Abstract
Objective
The objective of this study is to describe our method and results for improvement of suboptimal initial post-implant dosimetry using targeted seed placement under local anesthesia within a clinic setting.
Methods
Re-implantation was performed in an outpatient clinic using local anesthesia with transrectal ultrasound (TRUS) and template-guided insertion of additional seeds in a shielded suite without general anesthesia. Patient reported discomfort is minimal, and time to complete the procedure is 30 min or less. D90 and V100 were used to measure implantation quality in both the initial and re-implantation setting.
Results
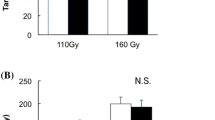
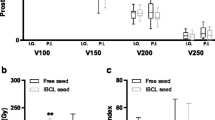
Ten patients were treated from October 2010 to December 2012 with additional Pd-103 seeds to improve initial post-implant dosimetry. A median of 73 seeds were placed initially (range 55–113), and a median of 3 additional seeds added later (range 2–6). Re-implantation was performed a median of 31 days after initial implantation (range 12–70). Median initial D90 was 100.2 % and initial V100 was 90.1 %. The median increase in D90 was 25.7 % (range 10.2–44.4 %), and the corresponding V100 increased by a median of 6.6 % (range 3.3–14.2 %). Median urethral D30 increased by 4.1 % (range 0.9–25 %) and rectal V100 increased by a median of 0.01 cm3 (range 0–0.75 cm3). A potential operating room cost reduction of $4000–$7000 and additional savings from general anesthesia fees is possible.
Conclusions
Re-implantation under local anesthesia for LDR prostate brachytherapy improves suboptimal dosimetry and avoids the risk and cost of OR/anesthesia time.

Similar content being viewed by others
References
Grimm P, Billiet I, Bostwick D et al (2012) Comparative analysis of prostate-specific antigen free survival outcomes for patients with low, intermediate and high risk prostate cancer treatment by radical therapy. Results from the Prostate Cancer Results Study Group. BJU Int 109:22–29
Crook JM, Gomez-Iturriaga A, Wallace K et al (2011) Comparison of health-related quality of life 5 years after SPIRIT: Surgical Prostatectomy Versus Interstitial Radiation Intervention Trial. J Clin Oncol 29:362–368
Herstein A, Wallner K, Merrick G et al (2005) I-125 versus Pd-103 for low-risk prostate cancer: long-term morbidity outcomes from a prospective randomized multicenter controlled trial. Cancer J 11:385–389
Potters L, Cao Y, Calugaru E et al (2001) A comprehensive review of CT-based dosimetry parameters and biochemical control in patients treated with permanent prostate brachytherapy. Int J Radiat Oncol Biol Phys 50:605–614
Nag S, Bice W, DeWyngaert K et al (2000) The American Brachytherapy Society recommendations for permanent prostate brachytherapy postimplant dosimetric analysis. Int J Radiat Oncol Biol Phys 46:221–230
Hughes L, Waterman FM, Dicker AP (2005) Salvage of suboptimal prostate seed implantation: Reimplantation of underdosed region of prostate base. Brachytherapy 4:163–170
Keyes M, Pickles T, Agranovich A et al (2004) 125I reimplantation in patients with poor initial dosimetry after prostate brachytherapy. Int J Radiat Oncol Biol Phys 60:40–50
Zaider M (2009) Dosimetric guidance on using brachytherapy (low-dose-rate or high-dose-rate) to offset a flawed permanent prostate implant. Brachytherapy 8:40–44
Shah C, Lanni TB Jr, Ghilezan MI et al (2012) Brachytherapy provides comparable outcomes and improved cost-effectiveness in the treatment of low/intermediate prostate cancer. Brachytherapy 11:441–445
Eldefrawy A, Katkoori D, Abramowitz M et al (2013) Active surveillance vs. treatment for low-risk prostate cancer: a cost comparison. Urol Oncol 31(5):576–580
Roessler B, Six LM, Gustorff B (2008) Anaesthesia for brachytherapy. Curr Opin Anaesthesiol 21:514–518
Wojcieszek E, Rembielak A, Bialas B et al (2010) Anaesthesia for radiation therapy—Gliwice experience. Neoplasma 57:155–160
Yue N, Dicker AP, Nath R et al (1999) The impact of edema on planning 125I and 103Pd prostate implants. Med Phys 26:763–767
Zelefsky MJ, Yamada Y, Cohen GN et al (2007) Intraoperative real-time planned conformal prostate brachytherapy: post-implantation dosimetric outcome and clinical implications. Radiother Oncol 84:185–189
Stone NN, Stone MM, Rosenstein BS et al (2011) Influence of pretreatment and treatment factors on intermediate to long-term outcome after prostate brachytherapy. J Urol 185:495–500
Wallner K (2002) Prostate brachytherapy under local anesthesia; lessons from the first 600 patients. Brachytherapy 1(3):145–148
Su Y, Davis BJ, Furutani KM et al (2007) Seed localization and TRUS fluoroscopy fusion for intraoperative prostate brachytherapy dosimetry. Comput Aided Surg 12:25–34
Song DY, Jain AK, Zhang Z et al (2011) Dynamic intraoperative dosimetry for prostate brachytherapy using a nonisocentric C-arm. Brachytherapy 10(2):98–106
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Kumar, R., Le, Y., Deweese, T. et al. Re-implantation following suboptimal dosimetry in low-dose-rate prostate brachytherapy: technique for outpatient source insertion using local anesthesia. J Radiat Oncol 5, 103–108 (2016). https://doi.org/10.1007/s13566-015-0198-3
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s13566-015-0198-3