Abstract
Background
This study aimed to analyse the feasibility and acute toxicity of radical hypo-fractionated radiotherapy (RT) for elderly patients with non-small-cell lung cancer (NSCLC).
Patients and methods
We conducted a retrospective evaluation of treatment with volumetric modulated arc therapy (VMAT) of elderly patients affected by stage III inoperable NSCLC. The dose prescription was 56 Gy in 20 fractions, 55 Gy in 22 fractions, or 50 Gy in 20 fractions. Target volume included only the primary lesion and the infiltrated lymph nodes. The primary end point was acute and late toxicity, while secondary end points were progression-free survival (PFS), and overall survival (OS).
Results
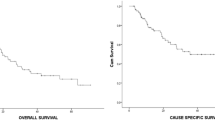
In all, 41 patients were included in this analysis. The mean age of the patients was 78.6 years, and 22 patients had staged IIIA while 19 patients had stage IIIB disease. All but one patient had pathological nodal involvement; 15 patients received chemotherapy before RT. Acute grade 1–2 toxicity was recorded in 25 (61%) patients. Late toxicity was recorded in 13 (32%) patients. No cases of G3 or G4 toxicity were recorded. Complete response was obtained in two (5%) patients, 26 (63%) showed a partial response, and two (5%) experience disease progression. At a mean follow-up of 9.9 months (range, 1.1–25.4), 17 patients had died from disease progression, one died from other causes, and 23 were alive. Median OS was 13.7 ± 1.5 months (95% CI: 10.7–16.7), OS at 12 and 18 months was 51.3 ± 9.5% and 35.1 ± 10.1%, respectively. Median PFS was 13.7 ± 2.3 months (95% CI: 9.1–18.2), and PFS at 12 and 18 months was 50.1 ± 9.9% and 38.9 ± 10.4%, respectively.
Conclusion
Radical hypo-fractionated VMAT is a promising treatment for locally advanced NSCLC in the elderly. The use of hypo-fractionated radiotherapy for lung cancer in older patients can be considered a valuable approach, particularly for patients with poor performance status or refusing other treatment approaches.
Zusammenfassung
Hintergrund
Durchführbarkeit und Nebenwirkungen der radikalen hypofraktionierten Radiotherapie (RT) bei älteren Patienten mit nichtkleinzelligem Bronchialkarzinom (NSCLC) wurden analysiert.
Patienten und Methoden
Ältere Patienten mit inoperablem NSCLC im Stadium III wurden mit volumetrischer Arc-Therapie (VMAT) mit 56 Gy Gesamtdosis in 20 Fraktionen (Fx) oder 55 Gy/22 Fx oder 50 Gy/20 Fx behandelt. Primäre Endpunkte waren Akut- und Spättoxizität. Als sekundäre Endpunkte wurden progressionsfreies Überleben (PFS) und Gesamtüberleben (OS) definiert.
Ergebnisse
Es wurden 41 Patienten (Stadium IIIA: n = 22, IIIB: n = 19) in die Analyse eingeschlossen. Das mediane Alter der Patienten betrug 78,6 Jahre. Bis auf einen Patienten wiesen alle histologisch gesicherte Lymphknotenmetastasen auf. Vor der Bestrahlung erhielten 15 Patienten eine Chemotherapie. Akute Nebenwirkungen vom Grad 1–2 wurden bei 25 (61 %) Patienten beobachtet. Bei 13 (32 %) Patienten wurden Spätnebenwirkungen dokumentiert. Es traten keine Nebenwirkungen vom Grad 3 oder 4 auf. Eine komplette Remission wurde bei 2 (5 %) der Patienten, eine partielle bei 26 (63 %) der Patienten dokumentiert. Bei 2 (5 %) Patienten war der Verlauf progredient unter Therapie. Nach einer mittleren Nachbeobachtungszeit von 9,9 (1,1–25,4) Monaten lebten noch 23 Patienten. Es starben 17 (41 %) Patienten infolge einer Tumorprogression, ein Patient infolge einer andere Ursache. Das mediane OS betrug 13,7 ± 1,5 Monate (95%-KI: 10,7–16,7), das 1‑ bzw.1,5-Jahres-OS lag bei 51,3 ± 9,5 % bzw. 35,1 ± 10,1 %. Im Median blieben die Patienten 13,7 ± 2,3 Monate (95 %-KI: 9,1–18,2) progressionsfrei. Das 1‑ bzw. 1,5-Jahres-PFS betrug 50,1 ± 9,9 % bzw. 38,9 ± 10,4 %.
Schlussfolgerung
Die radikale hypofraktionierte VMAT ist ein vielversprechendes Therapiekonzept für ein lokal fortgeschrittenes NSCLC bei älteren Patienten. Der Einsatz der hypofraktionierten Radiotherapie beim Bronchialkarzinom des älteren Patienten kann als nützlicher Ansatz betrachtet werden, insbesondere bei Patienten mit schlechtem Performance-Status oder bei Ablehnung anderer Ansätze.


Similar content being viewed by others
References
Jemal A, Siegel R, Xu J, Ward E (2010) Cancer statistics. CA Cancer J Clin 60:277–300
Owonikoko TK, Ragin CC, Belani CP et al (2007) Lung cancer in elderly patients: An analysis of the surveillance, epidemiology, and end results database. J Clin Oncol 25:5570–5577
Aupérin A, Le Péchoux C, Rolland E et al (2010) Meta-analysis of concomitant versus sequential radiochemotherapy in locally advanced non-small-cell lung cancer. J Clin Oncol 28:2181–2190
Maguire J, Khan I, McMenemin R, O’Rourke N, McNee S, Kelly V, Peedell C, Snee MSOCCAR (2014) A randomised phase II trial comparing sequential versus concurrent chemotherapy and radical hypofractionated radiotherapy in patients with inoperable stage III Non-Small Cell Lung Cancer and good performance status. Eur J Cancer 50:2939–2949
De Ruysscher D, Botterweck A, Dirx M et al (2009) Eligibility for concurrent chemotherapy and radiotherapy of locally advanced lung cancer patients: A prospective, population-based study. Ann Oncol 20:98–102
Martel MK, Ten Haken RK, Hazuka MB et al (1999) Estimation of tumor control probability model parameters from 3‑D dose distributions of non-small cell lung cancer patients. Lung Cancer 24:31–37
Le Chevalier T, Arriagada R, Quoix E et al (1991) Radiotherapy alone versus combined chemotherapy and radiotherapy in nonresectable non-small cell lung cancer: First analysis of a randomized trial in 353 patients. J Natl Cancer Inst 83:417–423
Machtay M, Paulus R, Moughan J et al (2012) Defining local-regional control and its importance in locally advanced non-small cell lung carcinoma: A Radiation Therapy Oncology Group analysis. J Thorac Oncol 7:716–722
Bradley JD, Paulus R, Komaki R et al (2015) Standard-dose versus high-dose conformal radiotherapy with concurrent and consolidation carboplatin plus paclitaxel with or without cetuximab for patients with stage IIIA or IIIB non-small-cell lung cancer (RTOG 0617): A randomised, two-by-two factorial phase 3 study. Lancet Oncol 16:187–199
Fowler JF, Chappell R (2000) Nonsmall cell lung tumors repopulate rapidly during radiation therapy. Int J Radiat Oncol Biol Phys 46:516–517
Mauguen A, Le Pechoux C, Saunders MI et al (2012) Hyperfractionated or accelerated radiotherapy in lung cancer: An individual patient data meta-analysis. J Clin Oncol 30:2788–2797
Scorsetti M, Clerici E, Navarria P, D’Agostino G, Piergallini L, De Rose F, Ascolese A, Tozzi a, Iftode C, Villa E, Comito T, Franzese C, Mancosu P, Tomatis S, Cozzi L (2015) The role of stereotactic body radiation therapy (SBRT) in the treatment of oligometastatic disease in the elderly. Br J Radiol 88:20150111
Scorsetti M, Navarria P, De Rose F, Ascolese A, Cletici E, Franzese C, Lobefalo F, Reggiori G, Mancosu P, Tomatis S, Fogliata A, Cozzi L (2014) Outcome and toxicity profiles in the treatment of locally advanced lung cancer with volumetric modulated arc therapy. Cancer Res Clin Oncol 140:1937–45
Froesch P, Martucci F, Györik S, Dutly AE, Cafarotti S (2014) Management of non-small cell lung cancer in the elderly. Eur J Intern Med 25:888–894
Extermann M, Aapro M, Bernabei R, Cohen HJ, Droz JP, Lichtman S et al (2005) Task Force on CGA of the International Society of Geriatric Oncology. Use of comprehensive geriatric assessment in older cancer patients: Recommendations from the task force on CGA of the International Society of Geriatric Oncology (SIOG). Crit Rev Oncol Hematol 55:241–252
Dillman RO, Herndon J, Seagren SL et al (1996) Improved survival in stage III non-small-cell lung cancer: Seven-year folow-up of cancer and leukemia group B (CALGB) 8433 trial. J Natl Cancer Inst 88:1210–1215
Komaki R, Scott CB, Sause WT et al (1997) Induction cisplatin/vinblastine and irradiation vs. irradiation in unresectable squamous cell lung cancer: Failure patterns by cell type in RTOG 88-08/ECOG 4588. Radiation Therapy Oncology Group. Eastern Cooperative Oncology Group. Int J Radiat Oncol Biol Phys 39:537–544
Bruner DW, Movsas B, Konski A et al (2004) Outcomes research in cancer clinical trial cooperative groups: The RTOG model. Qual Life Res 13:1025–1041
Kale MS, Mhango G, Gomez JE, Sigel K, Smith CB, Bonomi M, Wisnivesky JP (2015) Treatment toxicity in elderly patients with advanced non-small cell lung cancer. Am J Clin Oncol 25784564. doi:10.1097/COC.0000000000000188
Maguire J, Khan I, McNememin R, O’Rourke N et al (2014) SOCCAR: A randomized phase II trial comparing sequential versus concurrent chemotherapy and radical hypofractionated radiotherapy in patients with inoperable stage III non small cell lung cancer and good performance status. Eur J Cancer 50:2939–2949
Kaster TS, Yaremko B, Palma DA, Rodrigues GB (2015) Radical-intent Hypofractionated radiotherapy for locally advanced nonesmall-cell lung cancer: A systematic review of the literature. Clin Lung Cancer 16:71–79
Partridge M, Ramos M, Sardaro A, Brada M (2011) Dose escalation for non small cell lung cancer: analysis and modelling of published literature. Radiother Oncol 99:6–11
Nguyen LN, Komaki R, Allen P, Schea RA, Milas L (1999) Effectiveness of accelerated radiotherapy for patients with inoperable nonesmall cell lung cancer (NSCLC) and borderline prognostic factors without distant metastasis: A retrospective review. Int J Radiat Oncol Biol Phys 44:1053–1056
Sun LM, Leung SW, Wang CJ et al (2000) Concomitant boost radiation therapy for inoperable nonesmall-cell lung cancer: Preliminary report of a prospective randomized study. Int J Radiat Oncol Biol Phys 47:413–418
Amini A, Lin SH, Wei C, Allen P, Cox JD, Komaki R (2012) Accelerated hypofractionated radiation therapy compared to conventionally fractionated radiation therapy for the treatment of inoperable nonesmall cell lung cancer. Radiat Oncol 7:33
Joo JH, Song SY, Kim SS, Jeong Y, Jeong SY, Choi W, Choi EK (2015) Definitive radiotherapy alone over 60 Gy for patients unfit for combined treatment to stage II-III non-small cell lung cancer: Retrospective analysis. Radiat Oncol 10:250. doi:10.1186/s13014-015-0560-z
Wang L, Correa CR, Zhao L, Hayman J, Kalemkerian GP, Lyons S et al (2009) The effect of radiation dose and chemotherapy on overall survival in 237 patients with Stage III non-small-cell lung cancer. Int J Radiat Oncol Biol Phys 73:1383–1390
Machtay M, Bae K, Movsas B, Paulus R, Gore EM, Komaki R et al (2012) Higher biologically effective dose of radiotherapy is associated with improved outcomes for locally advanced non small cell lung carcinoma treated with chemoradiation: An analysis of the Radiation Therapy Oncology Group. Int J Radiat Oncol Biol Phys 82:42534
Author information
Authors and Affiliations
Corresponding authors
Ethics declarations
Conflict of interest
D. Franceschini, F. De Rose, P. Navarria, E. Clerici, C. Franzese, T. Comito, A. Tozzi, C. Iftode, G. D’Agostino and M. Sorsetti declare that they have no competing interests. L. Cozzi acts as Scientific Advisor to Varian Medical Systems and is Clinical Research Scientist at Humanitas Cancer Center.
Rights and permissions
About this article
Cite this article
Franceschini, D., De Rose, F., Cozzi, L. et al. Radical hypo-fractionated radiotherapy with volumetric modulated arc therapy in lung cancer. Strahlenther Onkol 193, 385–391 (2017). https://doi.org/10.1007/s00066-017-1103-3
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00066-017-1103-3