Abstract
Huntington’s disease (HD) is a movement disorder characterized by the early selective degeneration of striatum. For motor control, the striatum receives excitatory inputs from multiple brain regions and projects the information to other basal ganglia nuclei. Despite the pathological importance of the striatal degeneration in HD, there are little anatomical data that show impaired striatal connectivity in HD. For the anatomical mapping of the striatum, we injected here a neurotracer DiD to the dorsal striatum of HD mouse model (YAC128). Compared with littermate controls, the number of the traced inputs to the striatum was reduced dramatically in YAC128 mice at 12 months of age suggesting massive destruction of the striatal connections. Basal ganglia inputs were significantly damaged in HD mice by showing 61 % decrease in substantia nigra pars compacta, 85 % decrease in thalamic centromedian nucleus, and 55 % decrease in thalamic parafascicular nucleus. Cortical inputs were also greatly decreased by 43 % in motor cortex, 48 % in somatosensory cortex, and 72 % in visual cortex. Besides the known striatal connections, the neurotracer DiD also traced inputs from amygdala and the amygdala inputs were decreased by 68 % in YAC128 mice. Considering the role of amygdala in emotion processing, the impairment in amygdalostriatal connectivity strongly suggests that emotional disturbances could occur in HD mice. Indeed, open-field tests further indicated that YAC128 mice exhibited changes in emotional behaviors related to symptoms of depression and anxiety. Although onset of HD is clinically determined on the basis of motor abnormality, emotional deficits are also common features of the disease. Therefore, our anatomical connectivity mapping of the striatum provides a new insight to interpret brain dysfunction in HD.








Similar content being viewed by others
References
Group THsDCR (1993) A novel gene containing a trinucleotide repeat that is expanded and unstable on Huntington’s disease chromosomes. Cell 72(6):971–983
Vonsattel JP, DiFiglia M (1998) Huntington disease. J Neuropathol Exp Neurol 57(5):369–384
Caine ED, Shoulson I (1983) Psychiatric syndromes in Huntington’s disease. Am J Psychiatry 140(6):728–733
Julien CL, Thompson JC, Wild S, Yardumian P, Snowden JS, Turner G, Craufurd D (2007) Psychiatric disorders in preclinical Huntington’s disease. J Neurol Neurosurg Psychiatry 78(9):939–943
Paulsen JS (2011) Cognitive impairment in Huntington disease: diagnosis and treatment. Curr Neurol Neurosci Rep 11(5):474–483. doi:10.1007/s11910-011-0215-x
Snowden JS, Craufurd D, Griffiths HL, Neary D (1998) Awareness of involuntary movements in Huntington disease. Arch Neurol 55(6):801–805
Cummings DM, Cepeda C, Levine MS (2010) Alterations in striatal synaptic transmission are consistent across genetic mouse models of Huntington’s disease. ASN Neuro 2(3):e00036. doi:10.1042/AN20100007
Clark VP, Lai S, Deckel AW (2002) Altered functional MRI responses in Huntington’s disease. Neuroreport 13(5):703–706
Andre VM, Cepeda C, Fisher YE, Huynh M, Bardakjian N, Singh S, Yang XW, Levine MS (2011) Differential electrophysiological changes in striatal output neurons in Huntington’s disease. J Neurosci 31(4):1170–1182. doi:10.1523/JNEUROSCI.3539-10.2011
Klapstein GJ, Fisher RS, Zanjani H, Cepeda C, Jokel ES, Chesselet MF, Levine MS (2001) Electrophysiological and morphological changes in striatal spiny neurons in R6/2 Huntington’s disease transgenic mice. J Neurophysiol 86(6):2667–2677
Kloppel S, Henley SM, Hobbs NZ, Wolf RC, Kassubek J, Tabrizi SJ, Frackowiak RS (2009) Magnetic resonance imaging of Huntington’s disease: preparing for clinical trials. Neuroscience 164(1):205–219. doi:10.1016/j.neuroscience.2009.01.045
Cepeda-Prado E, Popp S, Khan U, Stefanov D, Rodriguez J, Menalled LB, Dow-Edwards D, Small SA et al (2012) R6/2 Huntington’s disease mice develop early and progressive abnormal brain metabolism and seizures. J Neurosci 32(19):6456–6467. doi:10.1523/JNEUROSCI.0388-12.2012
Slow EJ, van Raamsdonk J, Rogers D, Coleman SH, Graham RK, Deng Y, Oh R, Bissada N et al (2003) Selective striatal neuronal loss in a YAC128 mouse model of Huntington disease. Hum Mol Genet 12(13):1555–1567
Van Raamsdonk JM, Pearson J, Slow EJ, Hossain SM, Leavitt BR, Hayden MR (2005) Cognitive dysfunction precedes neuropathology and motor abnormalities in the YAC128 mouse model of Huntington’s disease. J Neurosci 25(16):4169–4180. doi:10.1523/JNEUROSCI.0590-05.2005
Van Raamsdonk JM, Murphy Z, Slow EJ, Leavitt BR, Hayden MR (2005) Selective degeneration and nuclear localization of mutant huntingtin in the YAC128 mouse model of Huntington disease. Hum Mol Genet 14(24):3823–3835. doi:10.1093/hmg/ddi407
Tepper JM, Abercrombie ED, Bolam JP (2007) Basal ganglia macrocircuits. Prog Brain Res 160:3–7. doi:10.1016/S0079-6123(06)60001-0
Joshi PR, Wu NP, Andre VM, Cummings DM, Cepeda C, Joyce JA, Carroll JB, Leavitt BR et al (2009) Age-dependent alterations of corticostriatal activity in the YAC128 mouse model of Huntington disease. J Neurosci 29(8):2414–2427. doi:10.1523/JNEUROSCI.5687-08.2009
Tang T-S, Chen X, Liu J, Bezprozvanny I (2007) Dopaminergic signaling and striatal neurodegeneration in Huntington’s disease. J Neurosci 27(30):7899–7910
Franklin KB, Paxinos G (1997) Mouse brain in stereotaxic coordinates. Academic Press, San Diego
Van Raamsdonk JM, Pearson J, Rogers DA, Bissada N, Vogl AW, Hayden MR, Leavitt BR (2005) Loss of wild-type huntingtin influences motor dysfunction and survival in the YAC128 mouse model of Huntington disease. Hum Mol Genet 14(10):1379–1392. doi:10.1093/hmg/ddi147
Noh H, Jeon J, Seo H (2014) Systemic injection of LPS induces region-specific neuroinflammation and mitochondrial dysfunction in normal mouse brain. Neurochem Int 69:35–40. doi:10.1016/j.neuint.2014.02.008
Honig MG, Hume RI (1989) Dil and diO: versatile fluorescent dyes for neuronal labelling and pathway tracing. Trends Neurosci 12(9):333–341
Fonnum F, Storm-Mathisen J, Divac I (1981) Biochemical evidence for glutamate as neurotransmitter in corticostriatal and corticothalamic fibres in rat brain. Neuroscience 6(5):863–873
Killcross S, Coutureau E (2003) Coordination of actions and habits in the medial prefrontal cortex of rats. Cereb Cortex 13(4):400–408
Pan WX, Mao T, Dudman JT (2010) Inputs to the dorsal striatum of the mouse reflect the parallel circuit architecture of the forebrain. Front Neuroanat 4:147. doi:10.3389/fnana.2010.00147
Wall NR, De La Parra M, Callaway EM, Kreitzer AC (2013) Differential innervation of direct- and indirect-pathway striatal projection neurons. Neuron 79(2):347–360. doi:10.1016/j.neuron.2013.05.014
Gomez-Tortosa E, del Barrio A, Barroso T, Garcia Ruiz PJ (1996) Visual processing disorders in patients with Huntington’s disease and asymptomatic carriers. J Neurol 243(3):286–292
Smith Y, Raju D, Nanda B, Pare JF, Galvan A, Wichmann T (2009) The thalamostriatal systems: anatomical and functional organization in normal and parkinsonian states. Brain Res Bull 78(2–3):60–68. doi:10.1016/j.brainresbull.2008.08.015
Kimura M (1992) Behavioral modulation of sensory responses of primate putamen neurons. Brain Res 578(1):204–214
Minamimoto T, Hori Y, Kimura M (2005) Complementary process to response bias in the centromedian nucleus of the thalamus. Science 308(5729):1798–1801. doi:10.1126/science.1109154
Minamimoto T, Kimura M (2002) Participation of the thalamic CM–Pf complex in attentional orienting. J Neurophysiol 87(6):3090–3101. doi:10.1152/jn.00564.2001
Heinsen H, Rub U, Gangnus D, Jungkunz G, Bauer M, Ulmar G, Bethke B, Schuler M et al (1996) Nerve cell loss in the thalamic centromedian–parafascicular complex in patients with Huntington’s disease. Acta Neuropathol 91(2):161–168
Henderson JM, Carpenter K, Cartwright H, Halliday GM (2000) Loss of thalamic intralaminar nuclei in progressive supranuclear palsy and Parkinson’s disease: clinical and therapeutic implications. Brain J Neurol 123(Pt 7):1410–1421
Chen JY, Wang EA, Cepeda C, Levine MS (2013) Dopamine imbalance in Huntington’s disease: a mechanism for the lack of behavioral flexibility. Front Neurosci 7:114. doi:10.3389/fnins.2013.00114
Vijayraghavan S, Wang M, Birnbaum SG, Williams GV, Arnsten AF (2007) Inverted-U dopamine D1 receptor actions on prefrontal neurons engaged in working memory. Nat Neurosci 10(3):376–384. doi:10.1038/nn1846
Callahan JW, Abercrombie ED (2011) In vivo dopamine efflux is decreased in striatum of both fragment (R6/2) and full-length (YAC128) transgenic mouse models of Huntington’s disease. Front Syst Neurosci 5:61. doi:10.3389/fnsys.2011.00061
Petersen A, Puschban Z, Lotharius J, NicNiocaill B, Wiekop P, O’Connor WT, Brundin P (2002) Evidence for dysfunction of the nigrostriatal pathway in the R6/1 line of transgenic Huntington’s disease mice. Neurobiol Dis 11(1):134–146
Gray TS (1999) Functional and anatomical relationships among the amygdala, basal forebrain, ventral striatum, and cortex: an integrative discussion. Ann N Y Acad Sci 877(1):439–444
Lidov HG, Molliver ME (1982) An immunohistochemical study of serotonin neuron development in the rat: ascending pathways and terminal fields. Brain Res Bull 8(4):389–430
Hare TA, Tottenham N, Davidson MC, Glover GH, Casey BJ (2005) Contributions of amygdala and striatal activity in emotion regulation. Biol Psychiat 57(6):624–632. doi:10.1016/j.biopsych.2004.12.038
Yu H, Zhou Z, Zhou X (2013) The amygdalostriatal and corticostriatal effective connectivity in anticipation and evaluation of facial attractiveness. Brain Cog 82(3):291–300. doi:10.1016/j.bandc.2013.04.011
Zorrilla EP, Koob GF (2013) Amygdalostriatal projections in the neurocircuitry for motivation: a neuroanatomical thread through the career of Ann Kelley. Neurosci Biobehav Rev 37(9 Pt A):1932–1945. doi:10.1016/j.neubiorev.2012.11.019
Mann DM, Oliver R, Snowden JS (1993) The topographic distribution of brain atrophy in Huntington’s disease and progressive supranuclear palsy. Acta Neuropathol 85(5):553–559
Smolinsky AN, Bergner CL, LaPorte JL, Kalueff AV (2009) Analysis of grooming behavior and its utility in studying animal stress, anxiety, and depression. In: Mood and anxiety related phenotypes in mice. Springer, pp 21–36
Kalueff AV, Tuohimaa P (2005) Contrasting grooming phenotypes in three mouse strains markedly different in anxiety and activity (129S1, BALB/c and NMRI). Behav Brain Res 160(1):1–10
Kalueff AV, Tuohimaa P (2005) The grooming analysis algorithm discriminates between different levels of anxiety in rats: potential utility for neurobehavioural stress research. J Neurosci Methods 143(2):169–177
DeLong M (2000) The basal ganglia. In: Kandel ER, Schwartz JH, Jessell TM (eds) Principles of neural science. McGraw-Hill, New York, pp 853–867
Kandel ER, Schwartz JH, Jessell TM (2000) Principles of neural science, vol 4. McGraw-Hill, New York
Wolf RC, Sambataro F, Vasic N, Wolf ND, Thomann PA, Landwehrmeyer GB, Orth M (2011) Longitudinal functional magnetic resonance imaging of cognition in preclinical Huntington’s disease. Exp Neurol 231(2):214–222
Wolf RC, Sambataro F, Vasic N, Depping MS, Thomann PA, Landwehrmeyer GB, Sussmuth SD, Orth M (2014) Abnormal resting-state connectivity of motor and cognitive networks in early manifest Huntington’s disease. Psychol Med 44(15):3341–3356. doi:10.1017/S0033291714000579
Poudel GR, Egan GF, Churchyard A, Chua P, Stout JC, Georgiou-Karistianis N (2014) Abnormal synchrony of resting state networks in premanifest and symptomatic Huntington disease: the IMAGE-HD study. J Psychiatry Neurosci 39(2):87
Gray M, Egan G, Ando A, Churchyard A, Chua P, Stout J, Georgiou-Karistianis N (2013) Prefrontal activity in Huntington’s disease reflects cognitive and neuropsychiatric disturbances: the IMAGE-HD study. Exp Neurol 239:218–228
Ferraro S, Nanetti L, Piacentini S, Mandelli ML, Bertolino N, Ghielmetti F, Epifani F, Nigri A et al (2014) Frontal cortex BOLD signal changes in premanifest Huntington disease A possible fMRI biomarker. Neurology 83(1):65–72
Ferris CF, Kulkarni P, Toddes S, Yee J, Kenkel W, Nedelman M (2014) Studies on the Q175 knock-in model of Huntington’s disease using functional imaging in awake mice: evidence of olfactory dysfunction. Front Neurol 5:94
Stack EC, Kubilus JK, Smith K, Cormier K, Del Signore SJ, Guelin E, Ryu H, Hersch SM et al (2005) Chronology of behavioral symptoms and neuropathological sequela in R6/2 Huntington’s disease transgenic mice. J Comp Neurol 490(4):354–370
Arnulf I, Nielsen J, Lohmann E, Schiefer J, Wild E, Jennum P, Konofal E, Walker M et al (2008) Rapid eye movement sleep disturbances in Huntington disease. JAMA Neurol 65(4):482–488. doi:10.1001/archneur.65.4.482
Dogan I, Sass C, Mirzazade S, Kleiman A, Werner CJ, Pohl A, Schiefer J, Binkofski F et al (2014) Neural correlates of impaired emotion processing in manifest Huntington’s disease. Soc Cogn Affect Neur 9(5):671–680. doi:10.1093/scan/nst029
Ille R, Holl AK, Kapfhammer HP, Reisinger K, Schafer A, Schienle A (2011) Emotion recognition and experience in Huntington’s disease: is there a differential impairment? Psychiatry Res 188(3):377–382. doi:10.1016/j.psychres.2011.04.007
Sprengelmeyer R, Young AW, Calder AJ, Karnat A, Lange H, Homberg V, Perrett DI, Rowland D (1996) Loss of disgust. Perception of faces and emotions in Huntington’s disease. Brain J Neurol 119(Pt 5):1647–1665
Yoshimura N, Kawamura M, Masaoka Y, Homma I (2005) The amygdala of patients with Parkinson’s disease is silent in response to fearful facial expressions. Neuroscience 131(2):523–534. doi:10.1016/j.neuroscience.2004.09.054
Acknowledgments
This work was supported by an intramural funding from the Korea Institute of Science and Technology (2E25023 and 2 V03400 to Y.K.) and the National Research Foundation of Korea (NRF) grant funded by the Korea government (MEST), the National Research Foundation of Korea (2012R1A2A2A02118 38 to Y.K. and 2011-0030928, 2011-0030049 and 2012-003338 to H.S.). This study was also supported by the National Institutes of Health (NIH) Grant (R01 NS067283 to H.R.)
Author information
Authors and Affiliations
Corresponding author
Additional information
Dohee Kim and Jeha Jeon contributed equally to this work.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Fig. S1
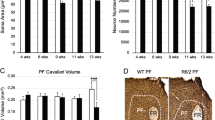
Striatal degeneration and motor deficits in YAC128 mice. a YAC128 mice showed neuronal loss in striatum by showing 28 % decrease of DARPP-32 (dopamine- and cAMP-regulated phosphoprotein, MW 32 kDa)-positive neurons. Scale bar: 100 μm. b Rotarod test indicates that YAC128 mice show significantly shortened latency to fall on the rod (DOC 428 kb)
Fig. S2
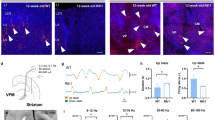
Photomicrography of brain slices presenting two types of DiD-labeled patterns. a VL region shows the amorphous shading pattern of DiD fluorescence and CM region shows DiD-labeled somata. b SNr region shows the amorphous shading pattern of DiD fluorescence, and SNc region shows DiD-labeled somata. Scale bars: 200 μm. VL ventrolateral nucleus, CM centromedian nucleus, SNc substantia nigra pars compacta, SNr substantia nigra pars reticulata (DOC 739 kb)
Rights and permissions
About this article
Cite this article
Kim, D., Jeon, J., Cheong, E. et al. Neuroanatomical Visualization of the Impaired Striatal Connectivity in Huntington’s Disease Mouse Model. Mol Neurobiol 53, 2276–2286 (2016). https://doi.org/10.1007/s12035-015-9214-2
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12035-015-9214-2