Summary
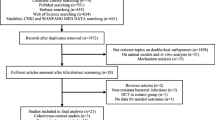
In a multinational, open, randomised, controlled clinical study, 474 hospitalised patients with moderate or severe infections were treated with sequential regimens of ofloxacin or ciprofloxacin. Ofloxacin 400 mg once daily or ciprofloxacin 200 mg twice daily were given intravenously for at least 3 days followed by oral treatment with ofloxacin 400 mg once daily or ciprofloxacin 500 mg twice daily. Overall cure rates of 86.8% (85.7%) in the ofloxacin group and 89.6% (89.5%) in the ciprofloxacin group were achieved in the intention-to-treat analysis (per protocol analysis). The overall bacteriological response rate (ofloxacin 89.5%, ciprofloxacin 89.0%) was comparable to the clinical cure rate. Both drugs were well tolerated and adverse events were rarely observed. It is concluded that ofloxacin and ciprofloxacin can be used successfully in the treatment of hospitalised patients with aerobic gram-positive and gram-negative infections. Ofloxacin has the advantage of a oncedaily regimen, compared to the twice-daily regimen with ciprofloxacin.
Zusammenfassung
In einer multinationalen, offenen, randomisierten, kontrollierten klinischen Studie wurden 474 hospitalisierte Patienten mit mittelschweren oder schweren Infektionen mit einer sequentiellen Therapie behandelt. Für mindestens 3 Tage wurde Ofloxacin 400 mg 1× täglich oder Ciprofloxacin 200 mg 2× täglich intravenös verabreicht. Anschließend wurde die Therapie oral fortgesetzt mit 400 mg Ofloxacin 1× täglich oder 500 mg Ciprofloxacin 2× täglich. Die Heilungsrate betrug 86,8% (85,7%) in der Ofloxacin- und 89,6% (89,5%) in der Ciprofloxacin-Gruppe in der „intention-to-treat“-Analyse („per-protocol“-Analyse). Die bakteriologische Wirksamkeit (Ofloxacin 89,5%, Ciprofloxacin 89,0%) war der klinischen Heilungsrate vergleichbar. Nebenwirkungen wurden selten beobachtet, die Verträglichkeit der beiden Therapien war gut. Die Ergebnisse haben gezeigt, daß Ofloxacin und Ciprofloxacin erfolgreich in der Behandlung hospitalisierter Patienten mit grampositiven (Aerobier) und gramnegativen Infektionen eingesetzt werden kann. Ofloxacin hat den Vorteil der Einmalgabe, Ciprofloxacin muß 2× am Tag verabreicht werden.
Similar content being viewed by others
References
Lockley, M. R., Wise, R., Dent, J. The pharmacokinetics and tissue penetration of ofloxacin. J. Antimicrob. Chemother. 14 (1984) 647–652.
Vance-Bryan, K., Guay, D. R. P., Rotschafer, J. C. Clinical pharmacokinetics of ciprofloxacin. Clin. Pharmacokinet. 19 (1990) 434–461.
Wolfson, J. S. Quinolone antimicrobial agents: adverse effects and bacterial resistance. Eur. J. Clin. Microbiol. Infect. Dis. 8 (1989) 1080–1092.
Paton, J. H., Reeves, D. S. Clinical features and management of adverse effects of quinolone antibacterials. Drug Safety 6 (1991) 8–27.
Hooper, D., Wolfson, J. Fluoroquinolone antimicrobial agents. N. Engl. J. Med. 324 (1991) 384–394.
Neu, H. C. Quinolone antimicrobial agents. Ann. Rev. Med. 43 (1992) 465–486.
Farrington, C. P., Manning, G. Test statistics and sample size formula for comparative binomial trials with null hypothesis of non-zero risk difference or non-unity relative risk. Stat. Med. 9 (1990) 1447–1454.
Naber, K. G., Sigl, G. Fleroxacin versus ofloxacin in patients with complicated urinary tract infection: a controlled clinical study. Am. J. Med. 94 (Suppl. 3A) (1993) 114S-117S.
Kromann-Andersen, B., Sommer, P., Pers, C., Larsen, V., Rasmussen, F.: Efficacy and safety of ofloxacin and ciprofloxacin in complicated urinary tract infection. 15th International Congress of Chemotherapy, July 19–24, 1987, Istanbul/Turkey. In: Advances in experimental and clinical chemotherapy, ecomed 3/88 (1987) pp. 45–47.
Chrysanthopoulos, C. J., Skoutelis, A. T., Starakis, J. C., Arvaniti, A., Bassaris, H. P. Use of ciprofloxacin in biliary sepsis. Infection 4 (1988) 249.
Thys, J. P., Jacobs, F., Byl, B. Role of quinolones in the treatment of bronchopulmonary infections, particularly pneumococcal and community-acquired pneumonia. Eur. J. Clin. Microbiol. Infect. Dis. 10 (1991) 304–315.
Gentry, L. O., Ramirez-Ronda, C. H., Rodriguez-Noriega, E., Thadepalli, H., del Rosal, P. L., Ramirez, C. Oral ciprofloxacin vs. parenteral cefotaxime in the treatment of difficult skin and skin structure infections. Arch. Intern. Med. 149 (1989) 2579–2583.
Gentry, L. O., Rodriguez-Gomez, G., Zeluff, B. J., Koshdel, A., Price, M. A comparative evaluation of oral ofloxacin versus intravenous cefotaxime therapy for serious skin and skin structure infections. Am. J. Med. 87 (Suppl. 6 C) (1989) 57S-60S.
Rahm, V., Schacht, P. Safety of ciprofloxacin: a review. Scand. J. Infect. Dis. 16 (Suppl.) (1989) 120–128.
Zaudig, M., von Bose, M., Weber, M. M., Bremer, D., Zieglgansberger, W. Psychotaxic effects of ofloxacin. Pharmacopsychiatry 22 (1989) 11–15.
Author information
Authors and Affiliations
Rights and permissions
About this article
Cite this article
Bassaris, P., Akalin, E., Calangu, S. et al. A randomised, multinational study with sequential therapy comparing ciprofloxacin twice daily and ofloxacin once daily. Infection 23, 227–233 (1995). https://doi.org/10.1007/BF01781203
Issue Date:
DOI: https://doi.org/10.1007/BF01781203