24 mmol/l NaHCO3, 15 mmol/l glucose, gassed with 95% O2 and 5% CO2 to maintain a pH of 7.4. The incubation medium for determining insulin secretion contained (in mmol/l): 122 NaCl, 4.8 KCl, 2.5 CaCl2, 1.1 MgCl2, 10 HEPES, 0.5% bovine serum albumin, pH 7.4.
Fura-2AM was obtained from Molecular Probes (Eugene, OR, USA). RPMI 1640 medium was from PromoCell (Heidelberg, Germany), penicillin/streptomycin was from GIBCO/BRL (Karlsruhe, Germany). All other chemicals were purchased from Sigma (Deisenhofen, Germany) and Merck (Darmstadt, Germany) in the purest form available.
Patch–clamp recordings
Patch pipettes were pulled from borosilicate glass capillaries (Clark, Pangbourne, UK) and had resistances between 3 and 5 MΩ when filled with pipette solution. Membrane currents and potentials were recorded at 32°C with an EPC-9 patch–clamp amplifier using ‘Pulse’ software (HEKA, Lambrecht, Germany) in the voltage-clamp or current-clamp mode respectively. Measurement of I K,slow currents was done using a modified protocol described by Göpel et al. [28]: After a depolarising step from −70 to −40 mV, a train of 26 voltage ramps (−40 to 0 to −40 mV within 200 ms) was applied. This train of simulated action potentials was followed by a period of at least 10 s at −40 mV prior to a voltage step back to −70 mV. Data were analysed with ‘Chart’ software (ADInstruments, Spechbach, Germany).
Membrane potential measurements with microelectrodes
V m was determined at 37°C with high-resistance microelectrodes [25], except for the data in Fig. 4 where the perforated-patch configuration was used. Beta cells from Sur1−/− islets were discriminated from non-beta cells by their lack of Na+ action potentials and the opposite glucose dependence of their electrical activity [32].
Measurement of [Ca2+]i
The cytosolic free Ca2+ concentration ([Ca2+]i) was measured at 37°C in single cells or small clusters by the fura-2 method according to Grynkiewicz et al. [33] using equipment and software from TILL photonics (Gräfelfing, Germany). Cells were identified as beta cells when [Ca2+]i was not decreased by 15 mmol/l glucose, as described for alpha cells [34]. The cells were loaded with fura-2AM (5 μmol/l) for 30 min at 37°C. Intracellular fura-2 was excited alternately at 340 nm or 380 nm by means of an oscillating diffraction grating. The excitation light was directed through the objective (PlanNeofluar ×40 objective, Zeiss, Stuttgart, Germany) by means of a glass fibre light guide and a dichroic mirror. The emitted light was filtered (LP515 nm) and measured by a digital camera. The ratio of the emitted light intensity at 340 nm/380 nm excitation was used to calculate [Ca2+]i following an in vitro calibration with fura-2 K+-salt.
Measurement of insulin secretion
Batches of five islets were incubated for 60 min at 37°C with the indicated substances. Insulin was determined by radioimmunoassay using rat insulin (Crystal Chem, Downers Grove, IL, USA) as the standard.
Presentation of results
Electrophysiological and [Ca2+]i experiments are illustrated by recordings representative of the indicated number of experiments carried out with different cells. At least three different cell preparations were used for each series of experiments. Where possible the means±SEM are given in the text for the indicated number of experiments. In microelectrode experiments recordings during the 4 to 6 min prior to changes in glucose concentration were analysed. The statistical significance of differences between means was assessed by a one sample t-test or Student’s t-test for paired values when two samples were compared; multiple comparisons were made by ANOVA followed by Student–Newman–Keuls test. A p value of less than 0.05 was considered significant.
Results
Influence of membrane depolarisation on [Ca2+]i and insulin secretion in Sur1−/− beta cells
To investigate whether [Ca2+]i is controlled by membrane potential, pancreatic beta cells devoid of KATP channels were depolarised by 10 mmol/l arginine or 30 mmol/l K+ respectively. V m recordings from intracellular microelectrodes in islets perfused with 15 mmol/l glucose displayed regular oscillations (slow waves) as described recently [9]. The addition of arginine (Fig. 1a) or an increase in extracellular K+ (Fig. 1c) resulted in depolarisation of V m; continuous Ca2+ action potentials were present when arginine was added. The depolarising agents terminated oscillations in [Ca2+]i by inducing a biphasic rise in [Ca2+]i with an initial peak followed by an increased steady-state level (Fig. 1b and d).
Influence of 10 mmol/l arginine (a, b) and 30 mmol/l K+ (c, d) on V m (a, c) and [Ca2+]i (b, d) in Sur1−/− beta cells. Experiments were done in 15 mmol/l glucose (15G). V m was determined with intracellular microelectrodes. In the presence of 10 mmol/l arginine (a) or 30 mmol/l K+ (c) oscillations of V m were terminated and the plasma membrane was persistently depolarised, displaying continuous Ca2+ action potentials in the presence of arginine. Oscillations of [Ca2+]i (b, d) were also abrogated by addition of the depolarising agents that induced a biphasic rise of [Ca2+]i with an initial peak followed by a plateau phase with steadily elevated [Ca2+]i. The recordings are representative of four (a), eleven (b), five (c) and ten (d) experiments
On average, the fraction of plateau phase (FOPP; percentage of time when the cell membrane is depolarised) increased from 44±6% to 100% after addition of arginine (p≤0.01, n=4) and from 37±4% to 100% after elevation of extracellular K+ (p≤0.001, n=5) respectively. Under control conditions (15 mmol/l glucose) [Ca2+]i oscillated between a peak value of 378±31 nmol/l and a nadir of 66±8 nmol/l (n=12). Application of 10 mmol/l arginine induced a peak increase in [Ca2+]i of 614±41 nmol/l followed by a plateau of 293±32 nmol/l (n=11). With 30 mmol/l K+ [Ca2+]i reached a peak value of 705±46 nmol/l and a sustained plateau of 339±20 nmol/l (n=10).
Insulin release from Sur1−/− islets was augmented when the glucose concentration was increased from 0.5 up to 40 mmol/l (Fig. 2a). Insulin secretion in 0.5 and 3 mmol/l glucose was significantly lower compared to 15 mmol/l glucose (G0.5: 0.23±0.05 ng·h−1·islet−1, n=6; G3: 0.24±0.06 ng·h−1·islet−1, n=5; G15: 0.48±0.06 ng·h−1·islet−1, n=6; p≤0.05). Stimulation with 25 mmol/l or 40 mmol/l glucose increased insulin release to 0.67±0.08 ng·h−1·islet−1 (n=5) or 0.74±0.11 ng·h−1·islet−1 (n=5; p≤0.05) respectively. Addition of arginine (10 mmol/l) or K+ (30 mmol/l) in the presence of 15 mmol/l glucose resulted in a rise in secretion consistent with increased Ca2+ influx acting as a stimulus for exocytosis. On average, insulin release was elevated from 0.48±0.06 (15 mmol/l glucose, n=6) to 1.10±0.14 ng·h−1·islet−1 by 10 mmol/l arginine (n=5; p≤0.01 compared to 15 mmol/l glucose) and to 1.02±0.10 ng·h−1·islet−1 by 30 mmol/l K+ (p≤0.001 compared to 15 mmol/l glucose n=5–6). Glucose-induced insulin release was also determined in wild-type islets. Basal secretion of wild-type islets (0.5 mmol/l glucose) was significantly lower, but stimulation with 15 or 40 mmol/l glucose potentiated the secretory response much more efficiently compared to Sur1−/− islets. The increase from 0.5 to 15 mmol/l glucose induced a 2-fold vs 7-fold elevation of insulin secretion in Sur1−/− and wild-type mice respectively. On average, insulin release in wild-type islets was elevated from 0.06±0.02 (0.5 mmol/l glucose, n=8; p≤0.01 compared to Sur1−/− islets) to 0.43±0.06 ng·h−1·islet−1 by 15 mmol/l glucose and to 0.64±0.08 ng·h−1·islet−1 by 40 mmol/l glucose (n=8; p≤0.001 and n=3; p≤0.05 compared to 15 mmol/l glucose in wild-type islets respectively). Insulin content amounted to 27.4±1.9 ng/islet in Sur1−/− and 26.8±1.5 ng/islet in wild-type islets (n=4 and n=8 independent preparations respectively).
Insulin secretion of isolated Sur1−/− islets with different glucose concentrations, depolarising agents and inhibition of glucose metabolism. Batches of five islets were incubated with the indicated substances for 60 min. a Insulin release was increased by elevating the glucose concentration. Compared with 15 mmol/l glucose (15G), insulin secretion in 0.5 (0.5G) or 3 mmol/l (3G) glucose was significantly lower, whereas increasing the glucose concentration to 40 mmol/l (40G) significantly increased secretion. The addition of 10 mmol/l arginine or 30 mmol/l K+ to Sur1−/− islets already stimulated with 15 mmol/l glucose led to a further rise in insulin release. *p≤0.05; **p≤0.01; ***p≤0.001 vs 15 mmol/l glucose. b The inhibition of mitochondrial ATP production by 2 μg/ml oligomycin had no effect on Sur1−/− islets incubated in 0.5 mmol/l glucose (0.5G), but decreased insulin release in islets stimulated with 15 mmol/l glucose (15G). Throughout this series of experiments 30 mmol/l K+ (30 K +) was present. **p≤0.01 vs 15 mmol/l glucose + 30 mmol/l K+. Insulin secretion was calculated as ng·h−1·islet−1±SEM of five to six independent series of experiments with different preparations
The contribution of ATP production to glucose-stimulated insulin secretion of Sur1−/− islets was assessed by inhibiting mitochondrial ATP production in the presence of 30 mmol/l K+ to depolarise V m and maintain elevated [Ca2+]i. Oligomycin (2 μg/ml) had only marginal effects on basal insulin secretion in 0.5 mmol/l glucose, but significantly lowered exocytosis from islets stimulated with 15 mmol/l glucose (Fig. 2b). On average, in 15 mmol/l glucose and 30 mmol/l K+ insulin release was 0.92±0.09 ng·h−1·islet−1 in the absence, versus 0.31±0.06 ng·h−1·islet−1 in the presence of oligomycin (p≤0.01; n=6 ).
Effect of Ca2+ influx on membrane potential and ion currents in Sur1−/− beta cells
In wild-type beta cells, changes in external Ca2+ concentration, which are assumed to determine [Ca2+]i, play a crucial role in the regulation of membrane potential oscillations. The influence of increased Ca2+ influx on V m oscillations in Sur1−/− beta cells was investigated with intracellular microelectrodes. Figure 3 shows that elevation of the extracellular Ca2+ concentration from 2.5 to 10 mmol/l markedly altered the pattern of oscillations. FOPP was reduced from 32±3% to 23±4% (p≤0.05; n=11). The average burst duration was not significantly changed, while the length of the interburst phase was increased from 62±7 s to 143±29 s (p≤0.05; n=11), consistent with the induction of a Ca2+-dependent hyperpolarising current.
Hyperpolarising effect of a rise in the extracellular Ca2+ concentration in Sur1−/− islets. Experiments were performed with intracellular microelectrodes. Increasing the extracellular Ca2+ concentration from 2.5 to 10 mmol/l decreased the fraction of the plateau phase and increased the length of interburst phases, indicating activation of a hyperpolarising ion current. The recording is representative of 11 experiments
To characterise this hyperpolarising current induced in Sur1−/− beta cells by increased Ca2+ influx, ion currents, were recorded in the perforated-patch configuration. As described previously [9, 15], single, cultured Sur1−/− beta cells are persistently depolarised and show slow waves of [Ca2+]i in the absence of V m oscillations. Stimulation of Sur1−/− beta cells with simulated bursts of action potentials, following the protocol described by Göpel et al. [Fig. 4a; 28], elicited a small outward current that could be inhibited by D600, an L-type Ca2+ channel blocker (Fig. 4b). This outward current amounted to 5.00±0.64 pA (n=20) and was reduced to 0.03±0.41 pA in the presence of 50–100 μmol/l D600 (p≤0.01; n=4). Figure 4c shows that BayK 8644, an L-type Ca2+ channel opener in beta cells [35], significantly increased the Ca2+-dependent outward current (3.67±0.46 pA without BayK 8644 vs 10.66±2.07 pA after the addition of 1 μmol/l BayK 8644; p≤0.01; n=13). In Fig. 4d the effect of BayK 8644 on V m was measured in isolated patch-clamped Sur1−/− beta cells. Prior to the addition of BayK 8644 persistent Ca2+ action potentials occurred. Application of BayK 8644 hyperpolarised the beta cell membrane potential by ∼8 mV (−49±1 mV vs an interburst potential of −57±2 pA in 0.5–1 μmol/l BayK 8644; p≤0.001; n=18) converting the continuous Ca2+ action potentials, characteristic of single Sur1−/− beta cells [9, 15], to an oscillatory pattern. This pattern was remotely reminiscent of the slow waves seen in whole islets, but with a much higher frequency. However, as already mentioned above, electrical activity of isolated beta cells markedly differs from whole islets, so that the frequency of oscillations cannot be directly compared.
Activation of Ca2+-dependent ion currents in isolated Sur1−/− beta cells. Experiments were performed in the perforated-patch configuration. The bath solution contained 15 mmol/l glucose (15G) in all experiments. a Pulse protocol for activation of ion currents recorded in (b) and (c). The pulse protocol consisted of a depolarising step from −70 to −40 mV, followed by 26 voltage ramps from −40 to 0 mV and vice versa. b, c The simulated burst of action potentials induced an outward current that was completely prevented by 100 μmol/l D600. The application of 1 μmol/l of the L-type Ca2+-channel opener BayK 8644 (c) significantly elevated the outward current. d The increased outward current in the presence of BayK 8644 coincided with hyperpolarisation of V m. Current measurements were representative of 20 with 15G, four with D600 (b) and 13 with BayK 8644 (c). The recording of V m (d) was representative of 13 experiments with similar results
Regulation of membrane potential oscillations, [Ca2+]i and insulin secretion by intracellular Ca2+ stores
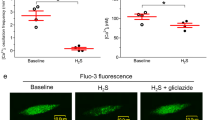
In wild-type beta cells Ca2+ uptake and release from intracellular stores is known to influence V m via changes in [Ca2+]i [36, 37]. Figure 5a shows that the addition of 10 μmol/l cyclopiazonic acid (CPA), a reversible inhibitor of ATP-dependent Ca2+ uptake into the endoplasmic reticulum [38], significantly increased the frequency of V m oscillations and shortened the duration of the interburst phase (frequency=0.43±0.03 vs 1.06±0.06 bursts/min in 10 μmol/l CPA, p≤0.001, n=6; interburst intervals=97±25 s vs 27±4 s, p≤0.05, n=5; FOPP=44±7% vs 58±5%, p≤0.05, n=5). CPA increased [Ca2+]i consistent with coupling of V m and [Ca2+]i in Sur1−/− beta cells (Fig. 5b) and increased insulin secretion from Sur1−/− islets stimulated with 15 mmol/l glucose (Fig. 5c). To quantify the effect of CPA on [Ca2+]i the area under the curve, AUC[Ca2+]i, was calculated for 5 min prior to changing the bath solution. In 10 μmol/l CPA the AUC[Ca2+]i increased by 3895±897 nmol·l−1·min−1 (p≤0.01; n=12) corresponding to an elevation of ~52% compared to the value in 15 mmol/l glucose. Insulin secretion increased from 0.45±0.14 ng·h−1·islet−1 in 15 mmol/l glucose to 0.63±0.17 ng·h−1·islet−1 in 15 mmol/l glucose plus 10 μmol/l CPA (p≤0.05; n=5).
Influence of store depletion on V m, [Ca2+]i and insulin release in Sur1−/− islets. Intracellular Ca2+ stores were emptied by 10 μmol/l cyclopiazonic acid (CPA). a Determination of V m with intracellular microelectrodes showed that addition of CPA accelerated burst frequency and decreased interburst intervals. b [Ca2+]i of isolated clusters displayed regular oscillations in the presence of 15 mmol/l glucose. After application of CPA, [Ca2+]i was elevated and oscillation frequency increased. The traces are representative of five (a), and 12 (b) experiments. c Isolated Sur1−/− islets were incubated with 0.5 mmol/l glucose (0.5G), 15 mmol/l glucose (15G) and 15 mmol/l glucose + 10 μmol/l CPA for 60 min. Compared to 0.5 mmol/l glucose, insulin secretion was stimulated by 15 mmol/l glucose and further increased in the presence of CPA. The diagram shows the average insulin release±SEM of five independent experiments with different preparations. *p≤0.05 vs 15 mmol/l glucose
The results with CPA suggest that Ca2+ store depletion can activate a depolarising current that counteracts the hyperpolarising current maintaining the interburst phases. To determine the contribution of Ca2+ influx via store-operated channels, L-type Ca2+ channels were inhibited by D600 in the presence of CPA. Figure 6 shows that addition of 100 μmol/l D600 immediately abrogated oscillations and drastically decreased [Ca2+]i. [Ca2+]i could be reduced further by omission of extracellular Ca2+ (Fig. 6a, arrowhead), but the effect was marginal in the absence of CPA (Fig. 6b, arrowhead). Omission of extracellular Ca2+ in the presence of CPA and D600, decreased [Ca2+]i by 34±4 nmol/l vs 8±1 nmol/l (p≤0.001; n=8) in D600 alone. This series of experiments was also performed with thapsigargin, another potent inhibitor of sarcoplasmic Ca2+ ATPases, leading to similar results: with 1 μmol/l thapsigargin plus 100 μmol/l D600, [Ca2+]i was reduced by 33±3 nmol/l after omission of extracellular Ca2+ (n=3; not shown).
Activation of Ca2+ influx by store depletion of Sur1−/− beta cells. Blockage of L-type Ca2+ channels by 100 μmol/l D600 terminated oscillations and decreased [Ca2+]i (a, b). In cells treated with 10 μmol/l CPA (a), the omission of extracellular Ca2+ further reduced [Ca2+]i. This reduction was significantly greater than in the absence of CPA (b). The recordings represent eight experiments with and eight experiments without CPA
Discussion
In contrast to what has been observed in beta cells from patients with congenital hyperinsulinism, several studies from KATP-channel-deficient mice [7, 8, 15] have shown that the loss of these channels, which play a key role in the triggering pathway of insulin secretion, does not result in hyperinsulinaemic hypoglycaemia. This implies that ablation of KATP channels in mice leads to compensatory mechanisms that allow for the maintenance of euglycemia. The observation that isolated sur1−/− beta cells were persistently depolarised while [Ca2+]i oscillated [8, 15], suggested that the coupling between V m and [Ca2+]i was disrupted in murine KATP-channel-deficient beta cells [8]. By contrast, we have demonstrated regular oscillations in beta cells when V m measurements were done on intact sur1−/− islets [9], suggesting V m is involved in the regulation of intracellular Ca2+ homeostasis. The present study extends this analysis showing that V m and [Ca2+]i are closely coupled in Sur1−/− beta cells. Arginine or high extracellular K+ abrogate V m oscillations, depolarise the beta cell membrane and provide a strong triggering signal for Ca2+ influx [Figs. 1 and 2], which further increases insulin release from Sur1−/− islets incubated with 15 mmol/l glucose (Fig. 2a).
Several studies demonstrate that insulin secretion from Sur1−/− islets remains sensitive to glucose stimulation, although the sensitivity appears reduced [8, 15, 17, 21]. We show that secretion from Sur1−/− islets can be elevated over a broad range of glucose concentrations (0.5–40 mmol/l; Fig. 2a). One prerequisite for exocytosis is the activation of mitochondrial ATP synthesis, and oligomycin completely suppressed glucose-stimulated insulin secretion under conditions where [Ca2+]i was elevated by application of 30 mmol/l K+ (Fig. 2b). This agrees with the recent report that elevated insulin secretion from sur1−/− islets can be suppressed with NaN3 [21]. Nenquin et al. [21] largely ascribed the regulatory role of glucose to an effective amplifying pathway, but found that elevating glucose induced an unexpected transient rise in [Ca2+]i. Together with our previous observation that oscillations of V m and [Ca2+]i were modified by glucose [9], this suggests a V m/[Ca2+]i-dependent pathway that contributes to glucose-regulated exocytosis in Sur1−/− mice.
In wild-type beta cells, repetitive activation of KATP channels, due to Ca2+-induced changes in the ATP:ADP ratio, contributes to the maintenance of V m oscillations [23, 26]. In addition, it has been shown that increased Ca2+ influx can induce hyperpolarisation of V m that is not mediated by KATP channels [39] and that a small Ca2+-dependent K+ current, referred to as I K,slow, is activated when [Ca2+]i is increased in response to simulated bursts of action potentials [28, 30]. As I K,slow in wild-type beta cells contains a tolbutamide-resistant component of ∼52% of the K+ current induced by a train of depolarisations [29], we examined this component in Sur1−/− beta cells. Application of a train of depolarising pulses revealed an outward current of ∼5 pA that was inhibited by D600 and potentiated by BayK 8644 (Fig. 4b, c). V m was significantly hyperpolarised by BayK 8644, demonstrating that the outward current was sufficient to interrupt the persistent depolarisation observed in isolated Sur1−/− beta cells (Fig. 4d). Together with the observation that an increase in extracellular Ca2+ markedly prolonged the interburst phase of V m in microelectrode experiments (Fig. 3), our data strongly support the view that the interplay between Ca2+ influx and activation of Ca2+-dependent K+ channels constitutes a feedback loop that maintains V m oscillations in KATP-channel-deficient islets. Whether the conductance we describe for Sur1−/− beta cells is identical with the tolbutamide-insensitive component of I K,slow as well as detailed characterisation of the underlying ion channel(s) remain subjects for further investigation.
A second mechanism that can influence intracellular Ca2+ dynamics is based on ATP-dependent Ca2+ sequestration by the endoplasmic reticulum (ER). Previous studies in wild-type beta cells demonstrated that emptying intracellular stores depolarised V m and affected the amplitude and frequency of oscillations in [Ca2+]i [36, 37, 40]. Our data show that V m in Sur1−/− beta cells is responsive to changes in Ca2+ stores. Store depletion with the SERCA-blocker CPA led to an increase in burst frequency that was coupled to elevated Ca2+ influx (Fig. 5a, b). The CPA-induced Ca2+ influx was resistant to D600 but sensitive to extracellular Ca2+ (Fig. 6), which is consistent with the activation of store-operated channels as described previously for wild-type beta cells [41]. We suggest that this store-operated depolarising current is sufficient to promote membrane depolarisation and thus increase the frequency of V m oscillations. Consistent with the idea that the V m/[Ca2+]i-dependent pathway is KATP-channel-independent, we were able to demonstrate that the CPA-induced increase in [Ca2+]i stimulated insulin secretion (Fig. 5c).
Our data show that the coupling of V m and [Ca2+]i can determine insulin secretion in Sur1−/− beta cells. This illustrates that signals of a triggering pathway exist in the absence of functional KATP channels. The central role in regulation of V m is provided by [Ca2+]i. Dependent on the origin of the [Ca2+]i increase, Ca2+ exerts a feedback on V m by activating depolarising and hyperpolarising ion currents that maintain membrane potential oscillations in beta cells of KATP-channel-deficient mice.
Abbreviations
- CPA:
-
cyclopiazonic acid
- [Ca2+]i :
-
cytosolic free calcium concentration
- FOPP:
-
fraction of plateau phase
- KATP :
-
channel ATP-dependent K+ channel
- Kir6.2:
-
inward rectifying K+ channel type 6.2
- SUR1:
-
sulphonylurea receptor type 1
- Vm :
-
plasma membrane potential
References
Henquin JC (2000) Triggering and amplifying pathways of regulation of insulin secretion by glucose. Diabetes 49:1751–1760
Ashcroft F, Rorsman P (1989) Electrophysiology of the pancreatic β-cell. Prog Biophys Mol Biol 54:87–143
Santos RM, Rosario LM, Nadal A, Garcia-Sancho J, Soria B, Valdeolmillos M (1991) Widespread synchronous [Ca2+]i oscillations due to bursting electrical activity in single pancreatic islets. Pflügers Arch-Eur J Physiol 418:417–422
Gilon P, Shepherd RM, Henquin JC (1993) Oscillations of secretion driven by oscillations of cytoplasmic Ca2+ as evidenced in single pancreatic islets. J Biol Chem 268:22265–22268
Hellman B, Gylfe E, Bergsten P et al (1994) Glucose induces oscillatory Ca2+ signalling and insulin release in human pancreatic beta cells. Diabetologia 37(Suppl 2):S11–S20
Zhou Z, Misler S (1996) Amperometric detection of quantal secretion from patch–clamped rat pancreatic β-cells. J Biol Chem 271:270–277
Miki T, Nagashima K, Tashiro F et al (1998) Defective insulin secretion and enhanced insulin action in KATP channel-deficient mice. Proc Natl Acad Sci U S A 95:10402–10406
Shiota C, Larsson O, Shelton KD et al (2002) Sulfonylurea receptor type 1 knock-out mice have intact feeding-stimulated insulin secretion despite marked impairment in their response to glucose. J Biol Chem 277:37176–37183
Düfer M, Haspel D, Krippeit-Drews P, Aguilar-Bryan L, Bryan J, Drews G (2004) Oscillations of membrane potential and cytosolic Ca2+ concentration in SUR1−/− beta cells. Diabetologia 47:488–498
Inagaki N, Gonoi T, Clement JP IV et al (1995) Reconstitution of IKATP: an inward rectifier subunit plus the sulfonylurea receptor. Science 270:1166–1170
Aguilar-Bryan L, Bryan J (1999) Molecular biology of adenosine triphosphate-sensitive potassium channels. Endocr Rev 20:101–135
Straub SG, Cosgrove KE, Ämmälä C et al (2001) Hyperinsulinism of infancy—the regulated release of insulin by KATP channel-independent pathways. Diabetes 50:329–339
Dunne MJ, Cosgrove KE, Shepherd RM, Aynsley-Green A, Lindley KJ (2004) Hyperinsulinism in infancy: from basic science to clinical disease. Physiol Rev 84:239–275
Gloyn AL, Pearson ER, Antcliff JF et al (2004) Activating mutations in the gene encoding the ATP-sensitive potassium-channel subunit Kir6.2 and permanent neonatal diabetes. N Engl J Med 350:1817–1818
Seghers V, Nakazaki M, DeMayo F, Aguilar-Bryan L, Bryan J (2000) SUR1 knockout mice. A model for KATP channel-independent regulation of insulin secretion. J Biol Chem 275:9270–9277
Nakazaki M, Crane A, Hu M, Seghers V, Ullrich S, Aguilar-Bryan L, Bryan J (2002) cAMP-activated protein kinase-independent potentiation of insulin secretion by cAMP is impaired in SUR1 null islets. Diabetes 51:3440–3449
Eliasson L, Ma X, Renström E et al (2003) SUR1 regulates PKA-independent cAMP granule priming in mouse pancreatic B-cells. J Gen Physiol 121:181–197
Sieg A, Su J, Buchenau M et al (2004) Epinephrine-induced hyperpolarization of islet cells without KATP channels. Am J Physiol Endocrinol Metab 286:E463–E471
Doliba NM, Quin W, Vatamaniuk MZ et al (2004) Restitution of defective glucose-stimulated insulin release of sulfonylurea type 1 receptor knockout mice by acetylcholine. Am J Physiol Endocrinol Metab 286:E834–E843
Li C, Buettger C, Kwagh J et al (2004) A signaling role of glutamine in insulin secretion. J Biol Chem 279:13393–13401
Nenquin M, Szollosi A, Aguilar-Bryan L, Bryan J, Henquin JC (2004) Both triggering and amplifying pathways contribute to fuel-induced insulin secretion in the absence of sulfonylurea receptor-1 in pancreatic β-cells. J Biol Chem 279:32316–32324
Cook DL, Satin LS, Hopkins WF (1991) Pancreatic B cells are bursting, but how? Trends Neurosci 149:411–414
Rolland JF, Henquin JC, Gilon P (2002) Feedback control of the ATP-sensitive K+ current by cytosolic Ca2+ contributes to oscillations of the membrane potential in pancreatic β-cells. Diabetes 51:376–384
Ämmälä C, Dukes ID, Gengo P et al (2000) Spontaneous oscillations in cytosolic calcium in islets from knockout mice lacking the sulphonylurea receptor-1 (SUR1). Diabetes 49(Suppl 1):A62 (Abstract)
Meissner HP, Schmelz H (1974) Membrane potential of beta-cells in pancreatic islets. Pflügers Arch-Eur J Physiol 351:195–206
Krippeit-Drews P, Düfer M, Drews G (2000) Parallel oscillations of intracellular calcium activity and mitochondrial membrane potential in mouse pancreatic B-cells. Biochem Biophys Res Commun 267:179–183
Kindmark H, Köhler M, Brown G, Bränström R, Larsson O, Berggren PO (2001) Glucose-induced oscillations in cytoplasmic free Ca2+ concentration precede oscillations in mitochondrial membrane potential in the pancreatic beta-cell. J Biol Chem 276:34530–34536
Göpel SO, Kanno T, Barg S, Eliasson L, Galvanovskis J, Renström E, Rorsman P (1999) Activation of Ca2+-dependent K+ channels contributes to rhythmic firing of action potentials in mouse pancreatic β-cells. J Gen Physiol 114:759–769
Kanno T, Rorsman P, Göpel SO (2002) Glucose-dependent regulation of rhythmic action potential firing in pancreatic beta-cells by KATP-channel modulation. J Physiol 545:501–507
Goforth PB, Bertram R, Khan FA, Zhang M, Sherman A, Satin LS (2002) Calcium-activated K+ channels of mouse β-cells are controlled by both store and cytoplasmic Ca2+: experimental and theoretical studies. J Gen Physiol 120:301–322
Plant TD (1988) Properties and calcium-dependent inactivation of calcium currents in cultured mouse pancreatic B-cells. J Physiol 404:731–747
Barg S, Galvanovskis J, Göpel SO, Rorsman P, Eliasson L (2000) Tight coupling between electrical activity and exocytosis in mouse glucagon-secreting α-cells. Diabetes 49:1500–1510
Grynkiewicz G, Poenie M, Tsien RY (1985) A new generation of Ca2+ indicators with greatly improved fluorescence properties. J Biol Chem 260:3440–3450
Nadal A, Quesada I, Soria B (1999) Homologous and heterologous asynchronicity between identified α-, β- and δ-cells within intact islets of Langerhans in the mouse. J Physiol 517:85–93
Rorsman P, Ashcroft FM, Trube G (1988) Single Ca channel currents in mouse pancreatic B-cells. Pflügers Arch-Eur J Physiol 412:597–603
Worley JF III, McIntyre MS, Spencer B, Mertz RJ, Roe MW, Dukes ID (1994) Endoplasmic reticulum calcium store regulates membrane potential in mouse islet β-cells. J Biol Chem 269:14359–14362
Arredouani A, Henquin JC, Gilon P (2002) Contribution of the endoplasmic reticulum to the glucose-induced [Ca2+]i response in mouse pancreatic islets. Am J Physiol Endocrinol Metab 282:E982–E991
Seidler NW, Jona I, Vegh M, Martonosi A (1989) Cyclopiazonic acid is a specific inhibitor of the Ca2+-ATPase of sarcoplasmic reticulum. J Biol Chem 264:17816–17823
Rosário LM, Barbosa RM, Antunes CM, Silva AM, Abrunhosa AJ, Santos RM (1993) Bursting electrical activity in pancreatic β-cells: evidence that the channel underlying the burst is sensitive to Ca2+ influx through L-type Ca2+ channels. Pflügers Arch-Eur J Physiol 424:439–447
Liu YJ, Grapengiesser E, Gylfe E, Hellmann B (1995) Glucose induces oscillations of cytoplasmic Ca2+, Sr2+ and Ba2+ in pancreatic beta-cells without participation of the thapsigargin-sensitive store. Cell Calcium 18:165–173
Miura J, Henquin JC, Gilon P (1997) Emptying of intracellular Ca2+ stores stimulates Ca2+ entry in mouse pancreatic beta-cells by both direct and indirect mechanisms. J Physiol 503:387–398
Acknowledgements
This work was supported by grants from the Deutsche Forschungsgemeinschaft (Dr225/6-1 and Du425/1-1) and the U.S. National Institute of Health (DK5277 and DK57671 to L. Aguilar-Bryan). We thank Mrs Isolde Breuning for skilful technical assistance.
Duality of interest.
There was no duality of interest in this study.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Haspel, D., Krippeit-Drews, P., Aguilar-Bryan, L. et al. Crosstalk between membrane potential and cytosolic Ca2+ concentration in beta cells from Sur1 −/− mice. Diabetologia 48, 913–921 (2005). https://doi.org/10.1007/s00125-005-1720-8
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00125-005-1720-8