Abstract
Objectives
Ethnic enclaves are ethnically, spatially, and socially distinct communities that may promote health through access to culturally appropriate resources and reduced exposure to discrimination. This study examined ethnic enclave residence and pregnancy outcomes among Asian/Pacific Islander (API) women in the USA.
Design
We examined 9206 API births in the Consortium on Safe Labor (2002–2008). Ethnic enclaves were defined as hospital regions with high percentage of API residents (> 4%), high dissimilarity index (> 0.41; distribution of API and white residents within a geographic area), and high isolation index (> 0.03; interaction between API and white residents in an area). Gestational diabetes mellitus (GDM), preterm birth (PTB), small for gestational age (SGA), and smoking and alcohol use during pregnancy were reported in medical records supplemented with ICD-9 codes. Hierarchical logistic regression models estimated associations between ethnic enclaves and pregnancy outcomes, adjusted for maternal factors, area-level poverty, and air pollution.
Results
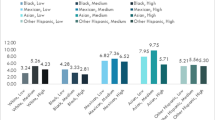
Women in enclaves had lower odds of GDM (OR 0.61; 95%CI 0.45, 0.82), PTB (OR 0.74; 95%CI 0.56, 0.99), and SGA (OR 0.68; 95%CI 0.52, 0.89) compared with women in non-enclaves. Prenatal smoking and alcohol use appeared less likely in enclaves, but estimates were imprecise. Within enclaves, about 10.5% of homes speak an API language, compared with 6.0% in non-enclaves. The mean percent of foreign-born API populations was 67.4% in enclaves and 68.8% in non-enclaves.
Conclusions
API women residing in ethnic enclaves had better pregnancy outcomes than API women residing in non-enclave areas. Access to culturally appropriate social supports and resources may be important for health promotion among API populations.


Similar content being viewed by others
Data Availability
Consortium on Safe Labor data is publicly available at https://dash.nichd.nih.gov/. Geographic identifying information is not publicly available; please see http://grants.nih.gov/grants/policy/data_sharing/ for National Institutes of Health data sharing policy. Census and American Community Survey data is publicly available from American Fact Finder at https://factfinder.census.gov. Dartmouth Atlas of Healthcare geographic crosswalks are publicly available at http://www.dartmouthatlas.org/tools/downloads.aspx?tab=39.
References
Lopez, G., N. Ruiz, and E. Patten. Key facts about Asian Americans, a diverse and growing population. Fact Tank: News in the Numbers. Pew Research Center. Washington, DC. 2017. [cited 2019 3/27/2019]; Available from: https://www.pewresearch.org/fact-tank/2017/09/08/key-facts-about-asian-americans/.
Bureau, U.S.C Place of birth (Asian alone) in the United States universe: Asian alone population in the United States more information 2013-2017 American Community Survey 5-year estimates. 2019; Available from: https://factfinder.census.gov/faces/tableservices/jsf/pages/productview.xhtml?pid = ACS_17_5YR_B06004D&prodType=table.
Bureau, U.S.C Race and Hispanic or Latino: 2010 - United States -- urban/rural and inside/outside metropolitan and micropolitan area more information 2010 Census Summary File 1. 2019; Available from: https://factfinder.census.gov/faces/tableservices/jsf/pages/productview.xhtml?pid = DEC_10_SF1_GCTP3.US26&prodType=table.
Liu M, Geron K. Changing neighborhood: ethnic enclaves and the struggle for social justice. Soc Justice. 2008;35(2 (112)):18–35.
Osypuk TL, Diez Roux AV, Hadley C, Kandula NR. Are immigrant enclaves healthy places to live? The multi-ethnic study of atherosclerosis. Soc Sci Med. 2009;69(1):110–20.
Lim S, Yi SS, Lundy de la Cruz N, Trinh-Shevrin C. Defining ethnic enclave and its associations with self-reported health outcomes among Asian American adults in New York city. J Immigr Minor Health. 2017;19(1):138–46.
Glaser SL, Chang ET, Clarke CA, Keegan TH, Yang J, Gomez SL. Hodgkin lymphoma incidence in ethnic enclaves in California. Leuk Lymphoma. 2015;56(12):3270–80.
Von Behren J, et al. The influence of neighborhood socioeconomic status and ethnic enclave on endometrial cancer mortality among Hispanics and Asian Americans/Pacific Islanders in California. Cancer Causes Control. 2018;29(9):875–81.
Janevic T, Borrell LN, Savitz DA, Echeverria SE, Rundle A. Ethnic enclaves and gestational diabetes among immigrant women in New York City. Soc Sci Med. 2014;120:180–9.
Deputy NP, et al. Prevalence and changes in preexisting diabetes and gestational diabetes among women who had a live birth - United States, 2012-2016. MMWR Morb Mortal Wkly Rep. 2018;67(43):1201–7.
Kane JB, Teitler JO, Reichman NE. Ethnic enclaves and birth outcomes of immigrants from India in a diverse U.S. state. Soc Sci Med. 2018;209:67–75.
Li Y, Luo Z, Holzman C, Liu H, Margerison CE. Paternal race/ethnicity and risk of adverse birth outcomes in the United States, 1989-2013. AIMS Public Health. 2018;5(3):312–23.
Yang TC, Shoff C, Noah AJ, Black N, Sparks CS. Racial segregation and maternal smoking during pregnancy: a multilevel analysis using the racial segregation interaction index. Soc Sci Med. 2014;107:26–36.
Pickett KE, et al. Ethnic density effects on maternal and infant health in the Millennium Cohort Study. Soc Sci Med. 2009;69(10):1476–83.
Grineski SE, Collins TW, Morales DX. Asian Americans and disproportionate exposure to carcinogenic hazardous air pollutants: a national study. Soc Sci Med. 2017;185(Supplement C):71–80.
Williams AD, Grantz KL, Zhang C, Nobles C, Sherman S, Mendola P. Ambient volatile organic compounds and racial/ethnic disparities in gestational diabetes mellitus: are Asian/Pacific Islander women at greater risk? Am J Epidemiol. 2019;188(2):389–97.
Ishimatsu J. Spotlight on Asian American and Pacific Islander poverty: a demographic profile. Washington, DC: National Coalition for Asian Pacific American Community Development; 2013.
DAHC. Dartmouth Atlas of health care: geographic crosswalks and research files. Lebanon, NH: Dartmouth College; 2013.
Zhang J, et al. Contemporary cesarean delivery practice in the United States. Am J Obstet Gynecol. 2010;203(4):326.e1–326.e10.
Chen G, Li J, Ying Q, Sherman S, Perkins N, Sundaram R, et al. Evaluation of observation-fused regional air quality model results for population air pollution exposure estimation. Sci Total Environ. 2014;485-486:563–74.
Williams AD, Wallace M, Nobles C, Mendola P. Racial residential segregation and racial disparities in stillbirth in the United States. Health Place. 2018;51:208–16.
Manson S, et al. IPUMS National Historical Geographic Information System: version 12.0 [database]. Minneapolis: University of Minnesota; 2016.
ADA. Gestational diabetes mellitus. Diabetes Care. 2003;26(suppl 1):s103–5.
Mannisto T, et al. Neonatal outcomes and birth weight in pregnancies complicated by maternal thyroid disease. Am J Epidemiol. 2013;178(5):731–40.
Howland RE, Mulready-Ward C, Madsen AM, Sackoff J, Nyland-Funke M, Bombard JM, et al. Reliability of reported maternal smoking: comparing the birth certificate to maternal worksheets and prenatal and hospital medical records, New York City and Vermont, 2009. Matern Child Health J. 2015;19(9):1916–24.
Allen J, Turner E. Ethnic residential concentrations in United States metropolitan areas. Geogr Rev. 2005;95(2):267–85.
Massey DS, Denton NA. The dimensions of residential segregation. Soc Forces. 1988;67(2):281–315.
Reardon SF, O’Sullivan D. Measures of spatial segregation. Sociol Methodol. 2004;34(1):121–62.
Cohen RA. Impact of type of insurance plan on access and utilization of health care services for adults aged 18-64 years with private health insurance: United States, 2007-2008. NCHS Data Brief. 2010(28):1–8.
Semega JL, Fontenot KR, Kollar MA. Income and poverty in the United States: 2016, in Current Population Reports. Washington, DC: U.S. Census Bureau; 2017. p. 60–259.
Robledo CA, et al. Preconception and early pregnancy air pollution exposures and risk of gestational diabetes mellitus. Environ Res. 2015;137(Supplement C):316–22.
Mendola P, et al. Preterm birth and air pollution: critical windows of exposure for women with asthma. J Allergy Clin Immunol. 2016;138(2):432–440.e5.
Ha S, Zhu Y, Liu D, Sherman S, Mendola P. Ambient temperature and air quality in relation to small for gestational age and term low birthweight. Environ Res. 2017;155:394–400.
Uphoff EP, Pickett KE, Crouch S, Small N, Wright J. Is ethnic density associated with health in a context of social disadvantage? Findings from the born in Bradford cohort. Ethn Health. 2016;21(2):196–213.
Bhopal RS. A four-stage model explaining the higher risk of Type 2 diabetes mellitus in South Asians compared with European populations. Diabet Med. 2013;30(1):35–42.
Zimmet P, Whitehouse S, Kiss J. Ethnic variability in the plasma insulin response to oral glucose in Polynesian and Micronesian subjects. Diabetes. 1979;28(7):624–8.
Lorch SA, Enlow E. The role of social determinants in explaining racial/ethnic disparities in perinatal outcomes. Pediatr Res. 2015;79:141.
Zhou M, Cho M. Noneconomic effects of ethnic entrepreneurship: a focused look at the Chinese and Korean enclave economies in Los Angeles. Thunderbird Int Bus Rev. 2010;52(2):83–96.
Osypuk TL, et al. Quantifying separate and unequal: racial-ethnic distributions of neighborhood poverty in Metropolitan America. Urban Aff Rev (Thousand Oaks, Calif). 2009;45(1):25–65.
Powell LM, Slater S, Chaloupka FJ, Harper D. Availability of physical activity–related facilities and neighborhood demographic and socioeconomic characteristics: a national study. Am J Public Health. 2006;96(9):1676–80.
Brewer M, Kimbro RT. Neighborhood context and immigrant children’s physical activity. Soc Sci Med. 2014;116:1–9.
Choi JY. Negotiating old and new ways: contextualizing adapted health care-seeking behaviors of Korean immigrants in Hawaii. Ethn Health. 2013;18(4):350–66.
Humes KR, Jones NA, Ramirez RR. Overview of Race and Hispanic Origin: 2010. 2010 Census Briefs. US Census Bureau. Washington, DC. 2011. [cited 2019 3/15/2019]; Available from: https://www.census.gov/prod/cen2010/briefs/c2010br-02.pdf.
ACOG. Practice Bulletin No. 180: gestational diabetes mellitus. Obstet Gynecol. 2017;130(1):e17–37.
Luu TM, Rehman Mian MO, Nuyt AM. Long-term impact of preterm birth: neurodevelopmental and physical health outcomes. Clin Perinatol. 2017;44(2):305–14.
Hong YH, Chung S. Small for gestational age and obesity related comorbidities. Ann Pediatr Endocrinol Metab. 2018;23(1):4–8.
Kataria Y, Gaewsky L, Ellervik C. Prenatal smoking exposure and cardio-metabolic risk factors in adulthood: a general population study and a meta-analysis. Int J Obes. 2018 43(4)763–73.
Paintner A, Williams AD, Burd L. Fetal alcohol spectrum disorders-- implications for child neurology, part 1: prenatal exposure and dosimetry. J Child Neurol. 2012;27(2):258–63.
Osypuk TL. Invited commentary: integrating a life-course perspective and social theory to advance research on residential segregation and health. Am J Epidemiol. 2013;177(4):310–5.
Kramer MS, Séguin L, Lydon J, Goulet L. Socio-economic disparities in pregnancy outcome: why do the poor fare so poorly? Paediatr Perinat Epidemiol. 2000;14(3):194–210.
DeSisto CL, Kim SY, Sharma AJ. Prevalence estimates of gestational diabetes mellitus in the United States, Pregnancy Risk Assessment Monitoring System (PRAMS), 2007-2010. Prev Chronic Dis. 2014;11:E104.
Fryer CD, Carroll MD, Ogden CL. Prevalence of overweight, obesity, and severe obesity among adults aged 20 and over: United States, 1990-1962 through 2015-2016. Health e-stats. National Center for Health Statistics. Hyattsville, MD. [cited 2019 2/16/2019] Available from: https://www.cdc.gov/nchs/data/hestat/obesity_adult_15_16/obesity_adult_15_16.pdf.
Nam S. Obesity and Asian Americans in the United States: systematic literature review. Osong Public Health Res Perspect. 2013;4(4):187–93.
Schempf AH, Mendola P, Hamilton BE, Hayes DK, Makuc DM. Perinatal outcomes for Asian, Native Hawaiian, and other Pacific Islander mothers of single and multiple race/ethnicity: California and Hawaii, 2003-2005. Am J Public Health. 2010;100(5):877–87.
Code Availability
Please contact corresponding author for the analytic file and code.
Funding
This research was supported by the Intramural Research Program of the National Institutes of Health, Eunice Kennedy Shriver National Institute of Child Health and Human Development (NICHD), including the funding for the Consortium on Safe Labor (Contract No. HHSN267200603425C) and the Air Quality and Reproductive Health Study (Contract No. HHSN275200800002I, Task Order No. HHSN27500008). This paper has been cleared for publication by the NICHD but the funding source had no role in the design, analysis, interpretation, or writing of the manuscript. The ZIP code–HRR crosswalk data was obtained from The Dartmouth Atlas, which is funded by the Robert Wood Johnson Foundation and the Dartmouth Clinical and Translational Science Institute, under the award number UL1TR001086 from the National Center for Advancing Translational Sciences (NCATS) of the National Institutes of Health (NIH).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of Interest
The authors declare that they have no conflicts of interest.
Ethical approval
This article does not contain any studies with human participants performed by any of the authors. Institutional Review Boards at all sites approved the CSL, and data are anonymous.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Williams, A.D., Messer, L.C., Kanner, J. et al. Ethnic Enclaves and Pregnancy and Behavior Outcomes Among Asian/Pacific Islanders in the USA. J. Racial and Ethnic Health Disparities 7, 224–233 (2020). https://doi.org/10.1007/s40615-019-00650-4
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s40615-019-00650-4