Abstract
Objective
To assess whether monitoring sedation status using bispectral index (BIS) as an adjunct to clinical evaluation was associated with a reduction in the total amount of sedative drug used in a 12 h period.
Design
Prospective randomized controlled clinical trial.
Setting
Tertiary care neurocritical care unit.
Patients
Sixty-seven mechanically ventilated adult patients receiving continuous intravenous sedation with propofol.
Interventions
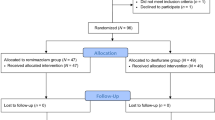
Sedation monitoring using clinical assessment with the Ramsay scale (Ramsay-alone group) or clinical assessment plus BIS monitoring (BIS-augmentation group). Subjects were randomized to Ramsay-alone (n = 35), or BIS-augmentation (n = 32). Nurses adjusted the dose of propofol to a Ramsay of 4, or a Ramsay of 4 and BIS between 60 and 70.
Measurements and Main Results
Patients in the BIS-augmentation group received significantly less propofol by volume (93.5 ml vs. 157.8 ml, respectively; P < .015), and had lower infusion rates (14.6 vs. 27.9 mcg/kg/min; P = .003). There is a lower risk of propofol infusion exceeding manufacturer’s recommended dosing guides in the BIS-augmentation group versus the Ramsay-alone group (0 vs. 23%, P = .0052). The BIS-augmentation group woke up much quicker than those in the Ramsay-alone group (1.2 vs. 7.5 min; P < .0001).
Conclusions
BIS-augmented sedation monitoring resulted in a marked reduction in the total dose of sedative used to achieve the same level of clinical sedation resulting in shortened time to wake up without any measurable adverse effects. Physiologic sedation assessment tools may provide a useful means of improving the care of sedated critically ill patients.


Similar content being viewed by others
References
Jacobi J, Fraser GL, Coursin DB, et al. Clinical practice guidelines for the sustained use of sedatives and analgesics in the critically ill adult. Crit Care Med. 2002;30(1):119–41.
Arbour RB. Using the Bispectral Index to assess arousal response in a patient with neuromuscular blockade. Am J Crit Care. 2000;9(6):383–7.
Carrasco G. Instruments for monitoring intensive care unit sedation. Crit Care. 2000;4(4):217–25. doi:10.1186/cc697.
Kollef MH, Levy NT, Ahrens TS, Schaiff R, Prentice D, Sherman G. The use of continuous I.V. sedation is associated with prolongation of mechanical ventilation. Chest. 1998;114(2):541–8. doi:10.1378/chest.114.2.541.
Weinert CR, Chlan L, Gross C. Sedating critically ill patients: Factors affecting nurses’ delivery of sedative therapy. Am J Crit Care. 2001;10(3):156–65. quiz 166–157.
Flaishon R, Windsor A, Sigl J, Sebel PS. Recovery of consciousness after thiopental or propofol. Bispectral index and isolated forearm technique. Anesthesiology. 1997;86(3):613–9. doi:10.1097/00000542-199703000-00013.
Mion LC, Minnick AF, Leipzig RM, Catrambone CD, Johnson ME. Patient-initiated device removal in intensive care units: a national prevalence study. Crit Care Med. 2007;35(12):2714–20.
Tung A, Lynch JP, Roizen MF. Use of the bis monitor to detect onset of naturally occurring sleep. J Clin Monit Comput. 2002;17(1):37–42.
Boulain T. Unplanned extubations in the adult intensive care unit: a prospective multicenter study. Association des Reanimateurs du Centre-Ouest. Am J Respir Crit Care Med. 1998;157(4 Pt 1):1131–7.
Grap MJ, Glass C, Lindamood MO. Factors related to unplanned extubation of endotracheal tubes. Crit Care Nurse. 1995;15(2):57–65.
Kaushal R, Bates DW, Franz C, Soukup JR, Rothschild JM. Costs of adverse events in intensive care units. Crit Care Med. 2007;35(11):2479–83.
Olson D, Lynn M, Thoyre SM, Graffagnino C. The limited reliability of the Ramsay scale. Neurocrit Care. 2007;7(3):227–31. doi:10.1007/s12028-007-0069-x.
Tallgren M, Pettila V, Hynninen M. Quality assessment of sedation in intensive care. Acta Anaesthesiol Scand. 2006;50(8):942–6. doi:10.1111/j.1399-6576.2006.01094.x.
Chisholm CJ, Zurica J, Mironov D, Sciacca RR, Ornstein E, Heyer EJ. Comparison of electrophysiologic monitors with clinical assessment of level of sedation. Mayo Clin Proc. 2006;81(1):46–52.
Watson BD, Kane-Gill SL. Sedation assessment in critically ill adults: 2001–2004 update. Ann Pharmacother. 2004;38(11):1898–906. doi:10.1345/aph.1E167.
Olson DM, Graffagnino C, King K, Lynch JR. Toward solving the sedation-assessment conundrum: bispectral index monitoring and sedation interruption. Crit Care Nurs Clin North Am. 2005;17(3):257–67. doi:10.1016/j.ccell.2005.04.008.
Abbott/American Association of Critical-Care Nurses; Saint Thomas Health System Sedation Expert Panel Members. Consensus conference on sedation assessment. A collaborative venture by Abbott Laboratories, American Association of Critical-Care Nurses, and Saint Thomas Health System. Crit Care Nurse 2004;24(2):33–41.
Ramsay MA, Savege TM, Simpson BR, Goodwin R. Controlled sedation with alphaxalone-alphadolone. BMJ. 1974;2(920):656–9.
Glass PS, Bloom M, Kearse L, Rosow C, Sebel P, Manberg P. Bispectral analysis measures sedation and memory effects of propofol, midazolam, isoflurane, and alfentanil in healthy volunteers. Anesthesiology. 1997;86(4):836–47.
Gan TJ, Glass PS, Windsor A, et al. Bispectral index monitoring allows faster emergence and improved recovery from propofol, alfentanil, and nitrous oxide anesthesia. BIS Utility Study Group. Anesthesiology. 1997;87(4):808–15. doi:10.1097/00000542-199710000-00014.
Song D, Joshi GP, White PF. Titration of volatile anesthetics using bispectral index facilitates recovery after ambulatory anesthesia. Anesthesiology. 1997;87(4):842–8. doi:10.1097/00000542-199710000-00018.
Johansen JW. Update on bispectral index monitoring. Best Pract Res Clin Anaesthesiol. 2006;20(1):81–99. doi:10.1016/j.bpa.2005.08.004.
Leblanc JM, Dasta JF, Kane-Gill SL. Role of the bispectral index in sedation monitoring in the ICU. Ann Pharmacother. 2006;40(3):490–500. doi:10.1345/aph.1E491.
Olson DM, Thoyre SM, Auyong DB. Perspectives on sedation assessment in critical care. AACN Adv Crit Care. 2007;18(4):380–95.
Cody RP, Smith JK. Applied statistics and the SAS programming language. 5th ed. Upper Saddle River, NJ: Pearson Prentice Hall; 2006.
Ahlen K, Buckley C, Pulsford AH. AstraZeneca’s response to the review by Wysowski and Pollock regarding deaths reported in association with propofol use. Anesthesiology. 2007;107(1):175. doi:10.1097/01.anes.0000268507.33332.a3. author reply 176.
Nicholson T, Patel J, Sleigh JW. Sleep patterns in intensive care unit patients: a study using the bispectral index. Crit Care Resusc. 2001;3(2):86–91.
Devlin JW, Nasraway SA Jr. Reversing oversedation in the intensive care unit: the role of pharmacists in energizing guideline efforts and overcoming protocol fatigue. Crit Care Med. 2008;36(2):626–8.
Avidan MS, Zhang L, Burnside BA, et al. Anesthesia awareness and the bispectral index. N Engl J Med. 2008;358(11):1097–108. doi:10.1056/NEJMoa0707361.
Lindholm ML, Brudin L, Sandin RH. Bispectral index monitoring: appreciated but does not affect drug dosing and hypnotic levels. Acta Anaesthesiol Scand. 2008;52(1):88–94.
Weinert CR, Calvin AD. Epidemiology of sedation and sedation adequacy for mechanically ventilated patients in a medical and surgical intensive care unit. Crit Care Med. 2007;35(2):393–401. doi:10.1097/01.CCM.0000254339.18639.1D.
Rodrigues GR Jr, do Amaral JL. Influence of sedation on morbidity and mortality in the intensive care unit. Sao Paulo Med J. 2004;122(1):8–11. doi:10.1590/S1516-31802004000100003.
Anis AH, Wang XH, Leon H, Hall R. Economic evaluation of propofol for sedation of patients admitted to intensive care units. Anesthesiology. 2002;96(1):196–201. doi:10.1097/00000542-200201000-00034.
Ostermann ME, Keenan SP, Seiferling RA, Sibbald WJ. Sedation in the intensive care unit: a systematic review. JAMA. 2000;283(11):1451–9. doi:10.1001/jama.283.11.1451.
Kost M. Manual of conscious sedation. Philadelphia: W.B. Saunders; 1998.
Deogaonkar A, Gupta R, Degeorgia M, et al. Bispectral Index monitoring correlates with sedation scales in brain-injured patients. Crit Care Med. 2004;32(12):2403–6. doi:10.1097/01.CCM.0000147442.14921.A5.
Haberthur C, Lehmann F, Ritz R. Assessment of depth of midazolam sedation using objective parameters. Intensive Care Med. 1996;22(12):1385–90. doi:10.1007/BF01709555.
Schulte-Tamburen AM, Scheier J, Briegel J, Schwender D, Peter K. Comparison of five sedation scoring systems by means of auditory evoked potentials. Intensive Care Med. 1999;25(4):377–82. doi:10.1007/s001340050861.
Sessler CN, Gosnell MS, Grap MJ, et al. The Richmond agitation-sedation scale: validity and reliability in adult intensive care unit patients. Am J Respir Crit Care Med. 2002;166(10):1338–44.
Acknowledgment
This research is supported by NIH T32 NR07091 Interventions to Prevent and Manage Chronic Illness and Aspect Medical Systems, Inc.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Olson, D.M., Thoyre, S.M., Peterson, E.D. et al. A Randomized Evaluation of Bispectral Index-Augmented Sedation Assessment in Neurological Patients. Neurocrit Care 11, 20–27 (2009). https://doi.org/10.1007/s12028-008-9184-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12028-008-9184-6