Abstract
Purpose
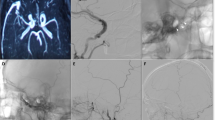
Most cavernous sinus dural arteriovenous fistulas (CSDAVF) are unilateral; however, simultaneous bilateral CSDAVFs occasionally may be found. This article reports on 141 patients and compares the angioarchitecture and outcomes of embolization of bilateral CSDAVFs with those of unilateral CSDAVFs, with reference to limited demographics (sex and age) of the patients.
Method
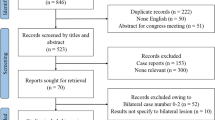
From January 2010 to February 2018 a total of 141 consecutive patients with CSDAVFs were referred for transvenous embolization. Bilateral CSDAVFs were found in 20 patients (14.2%, with a mean age of 62.2 years). The angioarchitecture of the 141 patients with CSDAVFs were evaluated by conventional cerebral angiography. We compared the angioarchitecture and treatment outcomes of 20 bilateral and 121 unilateral CSDAVFs, and in relation to the patients’ sex and age.
Results
Female patients significantly dominated the bilateral CSDAVFs (90%, p = 0.043). Bilateral eye symptoms were significantly more common in bilateral CSDAVFs (p = 0.011), with dominant orbital and cavernous symptoms, and showed statistical significance (p = 0.049 and 0.011, respectively). Occlusion of one CSDAVF may significantly decrease the fistula flow of the other untreated side (n = 13, 65%), leading to less coil utilization for embolization in bilateral CSDAVFs (p < 0.001). There was no statistical significance in the occurrence of occlusion of the inferior petrous sinus(s), in pial vein reflux, and treatment outcomes in the unilateral and bilateral CSDAVFs.
Conclusion
Bilateral CSDAVFs were more dominant in female patients and frequently presented with orbital and cavernous symptoms. Fewer coils were used per lesion in the bilateral CSDAVFs. There was no statistical significance in bilateral and unilateral CSDAVFs in terms of impact of venous drainage, pial vein reflux and treatment outcomes.


Similar content being viewed by others
References
Barrow DL, Spector RH, Braun IF, Landman JA, Tindall SC, Tindall GT. Classification and treatment of spontaneous carotid-cavernous sinus fistulas. J Neurosurg. 1985;62:248–56.
Kurata A, Miyasaka Y, Kunii M, Nagai S, Ohmomo T, Morishima H, Fujii K, Kan S. The value of long-term clinical follow-up for cases of spontaneous carotid cavernous fistula. Acta Neurochir (Wien). 1998;140:65-72.
Nukui H, Shibasaki T, Kaneko M, Sasaki H, Mitsuka S. Long-term observations in cases with spontaneous carotid-cavernous fistulas. Surg Neurol. 1984;21:543–52.
Sasaki H, Nukui H, Kaneko M, Mitsuka S, Hosaka T, Kakizawa T, Kimura R, Nagaseki Y, Naganuma H. Long-term observations in cases with spontaneous carotid-cavernous fistulas. Acta Neurochir (Wien). 1988;90:117-20.
Suh DC, Lee JH, Kim SJ, Chung SJ, Choi CG, Kim HJ, Kim CJ, Kook M, Ahn HS, Kwon SU, Kim JS. New concept in cavernous sinus dural arteriovenous fistula: correlation with presenting symptom and venous drainage patterns. Stroke. 2005;36:1134–9.
Cognard C, Gobin YP, Pierot L, Bailly AL, Houdart E, Casasco A, Chiras J, Merland JJ. Cerebral dural arteriovenous fistulas: clinical and angiographic correlation with a revised classification of venous drainage. Radiology. 1995;194:671–80.
Benndorf G, Bender A, Lehmann R, Lanksch W. Transvenous occlusion of dural cavernous sinus fistulas through the thrombosed inferior petrosal sinus: report of four cases and review of the literature. Surg Neurol. 2000;54:42–54.
Klisch J, Huppertz HJ, Spetzger U, Hetzel A, Seeger W, Schumacher M. Transvenous treatment of carotid cavernous and dural arteriovenous fistulae: results for 31 patients and review of the literature. Neurosurgery. 2003;53:836–56. discussion 856–7.
Luo CB, Chang FC, Teng MM, Guo WY, Ting TW. Transvenous embolization of cavernous sinus dural arteriovenous fistula via angiographic occlusive inferior petrous sinus. J Chin Med Assoc. 2015;78:526–32.
Davies MA, Saleh J, Ter Brugge K, Willinsky R, Wallace MC. The natural history and management of intracranial dural arteriovenous fistulae. Part 1: benign lesions. Interv Neuroradiol. 1997;3:295–302.
Kirsch M, Henkes H, Liebig T, Weber W, Esser J, Golik S, Kühne D. Endovascular management of dural carotid-cavernous sinus fistulas in 141 patients. Neuroradiology. 2006;48:486–90.
Yoshida K, Melake M, Oishi H, Yamamoto M, Arai H. Transvenous embolization of dural carotid cavernous fistulas: a series of 44 consecutive patients. AJNR Am J Neuroradiol. 2010;31:651–5.
Geibprasert S, Krings T, Pereira V, Pongpech S, Piske R, Lasjaunias P. Clinical characteristics of dural arteriovenous shunts in 446 patients of three different ethnicities. Interv Neuroradiol. 2009;15:395–400.
Luo CB, Chang FC, Mu-Huo Teng M, Lin CJ, Wu HM, Guo WY, Chang CY. Transarterial Onyx embolization of intracranial dural arteriovenous fistulas: a single center experience. J Chin Med Assoc. 2014;77:184–9.
Reynolds MR, Lanzino G, Zipfel GJ. Intracranial dural arteriovenous fistulae. Stroke. 2017;48:1424–31.
Rhim JK, Cho YD, Yoo DH, Kang HS, Cho WS, Kim JE, Cho MJ, Hwang G, Kwon OK, Han MH. Endovascular treatment of bilateral cavernous sinus dural arteriovenous fistula: therapeutic strategy and follow-up outcomes. Korean J Radiol. 2018;19:334–41.
Biondi A, Milea D, Cognard C, Ricciardi GK, Bonneville F, van Effenterre R. Cavernous sinus dural fistulae treated by transvenous approach through the facial vein: report of seven cases and review of the literature. AJNR Am J Neuroradiol. 2003;24:1240–6.
Satomi J, Satoh K, Matsubara S, Nakajima N, Nagahiro S. Angiographic changes in venous drainage of cavernous sinus dural arteriovenous fistulae after palliative transarterial embolization or observational management: a proposed stage classification. Neurosurgery. 2005;56:494–502. discussion 494–502.
Kim DJ, Kim DI, Suh SH, Kim J, Lee SK, Kim EY, Chung TS. Results of transvenous embolization of cavernous dural arteriovenous fistula: a single-center experience with emphasis on complications and management. AJNR Am J Neuroradiol. 2006;27:2078–82.
Kato S, Ishihara H, Nakayama H, Fujii M, Fujisawa H, Kajiwara K, Nomura S, Sadanaga H, Suzuki M. Transvenous embolization for dural arteriovenous shunt of the cavernous sinus. Comparison of multi-staged transvenous embolization and transvenous embolization with sinus packing. Interv Neuroradiol. 2007;13:353–8.
Ducruet AF, Albuquerque FC, Crowley RW, McDougall CG. The evolution of endovascular treatment of carotid cavernous fistulas: a single-center experience. World Neurosurg. 2013;80:538–48.
Luo CB, Chang FC, Wang AG, Lin CJ, Guo WY, Ting TW. Transvenous coil embolization of cavernous sinus dural arteriovenous fistula on a revised classification. World Neurosurg. 2016;95:357–67.
Park SH, Park KS, Kang DH, Hwang JH, Hwang SK. Stereotactic radiosurgery for intracranial dural arteriovenous fistulas: its clinical and angiographic perspectives. Acta Neurochir (Wien). 2017;159:1093-103.
Guo WY, Pan DH, Wu HM, Chung WY, Shiau CY, Wang LW, Chiou HJ, Yen MY, Teng MM. Radiosurgery as a treatment alternative for dural arteriovenous fistulas of the cavernous sinus. AJNR Am J Neuroradiol. 1998;19:1081–7.
Kai Y, Hamada J, Morioka M, Yano S, Kuratsu J. Treatment of cavernous sinus dural arteriovenous fistulae by external manual carotid compression. Neurosurgery. 2007;60:253–7. discussion 257–8.
Kobkitsuksakul C, Jiarakongmun P, Chanthanaphak E, Pongpech S. Radiographic evaluation and clinical implications of venous connections between dural arteriovenous fistula of the cavernous sinus and cerebellum and the Pontomedullary venous system. World Neurosurg. 2015;84:1112–26.
Meyers PM, Halbach VV, Dowd CF, Lempert TE, Malek AM, Phatouros CC, Lefler JE, Higashida RT. Dural carotid cavernous fistula: definitive endovascular management and long-term follow-up. Am J Ophthalmol. 2002;134:85–92.
Lee RJ, Chen CF, Hsu SW, Lui CC, Kuo YL. Cerebellar hemorrhage and subsequent venous infarction followed by incomplete transvenous embolization of dural carotid cavernous fistulas: a rare complication: case report. J Neurosurg. 2008;108:1245–8.
Yu SC, Cheng HK, Wong GK, Chan CM, Cheung JY, Poon WS. Transvenous embolization of dural carotid-cavernous fistulae with transfacial catheterization through the superior ophthalmic vein. Neurosurgery. 2007;60:1032–7. discussion 1037–8.
Jung KH, Kwon BJ, Chu K, Noh Y, Lee ST, Cho YD, Han MH, Roh JK. Clinical and angiographic factors related to the prognosis of cavernous sinus dural arteriovenous fistula. Neuroradiology. 2011;53:983–92.
Luo CB, Chang FC, Teng MM, Lin CJ, Wang AG, Ting TW. Aggressive cavernous sinus dural arteriovenous fistula: angioarchitecture analysis and embolization by various approaches. J Chin Med Assoc. 2016;79:152–8.
Funding
This study was funded by Taipei Veterans General Hospital (grant number: V107C-170, 023) and the Ministry of Science and Technology (grant number: MOST-106-2314B-075-011).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
L.-Y. Fay, C.-B. Luo, L.-W. Chen, J.-C. Wu, C.-H. Wu, F.-C. Chang and C.-J. Lin declare that they have no competing interests.
Ethical standards
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1975 Helsinki declaration and its later amendments or comparable ethical standards. Informed consent was obtained from all individual participants included in the study.
Rights and permissions
About this article
Cite this article
Fay, LY., Luo, CB., Chen, LW. et al. Bilateral Cavernous Sinus Dural Arteriovenous Fistulae. Clin Neuroradiol 31, 165–172 (2021). https://doi.org/10.1007/s00062-019-00868-z
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00062-019-00868-z